Research Article
Austin J Anat. 2014;1(5): 1022.
A 3D Reconstruction Model of the Female Pelvic Floor by Using Plastinated Cross Sections
Feil P1 and Sora MC2*
1Department of Surgery, Division of Pediatric Surgery, Medical University of Vienna, Austria
2Plastination Laboratory, Medical Imaging Cluster, Microscopy & Advanced Optical Imaging, Medical University of Vienna, Austria
*Corresponding author: Sora MC, Centre for Anatomy and Cell Biology, Plastination and Topografic Anatomy, Währingerstr 13/3, A-1090 Wien, Austria.
Received: July 24, 2014; Accepted: October 02, 2014; Published: October 07, 2014
Abstract
Background: The structures of the pelvic floor are clinically important but difficult to assess. To facilitate the understanding of the complicated pelvic floor anatomy, a computer-aided 3D-model was created from a female pelvis by using sheet plastination. The aim of this project was to create a three-dimensional model of the female pelvis and pelvic contents. This detailed 3D-model will be forwarded to the Technical College Aachen (Germany) for an additional biomechanical study regarding the pelvic floor dynamic.
Method: A slice anatomy study, using plastinated transparent pelvis cross sections, was performed in order to obtain a 3D reconstruction. One female human pelvis used for this study was first plastinated as a block according to the E12 ultrathin plastination method, then sliced into thin slices, and eventually subjected to 3D computerized reconstruction using the WinSURF modeling system (SURFdriver Software).
Results: The finished E12 slices provide excellent high-resolution anatomical images. Qualitative observations revealed that the morphological features of the model were consistent with those displayed by typical cadaveric specimens. The quality of the reconstructed images appeared distinct, especially the spatial positions and complicated relationships of contiguous structures of the female pelvis.
Conclusions: The high resolution of thin plastinated slices makes accurate anatomical surface reconstructions possible. The 3D-model of the female pelvis presented in this paper provides a stereoscopic view to study the adjacent relationship and arrangement of respective pelvis sections and can serve for finite element biomechanical simulations of the pelvic floor dynamics, as well as for teaching.
Keywords: Female pelvis; Three-dimensional model; Plastination; Levator ani; Gross anatomy; E12
Abbreviations
USL: Uterosacral Ligament; PUL: Pubourethral Ligament; B: Bladder; V: Vagina; Ut: Uterus; N: Nerves; Mpc: Pubococcygeus Muscle; Mpr: Puborectalis Muscle; EAS: External Anal Sphincter; S: Sacrum; PM: Piriformis Muscle; FA: Femural Artery; IC: Ischiocavernousus Muscle; No: Obturator Nerve; Cu: Cervix Uteri; Np: Pudendal Nerve; OM: Obturatorius Internus Muscle; CL: Cardinal Ligament; PVL: Pubovesical Ligament; Ur: Urethra: R: Rectum; U: Ureter; LA: Levator Ani; Mic: Illiococcygeus Muscle; Mco: Coccygeus Muscle; Cx: Coccyx; S: Pubic symphysis; Ni: Sciatic Nerve; FN: Femural Nerve; Ao: Obturator Arterie; Fp: Fornix Posterior; ACL: Anococcygeal Ligament; STP: Superficial Transverse Perineal Muscle
Introduction
Although “falling of the womb” and other pelvic floor problems were first described in the Kathun Papryrus [1], approximately 3000 years later, the specific birth induced injuries that result in pelvic floor dysfunction remain to be fully characterized. Since the early 1900s we know about the relationship of vaginal delivery to trauma to pelvic floor structures from cadaver dissections [2]. Pelvic floor dysfunction, which includes urinary and faecal incontinence as well as pelvic organ prolapse, is a highly prevalent disease in women. Ten percent of all women undergo at least one operation to treat pelvic floor dysfunction during their lifetime [3]. The annual cost of treating urinary incontinence in Austria alone is estimated at€48 million annually. However, little is known about specific pelvic floor pathomorphology and even less about pathophysiology as it relates to pelvic floor dysfunction. Investigations by DeLancey et al. [4,5] with modern imaging techniques confirmed these associations between morphologic pelvic floor damage and pelvic floor dysfunction. They showed an association between first vaginal delivery and Levator ani muscle damage, between Levator ani muscle damage and Levator ani muscle dysfunction, between Levator ani muscle damage and stress urinary incontinence and between Levator ani muscle damage and pelvic organ prolapse. DeLancey et al. [4,5] used Magnetic Resonance Imaging (MRI) to investigate Levator ani muscle damages. In a case-control study they found damaged Levator ani muscles in 20% of all women after their first vaginal delivery and in 0% of nulliparous women. Computerized modelling of the female pelvis can help to simulate the forces which are exerted onto the pelvic floor during a vaginal delivery. Lien et al. [6] constructed a computerized model in order to determine the stretch forces that exceed the forces which muscle tissue can usually sustain. They found stretch forces that exceed the forces which muscle tissue can usually sustain. One of the questions which arise is how in the majority of women the Levator ani muscle accommodates remarkable levels of tissue stretch without injury. In our study, a three-dimensional (3-D) model of the pelvis was built for the first time based on thin slice plastination cross-sections (1.5 mm) of the adult female pelvis and 3D reconstruction technology. In order to investigate this topic, we need to know the orientation of the Levator ani muscle and the interaction of muscles, bones, connective tissue and pelvic organs. Sections of a plastinated pelvis can help us to understand the Levator ani architecture. The relation of muscles, fascia, organs and bones can be studied perfectly and therefore suit best for a 3D reconstruction. This offers the opportunity to compare the use of identical physical and virtual models for the development of a 3D anatomical computer models basic system and its interactive manipulation.
The aim of this paper is to establish a 3D reconstruction model of the female pelvic floor based on plastinated slices. This detailed 3D-model will be forwarded to the Technical College Aachen (Germany). A further study will be carried out to calculate biomechanical data with our 3D-model. The aim of their calculations is to review the Integral Theory of Petros and to optimize implants that are placed in the pelvic floor, and thereby improve incontinence therapy. Moreover, the effort of each of the three components of the Levator ani muscle and the load-bearing capacity of the ligaments has to be determined. The model serves best for the visualization of the pelvic floor anatomy and for finite element simulations of the pelvic floor dynamics. Although databases consisting of serial sections derived from frozen cadaver material exist, plastination represents an alternative method for developing anatomical data that can be used for computerized reconstruction.
Materials and Methods
The 3D model was reconstructed from a 70 year old female cadaver specimen. The specimen was a part of the human donation program of the Medical University of Vienna. The Ethical Committee of the university provided approval for using the pelvis for 3D reconstruction: EK Nr: 1191/2011. The female pelvis was frozen at –80°C for one week. Afterwards, we plastinated it conform to the standard ultra-thin E12 slice plastination method [7]. Freeze substitution is the standard dehydration procedure for plastination. Shrinkage is minimized when cold acetone is used. The tissue block was submerged in cold (-25°C) technical quality 100% acetone for dehydration. Degreasing was performed by using methylene chloride. Impregnation was performed using the following epoxy Biodur (Rathausstr.18, 69126 Heidelberg, Germany) mixture: E12 (resin)/ E6 (hardener)/ E600 (accelerator) Sora et al. [7]. When impregnation was completed, the tissue block was removed from the vacuum chamber. A mold of Styrofoam was constructed and lined with polyethylene foil. The tissue block was inserted into the mold. The mold containing the impregnated specimen and resin-mix was placed in a 65°C oven for four days to harden the resin-mix. The tissue/resin block was cooled to room temperature and the mold was removed. A contact point diamond blade saw, Exact 310 CP (Exact Apparatebau GmbH, Norderstedt, Germany) was used for cutting the block. The hardened E12 block was cut into 1.6 ± 0.26 mm. Finally the caudal surfaces of the plastinated slices were scanned into a computer using an EPSON GT-10000+ Color Image Scanner. In every scan we included a ruler as a calibration marker. For morphological measurements we used the UTHSCSA IMAGE TOOL v.2.0 for Windows software (The University of Texas Health Science Center in San Antonio). The objects which had to be reconstructed were traced manually by using a graphic table (Wacom Cintiq 24HD). Each object was traced and numbered accordingly on every BMP file. After that, the reconstruction was rendered, visualized, and qualitatively checked for surface discontinuities by rotating the model. The following features, defined as objects, were used in the reconstruction: pelvic girdle, Levator ani muscle, obturator internus muscle, coccygeus muscle, piriformis muscle, rectum, uterus, uterosacral ligaments, cardinal ligament, ureter, urinary bladder,pubovesical ligament, urethra, pubourethral ligament, vagina, lumbosacral plexus, internal and external iliac arteries, sciatic nerve, lumbar plexus, obturator nerve and pudendal nerve.
Results
The finished E12 slices provided excellent high-resolution anatomical images (Figure 1a,1b,2a,2b). Sectional plastination showed the structures of the pelvic floor muscles and their relationship to adjacent structures with a resolution down to the microscopic level. By segmentation of the outlines, it was possible to create a 3D-model which consisted of the Levator ani muscle, pelvic organs, arteries, nerves, muscles and the pelvic bones. The anatomical structures of the pelvis could easily be identified and the borders could be traced rapidly and reliably. The thin plastinated slices distinctly displayed the nerves, muscles, vessels and bones of the pelvic region. Once scanned and loaded into WinSURF, edge detection was used to quickly collect tissue borders or contours. A three-dimensional model of the female pelvis, pelvic contents and perineum was created using thin plastinated sections. The generated 3D pelvis model displays a morphology corresponding qualitatively to the actual cadaver specimen (Figure 3,4,5). Qualitative observations revealed that the morphological features of the model were consistent with those displayed by typical cadaveric specimens. The quality of the reconstructed images appeared distinct, especially the spatial positions and complicated relationships of contiguous structures of the female pelvis. All reconstructed structures can be displayed in groups or as a whole and interactively rotated in 3D space. The result was a lifelike 3D-model that can be rotated in all levels and provides extraordinary insights into the anatomy of the pelvis and the pelvic floor.
Figure la-b: Female pelvis. a) Plastinated transverse section of the pelvis at the level of coccygis. Slice thickness 1.6 mm. b) Corresponding detail of the marked area on fig 1ashowing the Levator ani and its components.
Figure 2a-b: Female pelvis. a) Plastinated transverse section of the pelvis at the level the femoral head. Slice thickness 1.6 mm. b) Corresponding detail of the marked area on figure 2a showing the complex topography of the pelvic components.
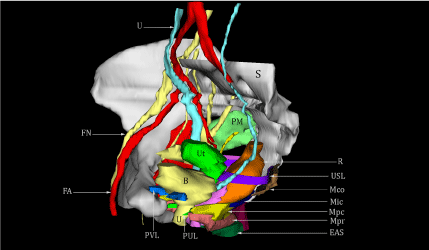
Figure 3: Lateral view of the 3D reconstruction of the female pelvis.
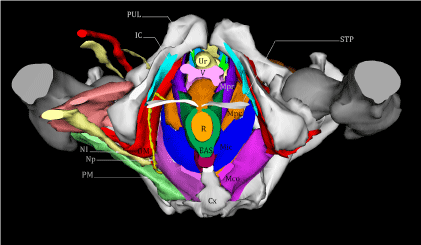
Figure 4: Structures of the female perineum. An inferior view of the structures of the female perineum.
Figure 5: Cranial view of the 3D reconstruction of the Levator ani muscle and its relation to the pelvic bone.
Discussion
As of recently, the E-12 plastination method has been used as a research tool, not only for slice plastination studies with the development of three-dimensional reconstructions, but also for the preservation and the representation of human or animal specimen for education and demonstration. The plastinated body slices can provide a unique insight into the human body. It is possible to show the smallest structures, e.g. capsule, ligaments, fascia, nerves, and vessels, and their correlation and composition to the neighboring structures in great detail. Moreover, with the help of the plastinated specimen anatomic-topographic structures can be measured, and based on the results conclusions can be drawn for surgical purposes. The pelvic floor has a complex spatial structure, of which only parts are visualized on sectional images [8,9]. It is, however, necessary for proper assessment of pathologies to correctly relate the visualized part to the entire structure. In contrast to anatomic preparation, the structures and spatial relationships of the tissues were not altered by plastination. To our knowledge, this is the first 3D-model of the female pelvic floor created using thin plastinated slices. Other models of the female pelvis have been created using a variety of cross-sectional data [10,11].The thin slices used in this study offer numerous advantages over other gross anatomical preparation methods currently utilized to generate images for computer reconstruction. The reconstruction of these anatomical structures is only possible due to the transparency of plastinated slices. One major advantage of our 3D-model is the reconstruction of connective tissue structures. Analyzing fine structures such as ligaments and fascia is crucial for the understanding of the pelvic dynamics; however they cannot be reconstructed by conventional radiological techniques. The system described here relies on relatively inexpensive hardware, including a scanner and computer. The WinSURF reconstruction package, from SURFdriver Software© (surface reconstruction driver), was developed expressly for use in three-dimensional anatomical reconstruction and is a simple icon-driven system [12]. A major problem that occurs with existing anatomical databases is the low resolution for smaller anatomical structures. Plastination provides a useful alternative for generating anatomical databases. Although the female pelvis reconstruction presented here did not appear to be affected by loss of information such as tissue loss between slices, further testing will be required to examine this issue. The capability of reconstructing individual and combined images of the pelvic structures, viewing them from all angles, and allowing for accurate measurement of their spatial relationships enables important guidance for teachers and students. The 3D reconstruction presented here allows interpretation of the sectional images in their 3D context and thus improves understanding of the radiologic sections [13,14]. The 3D-model of the pelvic floor, developed in our study, can serve as a teaching tool for anatomical and radiological education as well as for residency education, testing an unusual surgery and for the development of new surgical approaches.
Conclusions
The utilization of plastinates for generating tissues sections is useful for 3D computerized modeling. The 3D-model of the female pelvis presented in this paper provides a stereoscopic view to study the adjacent relationship and arrangement of respective pelvis sections and can serve for a finite element biomechanical simulation of the pelvic floor dynamics. Our model could lead to a better understanding of the pelvic floor anatomy, which is highly relevant for gynecologists, radiologists, surgeons, urologists, physical therapists and all health care professionals who treat women with pelvic floor dysfunction.
References
- Ricci JV. The genealogy of gynaecology. Philadelphia: Blakiston. 1943: 9-16.
- Halban J, Tandler J. Anatomie und Ätiologie der Genitalprolapse beim Weibe. Wien: Braumüller. 1907.
- Mant J, Painter R, Vessey M. Epidemiology of genital prolapse: observations from the Oxford Family Planning Association Study.Br J Obstet Gynaecol. 1997; 104: 579-585.
- DeLancey JO, Sørensen HC, Lewicky-Gaupp C, Smith TM. Comparison of the puborectal muscle on MRI in women with POP and levator ani defects with those with normal support and no defect.Int Urogynecol J. 2012; 23: 73-77.
- DeLancey JO, Kearney R, Chou Q, Speights S, Binno S. The appearance of levator ani muscle abnormalities in magnetic resonance images after vaginal delivery.Obstet Gynecol. 2003; 101: 46-53.
- Lien KC, Mooney B, DeLancey JO, Ashton-Miller JA. Levator ani muscle stretch induced by simulated vaginal birth.Obstet Gynecol. 2004; 103: 31-40.
- Sora MC, Epoxy Plastination of Biological Tissue: E12 Ultra-thin Technique. J Int Soc Plastination. 2007; 22: 40-45.
- Fritsch H, Lienemann A, Brenner E, Ludwikowski B. Clinical anatomy of the pelvic floor.Adv Anat Embryol Cell Biol. 2004; 175: III-IX, 1-64.
- Standring S. Muscles of the pelvis. In: Gray's anatomy, 40th(edn). Churchill-Livingstone, London. 2008; 1083.
- Beyersdorff D, Schiemann T, Taupitz M, Kooijman H, Hamm B, Nicolas V,et al. Sectional depiction of the pelvic floor by CT, MR imaging and sheet plastination: computer-aided correlation and 3D model.Eur Radiol. 2001; 11: 659-664.
- Parikh M, Rasmussen M, Brubaker L, Salomon C, Sakamoto K, Evenhouse R,et al. Three dimensional virtual reality model of the normal female pelvic floor.Ann Biomed Eng. 2004; 32: 292-296.
- Moody D, Lozanoff S.SURFdriver a practical computer program for generating three-dimensional models of anatomical structures using a PowerMac. Clinical Anatomy. 1998; 11:133.
- Höhne KH, Pflesser B, Pommert A, Riemer M, Schiemann T, Schubert R. A new representation of knowledge concerning human anatomy and function.Nat Med. 1995; 1: 506-511.
- Tan IL, Stoker J, Zwamborn AW, Entius KA, Calame JJ, Laméris JS,et al. Female pelvic floor: endovaginal MR imaging of normal anatomy.Radiology. 1998; 206: 777-783.