
Case Report
Austin J Anat. 2015;2(2): 1037.
Enhanced Anatomy Provided by Clinical Anomaly: Fourth Stage Vaginal Prolapse in a Medical Anatomy Lab
Viscomi NS and Clough RW*
Department of Anatomy, SIUC Life Sciences III, USA
*Corresponding author: Rich W Clough, Department of Anatomy, SIU School of Medicine Carbondale, Carbondale, IL 62901, USA
Received: June 23, 2015; Accepted: July 29, 2015; Published: August 03, 2015
Abstract
There is increased emphasis in early medical education to further enhance student empathy and compassion, to model physician, patient and care-giver considerations, and to heighten professionalism. The cadaver dissection lab offers a unique venue to hone these important considerations and it remains a valuable and time-honored practice in the training of physicians and other health professionals. Discoveries of congenital and acquired anomalies, pre-mortem clinical interventions including surgeries, device implantations, etc., as well as natural anatomical variations in cadaveric remains in the medical anatomy lab can be extraordinarily useful to facilitate these emphases and augment the overall learning experience of medical professionals in training. The authors present an unusual case-discovery in the anatomy lab, of a fourth stage vaginal prolapse with complete eversion and protrusion from the pelvis through the vaginal orifice and containing a rectocele. This anomaly discovered in a cadaver of an 89-year-old Caucasian woman proved to be extraordinarily instructive as well as motivating to our medical students learning female reproductive and pelvic anatomy. Discussions regarding compassion, empathy, care-giver and physician responsibilities, and professionalism all contributed to this learning experience. This and numerous other anomalous findings in the anatomy lab provide extraordinarily valuable tools to further enlighten students regarding ‘Doctoring’, and of course, facilitate learning of human anatomy.
Keywords: Learning enhancement; Pelvic anatomy; Vaginal prolapse; Clinical anomaly; Medical gross anatomy
Introduction
Anatomical variations, anomalies, clinical pathologies and a wide variety of pre-mortem clinical and prosthetic interventions are routinely discovered in gross anatomy labs across the world. Intuitively, clinical findings and peculiar anatomical variations would seem to greatly enhance the experience of training in the anatomical sciences, perhaps particularly with regard to human clinical anatomy. Anomalies, anatomical variations, clinical interventions, etc. can be studied and learned about in several different venues, but direct, hands on experience with cadavers in the anatomy lab yields a learning experience enriched with primary discovery, pathos, professionalism and other more intangible attributes of learning. Discovery was recently made in the authors’ medical school anatomy lab of a fourth stage vaginal prolapse in a cadaver of an 89-year-old Caucasian woman. Unfortunate as the case was, this presentation proved to enhance the gross anatomy learning experience for the medical students in witness.
Investigation and research of this condition would discover the following information. Vaginal vault prolapse is a non life-threatening medical condition in which the vagina loses its internal suspensor and muscular support allowing it to fall and protrude through the vaginal opening. Estimates vary widely, but as many as 50% of parous woman may develop some degree of genital prolapse or pelvic floor dysfunction [1-3]. Hysterectomy increases the risk for more severe stages of vaginal vault prolapse, and an estimated 11% of women who have undergone hysterectomy and who have compromised internal vaginal supports will develop prolapsed [4,5]. There are four categorical stages of prolapse as described by the POP-Q (Pelvic Organ Prolapse - Quantification) system of classification: a first stage prolapse is the term used to describe when the uterus or cervix moves into the upper part of the vagina but remains greater than 1 cm above the hymenal plane; second stage prolapse describes when the uterus or cervix moves into the lower part of the vagina and is less than 1cm below the hymenal plane but above the vaginal orifice; third stage prolapse describes when the uterus or cervix is just slightly protruding through the vaginal opening and is greater than 1cm but less than 2cm below the plane of the hymen; and fourth stage prolapse describes when the vagina, containing or not the uterus, is completely everted and protruded outside the body [6,7]. The first- and secondstage prolapses are most common whereas the fourth stage vaginal prolapse is least common and indeed quite rare. When the uterus and cervix are present within the prolapsed vagina, it is referred to as procidentia. The fourth stage prolapse is often accompanied by prolapse of surrounding structures such as the rectum, bladder, urethra or small intestine. There are several predisposing factors for vaginal prolapse, which include multigravida, advanced age, menopause, hysterectomy, obesity, hypertension, or delivering a macrosomic infant [8].
Understanding the anatomical reasons for vaginal prolapse requires that the student become familiar with the normal anatomy of the internal female genitalia and particularly the suspensor components of the vagina. Thus, the discovery of this clinical anomaly greatly and directly enhanced a Need-To-Know notion regarding support of the female genitalia. Moreover, witness of this anomaly by our medical student enhanced empathy, professionalism, patient-care considerations, and other more tacit attributes of physician training.
Case Presentation
This case reports the first such discovery of a complete, fourth stage vaginal prolapse seen by the authors in over 35 years of combined teaching in a school of medicine gross anatomy lab. The cadaver of an 89-year-old female showed a previous hysterectomy and exhibited other predisposing factors for prolapse including advanced age and moderate obesity. This condition is shown in (Figures 1,2). Careful observation and subsequent dissection revealed the vagina to be completely externalized inside-out with the ovaries and fallopian tubes remaining intact and in normal anatomical position. Additionally, the urinary bladder was retained in proper anatomical position within the lesser pelvis. The uterus was found to be absent, owing to hysterectomy earlier in life. During palpation of the prolapsed vagina, a large, soft mass was found within the posterior aspect. The vagina had a total length from superior to inferior of 12 cm, a circumference at the largest site of 28.5 cm (Figure 1), an anterior to posterior length at the vaginal orifice of approximately 12 cm and a calculated volume of 904.8 ml. Once measurements were completed, the everted vagina was incised anteriorly in the sagittal plane. Once opened, the soft mass in the posterior aspect of the externalized vagina was found to be a severe rectocele (rectal prolapse, Figure 2). The externalized vaginal mucosa was of a leathery consistency suggesting that it had been externalized for some time prior to death.
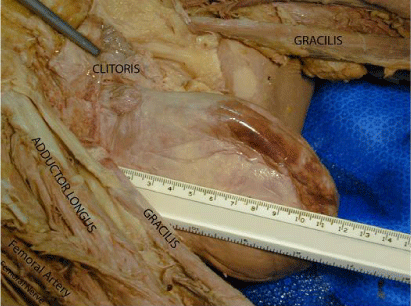
Figure 1: A lateral view of a 4th stage vaginal prolapse found on an 89-yearold
Caucasian female. Dissection and labeling of the surrounding structures
has been completed for orientation. A ruler has been placed to show the
superior to inferior extent of the anomaly.
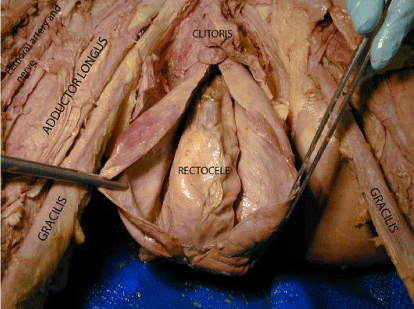
Figure 2: An anterior view of the prolapsed vaginal vault following sagittal
dissection to show an accompanying rectocele.
Discussion
In the training of physicians and other health care providers, it is our aim to instill and foster what we believe are essential and core attributes. These would certainly include basic and clinical knowledge, and beyond that, a variety of more tacit values such as professionalism, empathy, compassion, responsibility, patient-physician etiquette. The case presented in this report helped to consolidate several of these issues in a direct and hands-on manner in “safe” theater where students could explore, wonder, study, mourn, question, hypothesize, investigate, discover and learn. Students would learn that the vagina is retained within the pelvic cavity by an array of supporting attachments that include those that support the cervix and uterus as well as those supporting the rectum. With or without hysterectomy, the vagina may prolapse to the extent of being completely everted and externalized through the as vagina, often pulling or being pushed by associated organs prolapsing with it, particularly the rectum and bladder. Hysterectomy exacerbates the probability of severe vaginal prolapse [7] and corrective surgery, prosthesis, or special exercises are generally recommended to ameliorate the condition. It is anticipated that 4th stage vaginal prolapse may be detrimental to physical health and likely increases the probability of infections and incontinence. Moreover, in the aware patient (i.e., without dementia), a condition such as this would likely be detrimental to psychological health resulting from embarrassment, stress, confusion, and other emotional turmoil. Accordingly, our students learn through investigation and discussion that caregivers, including them, must be aware of and trained to be mindful of psychological co-morbidities that accompany medical conditions such as that reported.
To summarize, this particular case discovery in our anatomy lab served to enhance student learning of female reproductive anatomy. Moreover, this case served to poignantly increase awareness of patient issues such as the physical and psychological well being as mentioned. In follow-up investigation, our students might also explore and learn about attempts to ameliorate patient issues regarding physical and psychological health related to vaginal prolapse. For example, they may explore surgical approaches developed to repair this condition including transvaginal, laparoscopic, and laparoscopic with robotic assisted procedures. Techniques of surgical management of vaginal prolapse have been reviewed by Irvin and Huffish [9] and generally favor vaginal apex attachment to the sacrospinous ligament or to the iliococcygeal fascia to provide more suspensor support. Reoccurrence of vaginal prolapse has previously approached 30% [2,9], but with updated procedures this rate has shown decline.
In conclusion, not knowing the temporal history of the presenting case as to when hysterectomy or vaginal prolapse occurred, nor the psychological condition of the patient, our students freely hypothesized and discussed the case and its many ramifications. Thus, this unfortunate but valuable discovery in the medical gross anatomy lab proved to be extraordinarily instructive to the authors and to all the first year medical students in witness at the time. Importantly, in addition to learning anatomy of the female internal genitalia and pelvis, this discovery induced considerable empathy coupled with discussions of physician and caregiver issues and responsibilities. Lastly, cases such as that presented here and other anomalies found routinely within gross anatomy labs across the world lend considerable credence to continuing the time-honored practice of cadaveric dissection in the training of physicians and other health care professionals.
Acknowledgment
The authors acknowledge and expressly thank the body donors and their families who so graciously facilitate research and learning of medical anatomy for future health care providers. The authors report no conflicts of interest pertaining to this work. This work was supported by Southern Illinois University School of Medicine.
Notes on Contributors
Natalie Viscomi, M.S., is a full-time instructor in the Department of Anatomy at Southern Illinois University School of Medicine (SIUSOM) Carbondale, Carbondale, Illinois. She teaches gross anatomy, neuro anatomy and embryology to first year medical students. Rich Clough is a full professor and Chair of the Department of Anatomy at Southern Illinois University School of Medicine Carbondale, Carbondale, Illinois. He teaches gross anatomy, neuro anatomy and embryology to first year medical students.
References
- Beck RP. Pelvic relaxational prolapse. In: Principles and Practice of Clinical Gynecology. New York: John Wiley and Sons. 1983; 667-685.
- Olsen AL, Smith VJ, Bergstrom JO, Colling JC, Clark AL. Epidemiology of surgically managed pelvic organ prolapse and urinary incontinence. Obstet Gynecol. 1997; 89: 501–506.
- MacLennan AH, Taylor AW, Wilson DH, Wilson D. The prevalence of pelvic floor disorders and their relationship to gender, age, parity, and mode of delivery. Br J Obstet Gynecol, 2000; 107: 1460–1470.
- Marchionni M, Bracco GL, Checcucci V, Carabaneanu A, Coccia EM, Mecacci F,et al. True incidence of vaginal vault prolapse: thirteen years of experience. J Reprod Med, 1999; 44: 679–684.
- Elliott DS, Frank I, Chow GK. Robotics and laparoscopy for vaginal prolapse and incontinence. Current Bladder Dysfunction Reports, 2007; 2: 214-218.
- Bump RC, Mattiasson A, Bø K, Brubaker LP, DeLancey JO, Klarskov P, et al. The standardization of terminology of female pelvic organ prolapse and pelvic organ dysfunction. Am J Obstet Gynecol, 1996; 175: 10-17.
- Swift SE. The distribution of pelvic organ support in a population of female subjects seen for routine gynecologic health care. Am J Obstet Gynecol, 2000; 183: 277-285.
- Progetto Menopausa Italia Study Group (Parazzini F). Risk factors for genital prolapse in non-hysterectomized women around menopause. Results from a large cross-sectional study in menopausal clinics in Italy. Eur J Obstet Gynecol Reprod Biol, 2000; 93: 135-140.
- Irvin W, Hullfish K. Surgical management of vaginal vault prolapse. OBG Management, 2005; 17: 22-29.