
Research Article
Austin J Anat. 2016; 3(1): 1045.
Open-Door Laminoplasty versus French-Door Laminoplasty in Cervical Compressive Myelopathy: Grading the Evidence through a Meta-Analysis
Yan Li, Wei Guo, Ling-Xiao C, Yu-Lin L, Xiao-Bo W, Guang-Zhi N and Shi-Qing F*
Department of Orthopaedics, Tianjin Medical University General Hospital, China
*Corresponding author: Shi-Qing Feng, Department of Orthopedics, Tianjin Medical University, General Hospital, 154 Anshan Road, Heping District, Tianjin 300052, People’s Republic of China, China
Received: October 12, 2015; Accepted: January 18, 2016; Published: January 22, 2016
Abstract
Purpose: To compare the clinical outcomes of cervical compressive myelopathy with Open-door laminoplasty or French-door laminoplasty.
Method: We searched electronic databases including PubMed, Embase, Cochrane Central Register of Controlled Trials, and Google Scholar from 1966 to Feb 2015. No language restriction was applied. We used the Cochrane risk of bias tool to evaluate the trial quality. Each reference list was viewed for any ignore studies. Two authors independently extracted data from all eligible studies, including study design, patients’ characteristics, interventions and outcomes. The available data were using random-effects models or fixed-effects with mean differences or stand mean differences for continuous variables. GRADE system was used to assess the level of evidence.
Results: The meta-analyses indicated there was no significant difference in operative time and blood loss between Open-door and French-door group (MD -3.87, 95% CI -10.58 to 2.84, P value=0.26, I2=56%; SMD -0.10, 95% CI – 0.63 to 0.42, P value=0.70, I2=72%, repectively). Open-door laminoplasty significantly decreased Japanese Orthopedic Association (JOA) scores when compared with French-door laminoplasty (MD 0.09, 95% CI 0.59 to 1.39, P value<0.00001, I2=0%).
Conclusion: Considering the results, we could not confirm which laminoplasty is the better one in patients with cervical compressive myelopathy. More high-quality RCTs were needed to test the result.
Keywords: Open-door laminoplasty; French-door laminoplasty; Cervical compressive myelopathy; Meta-analysis; Randomized controlled trial GRADE
Introduction
Cervical Compressive Myelopathy (CCM) is generally defined as the compression of cervical spinal cord caused by various pathological changes [1]. The principles of treatment for CCM are pain relief recovery of neural functions and preservation of patients’ locomotion. Surgery is still the only effective method to deal with CCM but the selection of surgical methods is still controversial.
Open-door and French-door laminoplasty have their own advantages and disadvantages, but the common purpose of both two is to enlarge the narrowed spinal canal and thus afford the challenge of reactivating the spinal cord. On one hand, Open-door laminoplasty is a standard procedure for the treatment of multiple levels of cervical spondylotic myelopathy. There are several techniques to maintain cervical canal expansion such as the Hirabayashi technique which is the classic open-door laminoplasty that maintains cervical canal expansion by suturing to the contralateral soft tissue [2]. On the other hand, French door laminoplasty consists of a median lamina split followed by a lateral thinning and opening of both hemilaminae. This technique provides satisfied and reliable results in patients with myelopathy due to cervical spondylosis and posterior thickening of the ligament umflavum [3]. In recent researches, scholars have suggested that open-door laminoplasty is superior to French-door laminoplasty, with respect to expansion of the sagittal diameter and because of lower complication rates [4]. Others have suggested that French-door laminoplasty is much more better than opendoor laminoplasty, for patients with multilevel cervical compressive myelopathy as determined by the Medical Outcomes Study 36-item Short- Form Health Survey (SF-36) and have recommended Frenchdoor laminoplasty to minimize postoperative C5 palsy in patients with asymmetrical Ossification Of The Posterior Longitudinal Ligament (OPLL) [5]. The aim of this study was to determine which of these two methods is more effective in terms of clinical and radiologic outcomes.
Methods
Criteria for considering studies
We included studies which compared open-door laminoplasty versus french-door laminoplasty in patients with cervical compressive myelopathy.
Studies were considered acceptable for inclusion in the system review if they met the criteria: (1) cervical compressive myelopathy; (2) Open-door laminoplasty compared with French-door laminoplasty.
Trials were excluded if they: (1) were abstracts, letters, or meeting proceedings; (2) had repeated data or did not report outcomes of interest.
Search methods
We searched A med (From 1985 to February 2015), British Nursing Index (From 1985 to February 2015), Embase (From 1974 to February 2015), PubMed (From 1966 to February 2015), the Cochrane Central Register of Controlled Trials (CENTRAL) (The Cochrane Library, most recent issue), Google scholar, SIGLE (System for Information on Grey Literature in Europe), the National Technical Information Service, the National Research Register (UK), and the Current Controlled Trials databases. Keywords and MeSH terms including “cervical compressive myelopathy” and “Opendoor laminoplasty” and “French-door laminoplasty” and “unilateral laminoplasty” and “sagittal splitting procedure” were used in the search strategy. We also viewed each reference list for any ignored papers
Selection of studies and assessment of risk of bias in included studies
Two review authors independently made the selection based on title and abstract. Any disagreement between review authors was resolved by discussion. If there were still some debates, a further reviewer and expert was consulted.
We used the Cochrane risk of bias tool to assess risk of bias [6]. The tool included seven domains, which were random sequence generation, allocation concealment, blinding of participants and personnel, blinding of outcome assessment, incomplete outcome data, selective reporting and other bias. The judgment for each domain was low risk of bias, high risk of bias, or unclear risk of bias and two authors independently evaluated the risk of studies.
Data extraction and management
Information including the authors, study design, mean age, sample size, study population, outcome measures and follow-up periods were extracted for each included study. For continuous data (e.g. Operation time, Blood loss, Japanese Orthopedic Association (JOA) scores), the Mean Differences (MDs) or Stand Mean Differences (SMDs) with 95%CI was used. We would contact the original author to ask for any missing information as possible as we can. If the paper didn’t support Standard Deviations (SDs) and we couldn’t get data from the author, there were two ways to be used. The first was calculation of the missing SDs if some other data were supplied, for example, MDs, P value and number of patients. The second was manual measurement by graphs presented in article. One review author entered the data into RevMan 5.2, after which another review author checked all values. Meta-analyses were only made when studies were considered to be sufficiently homogeneous and a random-effects model was used for the pooled analysis. We assessed the heterogeneity firstly by observing the overlap of CIs in the forest plots. And then, we used I2 analysis to evaluate the heterogeneity (I2 larger than 50% was considered high heterogeneity).
Assessment of reporting biases and sensitivity analyses
We used a funnel plot to identify possible publication bias. We changed the model and excluded study one by one to test the robustness of the result.
Level of evidence
The Grading of Recommendations Assessment, Development, and Evaluation (GRADE) approach is to grade the quality of evidence and strength of recommendations [6]. Risk of bias, limitations, the indirectness, the consistency of the results across studies, the precision of the overall estimate across studies and other considerations are six domains of the tool. For each outcome, if further research was very unlikely to change our confidence in the estimate of effect, the quality of the evidence was rated as high; if further research was likely to have an important impact on our confidence in the estimate of effect and may change the estimate, the quality was moderate; if further research was very likely to have an important impact on our confidence in the estimate of effect and is likely to change the estimate, the quality was low; if the estimate was very uncertain, the quality was very low. The GRADE pro 3.6 software was used to estimate the methodological quality of the evidence in the meta-analysis by two reviewers. If there were disagreements between the two reviewers, a third author would join to discuss and make decisions
We used GRADE pro 3.6 to assess the level of evidence.
Results
Study identification and selection
The PRISMA flow diagram of studies in the article is depicted in (Figure 1). The search was performed on February16th, 2014 and identified 78 references in the primary search and 7 through other sources. After removal of 43 duplicate references, the total amount of references to be screened was 42. After a screening by one author (Li) a total of 8 publications appeared eligible for inclusion, others were not selected for various reasons (e.g. Two studies were case reports and one study was about biomechanics) [7-9]. In total, 5 studies were included in the narrative review and data on 4 of these studies were included in the meta-analysis [10-13].
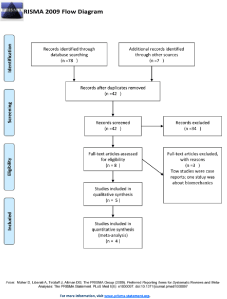
Figure 1: RISMA flow diagram.
Study characteristics
Table 1 provides a summary of the studies included in the review. A total of 268 participants (120 Open-door, 148 French-door).Study sample size ranged from 37 to 92. All studies were directly comparing Open-door group to French-door group. These studies were published between 1994 and 2014. Studies included patients whose mean age was between 59.4 and 63.2 years in Open-door group, 59.3 and 63.4 in French-door group.
Study
Sample size
Follow-up (months)
Mean ages (years)
Study design
Outcomes
2014,Hiroaki
92(46/46)
O:29.3/F:28.4
O:62.6±9.5/F:63.4±10.7
RCT
OT,BL,PC,JOA,ROM,MRI
2013, Lee
51(23/28)
O:24.6±1.3/F:27.8±1.2
O:59.4±1.9/F:59.3±2.0
Retrospective study
JOA,ROM,NDI,VAS,OT,BL,HS
2009,Motohiro
40(20/20)
N
O:59.9/F:61.1
RCT
OT,BL,PC,JOA,SF-36,LA
2000, Yue
37(12/25)
32.1
57.1
Retrospective study
JOA,OT,HS
1994, M. Naito
83(35/19/29)
N
62
Retrospective study
OT,BL
N: Not Mentioned; OT: Operation Time; BL: Blood Loss; JOA: Japanese Orthopedic Association Scores; HS: Hospitl Stay; ROM: Range Of Motion; NDI: Neck Disability Index; LA: Lordotic Angles; PC: Perioperative Complications; VAS: Visual Analog Scale; SF-36: Short-Form 36
Table 1: Main characteristics.
Risk of bias in included studies
(Figure 2 & 3) show Risk bias judgments in all 5 studies. There was no adequate information to evaluate whether other important risks existed or not. There was no adequate information to evaluate whether other important risks existed or not. There was no adequate information to evaluate whether other important risks existed or not. There was no adequate information to evaluate whether other important risks existed or not. Three studies (60%) described blinding of outcome assessment. There was no adequate information to evaluate whether other important risks existed or not.
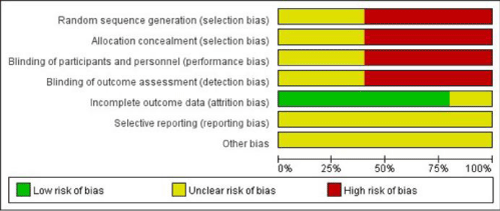
Figure 2: Risk of bias graph: review authors’ judgments about each risk of
bias item presented as percentages across all included studies.

Figure 3: Risk of bias summary: review authors’ judgments about each risk
of bias item for each included study.
There was no adequate information to evaluate whether other important risks existed or not.
Outcomes
Operation time
The pooled estimate of four studies examining data sets indicated there was no significant difference in operation time (MD -3.87, 95% CI -10.58 to 2.84, P value=0.26, I2=56%) (Figure 4).
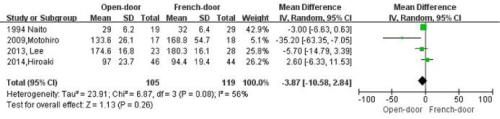
Figure 4: Forest plots of pooling operation time.
There was no significant difference in operation time (MD -3.87, 95%CI
-10.58 to 2.84, P value=0.26, I2=56%).
Blood loss
The pooled estimate of four studies examining data sets indicated there was no significant difference in blood loss (SMD -0.10, 95% CI –0.63 to 0.42, P value=0.70, I2=72%) (Figure 5).
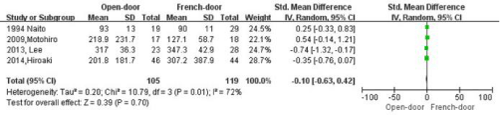
Figure 5: Forest plots of pooling blood loss.
There was no significant difference in blood loss (SMD -0.10, 95%CI –0.63 to
0.42, P value=0.70, I2=72%)..
JOA scores
The pooled estimate of three studies examining datasets indicated there was no significant difference in JOA scores (MD 0.19, 95% CI -0.91 to 1.29, P value=0.73, I2=76%) (Figure 6).
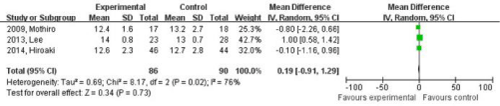
Figure 6: Forest plots of pooling Japanese Orthopedic Association (JOA)
cores.
There was no significant difference in JOA scores (MD 0.19, 95%CI -0.91 to
1.29, P value=0.73, I2=76%).
Other Outcomes
Hiroaki 2014
The main outcome measures were postoperative cervical lordotic angles, range of motion (ROM), spinal canal enlargement rate and spinal canal/ spinal body rations. The Open-Door group significantly increased spinal canal enlargement rate compared with French-Door group (French-Door group, 13.5%±69.8%; Open- Door group, 256.6%±76.6%; P=0.007). There were no significant differences in terms of Postoperative cervical lordotic angles, ROM and postoperative spinal canal/ spinal body rations.
Dong-Geun Lee 2013
The main outcome measures were ROM, Neck Disability Index (NDI), Visual Analog Scale (VAS), hospital stay and Nurick grades. There were no significant differences in terms of ROM, NDI, VAS, hospital stay and Nurick grades.
Motohiro 2009
The main outcome measures were Perioperative Complications, Axial Pain, Cob angle and the scores of SF-36 subscale (SF-36). The French-Door group significantly increased Axial Pain compared with Open-Door group (French-Door group, preoperative, 32.0±33.5 mm; postoperative, 26.7±30.4 mm; Open-Door group: preoperative, 14.3±31.0 mm; postoperative, 39.8±30.7 mm). The Cobb angle between preoperative and postoperative was significantly more in French-Door group as compared with Open-Door group. The French-Door group significantly increased SF-36 compared with Open-Door group. Wai MunYue 2000 the main outcome measures were hospital stay. There were no significant differences in terms of hospital stay.
Two studies mentioned ROM and hospital stay, the results were the same: there was no significant difference between two groups.
Publication bias
Publication bias was not assessed because the number of studies was small (<10).
Sensitivity analysis
Overall, most outcomes were stable. JOA scores there was a positive relationship
When we used fixed model (HR 0.74, 95% CI 0.37 to 1.12, P value=0.0001).The detail of sensitivity analyses was indicated in Table 2.
Sensitivity analysis
Heterogeneity
Effect
I2
Chi2
MD and 95%CI
P
Operation time
All studies (random model)
All studies (fixed model)
Exclude Lee 2013
Exclude Motohiro 2009
Exclude M.Naito 1994
56%
56%
61%
69%
0%
71%
6.87
6.87
5.13
6.50
1.79
6.87
-3.87 (-10.58, 2.4)
-3.03 (-6.17, 0.11)
-6.81 (-15.80, 2.19)
-4.24. (-14.42, 5.93)
-2.63 (-5.78, 0.53)
-6.853 (20.25, 6.55)
0.26
0.06
0.14
0.41
0.10
0.32
Blood loss
All studies (random model)
All studies (fixed model)
Exclude Hiroaki 2014
Exclude Lee 2013
Exclude Motohiro 2009
Exclude M.Naito 1994
72%
72%
79%
66%
66%
76%
10.79
10.79
9.59
5.81
5.81
8.26
-0.10 (-0.63, 0.42)
-0.17 (-0.44, 0.10)
0.00 (-0.77, 0.77)
0.10 -(0.45, 0.64)
-0.29 (-0.80, 0.22)
-0.21 (-0.86, 0.43)
0.70
0.22
1.00
0.73
0.27
0.51
JOA scores.
All studies (random model)
All studies (fixed model)
Exclude Hiroaki 2014
Exclude Lee 2013
Exclude Motohiro 2009
76%
76%
81%
0%
72%
8.17
8.17
5.39
0.58
3.57
0.19(-0.91, 1.29)
0.74(0.37, 1.12)
0.24 (-1.50, 1.98)
-0.34(-1.20, 0.52)
0.56 (-0.49,1.62)
0.73
0.0001
0.79
0.44
0.30
Table 2: Sensitivity analysis.
GRADE profile evidence
Table 3 indicates the GRADE quality of evidence.
Open-door laminoplasty compared to French-door laminoplasty for cervical compressive myelopathy
Patient or population: patients with cervical compressive myelopathy
Settings: inpatient
Intervention: Open-door laminoplasty
Comparison: French-door laminoplastyOutcomes
Illustrative comparative risks* (95% CI)
Relative effect
(95% CI)No of Participants
(studies)Quality of the evidence
(GRADE)Comments
Assumed risk
Corresponding risk
French-door laminoplasty
Open-door laminoplasty
Operation time
The mean operation time in the intervention groups was
3.87 lower
(10.58 lower to 2.84 higher)224
(4 studies)⊕⊕⊝⊝
low1,2blood loss
The mean blood loss in the intervention groups was
0.1 lower
(0.63 lower to 0.42 higher)224
(4 studies)⊕⊕⊝⊝
low1,2JOA scores
The mean joa scores in the intervention groups was
0.99 higher
(0.59 to 1.39 higher)176
(3 studies)⊕⊕⊕⊝
moderate1*The basis for the assumed risk (e.g. the median control group risk across studies) is provided in footnotes. The corresponding risk (and its 95% confidence interval) is based on the assumed risk in the comparison group and the relative effect of the intervention (and its 95% CI).
CI: Confidence Interval;GRADE Working Group grades of evidence
High quality: Further research is very unlikely to change our confidence in the estimate of effect.
Moderate quality: Further research is likely to have an important impact on our confidence in the estimate of effect and may change the estimate.
Low quality: Further research is very likely to have an important impact on our confidence in the estimate of effect and is likely to change the estimate.
Very low quality: We are very uncertain about the estimate.1Some researchers were open-lable studies.
2I2 > 50% was considered as a high risk bias.
Table 3: GRADE evidence.
Discussion
Summary of main results
The meta-analyses indicated that: (1) there was no significant difference in operation time in patients who received Open-door laminoplasty when compared with French-door laminoplasty, (2) patients who received open-door laminoplasty demonstrated no significant decrease in blood loss when compared with those who received french-door laminoplasty, (3) patients who received opendoor laminoplasty in addition to french-door laminoplasty were scores.
Agreements and disagreements in the current literature
The previous systematic review showed there was no significant difference in operation time, blood loss and JOA scores between Open-door group and French-door group by reporting one RCT and one cohort study [14]. Our article results were the same as the previous one. Our article also described some other outcomes like ROM, NDI and SF-36.
Weaknesses
The results of the review should be interpreted under some limitations. Firstly, only papers written in English were included in this article although we searched researches in all language, which means some potential biases might occur. Secondly, the sample size of studies was small, so we couldn’t totally exclude type-II error. Thirdly, there was substantial heterogeneity on account of different methodologies, duration of follow-up, ways of outcome measure and its presentation. The three issues made it difficult to reach any strong conclusions. Fourthly, only four trails included 268 patients in this article, we could not exclude type-II error and we had better cautiously make any recommendation based on these studies.
Conclusion
Implications for practice
The results of this review suggest there was no significant difference in operation time, blood loss and JOA scores in patients who received Open-door laminoplasty when compared with Frenchdoor laminoplasty. The limited study simple make us not draw a conclusion about which surgery method is the better one.
Implications for research
More large-scale studies are needed to examine the effect of opendoor laminoplasty and french-door laminoplasty for people with cervical compressive myelopathy. Also, perioperative complications, range of motion and hospital stay often reported or reported insufficiently and need to be assessed in future studies. In addition, more studies are needed to ascertain economic evaluation about costing and longer-term follow-up studies will help to determine any carryover effects.
Authors’ contributions
Shi-Qing Feng conceived of the design of the study. Yan Li and Wei Guo collected the data and contributed to the design of the study. Ling-Xiao Chen, Yu-Lin Li, Qiu-Li Wu and Guang-Zhi Ning prepared the manuscript. Xiao-Bo Wang edited the manuscript. All authors read and approved the final manuscript.
References
- Ulrich NHa, Maier M, Bernays RL, Krayenbuhl N, Kollias S. Cervical myelopathy due to chronic overshunting in a pediatric patient: case report and review of the literature. Turk Neurosurg. 2013; 23: 410-414.
- Ratliff JK, Cooper PR. Cervical laminoplasty: a critical review. J Neurosurg. 2003; 98: 230-238.
- Seichi A, Takeshita K, Ohishi I, Kawaguchi H, Akune T, Anamizu Y, et al. Long-term results of double-door laminoplasty for cervical stenotic myelopathy. Spine (Phila Pa 1976). 2001; 26: 479-487.
- Asgari S, Bassiouni H, Massoud N, Schlamann M, Stolke D, Sandalcioglu IE. Decompressive laminoplasty in multisegmental cervical spondylotic myelopathy: bilateral cutting versus open-door technique.Acta neurochirurgica. 2009; 151: 739-749.
- Kaneyama S, Sumi M, Kanatani T, Kasahara K, Kanemura A, Takabatake M, et al. Prospective study and multivariate analysis of the incidence of C5 palsy after cervical laminoplasty. Spine (Phila Pa 1976). 2010; 35: E1553-1558.
- GS. HJ: Handbook for Systematic Reviews of Interventions Version 5.1.0. The Cochrane Collaborationk. 2011.
- Faccioli F, Buffatti P, Grosslercher JC, Bricolo A, Dalle Ore G. [Open-door decompressive cervical laminotomy. Technic and initial experiences]. Neurochirurgie. 1987; 33: 38-43.
- Kaner T, Sasani M, Oktenoglu T, Ozer AF. Clinical outcomes following cervical laminoplasty for 19 patients with cervical spondylotic myelopathy. Turkish neurosurgery. 2009; 19: 121-126.
- Puttlitz CM, Deviren V, Smith JA, Kleinstueck FS, Tran QN, Thurlow RW, et al. Biomechanics of cervical laminoplasty: kinetic studies comparing different surgical techniques, temporal effects and the degree of level involvement.European spine journal: official publication of the European Spine Society, the European Spinal Deformity Society, and the European Section of the Cervical Spine Research Society. 2004; 13: 213-221.
- Lee DG, Lee SH, Park SJ, Kim ES, Chung SS, Lee CS, et al. Comparison of surgical outcomes after cervical laminoplasty: open-door technique versus French-door technique. Journal of spinal disorders & techniques. 2013; 26: E198-203.
- Nakashima H, Kato F, Yukawa Y, Imagama S, Ito K, Machino M, et al. Comparative effectiveness of open-door laminoplasty versus French-door laminoplasty in cervical compressive myelopathy. Spine (Phila Pa 1976). 2014; 39: 642-647.
- Okada M, Minamide A, Endo T, Yoshida M, Kawakami M, Ando M, et al. A prospective randomized study of clinical outcomes in patients with cervical compressive myelopathy treated with open-door or French-door laminoplasty. Spine (Phila Pa 1976). 2009; 34: 1119-1126.
- Yue WM, Tan CT, Tan SB, Tan SK, Tay BK. Results of cervical laminoplasty and a comparison between single and double trap-door techniques. J Spinal Disord. 2000; 13: 329-335.
- Heller JG, Raich AL, Dettori JR, Riew KD. Comparative effectiveness of different types of cervical laminoplasty. Evidence-based spine-care journal. 2013; 4: 105-115.