
Case Presentation
Austin J Anat. 2017; 4(1): 1060.
A Unique Case of Split Median Nerve at the Wrist by a Branch of the Ulnar Artery
Samarawickrama MB*
Department of Anatomy, University of Ruhuna, Srilanka
*Corresponding author: Samarawickrama MB, Department of Anatomy, Faculty of Medicine, University of Ruhuna, Karapitiya, Galle, Srilanka
Received: December 14, 2016; Accepted: January 03, 2017; Published: January 06, 2017
Abstract
Anatomical variations of the median nerve at the wrist level have been detected during imaging, dissections and surgical operations. These include bifid median nerve and abnormal branching pattern of the median nerve. Splitting of the median nerve due to persistent median artery, accessory muscles and ulna artery also been reported in the literature. The knowledge of any such variation at the wrist is very important as injury to the nerve is common at this site and nerve decompression is commonly performed at the carpel tunnel. Based upon findings of his own study and the other published reports, Lanz classified the variations of the median nerve at the wrist into four groups in 1977. This report is on a special case where splitting of median nerve due to a branch of the ulna artery at the vicinity of the wrist and not included in the Lanz classification.
Keywords: Median nerve; Anatomic variations; Split nerve; Bifid nerve
Case Presentation
A unilateral variation of the median nerve was found at the left wrist during routine dissection of upper limbs of a 72 year-old male cadaver. The median nerve had normal anatomy at its origin in the axilla and course in the arm and forearm up to the distal part of the forearm where it was split by a branch of the ulnar artery about 6 cm proximal to the proximal border of the flexor retinaculum (Figures 1 and 2). This split portion of the median nerve measured about 3.3 cm in length and rejoined together and form a single trunk before entering the carpel tunnel. Median nerve traversed within the carpel tunnel as a single trunk as in normal subjects. Its distribution within the hand was normal. The palmaris longus muscle was absent. The ulnar artery which had normal anatomy in the forearm gave off a small branch about 7 cm proximal to the proximal border of the flexure retinaculum [1]. This small branch passed laterally anterior to the flexor digitorum superficially tendon to become posterior to the median nerve. Then it pierced the MN and appeared on the anterior surface of the nerve and diminished in size as it passes on the anterior surface of the split portion of the median nerve (Figure 3).
Discussion
Median nerve is formed on the anterior or the lateral surface of the 3rd part of the axilary artery by joining the lateral and median roots from lateral and medial cords of the brachial plexus respectively. It then passes first lateral and then medial to the brachial artery up to the cubital fossa. The nerve enters the forearm to lie between flexure digitorum superficialis and flexure digitorum profunduds and reaches down the region of the wrist. There it passes lateral to the flexure digitorum superficialis tendons and lies deep and lateral to palmaris longus tendon and passes deep to the flexure retinaculum and gives off its terminal digital branches to the lateral three and half fingers and the motor branch to the thenar muscles [2].
Anatomical variation of the MN at the region of the wrist and the branching pattern in the palm is well reported due to its diagnostic and surgical importance. These variations have been detected in cadaveric studies, clinical dissections during hand surgeries and radiological imaging. These anatomical variations have been precisely describe by Lanz and classified in to four groups as follows [2].
I. Variation in the course of the thenar branch
II. Accessory branches at the distal portion of the carpal tunnel
III. High divisions of the median nerve
IV. Accessory branches proximal to the carpel tunnel
The case described here also shows high division of the median nerve. But it differ from the Lanz type III as the division do not continue distally and two divisions reunite before passing deep to the flexure retinaculum. The variation described in type III of the above classification, the divided nerve does not reunite and continue to the palm as in the case reported by Sanmuga et al [3].
There are number of associated conditions with high or abnormal division of the median nerve. These include persistent median artery, presence of an epineural septum, accessory muscle, and improper insertion of Palmaris longus tendon [4-6]. A case reported by the Arzu Hisahi showed that the median nerve has formed a ring around the ulnar artery [4]. The reason for the split in this case is due to the presence of an abnormal arterial branch from the ulnar artery which pierced the median nerve. So this is a unique case and this cause for the splitting of median nerve is not reported elsewhere.
The incidence of split median nerve in patients with median nerve entrapment is reported to be 2.8% according to the Lanz study. After that many studies have been done on patients with carpel tunnel syndrome using imaging techniques [5]. They have shown higher incidence of bifid median nerve in those patients ranging from 1-19% [6]. There are very few studies on normal population to find out the incidence of bifid median nerve. A study which was done by Walker et al., using 1026 wrists of manual laborers shows bifid median nerve in 8.6% of those wrists [7].
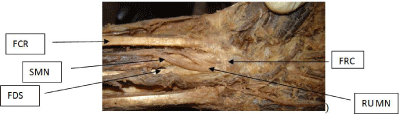
Figure 1: FCR: Flexor carpi radialis; FDS: Flexor digitorum superficialis;
FRC: Flexor reticnaculum; RUMN: Reunited median nerve; SMN: Split part
of the median nerve.
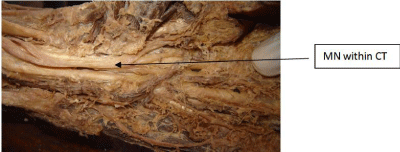
Figure 2: MN within CT = Median nerve within the carpal tunnel (the flexure
retinaculum is removed).

Figure 3: B: Branch; MN: Median Nerve; UA: Ulnar Artery.
High division of median nerve as in Lanz classifications results high frequency of nerve compression within the carpel tunnel [8,9]. There are several adverse effects encountered during decompression procedures due to Lanz type III anomaly. These include inadvertent damage to the nerve during surgery for carpel tunnel syndrome, difficult endoscopic carpel tunnel decompression and needing to convert in to open carpel tunnel decompression [3,10]. Split median nerve at the wrist makes difficulty in identification of structures during traumatic repair of injuries at the wrist and complications in nerve anastomosis. However the type of median nerve split described in this case will not increase the risk of carpel tunnel syndrome or make any difference in carpel tunnel decompression as the split is limited only proximal to the flexure retinaculum. But this type of split median nerve will definitely cause difficulties in identification and repair of traumatic nerve and tendon injuries at the wrist.
Conclusion
Anatomic variations of the median nerve at the wrist are not uncommon and may lead to diagnostic confusion and present surgical risks if not recognized. Therefore the knowledge of the presence of such anomalous median nerve at the wrist is important not only for anatomists but also for radiologists who do imaging at the wrist to avoid misinterpretations of findings and for hand surgeons to avoid inadvertent damage to the nerve during carpel tunnel decompression and prevent mishaps during traumatic repair of tendons and nerves at the wrist.
References
- Lanz U. Anatomical variations of the median nerve in the carpal tunnel. Hand Surg Am. 1977; 2: 44-53.
- BD Chaurasia’s. Human Anatomy sixth edition upper limb and thorax. Median Nerve. 109-110.
- Sundaram SM, Madhan SJ, Kumar. Split median nerve with variation in its common digital branch – a case report; Neuroanatomy. 2008; 7: 15-16.
- Hizay LA. Sarikcioglu. A unique case with splitting of the median nerve by the ulnar artery. Rom J Morphol Embryol. 2011; 52: 723-724.
- Granec D, Bicanic G, Boric I, Delimar D. Bifid median nerve in a patient with carpal tunnel syndrome – correlation of clinical, diagnostic and intra operative findings: case report and review of the literature. Acta Clin Croat. 2012; 51: 667-671.
- Krol A, Palczak A, Kazimierz S. Split median nerve. A report of two cases; Folia Morphol. 64: 341-344.
- Walker FO, Cartwright MS, Blocker JN. Prevalence of bifid median nerves and persistent median arteries and their association with carpal tunnel syndrome in a sample of latino poultry processors and other manual workers. Muscle Nerve. 2013; 48: 539-544.
- Klauser AS, Halpern EJ, Faschingbauer R. Bifid Median Nerve in Carpal Tunnel Syndrome: Assessment with US Cross-sectional Area Measurement; Radiology. 2011; 259: 3.
- Bayrak IK, Bayrak AO, Kale M, Turker H, Diren B. Bifid Median Nerve in Patients with Carpal Tunnel Syndrome. J Ultrasound Med. 2008; 27: 1129- 1136.
- Iannicelli E, Chianta A, Salvini V. Evaluation of Bifid Median Nerve with Sonography and MR Imaging. J Ultrasound Med. 2000; 19: 481-485.