
Case Report
J Bacteriol Mycol. 2016; 3(2): 1026.
A Patient with Acute Promyelocytic Leukemia and Persistent Skin Lesions Following Thorn Injury
Sunil M¹, Tarand JJ² and Kontoyiannis DP³*
¹Byrd Regional Clinic and Hospital, Leesville, USA
²Division of Internal Medicine, Department of Infectious Diseases, The University of Texas M.D. Anderson Cancer Center, USA
³Division of Internal Medicine, University of Texas M.D. Anderson Cancer Center, USA
*Corresponding author: Kontoyiannis DP, Division of Internal Medicine, University of Texas M.D. Anderson Cancer Center, USA
Received: April 29, 2016; Accepted: June 06, 2016; Published: June 08, 2016
Abstract
A 64 year old male patient with recently diagnosed acute promyelocytic leukemia treated with arsenic, all-trans retinoic acid and gemtuzumab developed bilateral pulmonary infiltrates and alveolar hemorrhage. He was started on high dose prednisone. He also had prolonged severe neutropenia. There were asymptomatic lesions on his knees bilaterally for few weeks prior to current hospitalization. The skin lesions developed at site of thorn injury sustained when he worked in his garden. Skin biopsy revealed presence of fungal elements on H&E and GMS stain showed round elements. Culture on Sabaraud’s agar showed growth of mold identified as Alternaria. Alternaria are dematiaceous fungi, predominantly plant pathogens but an increasing cause of opportunistic infection in immunocompromised hosts. The case highlights infection due to an emerging opportunistic pathogen and illustrates importance of biopsy for innocuous appearing skin lesions in the immunocompromised patients.
Keywords: Leukemia; Alternaria; Skin lesions
Introduction
The genus Alternaria include nine species groups of dematiaceous fungi found worldwide in association with a wide variety of substrates [1]. Several Alternaria species mainly attributed to A. alternata or A. infectoria and a number of uncharacterized Alternaria isolates have been associated with infections or allergy reactions. They have become an increasingly recognized cause of infection in immunocompromised hosts which can range from allergic disorders and infections of skin and subcutaneous tissues to more invasive infections [2,3].
Case Presentation
A 64 years old Caucasian male diagnosed with Acute Promyelocytic Leukemia (APL), was treated with arsenic, All-Trans Retinoic Acid (ATRA) and gemtuzumab. His post chemotherapy course was complicated by pancytopenia, diffuse bilateral pulmonary infiltrates, hemoptysis and alveolar hemorrhage. He was placed on intravenous high dose methyl prednisone for 3 weeks. Additionally he had severe neutropenia with Absolute Neutrophil Count (ANC) <500 cells/μL for about 2 weeks. Patient had asymptomatic skin lesions on his knees that were present since a few weeks prior to current hospitalization. On inquiry, he was injured by thorns while working on his knees in the garden preceding the onset of skin lesions. The lesions crusted over and persisted. On exam, he was afebrile (on corticosteroids), in mild respiratory distress, had diffuse coarse rhonchi in his chest bilaterally and 15-20 skin lesions confined to both knees. These were non-tender erythematous papules with central hemorrhagic crusts about 4-8mm in size (Figure 1A). Lab results revealed total white cell count of 1.0 K/μL, ANC of 0.87, hemoglobin of 9.1 gm/dL, hematocrit of 27.8%, and platelets of 34 K/μL. He had a mild renal insufficiency and mild transaminitis with normal electrolytes, alkaline phosphatase and bilirubin. Chest X-ray showed bilateral diffuse airspace opacities. Skin biopsy from the knee lesion revealed a pseudoepitheliomatous epidermal hyperplasia with dermal acute inflammation. Fungal elements were identified on H & E section. GMS stain highlighted large round elements and rare toruloid septated hyphae (Figure 1B). The Fite and gram stains were negative for acid fast bacilli or bacteria respectively. Fontana-Masson special stain revealed pigmented fungal organisms as well which supported the diagnosis of a dematiaceous fungus. Culture from the biopsy grew mold on Sabauraud’s Emmons dextrose agar in 7 days, identified as Alternaria (Figure 1C). The patient was treated with liposomal amphotericin B and posaconazole. He had a bronchoscopy with BAL that was negative for fungi. His cutaneous lesions slowly improved over the ensuing weeks but due to significant respiratory complications from underlying disease he has had a prolonged course in the intensive care unit. He presently remains ventilator dependent but continues to slowly recover from his multisystem organ failure and is no longer neutropenic. His APL is in remission.
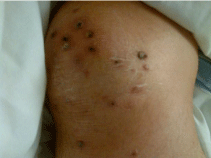
Figure 1A: Erythematous papules with central hemorrhagic crust over the
knee.

Figure 1B: Rounded fungal elements on GMS stain and on H & E stained
sections.
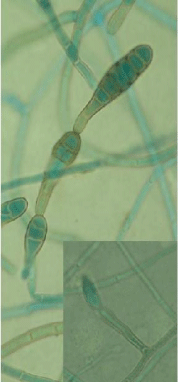
Figure 1C: Alternaria with Conidia arising in unbranched chains, golden
brown, smooth-walled or slightly verrucose, generally with 4-7 transverse and
one or two longitudinal septa.
Discussion
Alternaria are dematiaceous fungi that are predominantly plant pathogens [2,4,5] Alternaria spores are ubiquitous in the environment found both indoors as well as in soil and water. They are rare but increasingly recognized cause of opportunistic infection in humans including keratitis, sinusitis, osteomyelitis, peritonitis, skin and soft tissue infections especially in the immunocompromised and occasionally reported in immunocompetent individuals [2,3,5- 7]. In addition Alternaria has been known to cause allergic and hypersensitivity reactions in humans [4]. Most common species causing human infections include Alternaria alternata and Alternaria infectoria. Growth occurs as thick grey wooly colonies with a dark undersurface on Sabaraud’s dextrose agar. Most of the human infections have been cutaneous or mucosal, although rarely more invasive pulmonary infections have been reported in transplant patients [5,6,8]. Of the 56 patients with phaeohyphomycosis identified from 15 centers, frequent isolates were Alternaria (32%) [6]. Nine patients had cutaneous disease and ten had disseminated disease.
Traumatic inoculation is the usual mode of cutaneous infections with Alternaria. Cutaneous lesions reported range from papules, plaques, verucciform, chronic vegetative forms to ulcers and eczematous lesions. Diagnosis requires biopsy and positive cultures [5,7-9]. Pigmented hyphae elements may sometimes be detected on melanin staining (Fontana - Masson) indicating a dematiaceous fungus [10]. Molecular analysis by sequencing the rDNA Internal Transcribed Spacers (ITS) domain has been used to help with pathogen identification [9]. The optimal antifungal agent and duration of therapy for alternariosis is not standardized and use of various agents including itraconazole, amphotericin B, voriconazole and posaconazole has been reported. A study to assess the in vitro susceptibility profile of clinical Alternaria isolates showed that amphotericin B had the lowest MICs in vitro against the 2 species of Alternaria [11]. Among the azoles, posaconazole had the lowest MICs more so to Alternaria infectoria (GM=0.66mg/L) than Alternaria alternata (GM=1.23 mg/L). Echinocandins had good activity to Alternaria alternata but not against Alternaria infectoria.
Thorn injury is a known mode of entry for fungal pathogens, especially in the immunosuppressed patients. Sporothrix schenkeii, Fusarium and agents of eumycetoma and chromoblastomycosis are the most commonly reported fungi following plant thorn injury [12- 14]. In a case series of cutaneous alternariosis reported by Coutinho et al. [7], 2 patients had reported trauma from plants prior to onset of the lesions similar to our patient. Due to the potential for causing invasive disease especially in the immunocompromised one needs to have a high index of suspicion for early diagnosis. Finally, our case emphasizes the utility of skin biopsy in patients with leukemia and unexplained skin lesions [15].
References
- Lawrence DP, Rotondo F, Gannibal PB. Biodiversity and taxonomy of the pleomorphic genus Alternaria. Mycological Progress. 2015; 15: 1-22.
- Miceli MH, Lee SA. Emerging moulds: epidemiological trends and antifungal resistance. Mycoses. 2011; 54: 666-678.
- Ben-Ami R, Lewis RE, Raad II, Kontoyiannis DP. Phaeohyphomycosis in a tertiary care cancer center. Clin Infect Dis. 2009; 48: 1033-1041.
- Pastor FJ, Guarro J. Alternaria infections: laboratory diagnosis and relevant clinical features. Clin Microbiol Infect. 2008; 14: 734-746.
- Secnikova Z, Juzlova K, Vojackova N, Kazakov DV, Hoskova L, Fialova J, et al. The rare case of Alternaria alternata cutaneous and pulmonary infection in a heart transplant recipient treated by azole antifungals. Dermatol Ther. 2014; 27: 140-143.
- McCarty TP, Baddley JW, Walsh TJ, Alexander BD, Kontoyiannis DP, Perl TM, et al. Phaeohyphomycosis in transplant recipients: Results from the Transplant Associated Infection Surveillance Network (TRANSNET). Med Mycol. 2015; 53: 440-446.
- Coutinho I, Teixeira V, Gameiro A, Santiago F, Rodrigues L, Tomé R, Vieira R. Cutaneous alternariosis--a case series of an increasing phaeohyphomycosis. J Eur Acad Dermatol Venereol. 2015; 29: 2053-2054.
- Michelon M, Greenlaw S, O'Donnell P, Geist D, Levin NA. Multifocal cutaneous alternariosis in a 70-year-old Kenyan renal transplant patient. Dermatol Online J. 2014; 20.
- Gerdsen R1, Uerlich M, De Hoog GS, Bieber T, Horré R . Sporotrichoid phaeohyphomycosis due to Alternaria infectoria. Br J Dermatol. 2001; 145: 484-486.
- Sundaram C, Shantveer GU, Umabala P, Lakshmi V. Diagnostic utility of melanin production by fungi: study on tissue sections and culture smears with Masson-Fontana stain. Indian J Pathol Microbiol. 2014; 57: 217-222.
- Alastruey-Izquierdo A, Cuesta I, Ros L, Mellado E, Rodriguez-Tudela JL . Antifungal susceptibility profile of clinical Alternaria spp. identified by molecular methods. J Antimicrob Chemother. 2011; 66: 2585-2587.
- Palmore TN, Shea YR, Childs RW, Sherry RM, Walsh TJ. Fusarium proliferatum soft tissue infection at the site of a puncture by a plant: recovery, isolation, and direct molecular identification. J Clin Microbiol. 2010; 48: 338-342.
- Engle J, Desir J, Bernstein JM. A rose by any other name. Skinmed. 2007; 6: 139-141.
- Halpern M, Raats D, Lev-Yadun S. The potential anti-herbivory role of microorganisms on plant thorns. Plant Signal Behav. 2007; 2: 503-504.
- Farmakiotis D, Ciurea AM, Cahuayme-Zuniga L, Kontoyiannis DP. The diagnostic yield of skin biopsy in patients with leukemia and suspected infection. J Infect. 2013; 67: 265-272.