Research Article
Austin J Cancer Clin Res 2014;1(3): 1015.
HER-2 Expression in Secondary Circulating Prostate Cells does not Increase Risk of Biochemical Failure after Radical Prostatectomy for Prostate Cancer
Murray NP1,2,3*, Reyes E1,4, Fuentealba C1, Orellana N1 and Dueñas R1
1Department of Urology, Hospital Carabineros, Chile
2Department of Medicine, Universidad Mayor, Chile
3Institute of Bio-Oncology, Chile
4Department of Medicine, Universidad Diego Portales, Chile
*Corresponding author: Murray NP, Department of Medicine, Institute of Bio-Oncology, Hospital Carabineros, Simon Bolivar 2200 Providencia, Santiago, Chile
Received: June 24, 2014; Accepted: July 24, 2014; Published: July 25, 2014
Abstract
Introduction: There is evidence linking HER-2 expression in prostate cancer to disease progression and the development of androgen independent disease. HER-2 expression increases after androgen blockade and is associated with increased prostate cancer specific mortality. We present the effect of HER-2 expression in circulating prostate cells (CPCs) on the risk of biochemical failure and its association with standard clinic-pathological parameters.
Methods and patients: Blood samples were taken 4 monthly after radical prostatectomy to detect CPCs using anti-PSA and standard immunocytochemistry. Samples positive for CPCs underwent analysis for HER-2 expression using the HercepTest® kit. Standard clinicopathological parameters were recorded. Kaplan Meier plots determined the different biochemical failure free survival curves.
Results: 92 biochemical failure free men participated, 37/92(40.2%) of men had secondary CPCs detected. Biochemical failure was significantly more frequent in men CPC positive than those CPC negative (p=0.001). The expression of HER-2 in secondary CPCs did not increase biochemical failure free survival in comparison with men CPC (+) HER-2 (-).
Conclusion: In men without biochemical failure the expression of HER-2 positive CPCs did not increase the risk of developing biochemical failure.
Keywords: Prostate cancer; Circulating prostate cells; HER-2; Biochemical failure
Introduction
There is evidence linking the expression of HER-2 in prostate cancer to disease progression and the development of androgen independent disease. HER-2 is a member of the ErbB family of receptor tyrosine kinases and plays a crucial role in growth, differentiation, and motility of normal and cancer cells. HER-2 has been proposed as a survival factor for prostate cells in the absence of androgens, possibly by activating the androgen receptor [1-3]. In hormone-naive patients, whether in patients undergoing observation, or post-treatment with or without biochemical failure, the expression of HER-2 is infrequent both in the original tumor, circulating prostate cells (CPCs) and micro metastasis [2,4], whereas patients treated with androgen blockage have significantly increased levels of HER-2 expression in both the original tumor, CPCs and micro metastasis [2,4]. There is a suggestion that HER-2 may have a role in prostate cancer development, however its expression is variable, ranging between 0 to 100% depending on the HER-2 assay used [5] and gene amplification ranges from 0 to 53% [6,7]. Despite this discrepancy, there is still a consistent association between HER-2 over expression with a higher risk of death and recurrence in men with prostate cancer according to a meta-analysis [8]. Secondary CPCs are associated with a seven fold increase of biochemical failure after radical prostatectomy and CPC detection using standard immunocytochemisty is able to identify a high risk group for biochemical failure before there is a rise in the serum PSA [9].
We present a prospective study of the detection of secondary CPCs and the expression of HER-2 in men with a PSA <0.2ng/ml, the association with clinic-pathological parameters and the occurrence of biochemical failure.
Patients and Methods
Patient selection
From January 2009 to December 2011 blood samples from consecutive prostate cancer patients were prospectively collected for the purpose of detecting CPCs and evaluating whether these cells were correlated with clinical outcomes. All patients who had undergone radical prostatectomy at the author’s institution and all those seen during follow up were invited to participate. Samples were taken from men at least three months after surgery and considered to be without evidence of disease and repeated four monthly. This was defined as being bone scan negative and a serum PSA <0.20ng/ ml. A group of men with a serum PSA of 0.2-1.0ng/ml and bone scan negative were selected to represent men with biochemical failure. All samples were obtained after written informed consent and collected using protocols approved by the local ethics committee.
Sample collection and cell enrichment
8ml of venous blood was collected in tubes containing EDTA (Beckson-Vacutainer®). Mononuclear cells were obtained using gel differential centrifugation using Histopaque 1,077® (Sigma-Aldrich) at room temperature according to manufacturer’s instructions and finally washed 3 times in phosphate buffered saline pH 7.4 (PBS). The pellet was re-suspended in 100μl of autologous plasma and 25�l used to prepare each slide (sialinzed DAKO, USA). The slides were air dried for 24 hours and finally fixed in a solution of 70% ethanol, 5% formaldehyde and 25% PBS for 5 minutes and then washed 3 times with PBS.
Identification of CPCs
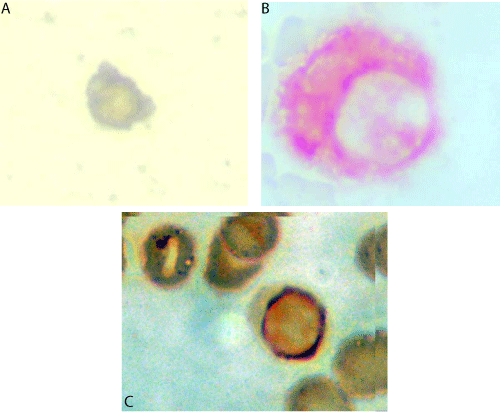
Slides were processed within 1 hour of fixation and incubated with anti-PSA clone 28A4 (Novocastra Laboratory, UK) in a concentration of 2.5 μg/ml for 1 hour at room temperature and identified using a detection system based on alkaline phosphatase-antialkaline phosphatase (LSAB2 DAKO, USA) with new-fuschin as the chromogen. To permit the rapid identification of positive cells there was no counter staining with Mayer’s hematoxilin. Levisamole (DAKO, USA) was used as an inhibitor of endogenous alkaline phosphatase. Positive and negative controls were processed in the same way. Definition of secondary CPCs using the criteria of ISHAGE was used to identify immunostained cells [10] (Figure 1A-B). A sample was classified as CPC positive if 1 cell PSA positive was detected.
Figure 1A: leucocyte. Figure 1B: PSA (+) CPC. Figure 1C: CPC HER-2 positive.
HER-2 immunostaining
Samples positive for CPCs underwent a second process using HercepTest®, HER-2 staining was classified as negative for 0 and 1+ staining and positive for 2+ and 3+ staining2 (Figure 1C). A sample was classified as HER-2 positive if there was 1 PSA positive cell staining HER-2 2+ or 3+.
Samples were analyzed at low power and photographed at a magnification of 400X with a Samsung Digimax D73 digital camera and processed using Digimax for Windows. The immunocytochemical processing and evaluation was carried out by a single person blinded to the clinical details.
Statistical methods
Descriptive statistics were, used to compare demographic and disease characteristics of patients with and without biochemical failure. Univariate comparisons were tested using Chi squared and Kaplan Meier methods were used to compare the unadjusted free from biochemical failure of patients with and without CPCs detected. Age, pathological stage (organ confined, non organ confined), pathological grade, margin status (positive, negative), capsule compromise (positive, negative), peri-neural, vascular and lymphatic infiltration (positive, negative) were compared with the presence/ absence of CPCs and with and without biochemical failure.
Because the time between radical prostatectomy and the blood sampling was not standardized, two separate models were considered. In the first model, the time under observation started at the date of radical prostatectomy. In the second the time under observation was started at the time of blood sampling post surgery. Patients who did not experience biochemical failure were censored at the date of last follow-up.
Results
114 men with a mean age of 71.5 ± SD 8.2 years participated. Table 1 shows the distribution of patients according to PSA levels, pathological stage at diagnosis and median time from surgery to blood sampling. Men in Group 1 had significantly less pT3 disease (p=0,04 Chi squared) then Group 2.
Group 1: PSA ≤0.20ng/ml
Group 2: PSA >0.20-1.00ng/ml
Total
N° Patients
92
22
114
Initial Stage
1
18
0
18
2
49
11
60
3
25
11
36
Median Gleason score (IQR)
6 (5-6)
6 (5-6)
Time from surgery (years)
3.8 ± 1.6
5.6 ± 3.6
Table 1: Demographic details of the study population.
Secondary CPCs were detected more frequently in men with biochemical failure 15/22 (68.2%) in Group 2 versus 37/92 (40.2%) men in Group 1 (p=0.02 Chi squared). 21/52 (40.4%) of men positive for secondary CPCs expressed HER-2, there was no significant difference in the frequency of HER-2 expression between men with or without biochemical failure; 17/37 (46%) in Group 1 compared with 4/15 (27%) in Group 2 (p=0.20 Chi squared).
Association of the presence of CPCs and clinicpathological parameters
Secondary CPCs were detected more frequently in patients with: positive margins compromised capsule, vascular and lymphatic infiltration but not with perineural infiltration (Table 2). There was a trend with increasing frequency of CPC detection with pathological stage, (p=0.002 Chi squared for trends) with a relative risk of 1.00, 3.63 and 10.83 for stage pT1, pT2 and pT3 respectively and with increasing Gleason score (p=0.015) with a relative risk of 1.00, 7.41, 4.00 and 44.00 for Gleason 4, 5+6, 7 and 8+9 respectively.
Clinical parameter
CPC (+)
CPC (-)
Margen (+)
Margen (-)
15
23
7
47
p=0.003
Capsule (+)
Capsule (-)
24
14
17
37
p=0.003
Perineural (+)
Perineural (-)
27
11
29
25
p=0.09
Vascular (+)
Vascular (-)
15
23
3
51
p=0.00005
Lymphatico (+)
Lymphatico (-)
13
25
4
50
p=0.001
Gleason 4
Gleason 5 +6
Gleason 7
Gleason 8 + 9
1
31
8
8
11���� RR 1.00
23���� RR 7.41
11���� RR 4.00
1������ RR 44.00
p=0.015 for trends
Table 2: Secondary CPC detection and association with clinical parameters.
HER-2 expression in secondary CPCs
There was no increased frequency of HER-2 expressing with increasing pathological stage (p=0.68 Chi squared for trends), being detected in 1/3, 11/29 and 9/21 CPC positive patients for stages 1, 2 and 3 respectively.
The expression of HER-2 in secondary CPCs was compared with the same clinical parameters (Table 3). There was no significant difference with respect to the clinic-pathological parameters between men with CPCs HER-2 positive or HER-2 negative except for vascular infiltration. Men with CPCs HER-2 positive had a higher frequency of tumors with vascular infiltration than men with CPCs HER-2 negative (p=0.02, Chi squared), and were older (p<0.033 T-test). The median serum PSA at the time of diagnosis was lower at the time of diagnosis in men with HER-2 posiitve CPCs.
Clinical Parameter
Age� (years)
Median PSA at diagnosis (ng/ml)
CPC HER-2 (+)
74.0 ± 7.9 years
6.01 (IQR 5.14-14.57)
CPC HER-2 (-)
69.5 ± 7.6 years
6.13 (IQR 5.07-8.17)
p<0.033
p<0.05
Margen (+)
Margen (-)
11
10
11
21
p=0.19
Capsule (+)
Capsule (-)
13
8
23
9
p=0.45
Perineural (+)
Perineural (-)
15
6
21
11
p=0.66
Vascular (+)
Vascular (-)
13
8
10
22
p<0.02
Lymphatic (+)
Lymphatic (-)
7
14
11
21
p=0.94
Gleason� 4
Gleason 5 + 6
Gleason 7
Gleason 8 + 9
2
11
5
3
0
22
4
6
p=0.91
Table 3: HER-2 expression and clinical parameters.
Biochemical failure and HER-2 expression in secondary CPCs
In the 37/92 subjects CPC positive and without biochemical failure at the start of the study, 27/37 (73%) experienced biochemical failure within 3 years. 11/18 (61%) of men CPC-HER-2 (+) and 16/20 (80%) of CPC-HER-2 (-) experienced biochemical failure (p=0.20, Chi squared). Her-2 positivity did not increase the frequency of biochemical failure in CPC positive men.
Frequency of biochemical failure in CPC positive and negative men with time from surgery
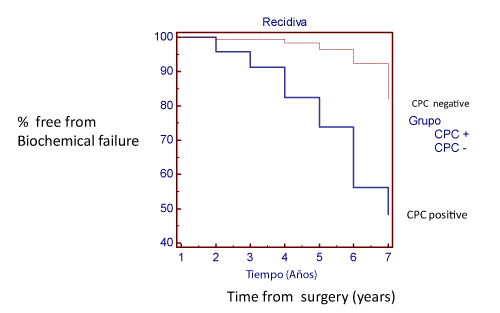
Men CPC positive had a higher frequency of biochemical failure during the first 5 years after surgery; however both CPC positive and negative men continued to experience biochemical failure after 5 years (Table 4 and Figure 2).
Figure 2: Kaplan Meier plot time free of biochemical failure from time of surgery.
0 years
1 year
2 years
3 years
4 years
5 years
6 years
7 years
CPC (+)
100% 38/38
37/37
26/31
24/28
18/24
13/17
9/14
6/7
CPC
(-)
100% 55/55
55/55
52/53
44/44
39/40
28/29
13/14
8/9
P=1.00
P=0.02
P=0.02
P=0.009
P=0.06
P=0.16
P=1.00
Table 4: Number of men without biochemical failure with time after radical prostatectomy.
Frequency of biochemical failure in CPC positive and negative men with time from first blood sample
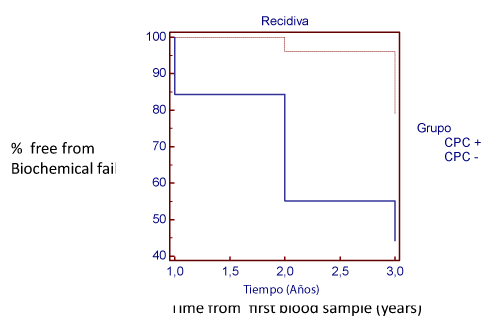
Men CPC positive had a higher frequency of biochemical failure at 1, 2 and 3 years of follow up (Table 5).
Figure 3: Kaplan Meier plot time free of biochemical failure from time of first blood sampling.
T= 0
T= 1 year
T=2 years
T= 3 years
CPC (+)
100%� (37/37)
74%��� (28/37)
45% (9/20)
20% (1/5)
CPC (-)
100%� (55/55)
100%� (55/55)
91/ (31/33)
77% (14/17)
p=0.00006
p=0.0001
p=0.02
Table 5: Frequency of men without biochemical failure comparing CPC (+) versus CPC with time from first blood sample.
Frequency of biochemical failure in CPC (+) HER-2 (+) and CPC (+) HER-2 (-) men with time from surgery
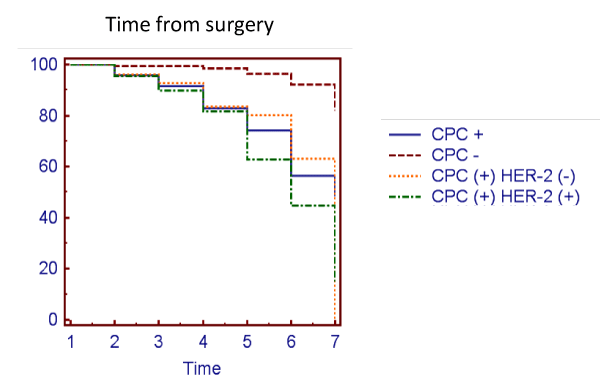
There was no difference in the frequency of biochemical failure from the time of surgery between men CPC (+) HER-2 (+) and men CPC (+) HER-2 (-), (Table 6). A Kaplan-Meier curve also failed to show a significant difference in biochemical free survival between CPC (+) HER-2 (+) and CPC (+) HER-2 (-) men. There remained a significant difference between these 2 groups of CPC (+) men and CPC (-) men (log rank p=0.04 and p=0.035 respectively) (Figure 4).
Figure 4: Kaplan-Meier plot of biochemical free survival from time of surgery in men CPC (+) HER-2 (+) and CPC (+) HER-2 (-).
1 year
2 years
3 years
4 years
5 years
6 years
7 years
CPC (+) HER-2 (+)
17/17
10/12
9/11
7/9
3/6
2/4
2/3
CPC (+) HER-2 (-)
20/20
16/19
15/17
11/15
10/11
7/10
4/4
p=1.00
p=1.00
p=1.00
p=1.00
p=0.10
p=0.58
p=0.42
Table 6: Number of men without biochemical failure with time after radical prostatectomy.
Frequency of biochemical failure in CPC (+) HER-2 (+) and CPC (+) HER-2 (-) men with time from first blood sample
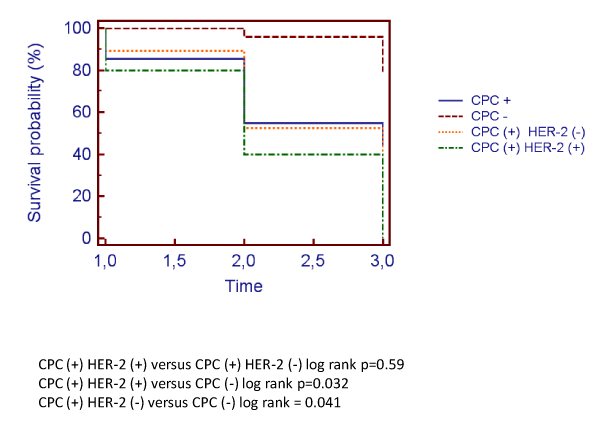
There was no significant difference in the frequency of biochemical free survival between men CPC (+) HER-2(+) and men CPC (+)HER-2 (-) at 1, 2 and 3 years after the taking of the first blood sample (Table 7). ). A Kaplan-Meier curve also failed to show a significant difference in biochemical free survival between CPC (+) HER-2 (+) and CPC (+) HER-2 (-) men. There remained a significant difference between these 2 groups of CPC (+) men and CPC (-) men (log rank p=0.04 and p=0.035 respectively) (Figure 5).
Figure 5: Kaplan-Meier plot of biochemical free survival from first blood sample in men CPC (+) HER-2 (+) and CPC (+) HER-2 (-).
1 year
2 years
3 years
CPC (+) HER-2 (+)
16/20
6/13
1/4
CPC (+) HER-2 (-)
12/17
3/7
0/1
Fisher Test
0.70
1.00
1.00
Table 7: Frequency of men without biochemical failure comparing CPC (+) HER-2 (+) versus CPC (+) HER-2(-) with time from first blood sample.
Discussion
HER-2 is a 185-kDa Tran’s membrane tyrosine kinase receptor and belongs to the epidermal growth factor family [11]. HER-2 is located on chromosome 17q21 and HER-2 signaling promotes cells proliferation through the RAS-MAPK pathway and inhibits cell death through the phosphatidylinositol 3 ’-kinase-AKT pathway [11]. Pre-clinical studies suggest that HER-2 expression plays a role in prostate cancer progression. Using a prostate cancer xenograft model it has been shown that androgen independent cancer cells have higher expressions than androgen dependent cancer cells, and that forced over-expression of HER-2 convert’s androgen dependent cells into androgen independent cells [3]. In the clinical, HER-2 has been proposed as a survival factor for prostate cells in the absence of androgens, possibly by activating the androgen receptor [1-3]. The proposed mechanism for the role of HER-2 in hormone escape is that it activates androgen receptor phosphorylation (via the MAPK or AKT pathways) which in turn maintains the androgen receptor integrity and thus its function in the absence of testosterone [12,13]. In prostate cell models it has been reported that, in androgen independent cell lines, HER-2 expression and AKT activation are increased, and the use of the anti-HER-2 drug trastuzumab can reverse this [14]. The use of androgen blockade has been shown to increase HER-2 expression and suggested that this therapy eliminates HER-2 cells thus decreasing the serum PSA in men with biochemical failure [14]. The same study showed that DES therapy did not increase HER-2 expression [4].
However, there is little known on the effect of HER-2 expression in men without androgen blockade. This study has shown that the presence of secondary CPCs increases with increasing serum PSA after radical prostatectomy, which suggests that with increasing disease (as measured by serum PSA levels) more prostate cancer cells enter the blood implying a more active disease. However, HER-2 expression was not significantly different between the three groups. This would suggest that in an environment with androgens HER-2 has little or no effect on this process of disease activity.
Except for perineural invasion the presence of secondary CPCs was associated with all the clinical and pathological parameters associated with increased risk of biochemical failure. The micro metastatic focus from which the secondary CPCs originated must have occurred pre-surgery and thus would be associated with those risk factors of dissemination.
In patients who had secondary CPCs expressing HER-2 there was an increased risk of vascular infiltration in the original tumor, as compared with men with CPCs HER-2 negative. Patients with HER- 2 positive CPCs were older at the time of diagnosis. There were no differences between men with HER-2 positive and negative CPCs with regards to the other clinical parameters. Gleason score was not related to HER-2 expression in CPCs, although the median serum PSA level at the time of diagnosis was lower in men with HER-2 positive CPCs.
It has been reported that HER-2 expression in bone marrow micro metastasis is higher than the original tumor in breast cancer and is associated with early dissemination and metastasis [15,16]. In patients prior to radical cystectomy for urothelial carcinoma of the bladder, HER-2 expression in circulating tumor cells was higher than in the tumor original [17]. Together these finding suggest that HER-2 positive cells in the original tumor have a higher capacity of vascular dissemination than HER-2 negative cells.
The presence of secondary CPCs is associated with a higher risk of biochemical failure than patients CPC negative independent of the serum PSA at the time of sampling, even men with a serum PSA of <0.02 had a higher risk of progression. The expression of HER- 2 in patients’ secondary CPC positive did not influence the risk of biochemical failure as determined by Kaplan-Meyer plots.
Conclusion
In men without androgen suppression, the presence of secondary CPCs is associated with the traditional risk factors for biochemical failure in men after radical prostatectomy for prostate cancer. However men secondary CPC positive have a 7 fold increase of biochemical failure compared with secondary CPC negative men within 2 years of sampling. Men with HER-2 positive secondary CPCs had a higher risk of vascular infiltration in the primary tumor compared with HER-2 negative men but the risk of biochemical failure was similar. Thus in an environment with androgens present the expression of HER-2 on patient outcome was minimal. Thus anti- HER-2 therapy in these patients may not be of benefit.
Acknowledgement
Mrs Ana Maria Palazuelos for her help in the study. The study was funded by a grant from the Hospital de Carabineros.
References
- Signoretti S, Montironi R, Manola J, Altimari A, Tam C, Bubley G, et al. Her-2-neu expression and progression toward androgen independence in human prostate cancer. J Natl Cancer Inst. 2000; 92: 1918-1925.
- Osman I, Scher HI, Drobnjak M, Verbel D, Morris M, Agus D, et al. HER-2/neu (p185neu) protein expression in the natural or treated history of prostate cancer. Clin Cancer Res. 2001; 7: 2643-2647.
- Craft N, Shostak Y, Carey M, Sawyers CL. A mechanism for hormone-independent prostate cancer through modulation of androgen receptor signaling by the HER-2/neu tyrosine kinase. Nat Med. 1999; 5: 280-285.
- Murray NP, Badinez LV, Dueñas RR, Orellana N, Tapia P. Positive HER-2 protein expression in circulating prostate cells and micro-metastasis, resistant to androgen blockage but not diethylstilbestrol. Indian J Urol. 2011; 27: 200-207.
- Ratan HL, Gescher A, Steward WP, Mellon JK. ErbB receptors: possible therapeutic targets in prostate cancer? BJU Int. 2003; 92: 890-895.
- Montironi R, Mazzucchelli R, Barbisan F, Stramazzotti D, Santinelli A, Scarpelli M, et al. HER-2 expression and gene amplication in pTa Gleason score 6 prostate cancer incidentally detected in cystoprostatectomy: comparison with clinically detected androgen dependent and androgen independent cancer. Hum Pathol. 2006; 37: 1137-1144.
- Liu HL, Gandour-Edwards R, Lara PN Jr, de Vere White R, LaSalle JM. Detection of low level HER-2/neu gene amplification in prostate cancer by fluorescence in situ hybridization. Cancer J. 2001; 7: 395-403.
- Neto AS, Tobias-Machado M, Wroclawski ML, Fonseca FL, Teixeira GK, Amarante RD, et al. Her-2/neu expression in prostate adenocarcinoma: a systematic review and meta-analysis. J Urol. 2010; 184: 842-850.
- Murray NP, Reyes E, Orellana N, Fuentealba C, Badinez L, Olivares R, et al. Secondary circulating prostate cell in prostate cancer patients after radical prostatectomy and without evidence of disease predict biochemical failure. TWSJ Urol. 2013.
- Borgen E, Naume B, Nesland JM, Kvalhein E, Beiske K, Fodsted O, et al. Standardization of the immunocitochemical detection of cancer cells in bone marrow and blood: Establishment of objec–tive criteria for the evaluation of immunostained cells. ISHAGE Cytotherapy. 1999; 1: 377-388.
- Hudis CA. Trastuzumab--mechanism of action and use in clinical practice. N Engl J Med. 2007; 357: 39-51.
- Wen Y, Hu MC, Makino K, Spohn B, Bartholomeusz G, Yan DH, et al. HER-2/neu promotes androgen-independent survival and growth of prostate cancer cells through the Akt pathway. Cancer Res. 2000; 60: 6841-6845.
- Yeh S, Lin HK, Kang HY, Thin TH, Lin MF, Chang C. HER2/Neu signal cascade to androgen receptor and itscoactivators: a novel pathway by induction of androgen target genes through MAP kinase in prostate cancer cells. Proceedings of the National Academy of Sciences of the United States of America. 1999; 96: 5458–5463.
- C. Guyader J, Ceraline E, Gravier A, Morin S, Michel E, Erdmann, et al. Risk of hormone escape in a human prostate cancer model depends on therapy modalities and can be reduced by tyrosine kinase inhibitors. Plos ONE, 2012; 7.
- Tiwari RK, Borgen PI, Wong GY, Cordon-Cardo C, Osborne MP. HER-2/neu amplification and overexpression in primary human breast cancer is associated with early metastasis. Anticancer Res. 1992; 12: 419-425.
- Fehm T, Müller V, Aktas B, Janni W, Schneeweiss A, Stickeler E, et al. HER2 status of circulating tumor cells in patients with metastatic breast cancer: a prospective, multicenter trial. Breast Cancer Res Treat. 2010; 124: 403-412.
- Rink M, Chun FK, Dahlem R, Soave A, Minner S, Hansen J, et al. Prognostic role and HER2 expression of circulating tumor cells in peripheral blood of patients prior to radical cystectomy: a prospective study. Eur Urol. 2012; 61: 810-817.