
Research Article
Austin Cardio & Cardiovasc Case Rep. 2016; 1(2): 1010.
Localized Pericarditis Induced by an Expanded Polytetrafluoroethylene Membrane used for Constrictive Pericarditis - Two Case Reports and Short Review
Misawa Y¹*, Kawada M² and Endo S³
¹Division of Cardiovascular Surgery, Jichi Medical University, Japan
²Division of Pediatric and Congenital Cardiovascular Surgery, Jichi Medical University, Japan
³Division of General Thoracic Surgery, Jichi Medical University, Japan
*Corresponding author: Yoshio Misawa, Division of Cardiovascular Surgery, Jichi Medical University, Japan
Received: June 24, 2016; Accepted: July 13, 2016; Published: July 15, 2016
Abstract
Cardiac injury is associated with a high morality. The importance of protecting the heart during repeat sternotomy should be emphasized. An expanded Polytetrafluoroethylene (e-PTFE) membrane is widely used for closure of the pericardium. We review the clinical effectiveness and adverse outcomes of the e-PTFE membrane. Although the e-PTFE membrane is effective and useful for repeat sternotomy, some complications, such as pericardial cyst formation, can occur in patients with constrictive pericarditis or repeat cardiac surgery.
Keywords: Constrictive pericarditis; Expanded polytetrafluoroethylene membrane; Heart surgery; Closure of the pericardium; Cardiac injury
Abbreviation
E-PTFE: Expanded Polytetrafluoroethylene
Introduction
Risk factors for cardiac injury during repeat sternotomy include a history of a previous operation, aneurysm of the ascending aorta, and enlargement of the atrium [1]. Cardiac injury is associated with a high morality. Therefore, protecting the heart during repeat sternotomy is important [2]. An expanded polytetrafluoroethylene (e-PTFE) membrane is widely used for closure of the pericardium, preventing cardiac injury during repeat sternotomy for additional procedures and/or repeated heart diseases. Some investigators have reported their experiences regarding operations for congenital heart diseases using e-PTFE membranes; others did those for acquired heart diseases [3-6].
Materials and Methods
We reviewed studies related to pericardial complications induced by an e-PTFE membrane. A survey was conducted for articles published after 1987 on PubMed. Our recent case was also included.
Results and Discussion
Clinical effectiveness
Jacobs et al. showed no preoperative complications or deaths attributable to the e-PTFE membrane in an entire series of 1085 patients [3]. Their study included 4769 patient-years of follow-up. They reported that there were no infections or other complications related to the use of the e-PTFE membrane during the follow-up. At reoperation, they recognized that the membrane was clearly separate from the sternum and resembled a sheet of clear plastic overlying the heart. Additionally, no problematic adhesions were observed between the membrane and the heart or between the membrane and the chest wall. They concluded that use of the e-PTFE membrane is safe and effective in helping to prevent cardiac injury during repeat sternotomy.
Loebe et al. reported the use of e-PTFE membranes in 324 patients with congenital heart disease [4]. One patient developed postoperative mediastinitis, but they showed that this incident was not different from that of patients without these membranes. Another patient had a superficial wound infection that was revised without a repeat sternotomy. One patient had pericardial effusion requiring insertion of a chest tube. In their series, 17 patients underwent a repeat sternotomy for a mean of 20 months after the original repair without any cardiac injury.
Amato et al. studied 96 patients with congenital heart disease who underwent pericardial closure with an e-PTFE membrane and seven patients who had a second cardiac operation [5]. They concluded that reoperation did not cause any adhesions to the chest wall or epicardium, and visualization of the cardiac surface, especially the coronary vessels, was not obscured. Minale et al. recommended the routine use of the e-PTFE membrane for complete closure of the pericardium in patients with a high probability of reoperation after implantation of bioprostheses and other acquired cardiac diseases [6].
Adverse outcomes
Sakuma et al. performed histological examinations of implanted e-PTFE membranes in dogs [7]. They showed that e-PTFE membranes produced severe adhesions to the heart and pleura with a more prominent inflammatory reaction. Additionally, absorbable pericardial substitutes were completely absorbed by 24 weeks after implantation, and were replaced with a fibrous membrane. Therefore, they recommended synthetic bioabsorbable polymers for closure of the pericardium.
Heydom et al. compared the e-PTFE membrane with bovine and equine epicardial patches [8]. They showed that adhesions to portions of the suture line required sharp dissection by 18 months after implantation as pericardial substitutes in each group. However, they recommended the e-PTFE membrane if there was concern about the possibility of calcification.
In 2001, we reported a unique case with late pericarditis secondary to pericardial patch implantation [9]. A 50-year-old man presented with signs of right heart failure due to localized pericarditis. The pericarditis was supposed to be secondary to implantation 25 years prior of an e-PTFE membrane following pericardiectomy for primary constrictive pericarditis. The clinical symptoms resolved completely after removal of the membrane. Recently, we experienced another similar case. A 23-year-old woman presented with right heart failure with pleural effusion and pretibial pitting edema. At the age of 2 years, she underwent closure of ventricular and atrial septal defects. When she was 13 years old, she underwent pericardiectomy for constrictive pericarditis. The pericardium was then closed with e-PTFE membranes because of the possible risk of reoperation for mitral valve regurgitation. Chest computed tomography showed a pericardial cyst below the sternum (Figure 1). A cardiac catheterization study was compatible with constrictive pericarditis, showing a typical dip-and-plateau pattern of right ventricular pressure. Our two cases had a history of constrictive pericarditis. We recommend avoiding the use of an e-PTFE membrane for closure of the pericardium in these types of cases.
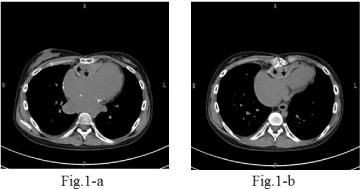
Figure 1: Preoperative chest computed tomography. A cystic lesion (black arrows) can be seen beneath the sternum, compressing the right atrium and ventricle.
Conflict of interest: none declared. Funding: This study received no specific grant from any funding agency.
Bergoënd et al. reported a unique case of localized constrictive pericarditis after an e-PTFE pericardial substitute [10]. A 65-yearold patient had undergone repeat aortic valve replacement 12 years before he presented with cardiac decompensation. At the operation, the epicardium underneath the e-PTFE membrane was white and had slightly thickened fibrinous adhesions, causing restriction of right ventricular diastolic expansion. Repeat open heart surgery could contribute to inflammatory changes of the epicardium and/or pericardium.
Long after pericardiectomy and pericardial closure with an e-PTFE membrane in 3 cases including our 2, the localized pericarditis occurred. A residual inflammatory change can exist because the dorsal portion of the pericardium was left un-resected. The implanted e-PTFE membrane might prevent exudates from being absorbed, resulting in fluid collection around the membrane. Further investigation is required to reveal the relationship.
Conclusion
Closure of the pericardium using a pericardial substitute at open heart surgery could avoid cardiac injury during repeat sternotomy. Routine use of the e-PTFE membrane for complete closure of the pericardium in patients with a high probability of reoperation is recommended. However, some adverse complications of pericardial cysts and other inflammatory changes can occur in patients with constrictive pericarditis or those who have repeated cardiac surgery.
References
- Loop FD. Catastrophic hemorrhage during redo sternotomy. Ann Thorac Surg 1984; 37: 271-272.
- Imran Hamid U, Digney R, Soo L, Leung S, Graham AN. Incidence and outcome of re-entry injury in redo cardiac surgery: benefits of preoperative planning. Eur J CrdiothoracSurg. 2015; 47: 819-823.
- Jacobs JP, Iyer RS, Weston JS, Amato JJ, Elliott MJ, de Leval MR, et al. Expanded PTFE membrane to prevent cardiac injury during resternotomy for congenital heart diseases. Ann Thorac Surg. 1996; 62: 1776-1782.
- Loebe M, Alex-Meskhishvili V, Weng Y, Hausdorf G, Hetzer R. Use of polytetrafluoroethylene surgical membrane as a pericardial substitute in the correction of congental heart defects. Tex Heart Inst J. 1993; 20: 213-217.
- Amato JJ, Cotroneo JV, Galdieri RJ, Alboliras E, Antillon J, Vogel RL. Experience with the polytetrafluoroethylene surgical membrane for pericardial closure in operations for congenital cardiac defects. J Thorac Cardiovasc Surg. 1989; 97: 929-934.
- Minale C, Nikol S, Hollweg G, Mittermayer C, Messmer BJ. Clinical experience with expanded polytetrafluoroethylene Gore-Tex surgical membrane for pericardial closure: a study of 110 cases. J Card Surg. 1988; 3: 193-201.
- Sakuma K, Iguchi A, Ikada Y, Tabayashi K. Closure of the pericardium using synthetic bioabsorbable polymers. Ann ThoracSurg. 2005; 80: 1835-1840.
- Hydom WH, Daniel JS, Wade CE. A new look at pericardial substitute. J Thorac Cardiovasc Surg. 1987; 94: 291-296.
- Endo S, Saito N, Misawa Y, Y Sohara. Late pericarditis secondary to pericardial patch implantation 25 years prior. Eur J Cardiothorac Surg. 2001; 20: 1059-1060.
- Bergoënd E, Marchand M, Casset-Senon D, Cosnay P. Localized constrictive pericarditis after Gore-Tex pericardial substitution. Interact Cardio Vasc Thorac Surg. 2010; 10: 813-815.