
Research Article
Chronic Dis Int. 2016; 3(1): 1020.
Evaluation of the Results of Repair of Flexor Digitorum Superficialis and Flexor Digitorum Profundus Tendon Injury of the Hand at Zone-V
Rahman MT¹*, Alim MA², Datta NK³, Uddin MJ4, Hossain MA5, Sharmin R6, Faisal MA7, Tarik MM8 and Nabi SG9
1Adhunic Sadar Hospital, Bangladesh
2Institute of Public Health Nutrition, Bangladesh
3Department of Orthopaedic Surgery, Bangabondhu Sheikh Mujib Medical University, Bangladesh
4Department of Orthopaedic Surgery, Cox’s Bazar Medical College Hospital, Bangladesh
5Department of Orthopaedic Surgery, Bangladesh
6Forensic Medicine, Dhaka Medical College, Bangladesh
7Department of Orthopaedic Surgery BSMMU, Bangladesh
8Tanor Upazila Health Complex, Bangladesh
9Mugda Medical College, Bangladesh
*Corresponding author: Rahman MT, Junior Consultant, Adhunic Sadar Hospital, Natore, Bangladesh
Received: April 16, 2016; Accepted: July 12, 2016; Published: July 13, 2016
Abstract
Hand is the most important organ of a man. For proper functioning of hand intactness of tendons (both flexor and extensor) are essential. Injury to the tendons in hand produces nonfunctioning or deforming hand. Deformity becomes worse when tendon injury occurs in zone- v (especially when injury occurs in flexor digitorum superficialis and flexor digitorum profundus). Flexor tendon injury is one of the most common hand injuries. Zone-v flexor tendon injuries may involve major nerves and arteries as well as the wrist and finger flexors. Total 17 patient’s repaired zone-v flexor tendons injuries were followed up for 2.5 to 12 months. The postoperative rehabilitation program consisted of a regime of modified kleinert technique was applied. Outcome parameters of the hand functions were measured according to the Buck-Gramco (1983) assessment system, grip and key pinch strength values, and return to work status. Out of 17 patients functional results were excellent in 4 (23.5%) patients, good in 10 (64.7%), fair in 2 (11.8%), and poor in 1 (5.9%) patient. No tendon ruptures or tenolysis occurred in our series of 17 patients who were employed at the time of injury, 14 patients returned to their original occupations. Satisfactory functional results can be obtained when proper surgical technique was coupled with careful postoperative management in patients with zone-v flexor tendon injuries.
Keywords: Flexor digitorum superficialis; Flexor digitorum profundus; Repair; Zone-v; Bangladesh
Introduction
Hand is the medium of introduction to the outside world. Its unique repertoire of pre-hensive movements and tactile activity sets us apart from all other species. The hand is the sophisticated and highly specialized organ, as it has grasping, pinching, and hooking functions, carried out by musculotendinous units. It can give information about the position, size, and shape of an object by its highly developed sensory mechanism and described as third eye. Flexor tendon injury is one of the most common hand injuries. Surgical repair of flexor tendon requires an exact knowledge of anatomy, careful adherence to some basic surgical principles, sound clinical judgment, strict atraumatic surgical technique and a well planned post operative programme. Hand function will be grossly impaired if flexor tendon is injured as muscle activity is finally carried out by intact tendon attached to the bone. For injured flexor tendon in the hand, the goal of treatment is recovery of functionally acceptable digital motion with intact tendon. Repair of all divided flexor tendons in zone-v has been encouraged because of the contributions of the Flexor Digitorum Superficialis (FDS) tendons to grip strength, their action in making pinch and flexion of the Proximal Interphalangeal (PIP) joint more stable and their effect in providing superior individual finger flexion.
Repair of flexor tendon in zone-v is easier than zone-II because presence of pulleys, which maintain gliding and prevent of bowstring effect of tendon during flexion and extension of fingers. If pulleys are injured, first reconstruct the pulleys then tendon by tendon graft. In zone-v tendon excursion is more than zone-II that’s why tendon repair is easier by positioning of hand.
Hand is the most important organ of a man. For proper functioning of hand intactness of tendons (both flexor and extensor) are essential. Injury to the tendons in hand produces nonfunctioning or deforming hand. Deformity is more when tendon injury occurred in zone-v (especially when injury occurs in FDS and Flexor Digitorum Profundus (FDP)). Deformed or nonfunctioning hand of a man produces burden not only to the family but also to the society. With the development of human civilization or the development of medical science day by day injured hand can be repaired. After repair of tendons in hand by proper technique hand function can be normal or near to normal and patient can able to re-back his/her normal job. Although there are several retrospective series of zone-v flexor tendon injuries [1-4], they have concentrated largely on the injuries to the median and ulnar nerves and not on injuries of the finger flexors. To the best of our knowledge no such work has been done in Bangladesh.
Therefore, the present work was carried out to evaluate the beneficial effect of repair of FDS and FDP tendon injury of the hand at zone-v.
Methods and Materials
A prospective study was carried out between January 2008 and December 2009 at Bangabandhu Sheik Mujib Medical University, Dhaka, Bangladesh. Within the study period 31 patients were treated with lacerations (sharp weapon) involving the flexor aspect of the wrist and /or distal third of the forearm. Of them 23 patients were selected for this study. Out of 23 patients 21 were included in the study had complete division of at least one digital flexor tendon. But two patients were below 12 years with a glass laceration of the wrist were excluded as they were not expected to comply with post operative physiotherapy regimen. Finally 19 patients were eligible for the study however, among them two failed to return for follow up for a minimum period of 2.5 months. Therefore, 17 patients (77% follow up rate) with lacerations of the flexor aspect of the wrist or distal forearm who had a total of 61 FDS and 51 FDP divisions were reviewed. The patients were followed up for 2.5 to 12 months. The deformity was determined by Buck-Gramco (1983) evaluation criteria [5].
Details of tendon repaired procedure
All patients were operated as the routine cases by general anesthesia. Patient was supine in position on the table with injured limb on side trolley at right-angle to body. Tourniquet was applied and continued for 75 minutes and released for 5-10 minutes and reapplied when needed. Painting of the limb was done by povidone iodine after soap water washing. The cut tendons were exposed by Lazy-s incision. Skin and palmar fascia were dissected in a single layer, and tendon sheath and neurovascular bundles were carefully identified and protected. Proximal and distal end were identified. If needed proximal cut ends were exposed through extending the incision proximally to the forearm. All tendons except palmaris longus were repaired by 4 ‘0’ atraumatic prolene for core suturing and 6 ‘0’ prolene for epitendinous suturing. After exposing both the cut ends were repaired by modified Kessler’s method with epitendinous suture by prolene. Finally skin was closed by interrupted sutures with a drain in situ.
Tension measurement: Full traction was applied to FDP musculotendinous unit and then released 20 percent tension, and attached. If tension would adequate, the fingers were extended when wrist was passively flexed.
Postoperative management
The patients were examined at the evening for vital signs, such as pulse, blood pressure, respiration, swelling of the hand, circulation of the fingers and collection in the drain. On the 2nd Post Operative Day (POD) drain was removed, on 3rd or 4th POD bulky dressing was replaced by light one and advised for passive flexion and active extension of the fingers in the plaster slab for 2 weeks. On the 12th POD stitches were removed and active contraction of flexor muscles of forearm were advised with wrist and fingers in fist position along with passive flexion and active extension of fingers and were advised to attend after 3 weeks outpatient department. At the end of 3 weeks, the patients were advised for controlled active flexion of the fingers to reduce the distance between fingers tip and palm by measuring the breadth of the fingers of other hand. During this period, patients were advised to remove the cast intermittently for 3 times a day and warm water and wax bath were advised at home or at physiotherapy department. They were also instructed to do gradual extension of the wrist with the fingers in passive flexion to improve the gliding of tendons and to maintain tendon length. After exercise, re-application of the cast was advised. At one month the patients were advised to remove the cast at day time and controlled active flexion exercise to continue. Passive hyperextension was strictly forbidden. Patients were also advised for deep friction massage, controlled passive extension of the fingers and to apply cast at bed time. After 6 weeks the cast was totally discarded and patients were instructed to start light activity like to hold glass, tea cup etc. At the end of 8 weeks the grip strengthening of the fingers along with controlled hyperextension of the fingers was emphasized. Grip strengthening was included squeezing of sponge roll and table pulley activity. Heavy resistance exercise was advised after 3 months and emphasis was on return to work.
In this series, total 17 patients were included and operated. The man age of the patients was 18 years. Among them, 2 (11.8%) patients were within 11-20 years of age group, 8 (47.1%) in between 21-30 years and 4 (23.5%) above 31 to 40 years, 2 (11.8%) patients were within 41-50 years, only 1 patient was within 51-60 years. Male patients were predominant (70.6%). More than half (52.9%) of the patients were businessmen and service holders. Right hand was involved over three-fourths (76.5%) cases. More than half (58.8%) injury was occurred due to broken glasses followed by machinery injury (17.7%). In this series, none of the patients were treated before the first 2 weeks of injury, 7 (41.2%) patient was operated within 5-8 weeks interval, 3 (17.7%) was operated within 9-12 weeks interval, 2 (11.8%) between 13-16 weeks, 1 (5.9%) between 17-20 weeks, 4 (23.5%) between 21-24 weeks. In case of 12 (70.6%) patients injury was associated with nerve involvement. Twenty nine percent of the patients were treated between 17-24 weeks interval since injury. Nearly half (47.1%) of the patients were followed up for the lowest duration 2.5 - 6 months after operations. However, 29.4% of the patients were followed up after operations for the highest duration 11 - 12 months. Socio-demographic with other characteristics is shown in the Table 1.
Variables
Frequency
Percentage
Age group (years)
11-20
2
11.8
21-30
8
47.1
31-40
4
23.5
41-50
2
11.8
51-60
1
5.9
Sex
Male
12
70.6
Female
5
29.4
Occupation
Businessman
5
29.4
Service-holder
4
23.5
Student
4
23.5
Housewife
3
17.7
Farmer
1
5.9
Side of involvement
Right hand
13
76.5
Left hand
4
23.5
Mode of injury
Sharp cut (knife)
02
11.8
Broken glass
10
58.8
Machinery injury (sharp weapon)
03
17.7
Self inflicted
02
11.8
Time interval between injury and operation (weeks)
2-8
7
41.2
9-12
3
17.7
13-16
2
11.8
17-20
1
5.9
21-24
4
23.5
Associated nerve injury
Present
12
70.6
Absent
5
29.4
Duration of follow-up (months)
2.5-6
8
47.1
7-8
1
5.9
9-10
3
17.6
11-12
5
29.4
Table 1: Socio demography of patients.
In case of flexor tendon division of 5 patients sustained division of the FDS tendons to 15 fingers but no division of FDP tendons and constitute the “FDS injuries only” group. The remaining 12 patients, who constitute the “FDS+FDP injuries” group sustained division of a mixture of 46 FDS and FDP tendons, with 4 fingers suffering division of FDS tendons only, no fingers suffering division of FDP tendons only, and 40 fingers suffering division of FDS and FDP tendons. In all, 19 fingers suffered division of FDS only, no finger suffered division of FDP tendons only, and 40 fingers suffered division of FDS and FDP where the tendons passed through 17 wrists and distal forearm included in this study. Flexor tendon division is shown in the Table 2.
No of wrists
Total no of fingers with flexor tendon division
No of fingers with FDS division only
No of fingers with FDP division only
No of fingers with FDS+FDP division
All injuries
17
61
19
0
40
“FDS injuries only” group
5
15
15
“FDS+FDP injuries” group
12
46
4
0
40
Table 2: Flexor tendon division (n= 17).
In the Table 3 multiplicity of divided digital flexor tendons per wrist shows all injuries included 5 FDS injury only and 12 FDS +FDP injuries. In case of FDS injury only, two FDS injury: 2, three FDS injury number: 1 and four FDS injury were 2. FDS+FDP injuries number were 10.
No of wrists with division of FDS
No of wrists with division of FDP
One FDS tendon
Two FDS tendons
Three FDS tendons
Four FDS tendons
One FDP tendon
Two FDP tendons
Three FDP tendons
Four FDP tendons
All injuries (n=17)
0
2
3
12
0
0
0
10
“FDS injuries only” group (n=5)
0
2
1
2
“FDS+FDP injuries” group (n=12)
0
0
2
10
0
0
0
10
Table 3: Multiplicity of divided digital flexor tendons per wrist (n=17).
Incidence of involved fingers is shown in the Table 4. The number of FDS division was 10 that involved in index finger and independent FDS action 5 (50%), index (adjusted) FDS division 6 and independent FDS action 4 (66%), number of FDS division in middle finger 15 and independent FDS action 10 (66%), number of FDS division in ring finger14 and independent FDS action 9 (64%), number of FDS division in little finger 9 and independent FDS action 5 (55%), in little fingers (adjusted) FDS division 7 and independent action 3 (42%) in this series.
Finger
No with FDS divisions
No. of these with independent FDS action (%)
Index
10
5 (50)
Index (adjusted)*
6
4 (66)
Middle
15
10 (66)
Ring
14
9 (64)
Little
9
5 (55)
Little (adjusted)*
7
3 (42)
*Adjustment to allow for those fingers without independent FDS action whom there was also no independent FDS action of the corresponding contra lateral fingers.
Table 4: Distribution of involved fingers.
In this series involvement of total wrists were 17 in number, among them spaghetti wrists 10, non-spaghetti wrists 7, average structures were divided in each wrist was 8 in number. FDS injuries occurred in 5 wrists, 6 wrists were average structures divided, FDS and FDP injuries occurred in total 12 wrists, among them spaghetti wrist 10, non-spaghetti wrists 2, average 9 structures were divided, which is shown in the Table 5.
Total no of wrists
Average no of structures divided
No of spaghetti wrists*
No of non spaghetti wrists
All injuries
17
8
10
7
FDS injuries only
5
6
0
5
FDS+FDP injuries
12
9
10
2
*Spaghetti wrists means 3-10 structures are divided in wrist (structures are nerve, artery and tendons).
Table 5: Number of Longitudinal Structure Involve In Wrists (Spaghetti or Non-Spaghetti Wrists).
We identified two patients with neurological deficit, two adhesion formations, and only one with ugly scar as the post operative complications (Table 6).
Complications
Number of patients
Percentage
Neurological deficit
2
11.8
Ugly scar
1
5.9
Adhesion formation
2
11.9
Table 6: Distribution of complications after operation (n=17).
In this series 17 (100) patients had motor involvement (grip) pre-operatively. While after operation 14 (82.35%) had no motor involvement (grip) and 3 (17.65%) patients had residual involvement. Here very highly significant difference was observed (p < 0.001). Motor power (grip) of the hand is reported in the Table 7.
Outcome
Number of patients
Percentage
Excellent
4
23.5
Good
10
58.8
Fair
2
11.8
Poor
1
5.9
Statistical analysis
Table 7: Final functional outcome by Buck-Gramco (1983) evaluation criteria (n= 17).
Frequency n (%)
p-value
Satisfactory
(Excellent + Good)
14 (82.3)
< 0.001
Unsatisfactory
(Fair + Poor)
3 (17.7)
Statistical analysis was done by paired t- test.
Table 7 & off:
Functional outcome was significantly satisfactory (excellent + good) in 82.3% of patients (p < 0.001); fair 11.8% and poor was 5.9%.
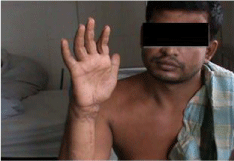
Figure 1: Pre-operative photograph.
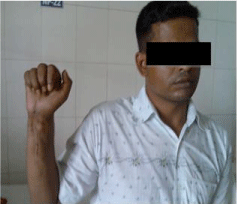
Figure 2: Post operative follow up.
Discussion
Injuries to the flexor tendons are common. Each specific movement of the hand relies on the finally tuned biomechanical interplay of the intrinsic and extrinsic musculotendinous forces. Flexor tendon injury of hand at zone-v always presented as a problem in the management. Most of the times, the injury involves both tendons that causes significant morbidity to the patients due to loss of grip and other fine activities. In Bangladesh, the injury was mainly due to broken glass and earning members were affected in a lot of cases. They need proper management with early return to their activities. But the procedure and aftercare was lengthy to achieve a full functional recovery. As there was no conservative treatment available, repair was the method of depending upon the necessity of the individual patient involved.
In our series, a little bit early mobilization programme was used which have many advantages, such as it allow tendon healing by decreased surrounding adhesion formation. Researchers have demonstrated that repaired tendon stressed through a early mobilization programme heal faster, gain tensile strength faster and have less adhesion and better excursion that unstressed repair. Some type of early mobilization programme is currently the accepted postoperative treatment after flexor tendon repair [6].
In this series, about half of the patients were in productive age group and the mean age of the patients was 18 years, which corresponds with other series where mean age was 19 years [7]. Eight patients (56.25%) in the age group 21-30 years corresponds to age group of series by Reinisch et al. and Kunzle et al. [7,8]. Even male and female ratio (2.3:1) was similar to the series of Hunter and Salisbury [9], although it does not correspond with the series of Chaka [10]. Male predominated far more than females in all other series. The result of distribution of involved fingers in our study is similar to YII N. W. et al. [11]. We found associated nerve injuries in 70.6% wrists, which correspond to the study of Reinisch et al. where they found 79 percent [7].
Ten patients (58.8%) out of total 17 patients had broken glass cut injury and 3 (17.6%) lacerated injury by machineries. The most frequent mechanism of injury was a glass cut (31 patients of total 38 wrists). This result was also similar to the series of Reinisch et al. [7]. Tang and Song [12] showed that 60 percent patients had sharp cut injury, 26.7% machine saw injury and 13.3% compression cut injuries. The study of Chacka [10] the result was 81.61 and 15.38 percent, respectively. Sharp cut injury was mainly by knife of hijacker which does not correspond to our series. It may be due to their industrialization and social security.
We found flexor tendon injury more in right dominating hand than left hand (76.5% Vs 23.5%). Similarly Jaffe and Eeckesser [13] found higher incidence in right hand than left hand.
The postoperative results might depend on the timing of starting the operation after injury. Due to ignorance of our patients and lack of expertise in the tendon surgery at the peripheral hospitals in our country and also delayed diagnosis and referral process, the length of time from injury to operation was a bit more, which does not correspond with the results of Kunzle et al. [8], although the length of time from injury to operation seemed to have little effect on the results. The range of postoperative follow-up from 2.5 to 12 months, which was similar to that of Dr. Debashis Biswas [14], but in this series average follow up was 8.18 months versus 8.28 months.
After operation most of the patients (82.4%) had no motor involvement (grip) while before operation all of them had motor involvement (grip). Functional outcome was satisfactory (excellent plus good) in 82.3% of fingers; excellent 4 hands (23.5%) and good 10 hands (58.8%). In a series by N. W. YII et al. [11] the excellent or good results were 90% of fingers which had repair of completely divided flexor tendons in zone-v and independent FDS action was achieved in 66 of the fingers. The unsatisfactory (fair plus poor) result was observed in 17.7% fingers in this series compared to 5.8% in patient with zone-v flexor tendon injuries of Noaman H [15]. Ahamad M et al. [16] showed that 97% satisfactory (excellent plus good) results in a series of 33 patient, 39 fingers. In their series, unsatisfactory (fair only) result was only 3% fingers and there was no poor result.
In most of the published series, there was no infection, but one patient (2.6%) developed infection in a series by Grobbelaar and Hudson [17] out of 38 children. In this series, 1 patient (5.9%) developed ugly scar over the fingers and palm. It impaired the function of gliding of the flexor tendons with a fair result. Neurological deficit was observed in 2 patients (11.8%), one on the radial side of index and one on the ulnar side of the little finger. There were two-point discrimination of >10 mm.
There was adhesion formation in 2 (11.8%) patients, which is a very common problem when injured tendon is repaired end-to-end with repair of sheath [18]. Adhesion sometimes significantly reduces the active digital motion. Interestingly the passive motion remained normal or near normal.
Surgical release of non-gliding adhesions that form along the surface of a tendon after injury or repair was a useful procedure in the salvage of tendon function. Tendon adhesion occur whenever the surface of a tendon is damaged either through the injury itself, be it lacerated or crushed or by surgical manipulation. At any point on the surface of the tendon where violation occurs, an adhesion would likely to form in the healing period [19]. Whenever these adhesions cannot be mobilized by therapy techniques, tenolysis should be considered. This procedure was demanding as tendon repair and itself cannot be undertaken lightly. It represents another onslaught in an area of previous trauma and surgery. Independent FDS action can be impeded by adhesion formation in zone-v repairs, which can be reduced with early motion. To permit early active motion the tendon repair must be strong enough to minimize the risk for gap formation and rupture [20].
In this series, I tried to do the procedure on the patients, those who developed adhesion but none of the patients were willing to do the second operation.
Conclusion
Satisfactory functional results were obtained when the proper surgical technique was coupled with careful postoperative management in patients with zone-v flexor tendon injuries.
References
- Hudson DA, De Jager LT. The spaghetti wrist. Simultaneous lacerations of the median and ulnar nerves with flexor tendons at the wrist. Journal of Hand Surgery. 1993; 18: 171-173.
- Puckett CL, Meyer VH. Results of treatment of extensive volar wrist lacerations: The spaghetti wrist. Plastic and Reconstructive Surgery. 1985; 75: 714-719.
- Rogers GD, Henshall AL, Sach RP, Wallis KA. A simultaneous laceration of median and ulnar nerves with flexor tendons at the wrist. Journal of Hand Surgery. 1990; 15: 990-995.
- Stefanich RJ, Putman MD, Peimer CA, Sherwin FS. Flexor tendon lacerations in zone V. Journal of Hand Surgery. 1992; 17: 284-291.
- Kleinert HE, Verdan C. Report of Committee on Tendon Injuries. Journal of Hand Surgery. 1983; 8: 794-798.
- Culp RW, Taras JS. Primary care of flexor tendon injuries. In Mackin EJ, editor, Rehabilitation of the hand and upper extremity. Vol.1, 5th edition, St. Louis, Mosby-Year Book, Inc. 1998; 415-430.
- Reinisch JF, Winters R, Puckett CL. The use of the osteocutaneous groin flap in gunshot wounds of the hand. The Journal of Hand Surgery. 1984; 9: 12-17.
- Kunzle AL, Brunelli G, Orsi R. Flexor tendon graft in the fingers. Journal of Hand Surgery. 1984; 9: 126-128.
- Hunter JM, Salisbury RE. Flexor tendon reconstruction in severely damaged hands: a two stage procedure using a silicon Dacron reinformed grafting prosthesis prior to tendon grafting. J Bone Joint Surg. 1971; 53: 829-853.
- Chacha P. Free autologus composite tendon grafts. J Bone Joint Surg. 1974; 56: 960-978.
- Yii NW, Urban M, Elliot D. A prospective study of flexor tendon repair in zone v. Journal of Hand Surgery. 1998; 23: 642-648.
- Tang JB, Gu YQ, Song YS. Repair of digital nerve defect with autogenous vein graft during flexor tendon surgery in zone 2. J Hand Surg Br. 1993; 18: 449-453.
- Jaffe S, Eeckesser E. Profundus tendon grafting with the sublimis intact. J Bone Joint Surg. 1976; 49: 1298-1308.
- Debashish D. Evaluation of the results of one stage tendon reconstruction in old flexor tendon injury of hand at zone II [Thesis submitted for MS degree, University of Dhaka]. 2002.
- Noaman HH. Management and functional outcomes of combined injuries of flexor tendons, nerves, and vessels at the wrist. Microsurgery. 2007; 27: 536-543
- Ahmad M, Hussain SS, Tariq F, Rafiq Z, Khan MI, Malik SA. Flexor tendon injuries of hand: experience at Pakistan Institute Medical Sciences, Islamabad, Pakistan. J Ayub Med Coll Abbottabad. 2007; 19: 6-9.
- Grobbelaar AO, Hudson DA. Flexor tendon injuries in children. Journal of Hand Surgery. 1994; 19B: 696-698.
- Wright PE II. Flexor and extensor tendon injuries. In Canale ST, editor, Campbell’s operative orthopedics, Vol. 4, 11thed, New York, Mosby-Year Book, Inc. 1998; 3851-3912.
- Potenza AD. Critical evaluation of flexor tendon healing and adhesion formation within artificial digital sheath. J Bone Joint Surg. 1963; 45: 1217- 1233.
- Bradon J, Wilhelmi MD. Optimizing independent finger flexion with zone v flexor tendon. Journal of Hand Surgery, 2005; 30: 230-236.