Case Report
Austin J Clin Case Rep. 2014;1(5): 1021.
Arachnoid Cyst Manifesting as Panhypopituitarism in the Setting of Septic Shock
Kariuki N1*, Rai AK1 and Shetty V2
1Department of Internal Medicine, Maimonides Medical Center, USA
2Division of Cardiology, Maimonides Medical Center, USA
*Corresponding author: Kariuki N, Department of Internal Medicine, Maimonides Medical Center, 4802 10th Avenue, Brooklyn, New York 11219, USA
Received: May 31, 2014; Accepted: June 25, 2014; Published: June 27, 2014
Abstract
Pituitary cystic sellar masses typically present with symptoms of headache and visual impairment Endocrinologic manifestations are less common. We describe a case of a sixty-two year-old female who presented with altered mental status. She initially appeared to be in septic shock but was also found to have panhypopituitarism secondary to an arachnoid cyst. This case highlights the diagnostic workup of panhypopituitarism in the emergent setting, and demonstrates how this diagnosis maybe masked by other clinical entities.
Keywords: Panhypopituitarism; Sellar masses; Arachnoid cyst; Adrenal stimulation testing; Critical illness related corticosteroid insufficiency
Abbreviations
TSH: Thyroid Stimulating Hormone; FSH: Follicle Stimulating Hormone; IGF-1: Insulinlike Growth Factor; MSSA: Methicillin-sensitive Staphylococcus Aureus; CIRCI: Critical-illnessrelated-corticosteroid Insufficiency
Case Presentation
A 62 year-old female with no known past medical history presented to our emergency room with altered mental status. Her neighbors had not seen her for two days and therefore notified EMS. She was found unresponsive at home, covered in feces and urine. Further history could not be obtained due to her mental state. On physical examination, she was hypothermic (oral temperature 84F), hypotensive (BP 77/59 mmHg), in a stupor and unable to follow commands. She opened her eyes spontaneously but had bilateralvisual impairment with absent pupillary light reflexes (both direct and consensual). Deep tendon reflexes were normal with a normal relaxation phase and Babinski sign was negative. In addition, she had stage three sacral decubiti and lower extremity partial thickness wounds. The rest of the physical examination was unremarkable, including lungs, heart and abdomen.
She was intubated for airway protection. Fluid resuscitation was unsuccessful and she was started on pressors. She received Dextrose 50% IV push for hypoglycemia (finger stick glucose 33 mg/dL). EKG showed sinus bradycardia with Osborne waves (J waves). Preliminary blood work was significant for leukopenia (total white blood cell count 2.6 K/UL with 86% neutrophils) and normocytic anemia (hemoglobin 10.3g/dL). CT Head showed a cystic lesion in the sellar region in the absence of midline and hydrocephalus. Hypopituitarism was suspected at this point and a serum cortisol was drawn. She was subsequently started on IV Levothyroxine 125 mcg q24h and IV Hydrocortisone 100mg q8h.
Results of further workup are listed in Table 1. Her low-normal serum cortisol level despite the presence of critical illness was suggestive of adrenal insufficiency. FSH was inappropriately low for the post-menopausal phase, indicating secondary hypogonadism. Low-normal TSH with low free T3 and T4 was consistent with secondary hypothyroidism. Serum IGF-1 was also low. Collectively, this indicated a central etiology for her hormone deficiencies. There was no evidence of hyperprolactinemia. Overall, these findings were consistent with panhypopituitarism, which correlated clinically with the abnormal visual examination and suprasellar mass. Myxedema coma was among the differential diagnoses, although it was not apparent given the absence of hyponatremia with normal deep tendon reflexes and normal serum creatine phosphokinase levels.
She was also started on broad-spectrum antibiotics for presumed septic shock. Preliminary blood cultures grew Methicillinsensitive Staphylococcus aureus (MSSA) and she was switched to Trimethoprime-Sulfamethoxazole (TMP-SMX) based on culture sensitivity. Chest X-ray was negative for focal consolidation; transthoracic echocardiogram was negative for valvular vegetations. The bacteremia was attributed to a stage three sacral decubitus ulcer and partial thickness skin tears on her feet.
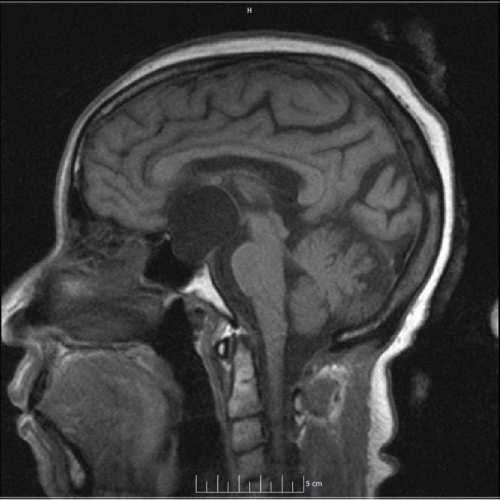
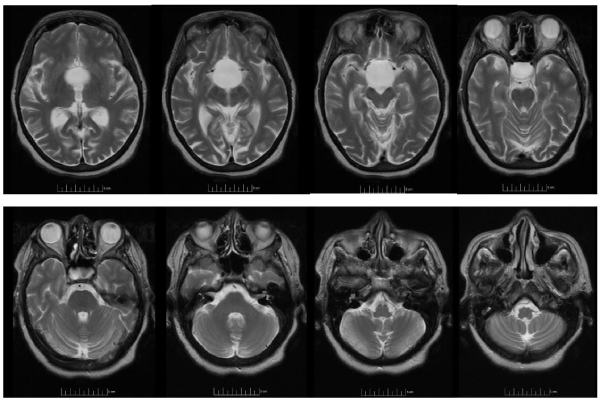
A follow-up brain MRI confirmed symmetric enlargement and expansion of the sella with erosion of the dorsum sellae filled with a 3.3 x 3.1 x 3.4 cm non-enhancing cystic mass of cerebrospinal fluid signal intensity extending into the suprasellar region and displacing the optic chiasm (Figures 1&2). The patient declined surgical intervention.
Figure 1: Brain MRI T1-weighted sagittal section that demonstrates symmetric enlargement and expansion of the sella with a cystic mass (marked with asterisk) of CSF signal intensity extending into the suprasellar cistern.
Figure 2: Brain MRI T2 weighted axial series show the same non-enhancing cystic mass of CSF signal intensity extending into the suprasellar cistern displacing the optic chiasm and blunting the anterior recesses of the third ventricle, displacing the midbrain posteriorly and elevating the floor of the third ventricle
She improved clinically, was successfully extubated and remained hemodynamically stable off pressors. Her mental status returned to baseline. She was discharged on an oral hormone regimen which comprised Hydrocortisone and Levothyroxine. It was anticipated that she would need lifelong hormone replacement. In addition, she was due to complete a total three-week course of TMP-SMX for MSSA bacteremia.
Discussion
Hypopituitarism is a rare manifestation of cystic sellar masses. It has been postulated that they cause sellar enlargement by extension of subarachnoid spaces into the sellar compartment [1]. This mass-like effect results in the impingement of adjacent structures causing anterior pituitary hormone deficiencies and visual defects including loss of visual field, ophthalmoplegia and diplopia. Indeed, our patient’s arachnoid cyst may have been the cause of her visual impairment. Records from her hospitalization three years prior documented gradual vision loss at the time, a negative hormonal workup and an “Empty Sella” with local mass effect seen on head CT scan. An empty sella refers to an enlarged but deformed sella turcica whereby herniation of the subarachnoid space through an incompetent diaphragm sella eventually leads to displacement of the pituitary gland as the cerebrospinal fluid-filled arachnoid tissue continues to expand [2]
The differential for cystic sellar masses includes Rathke cleft cysts, arachnoid and dermoid cysts. Magnetic resonance imaging (MRI) is the best imaging study to characterise these cysts. Arachnoid cysts typically have CSF signal intensity and are non-enhancing with contrast imaging. Conversely, dermoid cysts have a heterogeneous signal intensity as they are derived from multiple germ layers while Rathke cleft cyst have a gadolinium contrast-enhancing capsule [3].
Arachnoid cysts consist of a collection of cerebrospinal fluid surrounded by arachnoid membrane that can occur in all age groups. One retrospective study on their natural history estimated their prevalence at 1.4%. Although the vast majority is asymptomatic and often an incidental finding on brain imaging, arachnoid cysts in certain locations have a higher likelihood of presenting with symptoms. For instance 67% of sellar and suprasellar cysts were symptomatic, most frequently presenting with headache due to obstructive hydrocephalus [4].
Laboratory workup for hypopituitarism entails measurement of basal serum hormone levels, which largely include both the trophic hormone and the target hormone. For example, an otherwise normal serum thyroid-stimulating hormone (TSH) level coupled with a low serum free tetraiodothyronine (free T4) highlights an anomaly in negative feedback that is indicative of central hypothyroidism. Of note, basal ACTH secretion may be assessed by measuring morning serum cortisol around 8 to 9 am. Serum cortisol ≥18 mcg/dL is consistent with adequate ACTH secretion. Cortisol deficiency is demonstrated by serum cortisol ≤3 mcg/dL on at least two occasions; when coupled with a normal or low ACTH level this implies secondary adrenal insufficiency. When the serum cortisol level is greater than 3mcg/dL but less than 18mcg/dL, ACTH reserve can then be checked using the Metyrapone or Cosyntropin tests. Our patient was critically ill on presentation with suspicion for septic shock. Random evening serum cortisol level was 6mcg/dL though ACTH stimulation testing was not pursued. It is a recognized concept that stressors such as trauma or critical illness can disrupt the hypothalamic-adrenal-pituitary axis, leading to a condition referred to as critical-illness-relatedcorticosteroid insufficiency (CIRCI). Similarly, the Cosyntropin testing can be skewed by CIRCI and adrenal stimulation testing is generally not recommended. Instead, corticosteroid therapy should be initiated particularly for unstable patients, typically with divided stress doses of up to 200mg per day of Hydrocortisone [5-7].
Conclusion
Hypopituitarism should be considered among the differential diagnoses for acutely altered mental status, albeit less common than underlying infection, which may present concurrently. When it presents in hemodynamically unstable patients, a presumptive diagnosis may be made on clinical grounds backed with laboratory and imaging findings. Provided it is feasible, it is recommended to draw serum basal hormone levels prior to the initiation of hormone replacement. In particular, Levothyroxine increases cortisol clearance and can potentially induce an adrenal crisis if not concurrently administered with corticosteroids in the event of cortisol deficiency.Emphasis is therefore placed on evaluating the pituitary-adrenal axis prior to thyroid hormone replacement. Nevertheless, in emergent scenarios where CIRCI may apply, it is reasonable to forego dynamic hormone stimulation tests and opt instead for basal serum hormone measurement.
References
- Dubuisson AS, Stevenaert A, Martin DH, Flandroy PP. Intrasellar arachnoid cysts. Neurosurgery. 2007; 61: 505-513.
- Ghatnatti V, Sarma D, Saikia U. Empty sella syndrome - beyond being an incidental finding. Indian J Endocrinol Metab. 2012; 16: S321-323.
- Yin Y, Tong D, Yuan TT, Zhao XE. Role of magnetic resonance imaging in the diagnosis of lesions in the sellar region. Zhongguo Yi Xue Ke Xue Yuan Xue Bao. 2012; 34: 492-496.
- Al-Holou WN, Terman S, Kilburg C, Garton HJ, Muraszko KM, Maher CO, et al. Prevalence and natural history of arachnoid cysts in adults. J Neurosurg. 2013; 118: 222-231.
- Van Aken MO, Lamberts SW. Diagnosis and treatment of hypopituitarism: an update. Pituitary. 2005; 8: 183-191.
- Streeten DH, Anderson GH Jr, Bonaventura MM. The potential for serious consequences from misinterpreting normal responses to the rapid adrenocorticotropin test. J Clin Endocrinol Metab. 1996; 81: 285-290.
- Hamilton DD, Cotton BA. Cosyntropin as a diagnostic agent in the screening of patients for adrenocortical insufficiency. Clin Pharmacol. 2010; 2: 77-82.