
Case Report
Austin J Clin Neurol 2017; 4(2): 1104.
A Case of Presenting Cerebral Hemorrhage as Cerebral Venous and Sinus Thrombosis
Sun M¹, Hou XX¹, Ren G², Chong ZZ³, Zhang YY4,5 and Cheng H¹*
¹Department of Neurology, First Affiliated Hospital of Nanjing Medical University, China
²Department of Radiology, First Affiliated Hospital of Nanjing Medical University, China
³Department of Anesthesiology, University of Illinois at Chicago, USA
4Department of Cardiovascular Surgery, East Hospital, Tongji University School of Medicine, China
5Key Laboratory of Arrhythmias of the Ministry of Education of China, East Hospital, Tongji University School of Medicine, China
*Corresponding author: Cheng Hong, Department of Neurology, First Affiliated Hospital of Nanjing Medical University, No. 300 Guangzhou Road, Nanjing 210029, Jiangsu Province, China
Received: March 16, 2017; Accepted: April 28, 2017; Published: May 11, 2017
Abstract
A 38-year-old man who had a history of paroxysmal nocturnal hemoglobinuria (PNH) was admitted with headache and vomiting. Based on the initial cranial computed tomography (CT), he was diagnosed of normal intracranial hemorrhage (ICH) at first. His condition got worse although treatment involving dehydration was started immediately. On the fifth day, cranial magnetic resonance venography (MRV) demonstrated cerebral venous and sinus thrombosis (CVST) with concomitant ICH, the therapy including anticoagulation and thrombosis had started. The patient completely recovered clinically. Concluded from our case, atypical cerebral hemorrhage should be treated carefully. MR and digital subtraction angiography (DSA) are the preferred images to evaluate the underlying vascular and other intracranial disease when the suspicion is found clinically or by radiological imaging.
Keywords: Cerebral venous and sinus thrombosis; Paroxysmal nocturnal hemoglobinuria; Intracranial hemorrhage
Abbreviations
PNH: Paroxysmal Nocturnal Hemoglobinuria; CT: Computed Tomography; ICH: Intracranial Hemorrhage; MRI: Magnetic Resonance imaging; MRV: Magnetic Resonance Venography; CVST: Cerebral Venous and Sinus Thrombosis; INR: International Normalized Ratio; DSA: Digital Subtraction Angiography; LMWH: Low Molecular Weight Heparin
Case Presentation
A 38-year-old man with paroxysmal nocturnal hemoglobinuria (PNH) was admitted to the hematology department because of a 2-week history of left side headache and vomiting. Based on the initial results of cranial computed tomography (CT) and magnetic resonance imaging (MRI), he was diagnosed as having Intracranial hemorrhage (ICH) in the left temporal lobe and the cerebellar hemisphere (Figure 1). His blood pressure was 130/70 mmHg, vital signs were in reference range with no abnormal finding on physical examination. Initial laboratory values revealed a hemoglobin level of 84g/L, an international normalized ratio (INR) of 0.91 and a D-Dimer of 0.22 (reference range, 0-0.500). At admission, to alleviate cerebral edema and relieve the symptom of headache, treatment comprising dehydration and an analgesic was started immediately, but the headache and vomiting persisted. On the fourth day of hospitalization, the patient’s condition got worse, although several dehydration agents were used more aggressively. To prevent increased bleeding after intracranial hemorrhage, the frozen plasma was used as well. However, he developed somnolence with enlarged focal edema and increased intracerebral bleeding accompanied by elevated intracranial pressure (Figure 2).
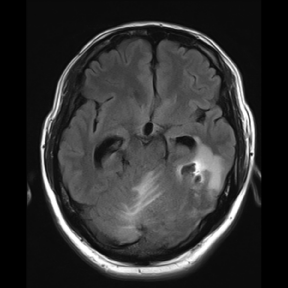
Figure 1: Cranial magnetic resonance imaging (MRI) showed initial
hemorrhage and edema in the left temporal lobe and the left cerebellar
hemisphere.
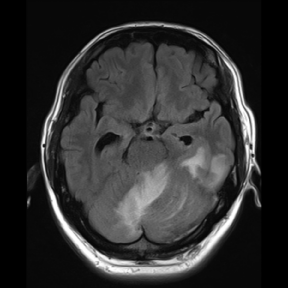
Figure 2: MRI of fluid attenuated inversion (FLAIR) showed enlarged
hemorrhage and edema in original site on the fourth day of hospitalization.
The patient was transferred to neurological department immediately. On the fifth day of hospitalization, another magnetic resonance venography (MRV) demonstrated that thrombosis caused substantial blood flow impairment in the left transverse and sigmoid sinus (Figure 3). The patient subsequently developed a coma due to progressively develop local edema and ICH, though intravenous heparin therapy of 4100U twice a day begun immediately after MRV imaging. On the seventh day, the patient underwent simultaneous digital subtraction angiography (DSA) and intrasinus thrombolysis. Three days later, he regained consciousness. On the day 15, the patient completely recovered clinically without sign of ICH on cranial CT images. One month later, MRV showed partly recanalization of the occluded dural sinuses and cerebral veins (Figure 4). On the 24-month follow-up in a neurology clinic, the patient lives his regular life with warfarin to maintain his INR within the therapeutic range.
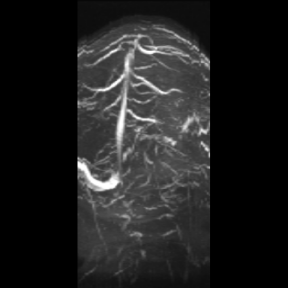
Figure 3: Cranial magnetic resonance venography (MRV) demonstrated the
blocking in the left transverse and sigmoid sinus.
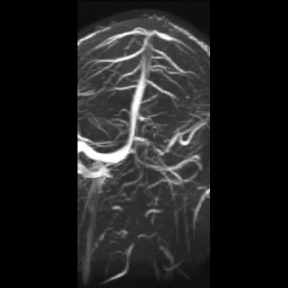
Figure 4: MRV showed partly recanalization of the occluded dural sinuses
and cerebral veins.
Discussion
Cerebral venous and sinus thrombosis (CVST) is a rare cerebrovascular disease, the prevalence of which is about 1.3 cases per 100, 000 and can present with a variety of clinical symptoms ranging from isolated headache to coma [1, 2]. Due to the non-typical symptoms, the diagnosis of CVST can be easily ignored. However, it is reported that the head CT scan can be used as the preferred imaging method of CVST, which has high sensitivity and specificity [3,4]. The more specific test for the diagnosis of CVST is MRV, CT venography or DSA [5]. Currently, anticoagulation is a first-line treatment to prevent the thrombus extension [6]. The 2010 European Federation of Neurological Society (EFNS) recommends thrombolysis to be a therapeutic option used in patients who deteriorate despite adequate treatment [7].
As an uncommon form in stroke, CVST is more common in those with PNH, although the cause remain to be elucidated [8]. PNH is an acquired blood disease that characterized by destruction of red blood cells. Forty percent of patients with PNH develop thrombosis, which is the main cause of severe complications and deaths in PNH. The thrombosis may develop in common sites involving deep vein of leg, lung and skin. Furthermore, some possible mechanisms including the release of free hemoglobin, the impairment of fibrinolysis or anticoagulation may promote thromboses in PNH [9].
The underlying pathophysiology of ICH in CVST is unknown. Hemorrhage may be precipitated by continued arterial perfusion in arterial ischemia. Elevation of venous pressure is also likely a cause [7]. To differentiate between ICH of the arterial origin and ICH of non-arterial origin by using basic CT and MRI is difficult. However, the imaging pattern of ICH may suggest the hemorrhagic source. Irregularly, hemorrhage with flame shape in parasagittal frontal and parietal lobes may be caused by superior sagittal sinus thrombosis. Hemorrhage in the temporal and occipital lobes may result from transverse sinus occlusion, as in the present patient. In contrast to arterial ischemia, many parenchymal abnormalities including ICH secondary to CVST are reversible [10].
The optimal treatment of CVST is still unclear. The combination of local thrombolysis and the use of low molecular weight heparin (LMWH) may offer an effective option in patients with severe CVST. However, further detailed information, which needs the cooperation of international multi centers, must be accumulated on the efficacy and safety of thrombolysis in CVST.
Acknowledgement
We thank the patient for providing permission to share his information. The study was partly supported by the Six Talent Peaks Project in Jiangsu (WSN-025) and Natural Science foundation of Jiangsu Province (BK20161063).
References
- Coutinho JM, Zuurbier SM, Aramideh M, Stam J. The incidence of cerebral venous thrombosis: a cross-sectional study. Stroke. 2012; 43: 3375-3377.
- Moll S, Waldron B. Cerebral and sinus vein thrombosis. Circulation. 2014;130: e68-e70.
- Garetier M, Rousset J, Pearson E, Tissot V, Gentric JC, Nowak E, et al. Value of spontaneous hyperdensity of cerebral venous thrombosis on helical CT. Acta Radiol. 2014; 55: 1245-1252.
- Filippidis A, Kapsalaki E, Patramani G, Fountas KN. Cerebral venous sinus thrombosis: review of the demographics, pathophysiology, current diagnosis, and treatment. Neurosurg Focus. 2009; 27: E3.
- Smith R, Hourihan MD. Investigating suspected cerebral venous thrombosis. BMJ. 2007; 334: 794-795.
- Sacco RL, Adams R, Albers G, Alberts MJ, Benavente O, Furie K, et al. Guidelines for prevention of stroke in patients with ischemic stroke or transient ischemic attack: a statement for healthcare professionals from the American Heart Association/American Stroke Association Council on Stroke: co-sponsored by the Council on Cardiovascular Radiology and Intervention: the American Academy of Neurology affirms the value of this guideline. Circulation. 2006; 113: e409-e449.
- Einhäupl K, Stam J, Bousser MG, De Bruijn SF, Ferro JM, Martinelli I, et al. EFNS guideline on the treatment of cerebral venous and sinus thrombosis in adult patients. Eur J Neurol. 2010; 17: 1229-1235.
- Parker C, Omine M, Richards S, Nishimura J, Bessler M, Ware R, et al. Diagnosis and management of paroxysmal nocturnal hemoglobinuria. Blood. 2005; 106: 3699-3709.
- Van Bijnen ST, Van Heerde WL, Muus P. Mechanisms and clinical implications of thrombosis in paroxysmal nocturnal hemoglobinuria. J Thromb Haemost. 2012; 10: 1-10.
- Leach JL, Fortuna RB, Jones BV, Gaskill-Shipley MF. Imaging of cerebral venous thrombosis: current techniques, spectrum of findings, and diagnostic pitfalls. Radiographics. 2006; 26: s19-s43.