
Case Report
Austin J Clin Neurol 2017; 4(4): 1115.
Excess Interleukin-6 Production and Multiple Ischemic Strokes – What is the Link?
Boehme C, Zangerle A, Mayer L, Toell T, Knoflach M, Willeit J and Kiechl S*
Department of Neurology, Medical University Innsbruck, Austria
*Corresponding author: Kiechl S, Department of Neurology, Medical University Innsbruck, Anichstrasse 35, Innsbruck, A-6020 Austria
Received: June 01, 2017; Accepted: June 26, 2017; Published: July 11, 2017
Abstract
Clinicians often have to deal with rare causes of stroke. We report the case of a 42-year old woman with a 3-year history of unclassified rheumatic disease and elevated level of interleukin-6 (IL-6), who suffered multiple ischemic strokes with an embolic pattern (MRI). Echocardiography revealed a mass in the left atrium suspicious for cardiac myxoma. The patient underwent surgery and recovered quickly. Histopathological examination confirmed the diagnosis of cardiac myxoma and full clinical remission was achieved after a period of four months.
Cardiac myxoma is the most common cardiac tumor and well known for ectopic IL-6-production resulting in rheumatic complaints. Clinicians should be aware that elevated IL-6 levels in the context with history of rheumatic diseases points to cardiac myxoma and should perform echocardiography before complications like stroke emerge.
Keywords: Stroke; IL-6; Cardiac myxoma; Embolic stroke; Interleukin 6
Abbreviations
ANA: Antinuclear Antibodies; ANCA: Anti-Neutrophil Cytoplasmatic Antibodies; IL-6: Interleukin 6
Case Presentation
A 42-year-old woman was admitted to our department because of vertigo, numbness of the left face and cold paraesthesia of the right leg. Neurological examination additionally revealed hemiataxia of the left extremities and Horner’s Syndrome leading to the clinical diagnosis of left-sided Wallenberg’s Syndrome. Cerebral MRI demonstrated micro-embolic infarcts in multiple vessel territories along with the clinically leading stroke in the left dorso-lateral medulla oblongata (Figure 1). She had fever up to 38°C without clinical evidence of infection and showed prominent livedo racemosa involving the lower arms and legs (Figure 2). Electrocardiogram and chest X-ray were unremarkable.
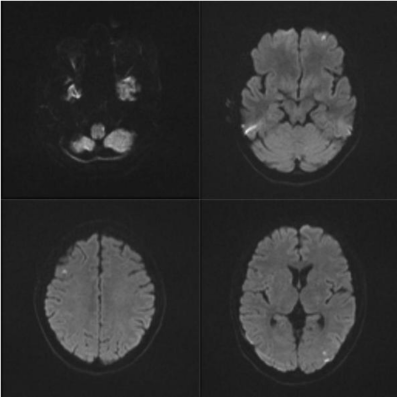
Figure 1: Multiple ischemic lesions in MRI Diffusion-weighted Imaging (DWI)
(left dorso-lateral medulla oblongata; left and right middle cerebral and left
posterior cerebral artery territories).
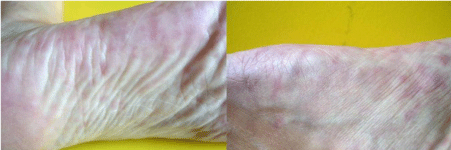
Figure 2: Livedo racemosa on both feet.
The patient had a 3-year period of unexplained recurrent fever, general fatigue, arthralgia and myalgia, dry eyes (sicca-syndrome), morning stiffness and swelling of metacarpophalangeal joints. Because of continuous deterioration of the complaints she sought medical advice by a rheumatologist. At that time, laboratory examination demonstrated elevated serum levels of interleukin-6 (IL-6; 11 pg/ml [normal < 3.0 pg/ml]) and presence of antinuclear antibodies (ANA titre 1:640 [normal < 1:80]) and anti-neutrophil cytoplasmic antibodies (ANCA) with a perinuclear and cytoplasmatic staining pattern. White blood cell count, erythrocyte sedimentation rate, anti-cyclic citrullinated peptide antibodies, rheumatoid factor and anti-cardiolipin antibodies were all within normal limits or absent. The patient was given the diagnosis of unclassified rheumatic disease. Therapy with non-steroidal anti-inflammatory drugs was commenced and escalated; however, no sustained amelioration of symptoms occurred. About 15 months later she started suffering from severe Raynaud’s syndrome. The diagnosis of rheumatic disease was reinforced and a therapy using hydroxychloroquine was initiated with the advice to switch to steroid therapy in case of insufficient symptom control.
15 months later the patient was admitted to our department because of multiple embolic strokes and also complained about both-sided flank pain. CT revealed multiple small splenic and renal infarcts (Figure 3). High-resolution ultrasonography of the lower extremity venous system was performed to rule out thrombosis causing embolism. The result of this exam was unremarkable as were D-Dimer concentrations in blood. Laboratory investigations revealed excessive IL-6 levels (100 pg/ml, Figure 4) and various other abnormalities suggestive of rheumatic or autoimmune disease (white blood cell count 12.1 G/l [normal < 10 G/L], C-reactive protein 5.4 mg/dl [normal < 0.7 mg/dl], erythrocyte sedimentation rate 36 mm/h [normal 6-18 mm/h], ANA 1:640 [normal <1:80] and positive ANCA). Repeated blood cultures for bacterial or fungal pathogens were negative, as well as the anti-phospholipid antibody testing.
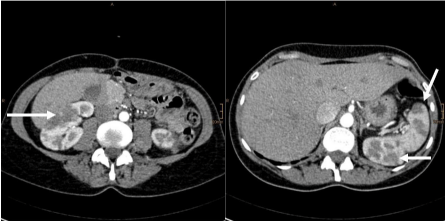
Figure 3: Renal and splenal infarcts on abdominal CT-scans (left: right-sided
renal infarction; right: left-sided renal and splenal infarction).
Once considering all these findings along with the patient’s medical history, the favourite differential diagnoses to assume were systemic vasculitis, thrombotic endocarditis, collagenosis, or cardiac myxoma with constitutional symptoms due to IL-6 excess production. Transesophageal echocardiography showed a left atrial mass - 44x26 mm in size - highly suggestive of cardiac myxoma. The patient underwent cardiac surgery. The tumor had a villous surface and grey stroma. Histological work-up confirmed its myxomatous nature. The postoperative course was uneventful and the patient’s constitutional symptoms shortly disappeared. Pathological laboratory findings including IL-6 levels normalised (Figure 4) and ANCAs disappeared in the consecutive examinations. The patient was discharged 13 days after cardiac surgery and was admitted to a rehabilitation facility to treat gait ataxia. Echocardiography follow-up after 9 months did not show recurrence of the tumor. The patient experienced full clinical remission and remained asymptomatic until her last visit one year after surgery.

Figure 4: Interleukin-6 level over time (T=Time point at cerebrovascular
event).
Discussion
Myxoma is the most common type of primary cardiac tumor and 75% of myxomas occur in the left atrium [1,2]. Patients present with one or more of the typical triad of intra-cardiac obstruction, systemic embolization and constitutional symptoms [3]. Systemic embolization results from tumor fragmentation or thrombotic material from the myxoma surface [4,5]. Constitutional symptoms imitating rheumatic or autoimmune diseases and related laboratory abnormalities originate from ectopic IL-6 expression and its release from myxoma cells and infiltrating mononuclear cells [3-6]. IL-6 is a pleiotropic cytokine capable of initiating a prominent and sustaining inflammatory response inducing fever and polyclonal B-cell differentiation with subsequent up-regulation and release of multiple auto-antibodies at low titres. There is a positive correlation between tumor size and IL-6 levels in patients suffering from first-ever myxoma and also a positive correlation between IL-6 concentration and severity of constitutional symptoms [7].
Therefore we recommend routine IL-6 testing in young stroke patients with a micro-embolic stroke pattern and all those suffering from constitutional symptoms. Diagnostic work-up in stroke patients with an assumed cardioembolic cause should always include transesophageal echocardiography and this especially true if IL-6 levels are increased.
Our patient suffered three years from rheumatic symptoms before cerebrovascular event occurred and the correct diagnosis was established. Our case report intends to increase awareness of clinicians that rheumatic symptoms and increased IL-6 levels may originate from cardiac myxoma. A delay in diagnosis may result in a life-threatening complication like stroke, systemic embolisms or mitral valve obstruction.
References
- Reynen K. Cardiac myxomas. N Engl J Med. 1995; 333: 1610-1617.
- He DK, Zhang YF, Liang Y, Ye SX, Wang C, Kang B, et al. Risk factors for embolism in cardiac myxoma: a retrospective analysis. Med Sci Monit. 2015; 21: 1146-1154.
- Acebo E, Val-Bernal JF, Gómez-Román JJ, Revuelta JM. Clinicopathologic study and DNA analysis of 37 cardiac myxomas: a 28-year experience. Chest. 2003; 123: 1379-1385.
- Elbardissi AW, Dearani JA, Daly RC, Mullany CJ, Orszulak TA, Puga FJ, et al. Embolic potential of cardiac tumors and outcome after resection: a casecontrol study. Stroke. 2009; 40: 156-162.
- Knepper LE, Biller J, Adams HP Jr, Bruno A. Neurologic manifestations of atrial myxoma. A 12-year experience and review. Stroke. 1988; 19: 1435- 1440.
- Shiraishi I, Yamagishi M, Kato R, Okumura Y, Sato H, Tanaka T, et al. A case in a child of giant left-atrial myxoma associated with recurrent high fever and myxoma cells expressing interleukin-6. Eur J Pediatr. 2006; 165: 346-347.
- Mendoza CE, Rosado MF, Bernal L. The role of interleukin-6 in cases of cardiac myxoma. Clinical features, immunologic abnormalities, and a possible role in recurrence. Tex Heart Inst J. 2001; 28: 3-7.