
Case Report
Austin J Clin Neurol 2017; 4(4): 1117.
Audiovestibular Loss in the Infarction of the Left Potine Brachium: How to Early Detect?
Yan YP¹ and Zhang B²*
¹Department of Neurology, Zhejiang University, China
²Department of Surgery, Zhejiang University, China
*Corresponding author: Bo Zhang, Department of Surgery, Second Affiliated Hospital, School of Medicine, Zhejiang University, No.88 Jiefang Road, Hangzhou, Zhejiang 310009, China
Received: June 12, 2017; Accepted: June 30, 2017; Published: July 18, 2017
Abstract
The anterior inferior cerebellar artery (AICA) usually supplies the inner ear, middle cerebellar peduncle, lateral pons, and anterior inferior cerebellum. When infarction occurs, hearing loss, as well as dizziness and dystaxia might appear. Here, we present a case of such syndrome, which was misdiagnosed for the first two weeks after feeling dizziness and deafness of his left ear.
Keywords: Anterior inferior cerebellar artery (AICA); Deafness; Infarction; Dizziness; Syndrome
Case Presentation
A 59-year-old male worker complained of persistent dizziness and deafness of his left ear for two weeks. At first, he went to the otorhinolaryngological department of another hospital and received a neurotrophic and improved circulatory therapy. However, his symptom didn’t improve after two weeks’ therapy. Magnetic resonance image (MRI) demonstrated left potine brachium lesion. So he went to our hospital for further treatment. Physical examination revealed apart from the deafness of his left ear, hypaesthesia of his left face and some problem in coordination. The patient could not complete both heel-knee-tibia test and finger-nose test, as well as poor performance when walking in a line. Diabetes was discovered one year ago. Although taking metformin twice every day, his blood glucose still had not been controlled well for the past year. He had a history of smoking and drinking. Diffusion weighted imaging demonstrated newly occurring infarction of the left potine brachium. While the signal in apparent diffusion coefficient (ADC) was low. Enhanced MRI showed a light ring-shaped enhancement around the lesion with a T1-low and T2- high signal. Magnetic resonance spectroscopy (MRS) also supported the report of infarction. Luckily, Magnetic Resonance Angiography (MRA) was normal as both anterior inferior cerebellar arteries (AICA) were not displayed (Figure 1).
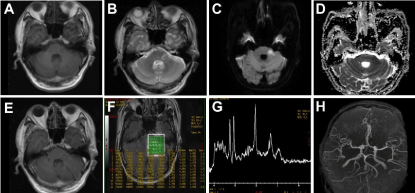
Figure 1: (A) T1 showing a low signal in the left potine brachium. (B) T2 showing a high signal in the same region. (C) Diffusion weighted imaging (DWI) and
apparent diffusion coefficient (ADC) (D) showing newly occurring infarction. (E) Enhanced MRI demonstrating a light ring-shaped enhancement around the lesion.
(F, G) MRS showing light declining of NAA value and light elevating of cho value, while the ratio of NAA/cho is in normal range. (H) MRA demonstrating normal,
while both AICA not displaying.
Three months later, dizziness and dystaxia was significantly relieved while deafness and numbness of his left face was still not improved.
Discussion
Sudden deafness in patients with cerebrovascular risk factors, especially in the presence of other brainstem signs, like facial hypaesthesia and dystaxia, suggests the possibility of labyrinthine artery ischemia. AICA usually arises from the basilar artery and supplies the inner ear, middle cerebellar peduncle, lateral pons, and anterior inferior cerebellum [1]. The labyrinthine artery usually derives from the AICA [2]. The potine brachium territory, where the seventh and eighth cranial nerves, some nerve nuclei like the spinal trigeminal nucleus, was supplied by the ipsilateral AICA [3,4]. Bilateral AICA infarction might also appear. The reason is that the two AICAs derive from 1 trunk [5-9]. Since Adams first reported the AICA occlusion syndrome [10], more and more cases are discovered. Sometimes, sudden deafness had also been reported as prodrome of AICA infarction [4]. Lee H reported that 81% patients who were followed for at least 1 year after onset with AICA infarction show partial or complete recovery of hearing loss [8]. In our case, deafness was still not improved after 3 months.
In summary, this case highlights the characteristics of the AICA syndrome, like hearing loss, vertigo, facial weakness and sensory loss and ataxia. Therefore, clinicians should recognize that unilateral hearing loss may be related to stroke in the AICA area. We sought to show a case with AICA territory infarction and to call for more attention on it.
Acknowledgement
The authors acknowledge the patients and their families for their important help in data acquisition and the Cancer Institute of Zhejiang University for Technical Assistance and advice. This work was supported by grants from the National Natural Science Foundation of China (No. 81570698) and (No.81200984), the Natural Science Foundation of Zhejiang Province (LY16H070003).
References
- Ogawa K, Suzuki Y, Takahashi K, Akimoto T, Kamei S, Soma M. Clinical Study of Seven Patients with Infarction in Territories of the Anterior Inferior Cerebellar Artery. J Stroke Cerebrovasc Dis. 2017; 26: 574-581.
- Renard D, Taieb G, Castelnovo G, Ghanem S, Ayrignac X, Labauge P. Isolated bilateral anterior inferior cerebellar artery infarction. Arch Neurol. 2010; 67: 766-767.
- Markowski J, Gierek T, Kluczewska E, Witkowska M. Assessment of vestibulocochlear organ function in patients meeting radiologic criteria of vascular compression syndrome of vestibulocochlear nerve--diagnosis of disabling positional vertigo. Med Sci Monit. 2011;17: CR169-CR173.
- Lee H. Audiovestibular loss in anterior inferior cerebellar artery territory infarction: a window to early detection? J Neurol Sci. 2012; 313: 153-159.
- Wu XQ, Zhang BR. Bilateral middle cerebellar peduncle infarcts caused by bilateral vertebral artery occlusion: a case report. Zhejiang Da Xue Xue Bao Yi Xue Ban. 2014; 43: 583-587.
- John S, Hegazy M, Cheng Ching E, Katzan I. Isolated bilateral middle cerebellar peduncle infarcts. J Stroke Cerebrovasc Dis. 2013; 22: e645-e646.
- Kataoka H, Izumi T, Kinoshita S, Kawahara M, Sugie K, Ueno S. Infarction limited to both middle cerebellar peduncles. J Neuroimaging. 2011; 21: e171-e172.
- Lee H, Baloh RW. Sudden deafness in vertebrobasilar ischemia: clinical features, vascular topographical patterns and long-term outcome. J Neurol Sci. 2005; 228: 99-104.
- Chang HM, Linn FH, Caplan LR. Bilateral anterior inferior cerebellar artery territory infarcts. J Neuroimaging. 1998; 8: 42-44.
- Adams RD. Occlusion of the anterior inferior cerebellar artery. Arch Neurol Psychiatry. 1943; 49: 765-770.