Research Articlee
Austin J Clin Ophthalmol. 2014;1(5): 1026.
Amniotic Membrane-Assisted Trabeculectomy for Refractory Glaucoma with Corneal Disorders
Kazuhiko Mori*, Yoko Ikeda, Shigeta Naruse, Morio Ueno and Shigeru Kinoshita
Department of Ophthalmology, Kyoto Prefectural University of Medicine, Japan
*Corresponding author: Kazuhiko Mori, Department of Ophthalmology, Kyoto Prefectural University of Medicine, 465 Kajii-cho, Hirokoji-agaru, Kawaramachidori, Kamigyo-ku, Kyoto 602-0841
Received: May 20, 2014; Accepted: June 30, 2014; Published: July 01, 2014
Abstract
Purpose: To report 6 consecutive cases which underwent amniotic membrane (AM)-assisted trabeculectomy (TLE) to treat refractory glaucoma with severe corneal disorders.
Materials and Methods: This study involved 6 patients (3 males/3 females, mean age: 69.5±15.8 years) with refractory glaucoma and severe corneal disorders. The surgical procedure for each patient involved trabecular tissue being excised, and human AM then being placed epithelial-side-up on the corneal surface, sutured at the limbal sclera, and flipped over onto the sclera to cover the TLE area. The remaining edge of the AM was then inserted into the sub conjunctival space and sutured. Medical records of all cases were reviewed in regard to intraocular pressure (IOP), visual acuity (VA), and condition of the filtering bleb and ocular surface.
Results: The mean observation period was 69.5±15.8 months, and mean IOP at pre surgery and at 1, 3, and 7 years postoperative was 40.3±6.9, 23.0±12.1, 25.6±12.8, and 28.5±19.1 mmHg, respectively. Glaucoma medications decreased from 3.0±1.1 drugs (pre-surgery) to 0.8±1.0 (7 years postoperative). However, in some cases, ocular surface conditions or VA worsened during the follow-up period.
Conclusion: Using AM as an internal patch for TLE, moderately good, long-term IOP control was maintained, however, ocular surface conditions required special care.
Keywords: Amniotic membrane; Refractory glaucoma; Trabeculectomy
Introduction
Glaucoma with corneal disorders including ocular surface diseases is one of the most refractory types of glaucoma. Filtering surgery often fails due to severe inflammation, recurrent conjunctival scarring, proliferation of subconjunctival fibrous tissue, and the high risk of infection in patients taking immune-suppressive drugs. Other surgical procedures such as tube-shunt surgery are not always effective for severe ocular surface disorders, because they may result in many problems such as cicatricial reaction of the conjunctivae, exposure of the tube or plate, and corneal endothelial damage.
Recently, the use of human amniotic membrane (AM) in ocular surface reconstruction has reportedly yielded good outcomes [1-7]. In 1910, Davis [8] first described the use of AM in skin transplantation procedures. In the field of ophthalmology, AM was reportedly employed in the 1940’s to repair conjunctival defects after chemical burns, [9,10] however, the results were not promising. Successful AM transplantation for ocular surface reconstruction was reported 50 years later [1,4], and AM is now the focus of attention as a biomaterial for the treatment of severe ocular surface diseases such as ocular pemphygoid, Stevens-Johnson syndrome, and chemical burns. Koizumi et al. [6] and Nakamura et al. [7] reported very good prognoses when using AM as a transporter of cultured corneal epithelium to treat patients with severe ocular surface diseases. In ocular surface reconstruction, AM offers several benefits, as it can be easily obtained and preserved for several months, is not rejected immunologically, suppresses fibroblast proliferation, and accelerates cell migration and growth. Therefore, we theorized that AM might be suitable for glaucoma filtering surgery.
To date, there have been few reports on the use of AM in glaucoma surgery [11-14]. Fujishima et al.[11] reported the effectiveness of AM for reducing intraocular pressure (IOP) in high-risk patients when it was placed under the scleral flap, yet Budenz et al. [12] found that AM transplantation was not an effective alternative to conjunctival advancement in patients undergoing the repair of leaking glaucoma filtering blebs; however, it should be noted that their total replacement of the leaking bleb with AM exposed it to constant pressure without supportive structures above or beneath the filtering bleb. In the presence of such structures, AM might be able to resist that pressure and function as part of the bleb wall. Based on these considerations we theorized that an AM patch could be introduced below the filtering bleb. The purpose of this present study was to report 6 patients with refractory glaucoma with corneal severe disorders who were treated with AM-assisted trabeculectomy (TLE).
Patients and Methods
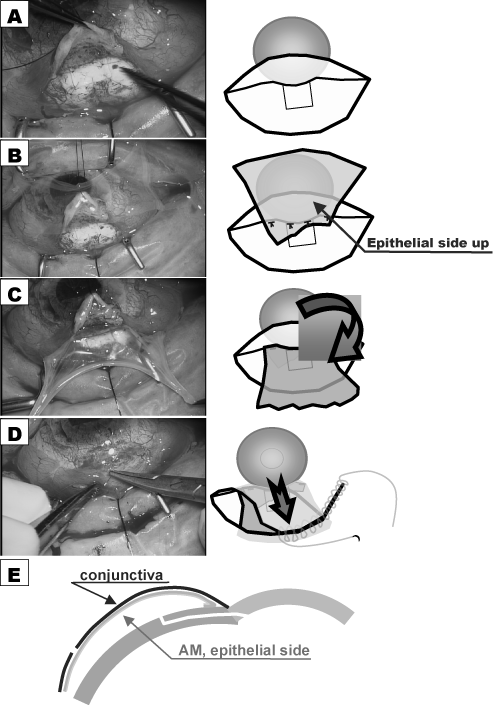
This study involved 6 consecutive patients (3 males and 3 females, mean age: 69.5±15.8 years) with refractory glaucoma and corneal disorders who were treated with AM-assisted trabeculectomy (TLE) between March 2000 and April 2002. Written informed consent was obtained from all patients for the use of AM, and the procedure was approved by the Human Studies Committee of Kyoto Prefectural University of Medicine. IOP measurements of each patient were obtained by use of a Goldman applanation tonometer, and the surgical procedure for each patient was as follows. First, under local anesthesia an adequate amount of sclera was exposed by careful detachment of the scarred conjunctiva and conventional TLE was then performed. A limbal-based conjunctival flap was then produced and inoculated with a 0.4 mg/ml treatment of mitomycin C (MMC) for 3 minutes (Figure 1A). Next, deep-frozen human AM obtained at the time of Caesarean section was thawed, trimmed to the proper size, placed epithelial-side-up on the corneal surface, and sutured at the limbal sclera beside the scleral flap using 10-0 nylon sutures (Figure 1B). The other edge of the AM was then flipped over (epithelial-side-down) to cover the scleral flap (Figure 1C). Finally, continuous conjunctival suturing with 10-0 polypropylene was performed (Figure 1D). A cross-sectional view of the filtering bleb with the AM patch is shown in (Figure 1E).
Figure 1 :
Figure 2 :
The medical records of all 6 cases were reviewed in regard to each patient’s IOP, visual acuity (VA), and the condition of the filtering bleb and ocular surface.
Results
The summary of all 6 cases is shown in Table 1, and the mean observation period was 69.5±15.8 months. All cases had severe corneal disorders with secondary glaucoma including pseudoexfoliation glaucoma, and 5 of the 6 cases had undergone penetrating keratoplasty. The details of 3 representative cases are here described as follows. The first patient was a 49-year-old man with severe chemical burn who had undergone ocular surface reconstruction. Three months later, his IOP rose to 30 mmHg and despite intensive medical therapy over a period of 6 months it was judged that his eye required surgical treatment. Because of his severely scarred, adhesive sub conjunctival tissue, we performed our newly developed surgical technique that consists of TLE with AM inserted under the AM that had been transplanted in the earlier procedure. Eight years after the AM-assisted TLE his IOP was maintained at 20 mmHg without any glaucoma medications. The second patient was a 58-year-old man with perforating corneal injury and traumatic cataract who had undergone intra capsular cataract extraction (ICCE) 40 years earlier. His eye progressed to secondary glaucoma and he underwent several filtering surgeries to control IOP. Ten years before his current treatment, he had undergone penetrating keratoplasty (PKP) to treat bullous keratopathy due to corneal de compensation. However, his IOP became uncontrollable and we performed AM-assisted TLE because of the conjunctival scarring caused by the previous surgical procedures. His mean IOP was maintained at around 15.8 mmHg, however, due to the past severe damage, his visual acuity (VA) became no light perception after several years. The third patient was a 57-year-old woman with a perforating corneal fungal infection. She had a previous history of perforating blunt trauma resulting in lens prolapse. After undergoing PKP, her IOP increased up to 40 mmHg. The first TLE failed due to existing conjunctival scarring, and after stabilization of her conjunctival inflammation she underwent AM-assisted TLE 8 months later.
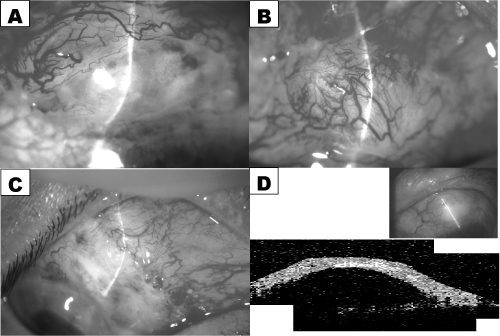
In all 6 cases, filtering blebs, comprised of an additional layer of AM with its epithelial side down, were established. The blebs functioned well without any leakage or wall thinning (Figure 2A-C). None of the patients experienced any ocular surface inflammation in the early postoperative phase, which often results in the failure of a conventional TLE in patients with glaucoma and ocular surface diseases.
The IOP time course of each case is shown in Figure 2. The mean IOP at pre-surgery and at 1, 3, and 7 years postoperative was 40.3±6.9, 23.0±12.1, 25.6±12.8, and 28.5±19.1 mmHg, respectively. Glaucoma medications decreased from 3.0±1.1 drugs (pre-surgery) to 0.8±1.0 (7 years postoperative). During the 7-year postoperative follow-up period, the IOP decreased compared to that at pre-surgery, although the patients’ filtering blebs were gradually becoming small and flat. However, in some cases the ocular surface conditions or VA worsened during the postoperative follow-up period.
We examined the sub conjunctival structure of the filtering bleb in the first case using optical coherence tomography (OCT-3000; Carl Zeiss Meditech, Ltd., Tokyo, Japan). This is a non-contact, non-invasive method to visualize not only the bleb wall constructed by the AM, but also the subconjunctival structure filled with aqueous humour. The OCT image showed a dome-shaped filtering bleb of equal thickness along the entire wall and a uniform subconjunctival lesion representing the aqueous humour posteriorly (Figure 2D).
Discussion
The effects of subconjunctival AM transplantation are two-fold, as the transplanted AM functions not only as a mechanical barrier, but also as a biological modifier. As a mechanical barrier, it patches the conjunctival hole or tear, strengthens the fragile wall of the bleb, and prevents aqueous humour from over-filtrating and bacteria from entering into the subconjunctival and intraocular space. As a biological modifier, the AM offers a foundation and substrate for the conjunctival basal cells that stimulates epithelialization, [15] traps polymorphonuclear cell infiltration, thereby preventing inflammation, [16] promotes wound healing by inhibiting protease activity, [17] and suppresses transforming growth factor beta (TGF-β) signaling, thereby exerting anti-scarring effects [18].
TGF-β reportedly plays an important role in conjunctival scarring after glaucoma surgery. Cordeiro et al. [19] investigated the effects of TGF-β1, -β2, and -β3 in vitro on Tenon’s fibroblast contraction, proliferation, and migration. They concluded that TGF-β, which exists in the anterior chamber and subconjunctival space, is implicated in the conjunctival scarring of the filtering bleb. Their group also reported the effects of a new recombinant human antibody to TGF-β2 on in vitro and in vivo conjunctival scarring and after glaucoma surgery [20,21]. We expect subconjunctival AM transplantation to have effects similar to those elicited by treatment of the subconjunctival tissue with anti-TGF-β2 antibody.
The two-fold effect of AM is derived from its histological structure; i.e., the epithelial cellular monolayer and the stromal layer, which have different characteristics. The stromal layer is beneficial as an extracellular matrix that promotes cellular proliferation and migration on the conjunctival epithelium, as epithelial cells produce cytokines to prevent severe scarring. Therefore, it may be important to place the AM epithelial-side-down on the scleral flap.
There are still many open questions regarding the use of AM in glaucoma surgery. For example, a question still exists as to whether or not the transplanted AM wall stays strong enough to maintain the filtering bleb wall for long periods. Also, it remains to be determined whether it is better to introduce the AM with the stromal side up or the epithelial side up on the scleral flap. In practice the filtering bleb used for our first patient consisted of two layers of AM and lasted for more than 2 years without dissolving. To determine the long-term prognosis regarding IOP control by AM-assisted TLE we continue to follow our patients carefully to identify and treat potential wound reopening or infection.
Recently, Nakamura et al. [22] also reported about AM-assisted TLE, comparing the intra-bleb structures of AM-TLE with those of TLE alone using an ultrasound bio microscope. The findings of that study revealed that the intra-bleb structures in AM-assisted TLE contained a wide fluid-filled space with a relatively thin wall, whereas those produced during TLE alone had no or minimal fluid-filled space. When the fluid-filled space extended posteriorly, IOP was reportedly well controlled, whereas if the eyes did not have any fluid-filled space or had a restricted space, the IOP control was poor. Case 1 in this present study also showed a large fluid-filled space with good IOP control at 2-years postoperative when examined by OCT (Figure 2D), yet the bleb size gradually decreased and IOP increased as time passed.
In conclusion, our new surgical technique that uses AM as an internal patch for TLE is an alternative treatment for patients with glaucoma and severe corneal disorders. However, special care and strict attention towards the condition of the ocular surface is required.
Acknowledgement
The authors wish to thank John Bush for reviewing the manuscript.
References
- Salvi M, Zhang ZG, Haegert D, Woo M, Liberman A, Cadarso L, et al. Patients with endocrine ophthalmopathy not associated with overt thyroid disease have multiple thyroid immunological abnormalities. J Clin Endocrinol Metab. 1990; 70: 89-94.
- McCorquodale T, Lahooti H, Gopinath B, Wall JR. Long-term follow-up of seven patients with ophthalmopathy not associated with thyroid autoimmunity: heterogeneity of autoimmune ophthalmopathy. Clin Ophthalmol. 2012; 6: 1063-1071.
- Eckstein AK, Plicht M, Lax H, Neuhäuser M, Mann K, Lederbogen S, et al. Thyrotropin receptor autoantibodies are independent risk factors for Graves' ophthalmopathy and help to predict severity and outcome of the disease. J Clin Endocrinol Metab. 2006; 91: 3464-3470.
- Paschke R, Vassart G, Ludgate M. Current evidence for and against the TSH receptor being the common antigen in Graves' disease and thyroid associated ophthalmopathy. Clin Endocrinol. 1995; 42: 565-569.
- Bahn RS. Clinical review 157: Pathophysiology of Graves' ophthalmopathy: the cycle of disease. J Clin Endocrinol Metab. 2003; 88: 1939-1946.
- Wiersinga WM, Bartalena L. Epidemiology and prevention of Graves' ophthalmopathy. Thyroid. 2002; 12: 855-860.
- Wall JR. The TSH-Receptor and Thyroid-Associated Ophthalmopathy-a Convenient Hypothesis with too many Exceptions to be true. Int J Endocrinol Metab. 2007; 5: 49-51.
- Tjiang H, Lahooti H, McCorquodale T, Parmar KR, Wall JR. Eye and eyelid abnormalities are common in patients with Hashimoto's thyroiditis. Thyroid. 2010; 20: 287-290.
- Gopinath B, Ma G, Wall JR. Eye signs and serum eye muscle and collagen XIII antibodies in patients with transient and progressive thyroiditis. Thyroid. 2007; 17: 1123-1129.
- Lytton SD, Li Y, Olivo PD, Kohn LD, Kahaly GJ. Novel chimeric thyroid-stimulating hormone-receptor bioassay for thyroid-stimulating immunoglobulins. Clin Exp Immunol. 2010; 162: 438-446.
- Lytton SD, Ponto KA, Kanitz M, Matheis N, Kohn LD, Kahaly GJ. A novel thyroid stimulating immunoglobulin bioassay is a functional indicator of activity and severity of Graves' orbitopathy. J Clin Endocrinol Metab. 2010; 95: 2123-2131.
- Lytton SD, Kahaly GJ. Bioassays for TSH-receptor autoantibodies: an update. Autoimmun Rev. 2010; 10: 116-122.
- Ardley M, McCorquodale T, Lahooti H, Champion B, Wall JR. Eye findings and immunological markers in probands and their euthyroid relatives from a single family with multiple cases of thyroid autoimmunity. Thyroid Res. 2012; 5: 4.
- Nunery WR, Martin RT, Heinz GW, Gavin TJ. The association of cigarette smoking with clinical subtypes of ophthalmic Graves' disease. Ophthal Plast Reconstr Surg. 1993; 9: 77-82.
- Mourits MP, Koornneef L, Wiersinga WM, Prummel MF, Berghout A, van der Gaag R. Clinical criteria for the assessment of disease activity in Graves' ophthalmopathy: a novel approach. Br J Ophthalmol. 1989; 73: 639-644.
- Werner SC. Classification of the eye changes of Graves' disease. Am J Ophthalmol. 1969; 68: 646-648.
- Weetman AP. Graves' disease. N Engl J Med. 2000; 343: 1236-1248.
- Gerding MN, van der Meer JW, Broenink M, Bakker O, Wiersinga WM, Prummel MF. Association of thyrotrophin receptor antibodies with the clinical features of Graves' ophthalmopathy. Clin Endocrinol (Oxf). 2000; 52: 267-271.
- Burch HB, Wartofsky L. Graves' ophthalmopathy: current concepts regarding pathogenesis and management. Endocr Rev. 1993; 14: 747-793.
- Won Bae Kim, Hyun Kyung Chung, Young Joo Park, Do Joon Park, Kazuo Tahara, Leonard D. Kohn, et al. The Prevalence and Clinical Significance of Blocking Thyrotropin Receptor Antibodies in Untreated Hyperthyroid Graves' disease Thyroid. 2000; 10: 579-586.
- Schott M, Minich WB, Willenberg HS, Papewalis C, Seissler J, Feldkamp J, et al. Relevance of TSH receptor stimulating and blocking autoantibody measurement for the prediction of relapse in Graves' disease. Horm Metab Res. 2005; 37: 741-744.
- Wall JR. Thyroid function. Pathogenesis of Graves ophthalmopathy--a role for TSH-R? Nat Rev Endocrinol. 2014; 10: 256-258.
- Gopinath B, Ma G, Wall JR. Eye signs and serum eye muscle and collagen XIII antibodies in patients with transient and progressive thyroiditis. Thyroid. 2007; 17: 1123-1129.
- Lahooti H, Parmar K R, Wall JR. Pathogenesis of Thyroid Eye Disease: important role of autoimmunity against calsequestrin and collagen XIII. A review. ClinOphthalmol. 2010; 14: 417-425.
- Salvi M, Miller A, Wall JR. Human orbital tissue and thyroid membranes express a 64 kDa protein which is recognized by autoantibodies in the serum of patients with thyroid-associated ophthalmopathy. FEBS Lett. 1988; 232: 135-139.