
Special Article - Cataract Surgery
Austin J Clin Ophthalmol. 2015;2(1): 1040.
Anterior Segment Optical Coherence Tomography in Anterior Dislocation of the Crystalline Lens
Jia-Kang Wang1,2,3,4
1Department of Medicine, National Yang Ming University, Taiwan
2Department of Ophthalmology, Far Eastern Memorial Hospital, Taiwan
3Department of Health Care Administration and Department of Nursing, Oriental Institute of Technology, Taiwan
4Department of Medicine, National Taiwan University, Taiwan
*Corresponding author: Jia-Kang Wang, Department of Medicine, National Yang Ming University, Taipei, 21, Sec. 2, Nan-Ya South Road, Pan-Chiao District, New Taipei City, 220, Taiwan
Received: February 13, 2015; Accepted: February 16, 2015; Published: February 17, 2015
Keywords
Anterior segment optical coherence tomography; Anterior dislocation of lens; Anterior chamber intraocular lens; Pars plana lensectomy
Clinical Image
A 54-year-old Taiwanese woman experienced blurred vision and pain in the left eye for one week. She suffered from head injury 9 years ago. Best-Corrected Visual Acuity (BCVA) was hand motion, and Intraocular Pressure (IOP) was as high as 80 mmHg in the left. Slit lamp biomicroscope showed the right crystalline lens dislocating to anterior chamber (Figure 1). Anterior segment optical coherence tomography (AS-OCT, RTVue, Optovue, CA, USA) demonstrated anterior capsule of the lens and corneal endothelium were very close (Figure 2). Fundus examination and macular OCT did not show macular abnormality. Anterior dislocation of the crystalline lens and acute secondary glaucoma were diagnosed. Treatment with intravenous mannitol, oral acetazolamide, and topical timolol and brimonidine eye drops proved ineffective in controlling the elevated IOP. Pars plana lensectomy with phacofragmentome and 20-gauge vitrectomy (Alcon lab, Texas, USA) were performed to remove the crystalline lens and prolapsed vitreous on the next day. Subsequent anterior chamber intraocular lens (MTA3UO, Alcon lab, Texas, USA) was inserted (Figure 3). Postoperative corneal edema gradually subsided. The IOP returned to normal value. Three months after the surgery, BCVA improved to 20/30.
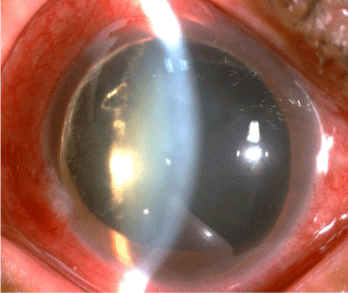
Figure 1: The crystalline lens dislocating to anterior chamber in the right eye.
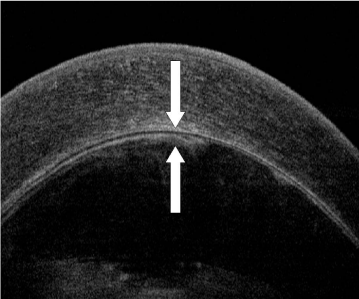
Figure 2: Anterior segment optical coherence tomography showed the anterior capsule of the lens (lower arrow) nearly touched the corneal endothelium (upper arrow).
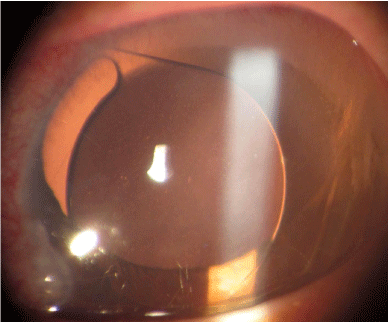
Figure 3: The anterior chamber intraocular lens was inserted.
Comment
Findings in AS-OCT were unique in the case with anteriorly dislocated crystalline lens. Proper removal of lens and intraocular lens insertion can improve vision and lower IOP effectively [1-3].
References
- Choi DY, Kim JG, Song BJ. Surgical management of crystalline lens dislocation into the anterior chamber with corneal touch and secondary glaucoma. J Cataract Refract Surg. 2004; 30: 718-721.
- Georgalas I, Ladas I, Papacostantinou D, Taliatzis S, Koutsandrea C. Management of crystalline lens dislocation into the anterior chamber in a victim of domestic violence. Clin Exp Optom. 2012; 95: 113-115.
- Salehi-Had H, Turalba A. Management of traumatic crystalline lens subluxation and dislocation. Int Ophthalmol Clin. 2012; 50: 167-179.