
Special Article - Ophthalmology: Clinical Cases and Images
Austin J Clin Ophthalmol. 2015;2(4): 1055.
Two Case Reports of HIV Related Optic Neuropathy
Elferink S¹*, Witmer AN² and Meenken C¹
1Department of Ophthalmology, VU Medical Center, Amsterdam, Netherlands
2Department of Ophthalmology, Onze Lieve Vrouwe Gasthuis Hospital, Amsterdam, Netherlands
*Corresponding author: Sjoerd Elferink, Department of Ophthalmology, VU Medical Center, Amsterdam, Netherlands
Received: May 01, 2015; Accepted: August 17, 2015; Published: August 27, 2015
Abstract
To report the importance of considering a primary Human Immunodeficiency Virus (HIV) infection in patients with unexplained optic neuropathy. Two separate patients are discussed in this article. The first patient was evaluated because of a decreased visual acuity in both eyes. Investigation showed bilateral optic disc edema. Further analysis with MRI and a lumbar puncture could not confirm a diagnosis. On a routine screening several months later the patient was tested positive for HIV and a re-evaluation of the Cerebrospinal Fluid (CSF) showed a high viral load. After treatment with antiretroviral therapy the papillary edema disappeared but visual acuity did not improve.
The other patient presented with unilateral complaints. Upon evaluation, a decreased visual acuity and unilateral optic disc edema was found. Further analysis showed visual field loss in both eyes. A CT scan showed no abnormalities. The patient was recently diagnosed with HIV, for which treatment was not yet started. Analysis of the lumbar puncture showed a high viral load. Visual acuity increased after antiretroviral treatment was started.
Keywords: Optic neuropathy; HIV; Cerebrospinal fluid; Viral load
Introduction
An important but rare cause of optic neuropathy is infection with HIV. More known ocular complications of HIV infection are HIV retinopathy and complications due to an opportunistic infection, such as Cytomegalovirus (CMV) retinitis. The occurrence of these complications is declining compared to the pre-antiretroviral therapy era but is still significant [1]. Optic neuropathy associated with HIV infection is described only in a few case reports in the literature and the pathophysiology is yet unknown. Especially when the diagnosis of HIV is not yet established, this diagnosis is easily missed and can have serious consequences for the patient.
Optic neuropathy refers to damage of the optic nerve. It is typically associated with visual field loss, dyschromatopsia and is often accompanied by a Relative Afferent Pupillary Defect (RAPD) if the neuropathy is unilateral. In several etiologies, it is associated with optic disc edema. Optic neuropathy has a broad differential diagnosis: it may be caused by ischemia, infectious or inflammatory causes, compressive/infiltrative lesions, toxic etiologies, trauma, hereditary causes or glaucoma [2].
We report on two HIV-positive patients with bilateral optic neuropathy and no signs of an opportunistic infection.
Case 1
An otherwise healthy 55-year-old male patient was referred to the outpatient clinic with a decline in vision in the left eye with a scotoma inferiorly since three weeks. His ocular history showed a moderate myopia in both eyes. Best Corrected Visual Acuity (BCVA) was 0.9 in the right eye and 0.4 in the left eye. No RAPD was present at presentation. Slit lamp biomicroscopy revealed no abnormalities, specifically no signs of uveitis. Fundoscopy revealed disc edema in both eyes (Figure 1a and 1b), most prominent in the left eye. No retinal hemorrhages or exsudates were present. Patient was then referred to the Department of Neurology for evaluation of intracranial pathology. Magnetic Resonance Imaging (MRI) of the brain and myelum showed no abnormalities. Lumbar puncture showed 10 cells with normal total protein count and glucose; opening pressure was within normal limits. Serology in the cerebral spinal fluid was negative for syphilis, Cryptococcus Neoformans and BorreliaBurgdorferi. Laboratory and radiologic examination revealed no active infectious parameters, nor active sarcoidosis.
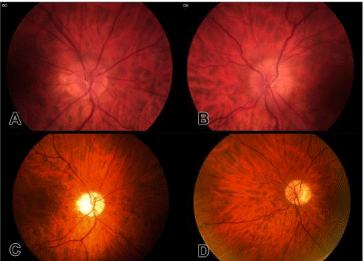
Figure 1: Fundus photographs of the optic discs of the right eye (a, c) and
left eye (b, d) before treatment (a, b) and after treatment (c, d). Note the
hyperemic discs with telangiectasia and blurring of the disc margin, more
prominent in the left eye before treatment. After treatment, the discs are pale
and well demarcated.
Two weeks later, BCVA decreased to 0.1 in the right eye and improved to 0.8 in the left eye. In accordance with the BCVA, the optic disc edema of the right eye increased; no changes in disc edema were observed in the left eye. Goldmannperimetry showed no defects in the right eye (Figure 2a) and a mild defect inferonasally in the left eye (Figure 2b). Genetic research for Leber optic neuropathy was negative.
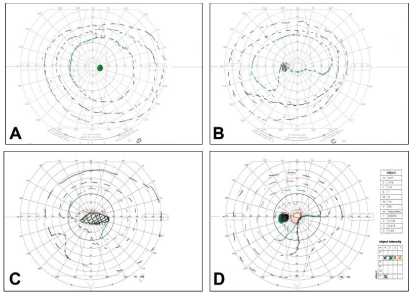
Figure 2: Goldmannperimetry of the right (a, c) and left (b, d) eye. Upon presentation, the right eye showed a normal visual field (a).The left eye showed a mild
inferonasal defect only visible for the I5 target (b). Within 18 months a dense cecocentralscotoma developed in the right eye (c). Likewise the inferior nasal defect
became more extensive in the left eye (d), including all isopters with a “sloping border”.
Six months prior to initial presentation, the patient tested negative on a routine HIV test. Six months after initial presentation, patient was tested positive for HIV on a routine test (viral load 250.000 copies/ml, 280 CD4 cells/ microliter). The lumbar puncture from the initial presentation was re-evaluated and showed a high viral load for HIV (8900 copies/ml). After treatment with Anti-Retroviral Therapy (ART), the viral load in the blood decreased. Lumbar puncture was not performed again. 18 Months after initial presentation, serology showed an undetectable viral load for HIV and 580 CD4 cells/ microliter. BCVA of both eyes were unchanged. On Fundoscopy the optic discs edema had disappeared and the discs were pale (Figure 1c and 1d). The visual field defects were more distinct (Figure 2c and 2d).
Case 2
An otherwise healthy 63-year-old male presented with a loss of vision based on cataract. His ocular history reported myopia in the right eye and hyperopia in the left eye. After an uncomplicated cataract extraction with phaco-emulsification and intraocular lens implantation in the right eye, BCVA increased from 0.3 to 1.0. At a routine follow-up visit 2 months post-operatively, slight optic disc edema in both eyes was observed. BCVA was unchanged; except for mild tenderness in the right eye upon ocular movement there were no ocular complaints. Shortly after, the patient was admitted at the Department of Internal Medicine for fever, diarrhea and loss of sensibility in the extremities. Investigation revealed a focal diverticulitis and an acute HIV infection. Because of a CD4 count of 350 cells /microliter ART was not immediately started. MRI with contrast of the brain showed no abnormalities. No lumbar puncture was performed at that time.
Four months after initial admission, the patient presented with painful eye movements and complaints of obscurations. BCVA in the right eye decreased from 1.0 to 0.2 and a RAPD was present. BCVA in the left eye was unchanged 0.8. Slit lamp investigation showed no abnormalities. Fundoscopy showed prominent optic disc edema in the right eye, and the optic disc was slightly elevated in the left eye. Visual field showed a cecocentralscotoma in both eyes (Figure 3a and 3b). CT scan without contrast showed no abnormalities. A lumbar puncture revealed a normal opening pressure and a high HIV viral load (16000 copies/ml). Serology showed a HIV viral load of 259.000 copies/ml and 390 CD4 cells/microliter. ART was started. 6 Months later, the HIV viral load was undetectable and CD4 count had risen to 700 cells/microliter. BCVA in the right eye increased to 0.5, BCVA in the left eye remained unchanged. The visual fields did not change. The optic discs were slightly pale but no optic disc edema was present.

Figure 3: Goldmannperimetry of the right (a) and left (b) eye. Note a cecocentralscotoma in both eyes.
Discussion
Globally, the number of new HIV infections continues to decrease;. In the Western World, with the availability of fast diagnostic tests and new treatments, advanced HIV-related pathology is less encountered [3].
HIV is neuroinvasive and has the potential to cause disease at any site of the neuro-axis during the evolution from seroconversion to late stage HIV [4]. In the literature, only a few cases of optic neuropathy related to HIV infection have been reported. In a prospective study, the prevalence of optic neuropathy in the early stages of HIV infection was 0.4% [5]. In addition, even without any visual complaints or visual loss HIV-positive patients may have visual field abnormalities [6]. Diffuse visual field loss predicts less survival in one study, with a trend to less survival with increasing field loss severity [7].
Several pathological mechanisms for HIV-related optic neuropathy are suggested. Histopathology results of optic nerves from HIV-positive individuals, without visual complaints or visual field loss and no retinitis, showed optic nerve axonal degeneration by HIV-infected macrophages [8]. Other studies suggest a mechanism of inflammation [9-12] with a good effect on visual function after the use of ART. Some patients showed a good response after the use of intravenously administered steroids [12-14]. In our first case, HIV infection was recognized only six months after initial presentation of ocular complaints and, thus, ART was started with some delay. It remains speculative whether the lack of increase in visual function is due to late start of treatment and whether earlier start would have resulted in an improvement in visual acuity.
In our cases, the diagnosis HIV-related optic neuropathy was a diagnosis by exclusion of other possible underlying causes and the presence of significant viral load of HIV in the Cerebrospinal Fluid (CSF). Research involving HIV viral load in CSF has been limited; a viral load, comparable with the viral load described in our cases can be found in HIV-positive individuals who are asymptomatic [15-18]. On the other hand, evidence of a CSF “escape” has been described in patients with neurologic symptoms, which were on ART and had low or undetectable plasma HIV levels [19]. Inflammation is then relatively compartmentalized in the central nervous system. Further investigation is required for a direct causative relationship between HIV viral load in CSF and optic neuropathy.
Conclusion
In case of an unknown optic neuropathy one should consider a primary HIV infection as the cause of the optic neuropathy.
References
- Jabs DA, Van Natta ML, Holbrook JT, Kempen JH, Meinert CL, Davis MD. Studies of the Ocular Complications of AIDS Research Group. Longitudinal study of the ocular complications of AIDS: 1. Ocular diagnoses at enrollment. Ophthalmology. 2007; 114: 780-786.
- Osborne B, Balcer L. Optic neuropathies. 2014.
- UNAIDS. AIDS by the numbers. 2013.
- Hogan C, Wilkins E. Neurological complications in HIV. Clin Med. 2011; 11: 571-575.
- Fabricius EM, Möller AA, Prantl F. [Disorders of the afferent visual pathway in HIV infection. 1. Optic nerve and 2. Visual pathways/visual cortex]. Fortschr Ophthalmol. 1991; 88: 721-730.
- Plummer DJ, Sample PA, Arévalo JF, Grant I, Quiceno JI, Dua R, et al. Visual field loss in HIV-positive patients without infectious retinopathy. Am J Ophthalmol. 1996; 122: 542-549.
- Sample PA, Plummer DJ, Mueller AJ, Matsubara KI, Sadun A, Grant I, et al. Pattern of early visual field loss in HIV-infected patients. Arch Ophthalmol. 1999; 117: 755-760.
- Sadun AA, Pepose JS, Madigan MC, Laycock KA, Tenhula WN, Freeman WR. AIDS-related optic neuropathy: a histological, virological and ultrastructural study. Graefes Arch Clin Exp Ophthalmol. 1995; 233: 387-398.
- Newman NJ, Lessell S. Bilateral optic neuropathies with remission in two HIV-positive men. J Clin Neuroophthalmol. 1992; 12: 1-5.
- Goldsmith P, Jones RE, Ozuzu GE, Richardson J, Ong EL. Optic neuropathy as the presenting feature of HIV infection: recovery of vision with highly active antiretroviral therapy. Br J Ophthalmol. 2000; 84: 551-553.
- Babu K, Murthy KR, Rajagopalan N, Satish B. Vision recovery in human immunodeficiency virus-infected patients with optic neuropathy treated with highly active antiretroviral therapy: a case series. Indian J Ophthalmol. 2009; 57: 315-318.
- Sweeney BJ, Manji H, Gilson RJ, Harrison MJ. Optic neuritis and HIV-1 infection. J Neurol Neurosurg Psychiatry. 1993; 56: 705-707.
- Burton BJ, Leff AP, Plant GT. Steroid-responsive HIV optic neuropathy. J Neuroophthalmol. 1998; 18: 25-29.
- Le Corre A, Robin A, Maalouf T, Angioi K. [Recurrent unilateral optic neuropathy associated with human immunodeficiency virus (HIV)]. J Fr Ophtalmol. 2012; 35: 272-276.
- von Giesen HJ, Adams O, Köller H, Arendt G. Cerebrospinal fluid HIV viral load in different phases of HIV-associated brain disease. J Neurol. 2005; 252: 801-807.
- Ellis RJ, Childers ME, Zimmerman JD, Frost SD, Deutsch R, McCutchan JA. HIV Neurobehavioral Research Center Group. Human immunodeficiency virus-1 RNA levels in cerebrospinal fluid exhibit a set point in clinically stable patients not receiving antiretroviral therapy. Journal of Infectious Diseases 2003; 187: 1818-1821.
- Chiodi F, Keys B, Albert J, Hagberg L, Lundeberg J, Uhlén M, et al. Human immunodeficiency virus type 1 is present in the cerebrospinal fluid of a majority of infected individuals. J Clin Microbiol. 1992; 30: 1768-1771.
- Schmid P, Conrad A, Syndulko K, Singer EJ, Handley D, Li X, et al. Quantifying HIV-1 proviral DNA using the polymerase chain reaction on cerebrospinal fluid and blood of seropositive individuals with and without neurologic abnormalities. Journal of acquired immune deficiency syndromes. 1994; 7: 777-788.
- Peluso MJ, Ferretti F, Peterson J, Lee E, Fuchs D, Boschini A, et al. Cerebrospinal fluid HIV escape associated with progressive neurologic dysfunction in patients on antiretroviral therapy with well controlled plasma viral load. AIDS. 2012; 26: 1765-1774.