
Special Article - Ophthalmology: Clinical Cases and Images
Austin J Clin Ophthalmol. 2016; 3(1): 1063.
Persistent Abducens Nerve Palsy after Successful Endovascular Treatment of a Dural Cavernous Sinus Arteriovenous Fistula
Neil R Miller¹* and James W McManaway²
¹Neuro-Ophthalmology Division, The Wilmer Eye Institute, The Johns Hopkins Hospital, USA
²Neuro-Ophthalmology Division, Hershey Pediatric Ophthalmology Associates, USA
*Corresponding author: Neil R. Miller, The Wilmer Eye Institute, Johns Hopkins Hospital, 600 North Wolfe Street, Baltimore, MD 21287-9204, USA
Received: November 03, 2015; Accepted: May 04, 2016; Published: May 12, 2016
Abstract
Although cranial neuropathies are not uncommon after endovascular occlusion of dural cavernous sinus arteriovenous fistulas (DCAVFs), they almost always resolve or at least improve. We report the case of a healthy 57-year-old woman who developed left proptosis, chemosis and conjunctival injection that led to a diagnosis of a left-sided DCSAVF. The fistula was successfully embolized using a combination of a detachable balloon and platinum coils; however, following treatment the patient developed a left sixth (abducens) nerve paresis that did not resolve and eventually required surgical correction. It is unclear if the sixth nerve palsy resulted from chronic ischemia due to interruption of the vascular supply to the abducens nerve or from direct compression of the nerve. Patients with DCAVFs for whom endovascular treatment is planned should be warned of the potential for both transient and persistent post-procedure diplopia that ultimately may require treatment.
Keywords: Dural arteriovenous fistula; Cavernous sinus; Sixth nerve palsy; Embolization; Superior ophthalmic vein; Endovascular
Introduction
Dural cavernous sinus arteriovenous fistulas (DCSAVFs) are abnormal communications between the meningeal branches of the external and/or internal carotid artery and the cavernous sinus that may require treatment by one of several endovascular techniques [1]. Although the endovascular techniques used to close DCSAVFs are generally safe, complications can occur regardless of the specific approach, the material used to close the fistula, and whether or not the fistula is successfully closed [1,2]. Most often, these consist of dysfunction of the cranial nerves within the cavernous sinus, with the abducens nerve being most frequently affected [2]. Such cranial neuropathies usually are transient, resolving within days to weeks after the embolization [2,3]. Occasionally, however, they persist. We describe a patient who developed an isolated, persistent abducens nerve palsy after successful endovascular closure of a DCSAVF and discuss the potential mechanisms by which this complication may have occurred.
Case Report
A 57-year-old woman with no history of head trauma began to hear a swishing sound in the left occipital region and then developed redness and swelling of her left eye. An examination revealed normal visual acuity, conjunctival chemosis of the left eye, 4 mm of left proptosis, and asymmetric intraocular pressures of 10 mmHg OD and 17 mmHg OS. Auscultation of the left orbit revealed a faint bruit. A diagnosis of probable DCSAVF was made, and the patient underwent magnetic resonance angiography that supported the diagnosis. A catheter angiogram demonstrated a left-sided DCSAVF fed by branches from the right internal and external carotid arteries as well as the left external carotid artery (Figure 1). It was elected to follow the patient in the hope that the fistula would close spontaneously. The patient did not improve over the subsequent 6 months. Accordingly, she underwent closure of the fistula using an inflatable balloon introduced into the cavernous sinus through the ipsilateral superior ophthalmic vein (SOV) in the manner first described by Miller et al. [4]. Prior to this procedure, the patient had visual acuity of 20/25 OU, with normal color vision, normal visual fields, and normally reactive pupils. Extraocular movements were full, and the patient was orthophoric at distance and near. The left eye was injected, with dilated, “arterialized” conjunctival and episcleral vessels (Figure 2). The irides were normal without evidence of rubeosis. Tensions were 6 mmHg on the right, and 15 mmHg on the left. Ocular pulse amplitudes were 1.4 mm on the right and 4.5 mm on the left. Ophthalmoscopy revealed a slightly hyperemic left optic disc and somewhat dilated retinal vessels. There were no retinal hemorrhages or exudates. The right optic fundus was normal in appearance. Exophthalmometry revealed values of 15 mm on the right and 19 mm on the left. Corneal and facial sensation were equal and normal bilaterally. The remainder of the patient’s neurologic examination was normal.

Figure 1: Preoperative cerebral angiogram shows an anteriorly draining,
left dural carotid-cavernous sinus fistula fed by branches of the right internal
and external carotid arteries. A, Selective right external carotid arteriogram,
anteroposterior view. Note main branch (arrow) to the left-sided fistula
(asterisk). B, Selective right internal carotid arteriogram, anteroposterior
view. Numerous small branches (asterisk) feed the fistula. Note early venous
drainage to the left transverse and sigmoid sinuses. The fistula also was fed
by branches from left external carotid artery (not shown).

Figure 2: External appearance of patient before embolization. Note proptosis
and marked injection of left eye with arterialized conjunctival vessels.
Postoperatively, the patient experienced a marked reduction of swelling and redness of the left eye but complained of double vision. An examination revealed normal visual sensory function, symmetric intraocular pressures and ocular pulse amplitudes, 3 mm of residual proptosis, and normal-appearing ocular fundi; however, there was a left sixth nerve paresis characterized by inability of the left eye to abduct to the midline and an esotropia of 60 prism diopters (PD) at distance and 40 PD at near, increasing on attempted left gaze and decreasing on attempted right gaze (Figure 3). Repeat cerebral angiography showed that the fistula was still open but now was draining posteriorly. Accordingly, platinum coils were detached into the cavernous sinus via the superior petrosal sinus, and acrylic glue was used to embolize several branches of the left external carotid artery. At the end of the procedure, angiography showed that the fistula was completely closed.
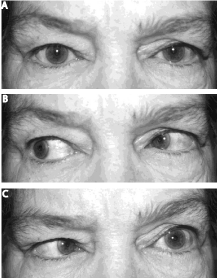
Figure 3: External appearance of patient after embolization. Note resolution
of left proptosis and injection; however, the patient now has weakness of
abduction of the left eye associated with a left esotropia, consistent with a
left abducens nerve paresis. A, primary position, B, right gaze, C, left gaze.
The patient was followed at regular intervals. Because there was no improvement in her sixth nerve paresis, she underwent injections of Botulinum A toxin (BotoxR) into the left medial rectus muscle 2 months and 4 months after surgery. No significant improvement occurred. A lateral skull x-ray revealed that both the balloon and coils were present within the left cavernous sinus (Figure 4). A repeat cerebral angiogram, which included selective injection of the right internal carotid artery and both external carotid arteries showed complete closure of the fistula with preservation of blood flow in the arteries (Figure 5). Brain magnetic resonance imaging 6 months after the embolization demonstrated only postoperative changes, without any evidence of mass effect. The patient subsequently underwent a lateral transposition of the left superior and inferior rectus muscles 1 year after the embolization, following which her diplopia resolved.
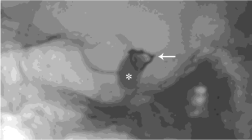
Figure 4: Lateral skull x-ray showing balloon (asterisk) and platinum coils
(arrow) in left cavernous sinus.
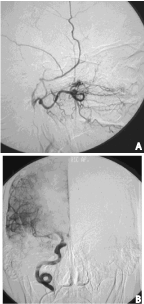
Figure 5: Postoperative cerebral angiogram showing complete closure of the
fistula with preservation of blood flow. A, Selective right internal maxillary
artereriogram, lateral view. B, Selective right internal carotid arteriogram,
anteroposterior view. There no longer is any early venous drainage (compare
with Figure 1B).
Discussion
Ocular motor nerve palsies related to DCSAVFs can occur as part of the orbital manifestations of an anteriorly draining fistula or as isolated signs in patients with fistulas that drain posteriorly into the inferior petrosal sinus (IPS) and cortical veins [1]. Most of these palsies resolve or recover within several weeks or months after endovascular treatment [2,3]. New ocular motor nerve palsies also occur after both transarterial and transvenous IPS embolizations; however, the also tend to resolve [2,3,5,6]. For example, three of 13 patients (Pts #4, 10 and 13) in the series reported by Nishina et al. [2] developed new abducens nerve pareses after complete obliteration of their DCSAVF using platinum coils. The paresis resolved in two of the patients (Pts #4 and 13) and improved in the third (Pt #10). Bink et al. [3] reported the resolution of new post-procedural ipsilateral oculomotor and abducens nerve pareses in one patient (Pt #4) with a DCSAVF who also was treated with transvenous coiling. A review of articles using PubMed revealed only one previous case of a permanent sixth nerve palsy after transvenous embolization of a DCSAVF via the SOV cited in the literature [7].
Several mechanisms could have produced the permanent sixth nerve palsy in our patient. The cavernous portion of the abducens nerve is supplied mainly by the dorsal meningeal branch of the meningohypophyseal trunk which originates from the cavernous portion of the internal carotid artery [8]. Obstruction of this trunk by a balloon placed in the cavernous sinus may have produced ischemia of the neural structures supplied by the trunk, including the abducens nerve. Obstruction of the sinus by a venous approach could also have produced acute elevated pressure in the veins normally draining the cavernous sinus, thereby inducing a venous infarct of the sixth nerve [9]. This is an unlikely mechanism in this setting of an isolated sixth nerve palsy, because most venous infarcts cause more widespread damage and would be expected to affect more than one cranial nerve within the cavernous sinus.
Compression of the sixth nerve must be also considered in this case. For example, the detachable balloon could have compressed the sixth nerve within the cavernous sinus, and the compression could have increased after platinum coils were introduced into the sinus. This mechanism was thought to have been responsible for one of the cases reported by Aihara et al. [9], although their patient recovered spontaneously. Compression of the sixth nerve also could have occurred within Dorello’s canal. This osteofibrous conduit is located at the level of the petrous apex, and it is through this structure that the sixth nerve courses to reach the cavernous sinus [8]. Thus, the sixth nerve can be compressed against the walls of the canal by a balloon or coils that migrate into the canal or by a distended IPS [10]. This latter mechanism is thought to explain the occasional development of an isolated sixth nerve palsy in posteriorly draining fistulas [11] and could have occurred when introduction of a detachable balloon into the cavernous sinus via the SOV in our case caused the previously anteriorly draining fistula to drain posteriorly; however, if this were the mechanism, we would have expected the palsy to have resolved once the fistula was closed.
Whatever the mechanism of the sixth nerve palsy in our patient, it is clear that permanent cranial neuropathies, including ocular motor nerve palsies, can occur after otherwise successful endovascular treatment of a DCSAVF. This potential risk must be considered and discussed with the patient prior to such treatment, particularly in a patient without pre-existing double vision.
References
- Miller NR. Carotid-cavernous sinus fistulas. Miller NR, Newman NJ, Biousse V, Kerrison JB, editors. In: Walsh and Hoyt’s Clinical Neuro-Ophthalmology 6th edn. Baltimore, Williams & Wilkins. 2005; 2: 2263-2296.
- Nishino K, Ito Y, Hasegawa H, Kikuchi B, Shimbo J, Kitazawa K, et al. Cranial nerve palsy following transvenous embolization for a cavernous sinus dural arteriovenous fistula: association with volume and location of detachable coils. J Neurosurg. 2008; 109: 208-214.
- Bink A, Goller K, Lüchtenberg M, Neumann-Haefelin T, Dützmann S, Zanella F, et al. Long-term outcome after coil embolization of cavernous sinus arteriovenous fistulas. AJNR. 2010; 31: 1216-1221.
- Miller NR, Monstein LH, Debrun GM, Tamargo RJ, Nauta JWN. Treatment of carotid- cavernous sinus fistulas using a superior ophthalmic vein approach. J Neurosurg. 1995; 83: 838-842.
- Tsai FY, Hieshima GB, Mehringer CM, Grinnell V, Pribram HW. Delayed effects in the treatment of carotid-cavernous fistulas. See comment in PubMed Commons below AJNR Am J Neuroradiol. 1983; 4: 357-361.
- Debrun G, Vinuela F, Fox A, Davis K, Ahn H. Indications, treatment and classification of 132 carotid cavernous fistulas. Neurosurgery. 1988; 22: 285- 289.
- Gioulekas J, Mitchell P, Tress B, McNab AA. Embolization of carotid cavernous fistulas via the superior ophthalmic vein. Aust NZ J Ophthalmol. 1997; 25: 47-53.
- Umansky F, Elidan J, Valarezo A. Dorello’s canal: a microanatomical study. See comment in PubMed Commons below J Neurosurg. 1991; 75: 294-298.
- Aihara N, Mase M, Yamada K, Banno T, Watanabe K, Kamiya K, et al. Deterioration of ocular motor dysfunction after transvenous embolization of dural arteriovenous fistula involving cavernous sinus. Acta Neurchir. 1999; 14: 707-710.
- Newton T, Hoyt W. Dural arteriovenous shunts in the region of the cavernous sinus. Neuroradiology. 1970; 1: 71-81.
- Acierno MD, Trobe JD, Cornblath WT, Gebarski SS. Painful oculomotor palsy caused by posteriorly-draining dural carotid cavernous fistulas. Arch Ophthalmol. 1995; 113: 1045-1049.