
Special Article - Ophthalmology: Clinical Cases and Images
Austin J Clin Ophthalmol. 2016; 3(1): 1065.
Role of Impression Cytology in Detecting Gobletcell Damage in Various Ocular Surface Disorder
Thatte Shreya* and Garg Poorvi
Department of Ophthalmology, Shri Aurbindo Institute of Medical Sciences, India
*Corresponding author: Thatte Shreya, Department of Ophthalmology, Shri Aurbindo Institute of Medical Sciences, 17, Yeshwant Colony Behind Sita Building , Indore (MP), India
Received: March 16, 2016; Accepted: May 25, 2016; Published: May 30, 2016
Abstract
Purpose: Normal ocular surface is maintained by healthy goblet cells.Any insult to normal ocular surface can lead to changes in goblet cells. The amount of changes in goblet cells depend on severity of OSD. The aim of this study is to demonstrate the correlation between goblet cells alteration and OSD using impression cytology.
Material and Method: Thirty nine cases with veneralkeratoconjuctivities (8), stevenjohnson syndrome (6), squamous cell carcinoma (4), pingecula (3), conjunctival melonosis(1), primary pterygium (10) and recurrent pterygium (7) were included in this study and underwent impression cytology.
Result: Changes in goblet cells morphology,studied by impression cytology were classified according to Saine et all criteria. Grade1 impression cytology changes were seen in conjunctival melanosis.Mild to moderateVKC, SJS, pingecula and recurrent pterygium showed grade 2 impression cytology changes.Incidence of grade 3 impression cytology was observed in squamous cell carcinomaand severe VKC. Grade 2 and 3 impression cytology changes were seen in primary, fleshy pterygium in equal percentage.
Conclusion: Impression cytology is a simple non invasive technique which offers to evaluate damage to goblet cell morphology which is helpful in detecting severity of OSD.
Keywords: Ocular surface; Impression cytology; Goblet cell morphology
Abbreviations
OSD: Ocular Surface Disorders; VKC: Veneral Kerato Conjuctivities; SJS: Steven Johnson Syndrome; PAS: Periodic Acid Schiff
Inroduction
Ocular surface consist of bulbar conjunctiva, palpebral conjunctiva, forniceal conjunctiva, limbus, corneal epithelium and pre corneal tear film [1].
Tear film maintains clarity of the cornea by regulating the moisturizationof the conjunctiva and the cornea.Ocular surface protects the globe from mechanical, toxic and infectious trauma¹.
Classification of ocular surface disorders [2].
1. OSD due to conjunctival etiology – goblet cell deficiency, formation of pseudomembranes, formation of follicles.
2. OSD due to tear film- due to lipid deficiency,lid related disorders , evaporative dry eye and aqueous tear deficiency.
3. OSD due to limbal stem cell deficiency.
Conjunctiva has a major contribution in ocular surface and goblet cell are indispensible part of ocular surface. Therefore alteration in ocular surface affects goblet cells morphology .
Goblet cells
These are non keratinized cells located within the epithelium of bulbar conjunctiva which are more dense in lower nasal area and least in upper temporal fornix [3,4]. Main function of these cells is to secrete mucous, innermost layer of tear film which protects ocular surface from dryness. Mucous covering is essential to keep cornea and conjunctiva moist inorder tomaintaining a healthy OS.
Goblet cell population increases in chronic inflammation and diminishes in OS disorders like dry eye syndrome, pterygium, neurotrophic keratitis, atopy, seasonal ocular allergy. Population and morphology of goblet cells can be studied by impression cytology (IC).
Impression cytology
Impression cytology was first described by Egbert et al in 1977 [5]. Usually diagnosis of OSD is made by clinical assessment, but changes in goblet cells are confirmed by impression cytology, which is a standard evaluation to assess goblet cell morphology.It refers to the application of a cellulose acetate filter to the ocular surface to remove the superficial layers of the ocular surface epithelium which are subjected to histological, immunohistological or molecular analysis [6]. Most commonly used stains are Periodic Acid Schiff and Papanicolaou stain.Generally 2 to 3 layers of cells are removed in one application but deeper cells can be accessed by repeat application over same site. Impression cytology is a minimally invasive method with little patient discomfort and relatively easy method to study conjunctival goblet cells morphology and density. The use of impression cytology is indicated in order to identify etiological diagnosis of preclinical lesions and to typify the OSD. Application include etiological diagnosis of variouspre clinical and established ocular surface disorders,ocumenting sequential changes in the conjunctival and corneal surface over time, pre and post treatment of dry eye, staging of squamous metaplasia and monitoring effects of treatment [6].
Materials and Method
It is prospective monoinstitusional study done within a span of one year . Patients attending out patient department with clinically diagnosed as cases of OSD were examined and those gave consent for the investigative procedure of impression cytology were enrolled . Thus we could include thirty nine eyes of various types of ocular surface disorder in the study,
Patients with VKC (8), SJS (6), squamous cell carcinoma (4), pingecula (3), conjunctival melonosis (1), primary pterygium (10) and recurrent pterygium (7) underwent impression cytology, were included in the study (Figure 1).
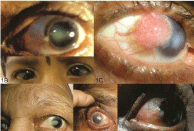
Figure 1: Various clinical pictures.
1A Pingecula
1B Veneralkeratoconjuntivities
1C Squamouscell carcinoma
1D Grade 2 atrohic pterygium
1E Steven Johson syndrome
1F Grade 2 fleshy pterygium
Exclusion criteria included patients with history of using any topical drugs, intraocular surgery, systemic diseases (diabetes mellitus, rheumatic arthritis), contact lens users and associated ocular pathology.
A detailed ocular symptoms and accurate anamnesiswere recorded. Onset, persistence and progression of reduction of vision, foreign body sensation, redness watering, growth in conjunctiva were reported.
Visual acuity and best corrected visual acuity were recorded. Ocular examination in detail was done on slit lamp to rule out any other associated ocular disease. Anterior segment wasevaluatedfor corneal, anterior chamber, iris and pupil pathology. Dilated fundus examination was done using 90D lens to examine the status of retina. Intraocular pressure was noted by using schiotztonometeryto excludeglaucoma.
Acetate cellulose filter paper strips of pore size 0.20 μm, 13 mm diameter by Sartorius stedim biotech was used for conjunctival impression cytology. The filter paper was cut into 2x2mm square size. Impression of conjunctival goblet cells was taken on dull surface of the paper and other surface was mark to identify the stained surface. In the present study, cut pieces of filter paper were placed 2mm away from limbus in all four quadrants of conjunctiva (superior, nasal, temporal and inferior) (Figure 2).
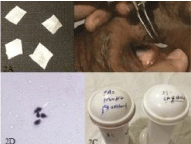
Figure 2: Method of impressincyotology.
2A- Acetate cellulose filter paper cut into strips.
2B- Placing of filter paper in the inferior quadrant of eye with the help of force
2C- bottles containing stains.
2D- microscopic view of goblet cells.
The paper was allowed to remain in contact with the conjunctivafor 5-10 seconds. With the help of blunt end of the forceps gentle pressure was applied over the strip for 3-5 seconds. This strip was peeled off with forceps. Filter paperwascut into pieces for two different fixative solutions and then transferred to marked glass slide. Marking of glass slide included registration number of the patient, eye and the quadrant from which sample was taken. After transferring filter paper to glass sides, slides were fixed in two different solutions. In first fixative solution, containing 70% ethyl alcohol, 37% formaldehyde and glacial acetic acid in a recommended standard volume ratio of 20:1:1, slides were fixed for 10 minutes and stained with PAS and haematoxylin stain. Second solution containing 95% ethyl alcohol slides were fixed for 5 minutes and stained with Papanicolaou stain . Both slides are cleared with xylene and viewed under a light microscope.
Grading
The entire slides were examined to determine the nature of the cytological changes occurring in goblet cells morphology.
Staging of conjunctival goblet cells density was based on Saini et al.’s criteria.
Grade 1: Small round epithelial cells with a cytoplasm to nuclear ratio of 1:2. Large numbers of deeply positive goblet cells present.
Grade 2: A good cell sheet consisting of larger polygonal epithelial cells with a decreased cytoplasmicnuclear ratio of 1:3. Goblet cells were reduced in number, but still deeply PAS-positive.
Grade 3: Larger polygonal cells with a further decrease in cytoplasmic to nuclear ratio with reduced number and in staining of goblet cells.
Grade 4: larger polygonal basophilic cells with pyknotic nuclei with demonstrable intracellular keratin and absent goblet cells (Figure 3).
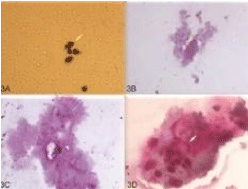
Figure 3: Different grade of impression cytology.
3A- Grade 1 Goblet cell changes: Small round epithelial cells, Nucleus to
cytoplasm ratio of 1:2, Deeply staining of goblet cells.
3B - Grade 2 Goblet cell changes: Sheet of larger polygonal epithelial cells,
Decreased nucleocytoplasmic ratio of 1:3, Goblet cells reduced in number,
Deeply PAS-positive goblet cells
3C- Grade 3 Goblet cell changes: Decrease in nucleus to cytoplasmic ratio,
Reduced staining of goblet cells.
4D- Grade 4 Goblet cell changes: Intracellular keratin, Absent goblet cells.
Results
Of all thirty nine cases (Table 1, Figure 4), 20.51% patients were affected byVKC. These cases were classified according totheseverity of symptoms and signs into mild, moderate and severe. Cases with only foreign body sensation with photophobia and occasional use of anti allergic drops were grouped under mild VKC. Moderate cases were classified as presence of photophobia with daily use anti- allergic drops. Severe category included corneal disease with use of daily steroids. Six (75%) cases of mild to moderate VKC showed 20% of alteration in goblet cellsmorphology out of all grade 2 impression cytology changes. Two (25%) patients of severe VKC had 25% of total grade 3 impression cytology changes.
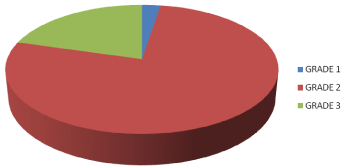
Figure 4: Showing different grade of impression cytology in different OSD.
Grades of IC
Disease
Total
Grade 1
Conjunctival melanosis (1)
1
Grade 2
Mild to moderateVKC (6), SJS(6),
pingecula (3), recurrent pterygium (7) and Grade 2 pterygium (8).
30
Grade 3
SCC(4), Severe VKC (2) and Grade 2 pterygium (2).
8
Grade 4
-
-
Total
-
39
Table 1: Different grade of impression cytology in different OSD.
All the seven (17.9%) Of recurrent pterygium in the study had 23.3% of all grade 2 impression cytology changes.
Among thirty nine cases, ten (25.6%) withprimary pterygium were included in the study. All the pterygium included were of grade 2 (less than 2mm involvement of cornea) [3]. According to nature, eight were of fleshy variety and 2 were of atrophic variety. Six fleshy pterygium and 2 atrophic pterygium showed grade 2 (26.6%) impression cytology changes; 2 fleshy pterygium showed grade 3 impression cytology changes (25%).
There were 6 (5.38%) cases of SJSin the study, and all showed grade 2 impression cytology changes. That are 20% of all grade 2 impression cytology changes found in the study.
In total of thirty nine patients, four (10.25 %)were of squamous cell carcinoma. All of these cases showed grade 3 impression cytology changes leading to 50% changes of total grade 3 impression cytology changes.
Three (7.69%) pingecula included in the study showed 10% of all grade 2 impression cytology changes.
It was reported only one (2.56%) case of conjunctival melanosis which showed grade 1 impression cytology changes.
Grade 2 impression cytology changes were observed in Mild to moderate VKC, SJS, pingecula, recurrent pterygium and Grade 2 pterygium.
Squamous cell carcinoma,Severe VKC and Grade 2 pterygium had grade 3 impression cytology changes.
There were no grade 4 impression cytology changes in our study.
Discussion
Impression cytology of the conjunctiva is considered an important diagnostic tool in assessing the goblet cell morphology in ocular surface disorders.
Dr.PushpaVerma et al havefound 2 of 7 patients with VKC had abnormal results of impression cytology. They concluded that impression cytology is an novel approach in evaluation of ocular surface changes [7].
In our study we evaluated eight patients with VKC, out of 6 were of mild to moderate VKC while 2 had severe VKC. Mild to moderate VKC had grade 2 impression cytology changes while severe VKC showed grade 3 impression cytology changes .
NapapornTananuvat et al compared the results of impression cytology with histolpathology of the lesion ina series of fifty five patients with ocular surface neoplasia. They concluded that impression cytology has a high positive predictive accuracy in diagnosing ocular surface neoplasia compared with tissue histology [5] .
In our study there were 4 cases with squamous cell carcinoma, impression cytology in all cases showed dysplastic changes.
R Singhetetal observed that grade 2 ocular surface changes occurs in eyes with SJS which similar to our experience .
Our study, accordance with the study of Xing Ming EN et al, stated that extension of ocular surface damage caused by pterygium is directly related to nature and corneal encroachment of pterygium [8].
Pre-operative impression cytology helped in diagnosing lesions in which there was clinical delima and according to IC grading intra and post operative treatment could be planned. As in cases with squamous cell carcinoma IC helped to decide treatment strategy with wide excision with intraoperative use of mitomycin C which helped in minimising recurrences and modification of rountine line of mangement of cases . Patients with VKC, grade 3 changes were kept on prolong treatment helping to decrease in frequency of symptoms there by lowering recurrences in such patients.
Impression cyotology serves as a valuable tool in screening of patients with ocular surface disorders with positive predictive value comparable to histopathology [5].
Conclusion
Impression cytology is a simple non invasive, technique which consents to evaluate damage to goblet cell morphology which is helpful in detecting severity of OSD. Although it is a economical technique , but a help of pathologist is required for the procedure and interpretation to diagnose severity of pathology.Impression cytologyaided a tool in medical and surgical management of the various OSD cases.
References
- Clinical Opthtalmology. 9th edn. 2011.
- Kruse FE. Classification of ocular surface disorders: ocular surface disease: Medical and surgical management. 2002.
- Kanski. Clinical Ophthalmology. 7th edn. 2011.
- Anthony J. Bron, Ramesh C. Tripathi, Brenda J, Tripathi. The ocular appendages: eyelids conjunctiva and lacrimal apparatus. In Wolf’s Anatomy of the eye and orbit, 8th edn. 2-6 Boundary Row, London SE 1BHN, UK: chapman and Hall. 1997; 51-70.
- Cornea Lippincott. Williams & Wilkins. 2008; 27: 261-389.
- Singh R, Joseph A, Umapathy T, Tint NL, Dua HS. Impression cytology of the ocular surface. See comment in PubMed Commons below Br J Ophthalmol. 2005; 89: 1655-1659.
- Pushpa Verma, Srivastava U, Singh S, Priti Meshram, Sheetal Paunikar. Conjunctival impression cytology a dignostic boon in diagnosis of dry eye in normal tear function test. AIOS proceedings. 2010.
- Xing Ming EN. Correlation Analysis Of Ocular Surface Changes and Clinical Characteristics of Pterygium J. 2012; 33: 223-227.