Abstract
Cravings for food as appetite and hunger is a healthy reflex reaction to the body’s need for nutriment, just as thirst is the subjective physiological reaction to dehydration. Hypothalamic neuro-peptides released in response to nutritional demands affect brain circuits driving hunger. Unusual cravings for non-nutritive foods or uncontrollable desires for odd choices or combinations of food may manifest during different altered physiological states. Cissa or cittosis is a craving for strange unusual, sometimes unwholesome, foods often encountered during pregnancy. Pica is a depraved or perverted appetite with hunger for non-nutritive substances not fit for food. Pica and cissa may occur separately, simultaneously or asynchronously. This article appraises odd cravings occasioned by pica and cittosis, related physiology of thirst and hunger, some dysfunctions of these, and defines distinctions between physiological demands for nourishment and the discussed cravings.
Keywords: Appetite; Cissa; Cittosis; Coprophagia; Chlorosis; Galanins; Hunger; Leptons; Thirst; Pica; Pregnancy
Introduction
During active synthetic anabolic states such as during pregnancy and lactation, and growth-spurt periods, as well as during silent or altered states of malnutrition, the body may release substances which cause conscious or sub-conscious cravings, seeking of foods to compensate for the body’s requirement. Neuro-peptides are released in the hypothalamus through obscure mechanisms, in response to fluctuating circulatory molecules. These neuro-peptides modulate our hunger as well as affecting higher centers in the choice of foods to satisfy. For example leptins and or galanins are released in response to high or low metabolic-molecule levels respectively and will moderate hunger. Liquid intake will usually quench a thirst in a healthy person, as will increased intake of food satisfy hunger [1,2]. However, cravings and compulsive consumption of strange foods, often obtains during pregnancy [3,4]. It also occurs in the young, or among those with dysfunctional physiological states. Nutritive or non-nutritive foods consumed may satisfy these cravings. Many obtuse references to these cravings exist but few explain, clarify or differentiate them [3-6].
Physiology of thirst and hunger
Healthy functioning of human physiology demands intake of water and nutritionals as food and drink. Inadequate food leads to chronic starvation, but lack of liquid results in dehydration with thirst, and relative to starvation, may result in a rapid demise. The average daily intake for liquid is 1.5 to 3 L per day, depending on physical activity, ambient temperature and other food intake. Consequently liquid deprivation leading to thirst is a basic drive to imbibe water. Prime among theories of thirst production, is the ‘dry mouth reflex’ in which a dry mouth and pharynx, due an excess of salivary evaporation, results in an increase flow of saliva that moistens the pharynx and thirst is suppressed. When dry mucous membranes of the pharynx without salivary flow is sustained, thirst is initiated and maintained till the individual corrects the situation by taking a drink [1,2]. Subtle changes in blood osmotic pressure due to hemoconcentration stimulates baroreceptors in the cardio-vascular system and also assists as a stimulus acting on the thirst center in the hypothalamus [2].
When the human body requires energy and/or metabolites to function, most people experience sensations of hunger. Body energy stores are used for ongoing daily physiological homeostasis; for long-term survival human tissue reserves, as carbohydrates, fats and proteins, are drawn into active metabolism which allows for shortterm energy demands. The food sources vary in their caloric density with protein and carbohydrates providing four kilocalories (kcals) per gram, and fats nine kcal per gram. Living cells derive energy from these fuels for many types of mechanical, chemical, osmotic, electrical and thermal work which they are required to do. Even in health, energy requirements for individuals vary widely and depends on their physical activity and on whether other metabolic processes are active, such as during menstruation, pregnancy and lactation, or with growth during childhood, puberty and adolescence [3-6].
A group of hypothalamic neuro-peptides, of which leptins and galanins dominate, are released into the blood as hormones to moderate hunger, satiety and associated pleasures arising, and are also present in the circulation during pregnancy [7-13].
Galanin
The GAL gene encodes for galanin; [7] the gene is most prevalent in the brain, but also in the spinal cord, and gastro intestinal tract of mankind and mammals. Galanin effector molecules may dock into three G protein-coupled receptors sites. Galanin is associated with a wide variety of biological reactions, including: pain, consciousness and slumber, cognition, eating, mood moderation, stabilizing blood pressure, and functions as a trophic factor in growth and development [8] Galanin is also associated with other pathologies such as eating disorders, depression, Alzheimer’s disease, epilepsy and cancer [9,10]. Galanin provokes an urge for high energy foods, like fats and sugars. Blood circulating galanin reaches throughout the body, including peripheral hormone producing organs and the brain. Low galanins are associated with satiety and fat and alcohol consumption seems to lower blood galanin levels.
Leptin
Leptin (from leptos Greek: denotes thin) is a protein16 kDa hormone which is important in appetite control, by moderating energy intake and expenditure. Leptins suppresses appetite, and is released after eating, when hunger is sated and thirst is slaked [11]. It is one of the most important adipose derived hormones [12] The Lep gene (or ObLep gene: Ob for obese, Lep for leptin) is located on chromosome 7 in humans [13]. Both neuropeptides (leptins and galanins) influence cerebral cortex centers that control higher orders of decision taking.
In pregnancy, for the mother to sustain her own body weight, she requires extra energy synthesis of complex compounds needed for healthy growth and development of the placenta, embryonic membranes, and her foetus. During the first trimester these requirements are small, but in the last trimester with rapid foetal growth, a daily extra 10% energy requirement of about 200kcal per day is common. Energy requirements during lactation are even greater than that required during pregnancy. If the milk requirement of an infant is about 1000kcal per day, daily intakes of food by the mother has to increase by at least 50% for the mother to sustain her own body weight. When these extra energy requirements are not provided adequately from food, the pregnant or lactating woman must mobilize fat deposits, or after their depletion, proteins from muscle and other protein fiber reserves [6,10]. During nutritionally stressed periods, galanins provoke stimulations to consume high amounts of fats and alcohol. In so doing the individual may divert their choices and develop cissa or pica. The precise mechanism of galanin action inducing cravings during pregnancy remains obscure. No specific nutrient deficiency has been defined for cravings, but according to the Journal of American Dietetic Association, iron deficiency chlorosis and cissa are possibly positively linked. Chlorosis is a form of chronic hypochromic microcytic (iron deficiency) anaemia [14-16]. Preferred consumption of sweet food during the third trimester may collectively reflect interactions between psychological, behavioural and physiological variables [17].
Cissa or cittosis
Cissa or cittosis (Greek: kissa, a craving for strange food) is a craving for unusual or rare elements of food. Cissa or pica (see below) may manifest during pregnancy, diabetes mellitus, cerebral tumours, anorexia nervosa, bulimia nervosa, and chlorosis [13,18-20]. Both cissa and pica cravings may manifest simultaneously or alternate asynchronously [11]. Many believe these cravings derive from intuitive corporal homeostatic mechanisms, as the body seeks out needed molecules like vitamins, minerals or trace elements missing or inadequate in a person’s diet. Malnutrition, physical, or mental illness and stress, all may be contributory etiologic agents with cravings.
Pica
Pica (Latin for magpie, a bird notorious for eating or carrying away odd objects). Pica is compulsive eating of non-nutritive substances [12]. Examples include crunching ice, (referred to as pagophagia), eating dirt (geophagia), laundry starch (amylophagia), hair (trichophagia), eating feces (coprophagia), or other substances easily at hand like gravel, flaking paint, plaster clay, paper or cardboard. When infants grow, thrive and develop, there is a tendency from about 18 months for a year afterward, to initiate and repeat pica experiences by bringing everything to the mouth [13]. This occurs about the second year of life, remits after a few months, but may persist into adolescence when pica is classified as DSMM- R, a rare mental disorder. Pica cravings are most commonly seen in children and occur in approximately 25-30% of all children. Most females experience some form of craving during pregnancy (as cissa above); yet the vast majority of these cravings are for high gustatory foods or odd combinations, such as ice-cream and sour pickles, or shellfish with chocolate. Pica cravings are most prevalent in children, and pica cravings in pregnant women though far less common, are more bizarre. Obesity seems to be related to circulating serum leptins predisposing to developing pica [21]. The calorie requirement is 2400kcal in pregnancy and 2750kcal in lactation. The daily extra energy requirement in the last trimester of pregnancy is generally 300-400kcal., during lactation 500kcal [22]. Some pregnant women crave daily sucking lemons and this habit could destroy a dentition through acid erosion (Figure 1).
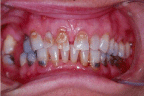
Figure 1: Destructive dental erosion (Chemical dissolution of tooth material
without bacteria or cavitations).
The dentition was destroyed from cravings for daily lemon sucking during pregnancy. Frequent, chronic repeated dental exposure to the acids in fresh lemon juice causes dental erosion.
Chewing paper or rubber bands is common as a pica observed among young school-going children [18]. Typical of the most common choices for substances craved during pregnancy are: dirt (soil), clay, and laundry starch. Other pica cravings include: burnt matches, ash, (Figure 2) stones, charcoal, mothballs, ice, cornstarch, toothpaste, soap, sand, plaster, coffee grounds, baking soda, and cigarette ashes [19].

Figure 2: Cooled ash from fires is often eaten by people suffering from pica.
Satisfying pica cravings may prove harmful to a fetus. Consuming unusual substances as food may harm both mother and child; these irregular food sources could disrupt absorption of other foods, and cause nutrient deficiency. These cravings may be toxic (like lead from paints) or introduce parasites (from geophagia or coprophagia) [13,18-19,23].
Concluding Remarks
Pica is a universal problem among pregnant women, affecting all socio-economic groups [5,24-30] and includes sweet and sugar cravings during pregnancy [31-32].
Cravings to over-eat, derives from disruption of central neuropeptides. For example resistance to leptins increases appetite and is attributed to fostering obesity [10-13]. Understanding cravings occur among growing children and infanticipating women, should allow for implementing therapeutic controlling and management strategies. Most cravings are not deemed pathological, but when manifest, should be discussed and if possible re-directed to eating healthy alternatives. For pregnant women, open transparent discussion of driving desires, pangs and cravings about diet is essential. Sharing awareness of cravings with health care professionals, friends and family also helps in controlling and avoiding cravings by redirecting them away from poor choices. For children, vigilance and ongoing observation of behavior is essential, and once noted, guidance, removal of offending substances and communicating (teaching, talking explaining and role-modeling) all play part in successfully resolving cissa and picca. Making healthy nutritious alternate foods easily available, especially for children and pregnant women, assists in minimizing eating unusual foods.
References
- Cannon WB. Digestion and Health. Passim. Secker and Warburg, London. 1937.
- Jenkins GN. In: The Physiology and Biochemistry of the Mouth. 4th Edn. G Neil Jenkins, Ch IX Saliva, Saliva. Water balance 344-345. Blackwell Scientific Publications. 1978.
- Shaw JH. In: Textbook of Oral Biology. Shaw JH, Sweeney EA, Capuccino CC, Meller SM, Eds. Ch 11. Nutrition. WB Saunders. 366-367.
- Bowen DJ, Grunberg NE. Variations in Food Preference and consumption across the menstrual cycle. Physiology& Behavior. 1990; 47: 287-291.
- Mikkelsen TB, Andersen AM, Olsen SF. Pica in pregnancy in a privileged population: myth or reality. Acta Obstet Gyecol Scand 2006; 85:1265-1266.
- Worthington-Roberts B, Little RE, Lambert MD, Wu R. Dietary cravings and aversions in the postpartum period. J Am Diet Assoc. 1989; 89: 647-651.
- Evans H, Baumgartner M, Shine J, Herzog H .Genomic organization and localization of the gene encoding human preprogalanin. Genomics 1993; 18: 473–477.
- Mitsukawa K, Lu X, Bartfai T. Galanin, galanin receptors and drug targets. Cell. Mol. Life Sci. 2008; 65: 1796–1805.
- Mechenthaler I. Galanin and the neuroendocrine axes.Cell. Mol. Life Sci. 2008; 65: 1826–1835.
- Lundström L, Elmquist A, Bartfai T, Langel U. Galanin and its receptors in neurological disorders. Neuromolecular Med. 2005; 7: 157–180.
- Zhang F, Basinski MB, Beals JM,Briggs SL,Churgay LM,Clawson DK, et al.Crystal structure of the obese protein leptin-E100. Nature. 1997; 387: 206–209.
- Brennan AM, Mantzoros CS. Drug Insight: the role of leptin in human physiology and pathophysiology--emerging clinical applications. Nat Clin Pract Endocrinol Metab. 2006; 2: 318–327.
- Green ED, Maffei M, Braden VV, Proenca R, DeSilva U, Zhang Y, et al. The human obese (OB) gene: RNA expression pattern and mapping on the physical, cytogenetic, and genetic maps of chromosome 7. Genome Res. 1995; 5: 5–12.
- Shaw JH. In: Textbook of Oral Biology. Shaw JH, Sweeney EA, Capuccino CC, Meller SM, Eds. Ch 11. Nutrition 366-369. WB Saunders.
- Stedman’s Medical Dictionary. Hensyl WR and Oldham JR, managing editors. 24th Edn. Williams and Wilkins. 1984; 284.
- Dorland’s Illustrated Medical Dictionary. Taylor EJ, Editor. 27th Edn. WB Saunders Pa USA. 1988; 1293.
- American Pregnancy Association. 2000-2009. Passim.
- American Academy of Family Physicians. 2009.
- American Dietetic Association.
- Bowen DJ. Taste and food preference changes across the course of pregnancy. Appetite. 1992; 19: 233-242.
- Considine RV, Sinha MK, Heiman ML, Kriauciunas A, Stephens TW, Nyce MR, et al, Serum Immuno-reactive-Leptin Concentrations in Normal-Weight and Obese Humans. N Engl J Med 1996; 334: 292–295.
- Corbett RW, Ryan C, Weinrich SP. Pica in preganancy: does it affect preganancy outcomes? MCN Am J Matern Child Nurs. 2003; 28: 183-189.
- Lopez LB, Ortega Soler CR, de Portela ML. Pica during pregnancy: a frequently underestimated problem. Arch Latinoam Nutr. 2002; 54:17-24.
- Saunders C, Padhila P deC, Della-Libera B, Nogueirs JL, Oliveira LM, Astulla A. Pica: epidemiology and association with pregnancy complications. Rev Bras Gynecol Obstet. 2009; 31: 440-446.
- Horner RD, Lackey CJ, Kolasa K, Warren K. Pica practices of pregnant women. J Am Diets Ass.1991; 91: 34-38.
- Ngozi PO. Pica practices of pregnant women in Nairobi Kenya. East Afr Med J. 2008; 85: 72-79.
- Simpson E, Mull JD, Longley E, East J. Pica during pregnancy in low income women born in Mexico. West J Med. 2000; 173: 17-24.
- Nyaruhucha CN. Food cravings, aversions and Pica among pregnant women in Dar Es Salaam Tanzania. Tanzan J Health Res. 2009; 11: 29-34.
- Sule S, Madugu HN. Pica in Pregnant women in Zaria, Nigeria. Niger Med. 2001; 10: 25-27.
- Elfhag K, Tynelius P, Rasmussen F. Sugar-sweetened and artificially sweetened soft drinks in association to restrained, external and emotional eating. Physiol Behav. 2007; 91: 191-195.
- Sygo J. Cleveland Clinic Canada. Jennifer Sygo: Resident Nutritionist. 2011.
- Geigy Scientific Tables. Lentner C, Ed. Recommended daily intakes of energy and nutrients. (Dept of Health and Social Security). 1984; 234.
