
Review Article
J Dent & Oral Disord. 2016; 2(2): 1013.
Oral Nutritional Health Risk Assessment: A Systematic Approach
Naik PR¹, Ravikiran A¹, Samatha Y¹, Nayyar AS²* and Vijay Kumar A¹
¹Department of Oral Medicine and Radiology, Sibar Institute of Dental Sciences, India
²Department of Oral Medicine and Radiology, Saraswati- Dhanwantari Dental College and Hospital and Post- Graduate Research Institute, India
*Corresponding author: Nayyar AS, Department of Oral Medicine and Radiology, Saraswati-Dhanwantari Dental College and Hospital and Post-Graduate Research Institute, India
Received: February 27, 2016; Accepted: April 26, 2016; Published: April 28, 2016
Abstract
A nutrient is a chemical that an organism has to exist and grow or a substance used in an organism’s metabolism which must be taken in from its milieu, which enriches the body. They are used to build and repair tissues, regulate the body processes and converted to and used as energy. Nutrition is a fundamental constituent of all living beings. There is a constant synergy between nutrition and the integrity of the oral cavity in health and disease. The World Health Organization defines malnutrition as the cellular imbalance between supply of nutrients and energy and the body’s demand for them to ensure growth, maintenance, and specific functions, often, the very early signs of sub-optimal nutritional status are initially seen in the oral cavity, which has been described as a “mirror of nutritional status”. Dental health professionals are, therefore, in a position to be the first to notice compromised nutrition, and a sound knowledge of the symptoms and signs permit them to take the appropriate action. For this, one should go in a systematic approach to assess the oral nutrition health risk of an individual. Hence, we are presenting herewith, might be a first of its kind of review, about how to approach to oral nutritional health risk assessment in a systematic way.
Keywords: Nutrition; Risk assessment; Dental health professionals; Oral health
Introduction
Nutrition is to be taught of how food affects the body, and is the sufficient provision of materials like vitamins, minerals, fiber, water and other food components to cells and organisms, to support life [1]. Nutrition affects oral wellbeing, and oral health affects nutrition. Nutrition is a key factor in disease and inflammation. An ample number of reports emphasize the synergistic association between malnutrition, infectious diseases and the immune system [2]. A responsibility for dental health professionals in providing dietary recommendation is being encouraged, and consequently knowledge of the consequences of compromised nutritional status on the oral health is necessary in order to accomplish this vital role, thereby, mandating, the dental health professionals to identify when a patient needs to be referred to a dietitian, and, similarly, dietitians should recognize the oral symptoms of nutritional deficiencies [3]. It is the responsibility of dental health professionals and dietitians to carryout the baseline assessment of oral and nutritional status and provide appropriate education, and refer patients accordingly to the suitable healthcare professionals [4]. The risk assessment process for dental health professionals and dietitians might differ to some extent in the approach; however, the outcomes and goals, in either case, are alike.
The aim of oral nutritional health risk assessment
The most imperative aim of oral nutritional health risk assessment is early recognition and intervention to lessen the occurrence and severity of nutritional risks and to maximize response to treatment.
Determining oral nutritional health risk
Nutritional risk factors are defined as “characteristics that are associated with an increased likelihood of poor nutritional status” [5]. The type and extent of these risk factors determines the nutritional risk. For this, dental health professionals should know the various risk factors as shown in Table 1. Nutritional risk assessment includes subjective statements in relation to the diet, oral well-being, biting and chewing capability, weight history as well as objective evaluation of the height, weight, and the state of the oral cavity. In addition to this, more extensive physical and laboratory evaluation becomes necessary when patients with complex medical histories are subjected to nutritional risk assessments [6].
CONDITION
SEVERITY OR TYPE OF INVOLVEMENT
1.
Acute or Chronic diseases
Anorexia, Autoimmune disorders, Multiple sclerosis, Bulemia, Musculoskeletal disorders, Cardiovascular disease, Neoplastic disease, Craniofacial anomalies, Osteoporosis, Developmental disorders, Diabetes, Disorders of taste and olfaction, Poor dentition/edentulism, Early childhood caries , Protein-energy malnutrition/wasting, End-stage renal disease, Erosion, Radiation therapy, Salivary dysfunction, Gastrointestinal disorders, Hypertension, Immunocompromising conditions (e.g., cancer, HIV infection, AIDS), Ulcers in the oral cavity, Juvenile periodontitis, Kaposi’s sarcoma, Xerostomia, Lupus, Zinc deficiency.
2.
Caries
Extensive involvement.
3.
Masticatory compromise
Biting/Chewing /Swallowing difficulties.
4.
Weight
Inadvertent and rapid weight loss/gain.
5.
Disorders
Related to Cranial nerves.
6.
Dental procedures
Altered ability to eat a usual diet.
7.
Pain
Chronic orofacial, Acute oral pains.
8.
Xerostomia
Salivary glands.
9.
Oral infections
Ulcerations/lesions.
10.
Diet
Inadequate intake.
11.
Taste
Altered taste sensation.
12.
Poverty
Poor.
Table 1: Risk factors for determining oral nutritional health risk.
History taking
A comprehensive patient history is the prime and most significant step in the nutritional risk evaluation by the dental health professionals as a part of routine care. Apart from asking patients about routine histories, diet and nutritional risk evaluation and supplemental questions related to oral health and nutrition should also be asked. A questionnaire based study can be done regarding the food habits, living situations, needs, desires and goals so that the first hand information could be obtained which can be added to the assessment of risk.
Medical history
Medical history has a very imperative role in the risk assessment. Each and every dental health professional must obtain a thorough history about the systemic status or general health status of the patient, in order to obtain the information related to acute or chronic disease states or immunological disorders, which are the prime risk factors for individuals with concurrent oral or dental problems that influence their ability to consume their usual diet [7]. One should rule out the following systemic disorders by asking supplemental questions, that include 1) Diabetes mellitus, 2) autoimmune diseases such as pemphigus vulgaris, 3) Inflammatory arthritides, 4) Xerostomia associated with Sjögren’s syndrome, 5) Pain related to temporomandibular joints, 6) Head and neck oral cancers, 7) Radiation therapy, 8) Individuals with HIV infection or acquired immunodeficiency syndrome (AIDS), 9) Oral complications and malnutrition secondary to the disease process and associated gastrointestinal, metabolic, immune, pharmacological, and psychosocial sequelae [8]. All the above mentioned disorders will directly or indirectly cause periodontal disease, dysgeusia, increased caries risk, candidiasis, burning tongue, and poor wound healing, in addition to joint pain or mechanical limitation, and alteration in the quantity and quality of saliva, eventually leading to a compromised masticatory ability, and compromised nutritional status.
Drug history
Patients must be cautiously questioned about use of prescription and Over-The-Counter (OTC) drugs, as well as use of herbs, minerals and vitamins, and other dietary supplements, because patients might be using drugs for various systemic or local disorders. These medications might affect an individual’s capability to consume, assimilate, and absorb an adequate diet [9]. This in turns leads to a compromised nutrient intake. Several groups of drugs which cause these consequences include the anti-vials’, anti-fungal, antihypertensive, anti-parasitic, anti-retroviral, anti-depressants, antihistaminics, narcotics, sedatives, and anti-neoplastic drugs. Alcohol disturbs nutrient metabolism primarily through its effect on the liver and other organs. Alcohol-induced abnormal pancreatic function leads to changes in vitamin absorption and utilization. Alcohol interferes with thiamine metabolism, resulting in deficiency that in its extreme form can cause Wernicke-Korsakoff syndrome, a chronic degenerative neurologic disorder. History regarding dietary habits while using some drugs for systemic health is also of paramount importance. A drug-food interaction occurs when the food one has disturbs the metabolism of the drug taken so that the drug does not work the way it should. Drug-food interactions can happen with both prescription as well as over-the-counter drugs, including antacids, vitamins and the usually prescribed iron supplements as well as it can be the other way round when the drug taken affects the absorption of the food consumed.
Personal dietary habits
Personal dietary habit assessment should include general questions about type of food intake and regarding previous and current dietary habits and also should focus on dietary patterns, nutritional adequacy, and factors influencing eating and fluid intake. A 24-hours recall, or recall of a typical day’s diet, provides a clear picture of the patient’s dietary pattern and a global assessment of the nutrient intake. For a precise evaluation of nutrient adequacy, the diet may be analyzed by means of many computerized nutrient analysis packages, including Interactive Healthy Eating Index, accessible free on the internet. This provides an assessment of actual calories and macro- and micro-nutrient intake according to an individual’s gender, age, and body size [10].
History of dietary supplements
As a part of a routine history and even follow-up schedule, questions about the use of dietary supplements, dosages, forms, and frequency of intake of such supplements must be incorporated. Select dietary supplements might alter the integrity of the oral cavity and impede the action of certain drugs, and/or, alter response to a select therapy.
Comprehensive oral examination
Dental health professionals should carry-out a comprehensive oral examination as a routine, during the initial visit of every patient, to distinguish unusual findings and symptoms related to diet and nutrition, provide basic education, and refer patients to the registered dietitians, if in case, the need is felt for a referral and opinion. Comprehensive oral examination should include lips, labial and buccal mucosa, gingiva, tongue, palate, floor of the mouth, teeth, salivary flow and TMJ. For every part, one should inquire about patient complaints, duration of symptoms, acuity, frequency of complaints, pain and any changes in the appearance and associated symptoms [11] (Table 2).
AREA OF INTEREST
FINDINGS TO BE CHECKED
1.
Lips
Angular cheilitis, Delayed wound healing, Dryness, Fissuring of lips, swellings, ulcerations.
2.
Labial and Buccal mucosa
Stomatitis, Burning sensation of oral mucosa, Aphthous ulcers, Delayed wound healing, Mucosal atrophy, Candidosis, Bad taste, Halitosis, Red or white patches/lesions, pigmentations.
3.
Gingiva
Bleeding gums, Bruising, Delayed wound healing, Recurrent aphthae, Candidiasis, Gingivitis/periodontitis, Changes in the consistency and appearance, Red or white patches/lesions, pigmentations.
4.
Tongue
Glossitis, Redness and burning of the tongue, Split tongue, Reduced taste perception, Candidosis, Red or white patches/lesions, pigmentations, ulcerations, growths.
5.
Palate
Delayed wound healing, Recurrent aphthae, Candidosis, Red or white patches/lesions, pigmentations.
6.
Floor of the mouth
Burning of oral mucosa, Delayed wound healing, Recurrent aphthae, Red or white patches/lesions, pigmentations.
7.
Teeth
Impaired tooth formation, Impaired tooth development, Hypoplasia, if deficiency occurs during tooth mineralization, Post-extraction hemorrhage, Mobility.
8.
Salivary glands
Xerostomia, Glandular pain or swelling, Sialorrhoea,Altered consistency and color.
9.
TMJ
Difficulty or painful opening, Difficulty in chewing, Weakness, atrophy or, hypertrophy of masticatory muscles.
Table 2: Areas presenting with patient complaints and changes in the appearance and associated symptoms.
Eating disorders
Individuals with eating disorders are at high oral and nutritional risk. Therefore, features of Anorexia and Bulemia nervosa should be examined for. Anorexia involves who purposely starve themselves, when they are already underweight and in contrast, to those with anorexia, individuals with bulemia, consume large amounts of foods during binge episodes, during which they feel out of control of their consumption. The cardinal oral manifestations include severe erosion of enamel on the lingual surfaces of the maxillary teeth. Also, fingernails of the patients reveal abnormalities related to the use of fingers to initiate purging. Parotid enlargement might also be seen as a sequela of constant and chronic starvation as also the soft tissue changes in the mucosa due to gastric acids [12].
Osteoporosis
The association between osteoporosis and oral health is progressively more obvious predominantly in reference to periodontal disease and implant surgical procedures. The existing studies usually support the theory that osteoporosis and osteopenia are associated with an adverse impact on oral health, particularly tooth loss in the elderly. However, the majority of the evidence to date comes from cross-sectional studies that cannot decide whether changes in the skeleton precede the oral conditions or result from risk factors common to both the conditions [13].
Pregnancy, child nutrition and oral health
The nutritional intake of a female during pregnancy has a significant impact on the development of dentition of the developing fetus apart from affecting the development and maturation of other oral and para-oral tissues as well. The specific effects are related to the formation of enamel and dentin of the primary and permanent dentition during fetal development. Insults from teratogens or lack of critical nutrients during pregnancy can also have a significant impact on the development of dentition as well as other oral and para-oral structures. A review of Early Childhood Caries (ECC) and hypoplasia in infants and children in developing countries revealed that these conditions were most closely associated with a general underlying nutritional deficiency state (malnutrition or under-nutrition) during the peri-natal period.
Drawing conclusion
A thorough history and intensive oral and peri-oral examination make the dental health professionals draw a conclusion about the precise risk factors, and oral health risks. Through history and intense oral and peri-oral examination like overall well-being of the oral cavity and general physical health, chewing ability, quality, quantity and nature of diet, height and weight ratio, in addition to these extensive physical and laboratory examination should be done to draw a correct conclusion so that it helps the dental professional to know about the precise risk factors, willpower of nutrition, and oral health risk [13,14].
Discussion with patient about recommendation to improve diet
The conclusion of the assessment should be discussed with the individuals in detail and dental health professionals should educate and motivate the affected individuals to meet oral and nutritional health needs; thereby, promoting health and preventing disease risk by focusing on risk identification and risk reduction, important parts of a preventive health care.
Nutrition education
Dental professionals and registered dietitians need to form networks with other general health care providers to advance health promotion and preventive and community health initiatives that endorse oral health and nutrition as they narrate to general health.
Suggestion for diet modification
This includes, eating little but frequent, high energy, high protein snacks and meals. Oral dietary supplements are a top-up to food intake rather than a substitute; they should be given between meals, and not at meal times.
Referral to (RD) Registered Dietitian for MNT (Medical Nutrition Therapy)
Once the patient is at nutritional risk, dental health professionals should consult with and refer the patients to a registered dietitian for MNT (Medical nutrition therapy) and management of nutritional risk reflected by a compromised oral health (Table 3).
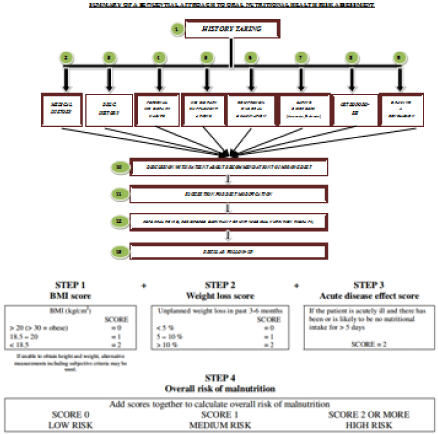
Figure 1: Sequential approach to Oral Nutritional Health Risk Assessment.
Conclusion
Having Knowledge about the consequences of a compromised nutritional status on oral health is the most fundamental and vital part for the dental health professionals, because nutrition is an integral constituent, where there is an unremitting synergy established between nutrition and the integrity of the oral cavity in health and disease; so, a systematic approach might help in judging the individuals with nutritional risk and can be prevented from its harshness.
Acknowledgement
We are earnestly grateful to our beloved teachers and dynamic friends for constantly helping us out and to come-up with this informative converse. Thanking you all.
References
- Moynihan P. The interrelationship between diet and oral health. Proc Nutr Soc. 2005; 64: 571-580.
- Mangan DF. Nutrition and oral infectious diseases: Connections and future research. Compend Cont Educ Dent. 2002; 23: 416-422.
- Mandel ID. Oral infections: Impact on human health, well-being, and health-care costs. Compend Cont Educ Dent. 2002; 23: 403-413.
- Position of the American Dietetic Association. Oral health and nutrition. J Amer Dietet Assoc. 2003; 103: 615-625.
- American Academy of Family Practice. Nutrition Screening Initiative. 2002.
- Touger-Decker R, Sirois DA, Connie C Mobley. Text book of Nutrition and Oral Medicine. V session. 17th chapter.
- Slavkin HC, Baum BJ. Relationship of dental and oral pathology to systemic illness. J Am Med Assoc. 2000; 284: 1215-1217.
- Sirois DA. Oral manifestations of HIV disease. Mt Sinai J Med. 1998; 65: 322-332.
- Feelds-Gardner C. Position of the American Dietetic Association and Dietitians of Canada: Nutrition intervention in the care of persons with human immunodeficiency virus infection. J Am Diet Assoc. 2000; 100: 708-717.
- Anonymous. Interactive Healthy Eating Index. 2002.
- Fitzsimons D, Dwyer JT, Palmer C, Boyd LD. Nutrition and oral health guidelines for pregnant women, infants and children. J Am Diet Assoc. 1998; 98: 182-186.
- Text book of Burket’s oral medicine diagnosis and treatment. 10th Edition. 14th Chapter.
- Wactawski-Wende J. Periodontal diseases and osteoporosis: Association and mechanisms. Ann Periodontol. 2001; 6: 197-208.
- Malnutrition screening and Nutritional assessment