
Special Article - Oral Cancer
J Dent & Oral Disord. 2016; 2(3): 1016.
Oral Squamous Cell Carcinoma in Young Indian Women -A Growing Concern
Jayalekshmy R¹* and Balan A²
¹Department of Oral Medicine & Radiology, Vydehi Institute of Dental Sciences, India
²Department of Oral Medicine & Radiology, Government Dental College, Thiruvananthapuram, India
*Corresponding author: Jayalekshmy R, Department of Oral Medicine & Radiology, Vydehi Institute of Dental Sciences, India
Received: March 28, 2016; Accepted: May 02, 2016; Published: May 03, 2016
Abstract
Oral Squamous Cell Carcinoma (OSCC) was considered as a disease of old age. Recent trends of increasing incidence of OSCC in young population especially women without the exposure of any potential risk factors have been noted. The causes for the increased incidence still remains an enigma, but might result from changing exposures to extrinsic risk factors and their interplay with intrinsic factors. The reported cases of OSCC in young women patients are increasing worldwide and also in developing countries like India and it is indeed an alarming situation. In view of this alarming trend this article highlights an update and a case series of OSCC with an overview of the risk factors in oral carcinogenesis.
Keywords: Oral squamous cell carcinoma; Carcinogenesis; Oral cancer
Introduction
Oral squamous cell carcinomas are the sixth most common cancers in the world [1]. India being called as the oral cancer capital of the world, OSCC represents the commonest cancer in males and the third commonest cancer among females [2]. Oral squamous cell carcinoma is predominantly seen in the middle and old age and is a rarity in those below 45 years [3]. Cancer of the oropharyngeal region is most common in the 6th or 7th decade of life [4]. The high prevalence of oral cancer in India is attributed to the widespread habit of tobacco chewing smoking and alcoholism. All the documented studies on oral cancer risk factors relate to their prolonged exposure in the middle aged and elderly population.
According to the recent reports, 6% of oral cancer occurs in the younger age group (<45 years) and is a cause of concern [4]. There is absolute absence of the potential risk factors in these young adults [3]. Interestingly, there is an unexpected increase in the incidence of OSCC in young women without any specific etiologic factors and tongue is the most common affected site [5,6,7]. This led to the consideration of other factors like viral infections EBV [8], HPV [9,10], immunosuppression [11], familial factors [12], genetic [13], chronic irritation [5], dietary factors [14] and hormonal factors [15] to be implicated in oral carcinogenesis.
Considering the alarming trend of the increasing incidence of OSCC in young Indian women without any significant risk factors, this article highlights an update and a case series of OSCC with an overview of the risk factors in oral carcinogenesis.
Case Presentation
Five cases of oral cancer in young female patients are presented here. All the patients were below 45 years of age. Their medical history and family history were noncontributory. They did not give any history of tobacco habits or alcoholism. Two patients reported chronic irritation from sharp teeth which were of a very short duration of one month. Four patients presented with ulceroproliferative growths on the lateral border of tongue and one patient presented with an ulceroproliferative growth on the palate. All the lesions clinically presented with indurate margins. No premalignant lesions or conditions were identified in this group. All the cases showed multiple palpable lymph nodes with hard consistency and were fixed to the underlying structures. Following the assessment of routine blood and urine investigations, an incision biopsy of sufficient width and depth to ensure inclusion of connective tissue was taken from the representative area in each case under local anesthesia. The tissue specimens were snap frozen in liquid nitrogen and stored in -800c freezer till use. DNA isolation from the specimens followed by quantitation was done. PCR was used to amplify the integrated viral DNA of HPV in the tissue specimen using DNA polymerase enzyme and two oligonucleotide primers. MY09, MY11 along with HPV 16 and HPV 18 forward and reverse primers were used for HPV genotyping. Among the five cases, two were positive for HPV 16. All the lesions were histopathologically confirmed as well differentiated oral squamous carcinoma. The patients were referred to Regional Cancer center for further management. In all our cases surgical excision of the lesion was done with radical neck dissection which was followed by a regimen of radiotherapy. The representative photographs are shown in Figure 1 & Figure 2.
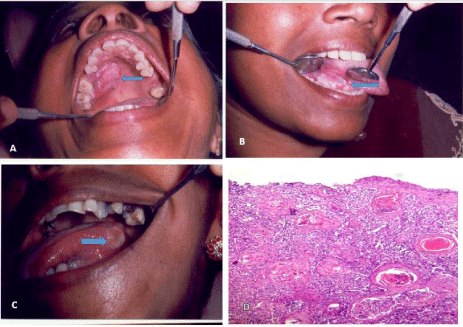
Figure 1: (A) Ulceroproliferative growth on the right hard palate. (B)
Ulceroproliferative growth on the right lateral border of tongue. (C)
Ulceroproliferative growth on the left lateral border of tongue. (D) H&E sectionparakeratinised
epithelium showing breach in the basement membrane.
Epithelial islands are seen in the form of nests in connective tissue with
keratin pearl formation. Dense inflammatory infiltrate and few blood vessels
are seen in connective tissue. Histopathological features suggestive of well
differentiated squamous cell carcinoma of tongue.
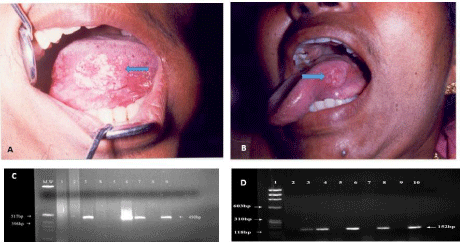
Figure 2: (A & B) Ulceroproliferative growth on the left lateral border of
tongue. (C) Picture of agarose gel showing HPV positive cases at 450 bp.
(D) Picture of agarose gel showing HPV 16 positive cases at 152 bp.
Discussion
Oral cancers constitute a heterogeneous group of cancers that arise in various sub sites of the oral cavity with differing predisposing factors, prevalence and outcomes. Globally there is an upsurge of increasing incidence of cancers of the oral cavity and the oropharynx among younger adults ranging between 1-6% with tongue being the commonest site of involvement [16-18]. Oral carcinoma in younger patients was considered to be an etiologically distinct entity from oral cancers in older patients owing to less significant exposure to risk factors such as tobacco and alcohol. Several studies in the Indian subcontinent as well in western world reported a disproportionate increase in OSCC of tongue in young women without any contributing factors [18-22]. Oral carcinogenesis being multifactorial, extensive research has been focused on geographical, dietary factors, chronic irritation, oncogenic virus like HPV, immunosuppression, role of sex hormones etc in the pathogenesis of OSCC in women population [4]. Unfortunately, no definite etiology or risk factors have been identified.
Among the five cases of OSCC in young females, only two tongue carcinomas were positive for HPV 16. Epidemiologic evidence suggests that the incidence of HPV-associated oral and oropharyngeal cancers has been on the rise over the past four decades, especially in young females without significant habits. This could be attributed to multiple sex partners and increasing orogenital sexual practices which cause transmission of oncogenic human papillomavirus and other sexually transmitted carcinogenic vectors [23]. Further research into the sexual practices among the young patients may be warranted. However later studies have shown that the incidence of HPV in nontobacco related oral tongue cancer was low and unlikely to constitute a significant factor in the rising trend of oral tongue cancer in the young population [24,25]. A need for large multivariate cross sectional and longitudinal studies in this cohort may be advocated combining both epidemiological and molecular approaches to establish a significant correlation with HPV.
Chronic irritation to the tongue in the form of ill-fitting appliances, prosthesis, or sharp teeth is considered to be one of the predisposing factors in OSCC of lateral tongue. The repeated trauma may expose the germinal basal cells to the entry of dietary carcinogens, act as a stimulus for uncoordinated proliferation. Among our five cases two of them had tooth trauma which was of a very short duration of one month. Some studies have demonstrated that in some OSCC patients an exaggerated response to inflammation due to polymorphisms of IL6 and TNF alpha has been noted this could result in a carcinogenic effect at a site of inflammation [26]. This warrants the need for the elimination of factors causing chronic irritation to the oral mucosa at an early stage for the prevention of OSCC.
Since there is an upsurge in Oral tongue SCC in women who were non-smokers and non-drinkers not associated with HPV, it becomes crucial to introspect whether female sex hormones and other endocrine hormones have an impending role in oral carcinogenesis. Sex hormones are believed to play a vital role in gene expression involved in the biological and neoplastic events. A study demonstrated that OSCC patients have altered estrogen metabolism which may represent an intrinsic risk factor for Oral carcinogenesis [27]. In a study by Schuller et al. Estrogen metabolism genes were present on the cell lines derived from HNC [28]. Various studies have demonstrated increased levels of Follicular Stimulating Hormone (FSH), Luteinizing Hormone (LH), and prolactin, and decreased ratio of testosterone: Estradiol in tongue cancer patients [29,30]. In a case control study, women using oral contraceptives were found to have polymorphisms in DNA repair genes (Xeroderma Pigmentosum Group D (XPD), which could pose them a high risk for developing squamous cell carcinoma [31]. Since there is paucity of large scale studies about the influence of hormones on the development and progression of OSCC in young women, further research at a molecular level about the expression of hormone receptors in this group is advocated.
Several case control studies have established that a diet rich in fruit and vegetables and low in meat and products of animal origin has aprotective role against OSCC [14]. The protective role of vegetables and fruits on OSCC has been attributed to several micronutrients, including carotenoids, vitamin C and E with their antioxidant effects, binding and dilution of carcinogens in the digestive tract. Polycyclic Aromatic Hydrocarbons (PAH) present in the environment are carcinogens and they are present in high concentrations in meat products [32]. The complex and diverse nature of the Indian diet makes it difficult to assess the role of dietary components in cancer development. There are no well-designed epidemiological studies from Asian countries regarding this aspect and further research in this field is warranted to explore the dietary influences in young women with OSCC.
Family history of malignancies could be a risk factor. Though there is no substantial evidence from well-designed studies, the plausibility cannot be ignored and needs to be explored. A case series of young adults with tongue SCC from India with no risk factors had a positive family history of malignancy is present in 2.4 to 14% [33]. A study by Mork et al. reported a significantly increased risk for developing OSCC in female patients, aged less than 45 years, who had first degree relatives with cancer [34]. Though there is no substantial evidence from well-designed studies, the plausibility cannot be ignored and needs to be explored in this young women cohort.
A significant contributor to the young adult onset oral carcinogenesis is genomic aberrations and genetic predisposition. Enhanced function of oncogenes or impaired function of Tumour- Suppressor Genes (TSGs) or their products, or increased telomerase activity is involved in carcinogenesis [35]. Genomic aberrations apart from alcohol, nicotine, or virus induced carcinogenesis might be responsible for this. The activation of oncogenes (EGFR, CCDN1, MYC, PIK3CA, RAS) and an abrogated pathway in tumor suppressors (TP53, TP73, RB, CDKN2A, CDKN1A) could be widely demonstrated in young onset HNSCC [36]. A study by Sebastian et al. on no habit associated anterior tongue OSCC in young adults found an overexpression of CCND1, a key cell cycle regulator and that may contribute to their aggressive clinical behavior [37]. Large scale studies in young women with OSCC with a detailed gene profiling may reveal the gender related risks and promote the development of novel therapeutic approaches.
OSCC in young women without any significant habits have been considered as a distinct clinical entity. Several differences in clinicopathological profile between young and older HNSCC patients have been observed. Various studies regarding the outcome and the disease specific survival in this subset have yielded conflicting results. Lacy et al. reported significantly superior survival of HNSCC patients below the age of 40 years old, [38] whereas Garavello et al. found significantly decreased survival of oral tongue cancer patients below the age of 40 compared to their older counterparts [39]. In general, it has been found that young patients lack significant co morbidity because of the absence of potential risk factors and the tolerance to treatment is better and in turn good prognosis.
Conclusion
The etiology behind the increasing incidence of OSCC in young women with no potential risk factors is still unclear and is an enigma. The reported cases of OSCC in young women patients are increasing worldwide and also in developing countries like India and it is indeed an alarming situation. There is paucity of the published literature examining all the intrinsic risk factors in this subset of patients. Conclusive evidence is also limited by the lesser number in this group which impedes with statistical significance also. This emphasizes the need for collaborative multicenter studies to address the possible risk factors in this group. Further research using genetic and molecular biomarkers may help understand the clinicopathological profile of OSCC in the young women and predicting the gender related risks. This in turn would be helpful for treatment planning, monitoring as well as early detection and prevention in this subset of patients.
References
- Parkin DM, Pisani P, Ferlay J. Estimates of the worldwide incidence of eighteen major cancers in 1985. Int J Cancer. 1993; 54: 594-606.
- Sharma M, Madan M, Manjari M, Singh T, Jain S. Prevalence of Head and Neck Squamous cell carcinoma in our population: The clinic pathological and morphological description of 198 cases. International Journal of Advanced Research. 2015; 3: 827-833.
- Llewellyn CD, Johnson NW, Warnakulasuriya KA. Risk factors for squamous cell carcinoma of the oral cavity in young people--a comprehensive literature review. Oral Oncol. 2001; 37: 401-418.
- Llewellyn CD, Linklater K, Bell J, Johnson NW, Warnakulasuriya S. An analysis of risk factors for oral cancer in young people: a case-control study. Oral Oncol. 2004; 40: 304-313.
- Kuriakose M, Sankaranarayanan M, Nair MK, Cherian T, Sugar AW, Scully C, et al. Comparison of oral squamous cell carcinoma in younger and older patients in India. Eur J Cancer B Oral Oncol. 1992; 28: 113-120.
- Mathew Iype E, Pandey M, Mathew A, Thomas G, Sebastian P, Krishnan Nair M. Squamous Cell Carcinoma of the Tongue Among Young Indian Adults. Neoplasia. 2001; 3: 273 - 277.
- Krishnamurthy A, Ramshankar V. Early Stage Oral Tongue Cancer among Non-Tobacco Users - An Increasing Trend Observed in a South Indian Patient Population Presenting at a Single Centre. Asian Pac J Cancer Prev. 2013; 14: 5061-5065.
- van Heerden WE, van Rensburg EJ, Engelbrecht S, Raubenheimer EJ. Prevalence of EBV in oral squamous cell carcinomas in young patients. Anticancer Res. 1995; 15: 2335-2339.
- D'Costa J, Saranath D, Dedhia P, Sanghvi V, Mehta AR. Detection of HPV-16 genome in human oral cancers and potentially malignant lesions from India. Oral Oncol. 1998; 34: 413-420.
- Gillison ML, Lowy DR. A causal role for human papillomavirus in head and neck cancer. Lancet. 2004; 363: 1488-1489.
- Thomas DW, Seddon SV, Shepherd JP. Systemic immunosuppression and oral malignancy: a report of a case and review of the literature. Br J Oral Maxillofac Surg. 1993; 31: 391-393.
- Trizna Z, Schantz SP. Hereditary and environmental factors associated with risk and progression of head and neck cancer. Otolaryngol Clin North Am. 1992; 25: 1089-1103.
- Sturgis EM, Wei Q. Genetic susceptibility--molecular epidemiology of head and neck cancer. Curr Opin Oncol. 2002; 14: 310-317.
- Bravi F, Bosetti C, Filomeno M, Levi F, Garavello W, Galimberti S, et al. Foods, nutrients and the risk of oral and pharyngeal cancer. Br J Cancer. 2013; 109: 2904-2910.
- Langevin SM, Grandis JR, Taioli E. Female hormonal and reproductive factors and head and neck squamous cell carcinoma risk. Cancer Lett. 2011; 310: 216-221.
- Oliver RJ, Dearing J, Hindle I. Oral cancer in young adults: report of three cases and review of the literature. Br Dent J. 2000; 188: 362-365.
- Müller S, Pan Y, Li R, Chi AC. Changing trends in oral squamous cell carcinoma with particular reference to young patients: 1971-2006. The Emory University experience. Head Neck Pathol. 2008; 2: 60-66.
- Hirota SK, Migliari DA, Sugaya NN: Oral squamous cell carcinoma in a young patient-case report and literature review. An Bras Dermatol. 2006; 81: 251-254.
- Sankaranarayanan R, Mohideen MN, Nair MK, Padmanabhan TK. Aetiology of oral cancer in patients less than or equal to 30 years of age. Br J Cancer. 1989; 59: 439-440.
- Mathew Iype E, Pandey M, Mathew A, Thomas G, Sebastian P, Krishnan Nair M. Squamous cell carcinoma of the tongue among young Indian adults. Neoplasia. 2001; 3: 273-277.
- Girod A, Mosseri V, Jouffroy T, Point D, Rodriguez J. Women and squamous cell carcinomas of the oral cavity and oropharynx: is there something new? J Oral Maxillofac Surg. 2009; 67: 1914-1920.
- Patel SC, Carpenter WR, Tyree S, Couch ME, Weissler M, Hackman T, et al. Increasing Incidence of Oral Tongue Squamous CellCarcinoma in Young White Women, Age 18 to 44 Years. Journal of clinical oncology. 2011; 29: 1488-1495.
- Bleyer A. Cancer of the oral cavity and pharynx in young females: increasing incidence, role of human papilloma virus, and lack of survival improvement. Semin Oncol. 2009; 36: 451-459.
- Liang XH, Lewis J, Foote R, Smith D, Kademani D. Prevalence and significance of human papillomavirus in oral tongue cancer: the Mayo Clinic experience. J Oral Maxillofac Surg. 2008; 66: 1875-1880.
- Poling JS, Ma XJ, Bui S, Luo Y, Li R, Koch WM, et al. Human papillomavirus (HPV) status of non-tobacco related squamous cell carcinomas of the lateral tongue. Oral Oncol. 2014; 50: 306-310.
- Serefoglou Z, Yapijakis C, Nkenke E, Vairaktaris E. Genetic association of cytokine DNA polymorphisms with head and neck cancer. Oral Oncol. 2008; 44: 1093-1099.
- Colella G, Izzo G, Carinci F, Campisi G, Lo Muzio L, D'Amato S, et al. Expression of sexual hormones receptors in oral squamous cell carcinoma. Int J Immunopathol Pharmacol. 2011; 24: 129-132.
- Schuller DE, Abou-Issa H, Parrish R. Estrogen and progesterone receptors in head and neck cancer. Arch Otolaryngol. 1984; 110: 725-727.
- Bauernhofer T, Pichler M, Wieckowski E, Stanson J, Aigelsreiter A, Griesbacher A, et al. Prolactin receptor is a negative prognostic factor in patients with squamous cell carcinoma of the head and neck. Br J Cancer. 2011; 104: 1641-1648.
- Bhatavdekar J, Patel D, Vora H, Balar D. Circulating hormones in patients with tongue cancer. Oncol Rep. 1994; 1: 461-463.
- Applebaum KM, Nelson HH, Zens MS, Stukel TA, Spencer SK, Karagas MR. Oral contraceptives: a risk factor for squamous cell carcinoma? J Invest Dermatol. 2009; 129: 2760-2765.
- Xia Z, Duan X, Qiu W, Liu D, Wang B, Tao S, et al. Health risk assessment on dietary exposure to polycyclic aromatic hydrocarbons (PAHs) in Taiyuan, China. Sci Total Environ. 2010; 408: 5331-5337.
- Ankathil R, Mathew A, Joseph F, Nair MK. Is oral cancer susceptibility inherited? Report of five oral cancer families. Eur J Cancer B Oral Oncol. 1996; 32: 63-67.
- Mork J, Møller B, Glattre E. Familial risk in head and neck squamous cell carcinoma diagnosed before the age of 45: a population-based study. Oral Oncol. 1999; 35: 360-367.
- ScullyC, J.K. Field, H. Tanzawa. Genetic aberrations in oral or head and neck squamous cell carcinoma 2: chromosomal aberrations. 2000; 36: 311-327.
- Knopf A, Lempart J, Bas M, Slotta-Huspenina J, Mansour N, Fritsche MK. Oncogenes and tumor suppressor genes in squamous cell carcinoma of the tongue in young patients Oncotarget. 2015; 5: 3443-3451.
- Sebastian P, Babu JM, Prathibha R, Hariharan R, Pillai MR. Anterior tongue cancer with no history of tobacco and alcohol use may be a distinct molecular and clinical entity. J Oral Pathol Med. 2014; 43: 593-599.
- Lacy PD, Piccirillo JF, Merritt MG, Zequeira MR. Head and neck squamous cell carcinoma: better to be young. Otolaryngol Head Neck Surg. 2000; 122: 253-258.
- Garavello W, Spreafico R, Gaini RM. Oral tongue cancer in young patients: A matched analysis. Oral Oncol. 2007; 43: 894-897.