
Research Article
J Dent & Oral Disord.2016; 2(3): 1018.
Pro-Inflammatory Cytokine Concentration in Gingival Fluid in Obese Patients with Periodontal Disease
Olavegogeascoechea P¹*, Brusca MI², Noier M¹, Carballo B¹, Casal M¹ and Palazzi J³
¹Faculty of Medicine and Health Sciences - Odontology - Open University Interamericana- Buenos Aires-Buenos Aires -Argentina
²Faculty of Medicine and Health Sciences - Odontology - Universidad Abierta Interamericana and Faculty of Dentistry, University of Buenos Aires - Buenos Aires - Buenos Aires -Argentina.
³International Integrated Clinical Trial Labs - Rosario – Argentina
*Corresponding author: Paul Olavegogeascoechea, Faculty of Medicine and Health Sciences, Universidad Abierta Interamericana. Av San Juan 951 -. Buenos Aires - Buenos Aires - Argentina
Received: May 06, 2016; Accepted: May 25, 2016; Published: May 26, 2016
Abstract
Introduction: The presence of high levels of inflammatory mediators both in periodontal disease and in obese people is well documented in the literature. However, there is weak evidence of the relation between both pathologies and cytokines concentration both in serum as in gingival fluid (i.e. Interleukin 6 and Gamma Interferon). The objective of our exploratory study is to measure the concentration of pro-inflammatory cytokines such as Interleukin 6 and Gamma Interferon in the gingival fluid of the obese patients with different clinical periodontal status.
Methods: Twenty one adult patients with a body mass index >30Kg/m2 were included. A medical and dental history of the participating patients was carried out. The periodontal index was measured and a gingival fluid sample was taken in order to measure the Interleukin 6 and Gamma Interferon concentrations.
Results: Nineteen patients (90%) had periodontal disease. Among them, the disease was mild in 43%, moderate in 14% and severe in 33% of the patients. The average cytokine concentration in gingival fluid for Interleukin 6 was 2,06+/ - 0,96 pg/ml and for Gamma Interferon 2,73 +/- 1,13 pg/ml. Interleukin 6 concentration in patients with concomitant diseases was 2,66 +/- 0,91 pg/ml and in those without concomitant diseases was 1,63 +/- 0,77 pg/ml (p=0.01); the Gamma Interferon concentration was 3,48 +/- 1,13 pg/ml and in the patients without concomitant diseases 2,19 +/- 0,79 pg/ml (p=0.009).
Conclusion: Even though the strong association between obesity and periodontal disease has been proved, the estimation of the persistence of the inflammatory response through the high levels of pro-inflammatory cytokines seems to be more related to the concomitant diseases with inflammatory origin disorders than with the association itself.
Keywords: Periodontal disease; Obesity; IL6; Gamma interferon; Gingival fluid
Abbreviations
IL6: Interleukin 6; INF-γ: Gamma Interferon; BMI: Body Mass Index; CD: Celiac Disease; WHO: World Health Organization
Introduction
The prevalence of obesity is increasing around the world. This trend has prompted the WHO to describe the increase as a global epidemic; therefore it would be considered a major problem in public health [1]. It is strongly associated with a higher risk for diseases such as diabetes, hypertension, some types of cancer, vascular disease [2] and periodontitis [3,4]. Periodontitis is a chronic inflammatory affection, related not only to risk factors for vascular disease but also related to cardiovascular and neurovascular events (i.e. acute myocardial infarction and ischemic stroke) [5]. Its pathogeny is complex [6] and would bear a part in similar paths to arteriosclerosis [7]. The mechanisms whereby the obese patients develop periodontitis most commonly are not well known, however, it is known that the adipose tissue is a major producer and reservoir of pro-inflammatory mediators [8].
The relation between both diseases [9], could be mediated by the constant production of pro-inflammatory cytokines [10-12].
The presence of high levels of inflammatory mediators both in patients with periodontal disease and in obese patients is well documented (i.e. pro-inflammatory cytokines). However, there is weak evidence of the relation between both pathologies and cytokines concentration both in serum as in gingival fluid (i.e. Interleukin 6 and Gamma Interferon). These two cytokines were strongly associated with severe or destructive periodontal disease [13-15]. The objective of our exploratory study is to measure the concentration of proinflammatory cytokines such as Interleukin 6 (IL6) and Gamma Interferon (INF-γ) in the gingival fluid of the obese patients with different clinical periodontal status.
Material and Methods
Twenty one obese adults, both male and female and with a BMI>30Kg/m² were recruited for this exploratory cross-sectional study. The study protocol was approved by Ethics Committee - Universidad Abierta Interamericana. Exclusion criteria: 1- Patients who received antibiotics or anti-fungal medication 30 days prior to the study; 2- Patients with orthodontia, either permanent or removable.
A medical and odontological history was taken from the patients. Clinical measurements were taken at 6 sites per tooth (mesiobuccal, buccal, distobuccal, distolingual, lingual and mesiolingual). The periodontal indexes (probing depth, periodontal attachment loss, Loe’s index) were measured. “Healthy” were considered the patients with no hemorrhage while probing, probing depth < 2 mm, attachment loss < 2 mm, absence of mobility, plaque index 0 or 1, gingival index 0 to 1. Those who did not apply as health periodontal status were considered having periodontal disease that will be divided in three groups: mild, moderate, severe. Patients were indicated to use a mouthwash (sterile physiological solution 0.98%) before taking the sample. A gingival fluid sample was obtained with paper cones during 10 seconds and it was placed in Eppendorf tubes with 0.5 ml of physiological solution. The samples were analyzed measuring the concentration of IL6 and Gamma INF in gingival fluid (with ELISA Human IFN-Gamma y Human IL-6, Quantikine; RD Systems Kits)
Statistics: Values for the cytokines were presented as averaged and SD. The differences in the distribution of males and periodontal status were examined using the Chi-square test and the levels of cytokines were examined using ANOVA test. The ROC curve was used to determine the Cut-off value of interleukins concentration.
Results
Baseline characteristics of the patients: 48% were men, the mean age was 46 years and the BMI 34, 84 +/-2, 93. Almost all (90%) had periodontal disease which was, mild in 9 (43%), moderate in 3 (14%) and severe in 7 (33%). Two patients showed healthy periodontal status. Eight patients (38%) had concomitant diseases: Celiac Disease (CD) 4, Diabetes 1 and Hypothyroidism 3.
The severity of the periodontal disease in the patients with hypothyroidism was: mild in 1 patient, moderate in 1 and severe in 1; in the patients with CD most were severe (moderate in 1 patient and severe in 3 patients) and in the diabetic patient was severe. The average cytokines concentration in gingival fluid were similar for IL6 in the two groups, with and without periodontal disease (2,06 +/- 0,96 vs. 1,08 +/- 0,39 pg/ml respectively; p=0.10) while INF γ concentration there were statistically significant differences (2,73 +/- 1,13 vs 1,38 +/- 0,11 pg/ml; p<0.01 respectively).
The concentration of IL6 and INF-γ between sex were similar (men: 2,11 +/-1,09 pg/ml vs women: 2,02 +/- 0,88 pg/ml; p=0,83 and men 2,89 +/- 1,42 pg/ml vs women 2,59 +/- 0,84 pg/ml; p=0,57, respectively). The IL6 concentration in patients with concomitant diseases was 2,66 +/- 0,91 pg/ml and in those without was 1,63 +/- 0,77 pg/ml (p=0.01) while INF-γ concentration was 3,48 +/-1,13 pg/ ml in the former group and it was 2,19 +/- 0,79 pg/ml in the later group (p=0,009) (Table 1 and Table 2).
Data
IL6 (pg/ml)
INF-γ (pg/ml)
n
8
8
Mean (pg/ml)
2,66
3,48
SD
0,91
1,13
Mínimum
1,50
2,40
Máximum
4,16
5,76
Range
2,66
3,36
Table 1: Cytokine concentration in patients with concomitant diseases.
Data
IL6 (pg/ml)
INF-γ (pg/ml)
n
11
11
Mean (pg/ml)
1,632
21,918
SD
0,77
0,79
Mínimum
,8
1,30
Máximum
3,4
3,60
Range
2,6
2,30
Table 2: Cytokine concentration in patients without concomitant diseases.
In patients with concomitant diseases the INF-γ was statistically significant higher than those without (3,48 +/-1,13 vs 2,19 +/- 0,79 pg/ml; p=0.009) and IL6 results also showed statistically significant differences between groups (2, 66 +/- 0,91vs 1,63 +/- 0,77; p=0.01). In hypothyroid patients IL6 concentration was significantly higher than those without (3,23 +/-0, 93 vs 1, 63 +/- 0,77 pg/ml; p=0.009) and similar differences were seen in INF-γ concentration (3,55 +/- 1,51 vs 2,58 +/- 0,94 pg/ml, respectively; p=0.04). On the other hand the IL6 concentration were similar in those patients with CD and those without (2,40 +/- 0,90 vs 1,63 +/-0,77 pg/ml; p=0.12), while INF-γ concentration were different between groups mentioned (3,47 +/- 0,73 vs 2,19 +/-0,79 pg/ml; p=0.01) (Table 3)
Cytokine*
Gender
Concomitant diseases
CD
Hypothyroidism
Men
Female
p
Yes
No
p
Yes
No
p
Yes
No
p
IL6
2,11 +/- 1,09
2,02 +/- 0,88
0.83
2,66 +/- 0,91
1,63 +/- 0,77
0.01
2,40 +/- 0,90
1,63 +/- 0,77
0.12
3,23 +/- 0,93
1,63 +/- 0,77
0.009
INF-γ
2,89 +/- 1,42
2,59 +/- 0,84
0.57
3,48 +/- 1,13
2,19 +/- 0,79
0.009
3,47 +/- 0,73
2,19 +/- 0,79
0.01
3,55 +/- 1,51
2,58 +/- 0,94
0.04
*Cytokine Concentration in pg/ml; IL6: Interleukin 6; INF-γ: Gamma Interferon; CD: Celiac Disease.
Table 3: Cytokine concentration according to gender and concomitant disease.
In obese patients with periodontal disease we found that the patients with concomitant diseases (Hypothyroidism, Diabetes, Celiac Disease) had a higher prevalence of severe disease than those without (20,8% vs 8,3% respectively; p<0.01). On the other hand, in patients with severe periodontal disease compared to the those with mild or moderate status, we found not only a higher concentration of INF-γ (3,93 +/- 0,32 vs 2,03 +/- 0,13, respectively; p<0.01) but also higher concentrations of IL6 in gingival fluid (2,64 +/- 0, 33 vs 1,72 +/- 0, 24, respectively; p=0.04).
In a Ad-hoc analysis and looking for a predictive cytokine concentration value of concomitant disease in this kind of patients we found: the best value found as cut-off point confirmed with the ROC curve (Area under the curve: 0,84) above which, the levels of IL6 (Elisa Human IL-6, Quantikine; RD Systems) in gingival fluid could be predictive of concomitant disease was: 1,66 pg/ml (Figure 1), giving a diagnostic value of: sensibility 87,5% (CI 95%: 64,6-110,4%), specificity 63,6% (CI 95%: 35,2-92,1%), PPV 64% (CI 95%: 35,2- 92,1%), NPV 88% (CI 95%: 64,6-110,4%) and Likelihood Ratio: 2,41 (CI 95%: 1,43-4,04).
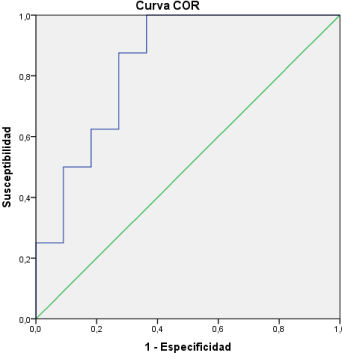
Figure 1: ROC Curve for IL6 concentrations.
The cut-off point confirmed with ROC curve (Area under the curve: 0,84), above which the INF-γ (Elisa Human IFN-Gamma, Quantikine; RD Systems) levels in gingival fluid could be predictive of concomitant disease was: 2,33 pg/ml (Figure 2), giving a diagnostic value of: sensibility 100%, specificity 63,6% (IC95%: 35,2-92,1%), PPV 67% (IC95%: 40-93%), NPV 100% y Likelihood Ratio: 2,75 (CI95%: 1,76-4,34).
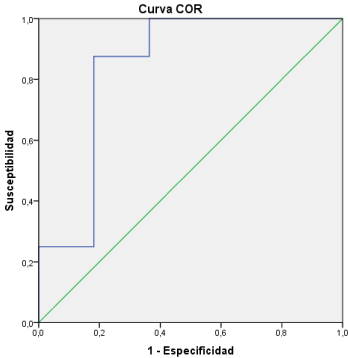
Figure 2: ROC Curve for INF-γ concentrations.
Discussion
The prevalence of periodontal disease in this obese patient population was 90% and the severe status less than 50%, this finding was different from the publication by Khan et al. (2015) [16], where the prevalence was 74% and the severe form reached more than half of the participants. Probably because in our study we used a higher BMI than in the above mentioned study (30 Kg/m2 vs 27, 5 Kg/m2). Our study sustains the strong association between obesity and periodontal disease, being obesity a potential risk factor for periodontal inflammation [17].
In our exploratory study the levels of cytokines concentration in salivary fluid (i.e. IL6 and INF-γ) showed differences depending on the severity of the periodontal disease, being higher not only in those patients with severe periodontal disease but also in those with concomitant disease (hypothyroidism, diabetes or celiac disease), this probably shows the higher impact in the production of these proinflammatory mediators in autoimmune diseases [18,19].
In this study the INF-γ levels were higher in the mentioned diseases, while the IL6 showed significative differences only in the patients with hypothyroidism. The hypothyroidism showed a significant difference in both cytokines concentration in the gingival fluid, unrelated to the severity of the periodontal disease, showing a possible association beyond that and perhaps obesity [20]. Another important finding in our study was the potential usefulness of IL6 and INF-γ concentrations in gingival fluid as predictors of concomitant disease in these kind of patients. Both pro-inflammatory cytokines showed a high negative predictive value, making it unlikely the existence of concomitant diseases with levels below the cutoffs found (IL6: 1.66 pg/ml and INF-γ: 2.33 pg/ml). The limitation in our study is the sample size, especially in those patients with concomitant diseases, therefore it would be needed more studies to aim more information in this regarding.
Conclusion
Even though the strong association between obesity and periodontal disease has been proved, the estimation of the persistence of the inflammatory response through the high levels of proinflammatory cytokines seems to be more related to the concomitant diseases with inflammatory origin disorders than with the association itself.
Acknowledgment
We are very grateful to Marcela Kalina, M.D. who is A Medical Translator and Medical Interpreter in Boston, MA and was the translator of this manuscript.
Compliance with Ethical Standards
Funding
The work was supported by the Cátedra de Microbiología, Carrera de Odontología de la Facultad de Ciencias Médicas – Universidad Abierta Interamericana, Buenos Aires - Argentina and the International Integral Clinical Trial Labs (IICT), Rosario - Argentina.
Ethical approval
All procedures performed in this study, involving human participants were in accordance with the ethical standards of the Institutional (Comité de Ética of the Universidad Abierta Interamericana) and National Research Committee (ANMAT, Resolución 1480/11) and with the 1964 Helsinki declaration and its later amendments.
Informed consent
Informed consent was obtained from all individual participants included in the study.
References
- Kopelman PG. Obesity as a medical problem. Nature. 2000; 404: 635-643.
- Hubert HB, Feinleib M, McNamara PM, Castelli WP. Obesity as an independent risk factor for cardiovascular disease: A 26-year follow-up of participants in the Framingham heart study. Circulation. 1983; 67: 968-977.
- Saito T, Shimazaki Y, Koga T, Tsuzuki M, Ohshima A. Relationship between upper body obesity and periodontitis. J Dent Res. 2001; 80: 1631-1636.
- Alabdulkarim M, Bissada N, Al-Zahrani M, Ficara A, Siegel B. Alveolar bone loss in obese subjects. J Int Acad Periodontol. 2005; 7: 34-38.
- Pires JR, Dos Santos IP, de Camargo LF, Zuza EP, de Toledo BE, Monteiro SC. Framingham cardiovascular risk in patients with obesity and periodontitis. Journal of Indian Society of Periodontology. 2014; 18: 14-18.
- Kurita-Ochiai T, Jia R, Cai Y, Yamaguchi Y, Yamamoto M. Periodontal Disease-Induced Atherosclerosis and Oxidative Stress. Antioxidants (Basel). 2015; 4: 577-590.
- Scannapieco FA, Bush RB, Paju S. Associations between periodontal disease and risk for atherosclerosis, cardiovascular disease, and stroke. A systematic review. Ann Periodontol. 2003; 8: 38-53.
- Wellen KE, Hotamisligil GS. Inflammation, stress, and diabetes. J Clin Invest. 2005; 115: 1111-1119.
- Suvan J, D'Aiuto F, Moles DR, Petrie A, Donos N. Association between overweight/obesity and periodontitis in adults. A systematic review. Obes Rev. 2011; 12: 381-404.
- Esposito K, Giugliano G, Scuderi N, Giugliano D. Role of adipokines in the obesity-inflammation relationship: the effect of fat removal. Plast Reconstr Surg. 2006; 118: 1048-1057.
- Imatani T, Kato T y Okuda K. Production of inflammatory cytokines by human gingival fibroblasts stimulated by cell-surface preparations of Porphyromonas gingivalis. Oral Microbial. Immunol. 2001; 16: 65-72.
- Morandini AC, Sipert CR, Ramos-Junior ES, Brozoski DT, Santos CF. Periodontal ligament and gingival fibroblasts participate in the production of TGF-β, interleukin (IL)-8 and IL-10. Braz Oral Res. 2011; 25: 157-162.
- Khosravi R, Ka K, Huang T, Khalili S, Hong Nguyen B, Nicolau B, et al. Tumor Necrosis Factor-α and Interleukin-6: Potential Interorgan Inflammatory Mediators Contributing to Destructive Periodontal Disease in Obesity or Metabolic Syndrome. Mediators of Inflammation, 2013: ID: 728987.
- Isaza-Guzmán DM, Cardona-Vélez N, Gaviria-Correa DE, Martínez-Pabón MC, Castaño-Granada MC, Tobón-Arroyave SI. Association study between salivary levels of interferon (IFN)-gamma, interleukin (IL)-17, IL-21, and IL-22 with chronic periodontitis. Arch Oral Biol. 2015; 60: 91-99.
- Cortela DC, de Souza Junior AL, Virmond MC, Ignotti E. Inflammatory Mediators of Leprosy Reactional Episodes and Dental Infections: A Systematic Review. Mediators Inflamm. 2015: 548540.
- Khan S, Saub R, Vaithilingam RD, Safii SH, Vethakkan SR, Baharuddin NA. Prevalence of chronic periodontitis in an obese population: a preliminary study. BMC Oral Health. 2015; 15: 114.
- Słotwińska SM, Słotwiński R. Host response, obesity, and oral health. Cent Eur J Immunol. 2015; 40: 201-205.
- Pascual V, Medrano LM, López-Palacios N, Bodas A, Dema B, Fernández-Arquero M, et al. Different Gene Expression Signatures in Children and Adults with Celiac Disease. PLoS One. 2016; 11: e0146276.
- Marchiori RC, Pereira LA, Naujorks AA, Rovaris DL, Meinerz DF, Duarte MM, et al. Improvement of blood inflammatory marker levels in patients with hypothyroidism under levothyroxine treatment. BMC Endocr Disord. 2015; 15: 32.
- Scardina GA, Messina P. Modifications of interdental papilla microcirculation: a possible cause of periodontal disease in Hashimoto's thyroiditis? Ann Anat. 2008; 190: 258-263.