
Research Article
J Dent & Oral Disord. 2016; 2(7): 1036.
Three-Dimensional Quantitative Evaluation of the Effect of Local Administration of Dexamethasone on Facial Swelling after Impacted Mandibular Third Molar Extraction
Matsuda M¹*, Kondo S¹, Seto M¹, Kita R¹, Mori H², Moriyama S² and Kikuta T¹
¹Department of Oral and Maxillofacial Surgery, Faculty of Medicine, Fukuoka University, Japan
²Department of Mechanical Engineering, Faculty of Engineering, Fukuoka University, Japan
*Corresponding author: Matsuda M, Department of Oral and Maxillofacial Surgery, Faculty of Medicine, Fukuoka University, Japan
Received: September 07, 2016; Accepted: September 23, 2016; Published: September 26, 2016
Abstract
The most common dental surgery, the removal of impacted mandibular third molars, is associated with complications including postoperative facial swelling, pain and limited mouth opening. The beneficial effects of local administration of adrenal steroids (dexamethasone) to the cheek muscle after impacted mandibular third molar extraction are evaluated using a non-contact three- Dimensional (3D) scanner and conventional anthropometric measurements. In this prospective randomized controlled study, results revealed that administration of dexamethasone significantly suppressed postoperative swelling as compared with physiological saline on postoperative day 1 (dexamethasone group [n = 41], 3.29 cm3; physiological saline group [n = 40], 8.46 cm3, p<0.05) and on postoperative day 3 (dexamethasone group, 6.56 cm3; physiological saline group, 10.34 cm3, p<0.001). Patients in the dexamethasone group were able to open their mouths considerably wider than the physiological saline group for all comparisons (day 1: dexamethasone group, 38.0 mm; physiological saline group, 30.2 mm p<0.05, day 3: dexamethasone group, 40.4 mm; physiological saline group, 32.9 mm p<0.001, day 7: dexamethasone group, 43.6 mm; physiological saline group, 38.8 mm p<0.05). Postoperative pain was only suppressed significantly more in the dexamethasone group than in the physiological saline group on postoperative day 1 (p<0.05). In conclusion, local administration of dexamethasone significantly reduces the postoperative complications and 3D measurement is a simple and precise method for evaluating volumetric changes after the removal of impacted mandibular third molars.
Keywords: Impacted mandibular third molar extraction; Dexamethasone, Postoperative facial swelling; Three-dimensional measurement
Introduction
Impacted mandibular third molar extraction is a common surgery in the field of oral surgery and is accompanied by a high incidence of postoperative complications including facial swelling, pain and limited mouth opening (trismus) [1]. Reports on devising pharmacotherapies and improving surgical procedures have been published in pursuit of mitigating these complications [2,3]. The number of studies of evaluation methods and measures to prevent postoperative facial swelling is particularly large [3-16].
The most commonly reported method for evaluating postoperative facial swelling is measuring the distance between two points on the face [3, 4, 6-15]. However, this method has a major drawback in term of objective and quantitative evaluations in that points on the face are displaced as a result of swelling of the reference points themselves and deformation of the facial skin due to contact with and pressure on the swollen area by the measuring instrument. Other reported methods include the face-bow method [4], the ultrasound method [5], and the laser scanner method [16]. These methods, however, have complicated approaches. The method using computed tomography [5] has the problem of radiation exposure, making it difficult to perform multiple scans and achieve objective, day-to-day quantification of swelling. We therefore decided to measure facial morphology using a simple, non-contact 3-Dimensional (3D) scanner.
Administration of adrenal steroids has been reported as a means of preventing swelling since the 1960s [17]. Due to the excellent anti-inflammatory action of adrenal steroids, these drugs have been used on a daily basis to reduce postoperative swelling in many cases. Numerous reports have stated that administration of corticosteroids suppresses facial swelling after extraction of impacted mandibular third molars [4-14]. Furthermore, systemic intravenous administration of corticosteroids for the purpose of preventing laryngeal swelling during tracheal extubation in the field of anesthesiology [18] has also been used to reduce recurrent nerve paralysis and prevent speech disturbance resulting from swelling of the vocal cords after thyroidectomy in the field of otolaryngology [19,20]. These reports show how corticosteroids are used in multiple fields to prevent perioperative swelling.
In the present study, we locally injected dexamethasone, a J Dent & Oral Disord 2(7): id1036 (2016) - Page - 02 Matsuda M Austin Publishing Group Submit your Manuscript | www.austinpublishinggroup.com corticosteroid, into the nearby cheek muscle after extraction of impacted mandibular third molars, and quantitatively evaluated changes in facial volume (cm3) using a 3D scanner. We also evaluated postoperative mouth opening and pain by quantifying these parameters.
Subjects and Methods
Patient characteristics and group allocation method
Subjects comprised patients ≥18 years old and <45 years old requiring mucosal resection and bone milling in extraction of impacted mandibular third molars. Subjects were rated Class I or II and Position A or B according to winter’s classification of the difficulty of surgery for impacted mandibular third molars, and the target sample size was set at 100. Of these 100 samples distribution of the classification was as: 78 horizontal, 22 mezioangular. Subjects were randomly allocated by lottery to a group that received a subcutaneous injection of 4 mg of dexamethasone (1 mL) to the cheek muscle at the base of the gingival mucosal incision immediately after tooth extraction (Dexamethasone [DEX] group; n = 50) and the other group that received subcutaneous injection of 1 mL of physiological saline to the same site immediately after tooth extraction (physiological Saline [SAL] group; n = 50). Patients who were pregnant, prohibited from using corticosteroids, suffering from a serious systemic disease (American Society of Anesthesiologists Physical Status III or IV), had a history of allergic reactions to drugs, or suffering from diabetes were excluded in advance. The two groups did not differ significantly in terms of sex, age, surgical duration, height, weight, or body mass index (Table 1). This study was conducted with the approval of the institutional review board of Fukuoka University Hospital (approval no.: 13-9-04) and all subjects provided informed consent to participate after receiving explanations of the purpose of this study and the tooth extraction procedure. After excluding patients with inadequate 3D scanner data for measurements of facial swelling and patients who failed to turn up on the day of scanning, the final number of patients was 40 in the DEX group and 41 in the SAL group.
Sex
Men: 24, Women: 26
Men: 23, Women: 27
0.82
Height (cm)
163.9±8.7
162.6±8.7
0.49
Weight (kg)
57.9±10.1
55.6±9.8
0.2
BMI (kg/m2)
21.5±2.9
21.5±2.9
0.35
Surgical duration(min)
21.7±8.1
21.0±6.5
0.66
Age(year)
23.1±5.4
23.4±5.9
0.76
Table 1: Patient Characteristics.
Extraction procedure for impacted mandibular third molars
In performing surgery, the skin around the oral cavity was disinfected with a cotton swab moistened with chlorhexidine and ethanol and the oral cavity was cleaned and disinfected with a cotton ball moistened with 10% povidone-iodine solution. Ethyl aminobenzoate was applied as a topical anesthetic to the site of local anesthesia injection for 30 second, after which conduction anesthesia was initiated at the mandibular foramen with 2% xylocaine with epinephrine 1:80,000 and infiltration anesthesia was initiated at the gingiva surrounding the mandibular 7th and 8th teeth. A longitudinal incision was then made at the mesial corner near the mandibular 7th tooth using a No. 15 scalpel blade and the gingival mucosa was cut from the centrifugal part of the mandibular 7th tooth to the anterior border of the mandibular ramus. The gingival periosteum was detached using an elevatorium and the crown was sufficiently exposed by milling the bone surrounding the outside of the crown of the mandibular 8th tooth using a 2.7 mm tungsten carbide round bur. A 1.6-mm tungsten carbide straight fissure bur was then used to remove the bone to check the neck of the mandibular 8th tooth and a 2.1 mm tungsten carbide straight fissure bur was used to split the crown and root where necessary (Figure 1). An elevator was used to dislocate the tooth, which was then removed with forceps. The tooth sac was also removed at this point. After tooth extraction, the wound site was cleaned with 10% povidone-iodine solution and stereotactically sutured with 3-0 polyglycolic acid sutures. The wound was also left partially open at the centrifugal part on the buccal side of the mandibular 7th tooth. No local hemostatic agent was used. Five dentists in their third to eight years after graduation performed the tooth extraction surgeries.
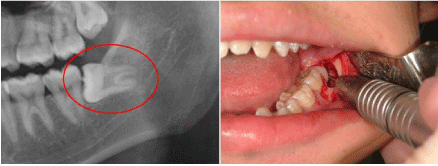
Figure 1: A) Left Mandibular 8th tooth, Winter’s classification class 1, position
A. B) Wassumund incision, bone milling and crown-root split.
Postoperative medication
Postoperative medication was given three times daily. Patients received a single administration of 1,000 mg of acetaminophen and 100 mg of cefcapene pivoxil, which have no anti-swelling effects, and 60 mg of loxoprofen sodium hydrate as a rescue drug for times of enhanced pain. No mouthwash was given.
Endpoints and measurement period
Endpoints were facial swelling, pain and mouth opening. All endpoints were measured immediately before surgery and 1, 3, and 7 days postoperatively.
Evaluation of 3D scanner accuracy
The scanner used was an Artec MHT® 3D scanner (Artec Group, Luxembourg). Hemispherical 3D models with a diameter of 52.0 mm created using a ProJet® 3D printer (3D Systems, Rock Hill, SC) were used to verify the measurement accuracy of this 3D scanner. The mean volume calculated from five Vernier caliper measurements of the contours of the hemisphere was set as the external volume of the model. The shape of the model was scanned three times with the 3D scanner and the obtained volumes were compared and verified for errors.
Volumetric calculations with the 3D scanner were made by inputting scanned data into a computer as point cloud data on a 3D coordinate axis. The 3D coordinates of the point cloud data had different reference points in each scan, which required superimposition of the point cloud data. This superimposition of preand postoperative point cloud data to measure volumetric change was done using the Iterative Closest Point (ICP) algorithm [21], which employs singular value decomposition to minimize the sum of distances to all points to find the rotation matrix.
Measurement of facial swelling
Actual facial swelling was measured using the Artec MHT® 3D scanner as follows. Scans were taken while the subject sat upright at a 90° angle on a chair in a dental X-ray suite at a distance of approximately 1 m from the scanner, which scanned 180° to the left and right (Figure 2.1). The subject’s head was positioned so that the lower edge of the mandible was parallel to the floor (Figure 2.2). Four dentists with experience of 3D scanning took the 3D scans. The amount of volumetric change each day compared with before surgery was calculated by superimposing point cloud data from before and after surgery using the ICP algorithm, which had been confirmed using a 3D model.
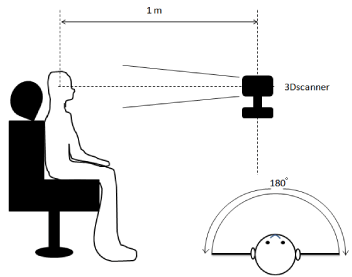
Figure 2: Distance between scanner and subject’s face during 3D scanning
and scanning range.
Evaluation of mouth opening and postoperative pain
Postoperative pain was evaluated each day using a Numerical Rating Scale (NRS) that allowed patients to rate the level of pain on a scale from 0 (no pain) to 10 (worst pain imaginable). Mouth opening was measured each day by a surgeon using Vernier calipers as the distance between the upper and lower central incisors.
Statistics
Statistical analysis was performed using the software program SPSS Statistics version 20 (IBM Corporation, Armonk, NY). Facial swelling, mouth opening and pain were assessed by the student`s t-test. Data were expressed as the mean ± standard deviation, and differences were considered significant at *P < 0.05 and **P < 0.001.
Results
Verification of 3D scanner accuracy
Measurement of the contours of the prepared hemisphere model by Vernier calipers produced a mean diameter of 52.3 mm. This was used to set a hemisphere radius of 26.2 mm. Mean height of the hemisphere was 26.0 mm, with an error of 0.8% with respect to the radius. The model was thus hemispherical. The volume of the contour of the model was consequently deemed to be 37.5 cm3. The mean of the 3D scanning data for the hemisphere was 38.6 cm3. When this was compared with the original volume, mean volume ratio was 103.3% (Figure 3).
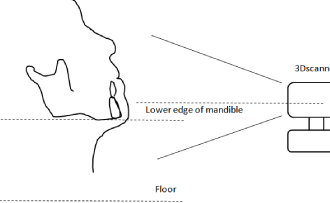
Figure 2b: Facial inclination during 3D scanning.
Postoperative volumetric changes in facial swelling
The increase in facial volume 1 day after surgery as compared with before surgery was 3.29 cm³ in the DEX group and 8.46 cm³ in the SAL group. Postoperative swelling was thus significantly suppressed in the DEX group as compared with the SAL group (P <0.001). Even 3 days after surgery, the increase in volume was 6.56 cm³ in the DEX group versus 10.34 cm³in the SAL group (P<0.05), indicating that the postoperative swelling was significantly suppressed in the DEX group. By 7 days after surgery, the volume increase was 1.79 cm³ in the DEX group and 3.91 cm³ in the SAL group, revealing a tendency for suppression of volumetric increase; however, the difference between groups was not significant (Figure 4).
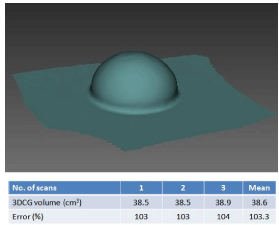
Figure 3: Verification of 3D scanner accuracy using a hemispere as the
sample.
Changes in mouth opening after surgery as compared with before
Preoperative mouth opening was 46.3 mm in the DEX group and 45.7 mm in the SAL group, indicating no significant difference between groups. These values in DEX and SAL groups were 38.0 mm and 30.2 mm on postoperative day 1, 40.4 mm and 32.9 mm on postoperative day 3, and 43.6 mm and 38.8 mm on postoperative day 7, respectively, revealing that the DEX group was significantly more able to open their mouths than the SAL group on all days (Figure 5).
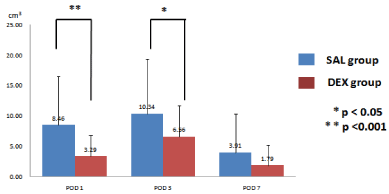
Figure 4: Amount of increase in facial volume after surgery.
Changes in postoperative pain
Postoperative pain was significantly more suppressed in the DEX group (NRS: 2.1) than in the SAL group (NRS: 3.0) on postoperative day 1. No significant differences were seen between groups on postoperative days 3 and 7 (Figure 6).
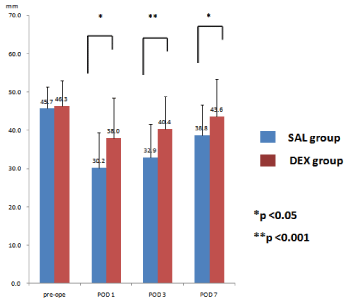
Figure 5: Change of mouth opening after surgery compared with before
surgery.
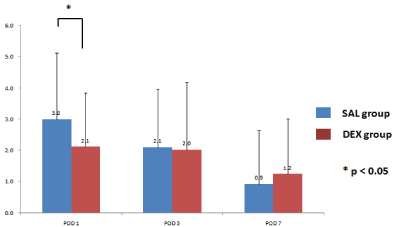
Figure 6: Change in postoperative pain (numerical rating scale).
Discussion
The most common method used to measure facial swelling after impacted mandibular third molar extraction is to measure the distance between two reference points. However, the results of measurement do not accurately reflect the true nature of swelling. We therefore designed a study using a non-contact 3D scanner to ensure the accuracy of clinical evaluations by comparing and quantifying volumetric changes in the face postoperatively. In some reports, changes in maxillofacial area have been evaluated by 3D measurement as soft tissue changes [16,22-25]. These reports also revealed that 3D measurements reflect actual soft tissue changes, thereby demonstrating the utility of 3D measurement.
The 3D scanner that we used in this study was an instrument that measures contour with a handheld visible light (non-laser), which allows 3D data to be obtained in a simple, non-contact manner. This 3D scanner can also be placed on top of a pillow on a chair for measurements and does not require any special installation space. However, because this instrument is a handheld scanner, the accuracy of facial measurements was a concern. Also of concern was that the measured digital data had different reference points in each scan and that 3D coordinates for point cloud data were not fixed. That is why we measured volumetric change by superimposing point cloud data using the ICP algorithm after confirming measurement accuracy with 3D models, as described above. Loon et al. [24] examined the clinical applications of the ICP algorithm by laser scanning the facial soft tissue of cleft lip and palate patients before and after surgery and comparing the pre- and postoperative volumes of the nose using the ICP algorithm. Verdenik et al. [25] also measured the superficial facial soft tissue before and after corrective surgery using a 3D scanner and used the ICP algorithm to measure displacement of the facial surface tissue before and after surgery by superimposing data from each scan. We also used the ICP algorithm to superimpose data. The ICP algorithm is extremely useful and we were able to demonstrate that measurements can be made with a high degree of accuracy. However, one issue to watch out for in scans taken with a handheld 3D scanner is the parts that the visible light does not reach during scanning due to hand movement-related camera shake. Parts of the face with a large amount of unevenness, such as the submandibular region, require particular caution during scanning. We saw cases of missing data during data analysis caused by the inability to scan the submandibular region. Hair exceeding a certain length can also result in missing data because it absorbs visible light. Accurate scans were therefore difficult to obtain in subjects with beards.
Many reports have described corticosteroid use for the purpose of preventing complications after extraction of impacted mandibular third molars [4-15]. Methods of administering corticosteroids have been described in a 2014 report by Selvaraj et al. [6], who injected methylprednisolone into the masseter and gluteal muscles prior to impacted mandibular third molar extraction and saw no significant difference between groups in terms of postoperative pain, swelling and trismus. Meanwhile, the anti-swelling effect of dexamethasone was addressed by Grossi et al. [7], who in 2007 submucosally administered dexamethasone at both 4 mg and 8 mg into the buccal vestibules of patients before surgery to compare changes in swelling. In 2008, Filho et al. [8] found that 8 mg of dexamethasone suppressed swelling significantly more than 4 mg of dexamethasone. In 2014, Darwade et al. [9] orally administered 8 mg of dexamethasone and 40 mg of methylprednisolone before surgery and saw no significant difference in pain in the dexamethasone group, but did report significant differences in swelling and limited mouth opening. Furthermore, in 2015, Chaudhary et al. [10] compared preoperative intravenous injection of 4 mg of dexamethasone and oral administration of 8 mg of dexamethasone and reported no significant differences in limited mouth opening, pain, or postoperative swelling. The aforementioned reports show that many studies have found a significant difference in the anti-swelling effects of dexamethasone; however, differences can arise depending on the method of measurement, dose, and route of administration.
In this study, we chose a simple method in which 4 mg of dexamethasone was locally injected into the cheek muscle on the side of the extracted tooth. We consequently saw significant suppression of swelling on postoperative day 1 and 3. These results are likely attributable to the long duration of action of about 36 hour for dexamethasone, which is one of the long acting corticosteroids. With regard to the limited mouth opening following impacted mandibular third molar extraction, Dionne et al. [11] in 2003 and Majid et al. [12] in 2010 reported that postoperative limitation of mouth opening is suppressed by the administration of 4 mg of dexamethasone. In our study, patient administered dexamethasone was able to open their mouths significantly more at 1, 3, and 7 days after surgery. These results suggest that dexamethasone acted for a long time on the masticatory muscles around the surgical site.
Taken together, 3D scanner is a useful tool in measuring facial swelling after the removal of impacted mandibular third molars. To avoid the complication, local administration of dexamethasone offers a significantly effective means of reducing postoperative swelling.
References
- Shugars DA, Gentile MA, Ahmad N, Stauropoulos MF, Slade GD, Phillips C, et al. Assessment of Oral Health-Related Quality of Life Before and After Third Molar Surgery. J Oral Maxillofac Surg. 2006; 64: 1721-1730.
- Kirtiloglu T, Bulut E, Sümer M and Cengiz I. Comparison of 2 Flap Designs in the Periodontal Healing of Second Molars After Fully Impacted Mandibular Third Molar Extractions. J Oral Maxillofac Surg. 2007; 65: 2206-2210.
- DE Menezes S A F, Cury P R. Efficacy of nimesulide versus meloxicam in the control of pain, swelling and trismus following extraction of impacted lower third molar. Int J Oral Maxillofac Surg. 2010; 39: 580-584.
- Beirne O R, Hollander B. The effect of methylprednisolone on pain, trismus and swelling after removal of third molars. Oral Surg Oral Med Oral Pathol. 1986; 61: 134-138.
- Esen E, Tasar F, Akhan O. Determination of the Anti-Inflammatory Effects of Methylprednisolone on the Sequelae of Third Molar Surgery. J Oral Maxillofac Surg. 1999; 57: 1201-1206.
- Selvaraj L, Rao SH, Lankupalli AS. Comparison of Efficacy of Methylprednisolone Injection into Masseter Muscle Versus Gluteal Muscle for Surgical Removal of Impacted Lower Third Molar. J Maxillofac Oral Surg. 2014; 13: 495-498.
- Grossi GB, Maiorana C, Garramone RA, Borgonovo A, Beretta M, Farronato D et al. Effect of submucosal injection of dexamethasone on postoperative discomfort after third molar surgery; A prospective study. J Oral Maxillofac Surg. 2007; 65: 2218-2226.
- Filho JRL, Maurette PE, Allais M, Cotinho M, Fernandes C. Clinical comparative study of the effectiveness of two dosages of dexamethasone to control postoperative swelling, trismus and pain after the surgical extraction of mandibular impacted third molars. Med Oral Patol Oral Cir Bucal. 2008; 13: 129-132.
- Chaudhary PD, Rastogi S, Gupta P, Indra BN, Thomas R, Choudhury R. Pre-emptive effect of dexamethasone injection and consumption on post-operative swelling, pain and trismus after third molar surgery; A prospective, double blind and randomized study. J Oral Biology and Crniofac Reserch. 2015; 15: 21-27.
- Dionne RA, Gordon SM, Rowan J, Kent A, Brahim JS. Dexamethasone suppresses peripheral prostanoid levels without analgesia in a clinical model of acute inflammation. J Oral Maxillofac Surg. 2003; 61: 997-1003.
- Majid OW, Mahmood WK. Effect of submucosal and intramuscular dexamethasone on postoperative sequelae after third molar surgery: Comparative study. Br J Oral Maxillofac Surg. 2010; 49: 647-652.
- Boonsiriseth K, Klongnoi B, Sirintawat N, Saengsirinavin C, Wongsirichat N. Comparative study of the effect of dexamethasone injection and consumption in lower third molar surgery. Int J Oral Maxillofac Surg. 2012; 41: 244-247.
- Alcântara CE, Falci SG, Oliveira-Ferreira F, Santos CR and Pinheiro ML. Pre-emptive effect of dexamethasone and methylprednisolone on pain, swelling, and trismus after third molar surgery; A split-mouth randomized triple-blind clinical trial. Int J Oral Maxillofac Surg. 2014; 43: 93-98.
- Marques J, Pie-Sanchez J, Figueiredo R, Valmaseda-Castellon E, Gay-Escoda C. Effect of the local administration of betamethasone on pain,swelling and trismus after impacted lower third molar extraction; A randomized, triple blinded, controlled trial. Med Oral Patol Oral Cir Bucal. 2014; 19: 49-54.
- Rana M, Gellrich NC, Ghassemi A, Gerressen M, Riediger D, Modabber A. Three-dimensional evaluation of postoperative swelling after third molar surgery using 2 different cooling therapy methods; a randomized observer-blind prospective study. J Oral Maxillofac Surg. 2011; 69: 2092-2098.
- Hooley J R, Francis F H. Betamethasone in traumatic oral surgery. J Oral Surg.1969; 27: 398-403.
- Fan T, Wang G, Mao B, Xiong Z, Zhang Y, Liu X, et al. Prophylactic administration of parenteral steroids for preventing airway complications after extubation in adults:meta-analysis of radomised placebo controlled trials. BMJ. 2008; 337: 1841.
- Schietroma M, Cecilia EM, Carlei F, Sista F, De Santis G, Lancione L, et al. Dexamethasone for the prevention of recurrent laryngeal nerve palsy and other complications after thyroid surgery; A randomized double-blind placebo-controlled trial. JAMA Otolaryngol Head Neck Surg. 2013; 139: 471-478.
- Worni M, Schudel HH, Seifert E, Inglin R, Hagemann M, Vorburger SA, et al. Randomized controlled trial on single dose steroid before thyroidectomy for benign disease to improve postoperative nausea, pain and vocal function. Ann Surg. 2008; 248: 1060-1066.
- Chung.H.K, Lindsay.M.H, Emma.J.H. A different look: 3-dimensional facial imaging of a child with Binder syndrome. Am J Orthod Dentofacial Orthop. 2007; 132: 704-709.
- Yamamoto S, Miyachi H, Watanabe S, Hujii H, Simozato K. Analysis of Facial Scanner depending on Postual Change. Jpn J Jaw Deform.2016; 26: 18-25.
- Loon BV, Maal TJ, Plooij JM, Ingels KJ, Borstlap WA, Kuijpers-Jagtman AM, et al. 3D Stereophotogrammetric assessment of pre-and postoperative volumetric changes in the cleft lip and palate nose. Int J Oral Maxillofac Surg. 2010; 39: 534-540.
- Verdenik M, Hren NI. Differences in three-dimensional soft tissue changes after upper, lower or both jaw orthognathic surgery in skeletal class III patients. Int J Oral Maxillofac Surg. 2014; 43: 1345-1351.