
Case Report
J Dent & Oral Disord. 2016; 2(9): 1044.
Localized Gingival Hyperplasia Influenced by Pregnancy
Sachdeva S¹*, Saluja H², Mani A¹, Tandon P² and Dalvi A¹
¹Department of Periodontics, Pravara Rural Dental College and Hospital, India
²Department of Oral and Maxillofacial Surgery, Pravara Rural Dental College and Hospital, India
*Corresponding author: Shivani Sachdeva, Department of Periodontics, Pravara Rural Dental College and Hospital, Maharashtra, India
Received: October 10, 2016; Accepted: November 16, 2016; Published: November 17, 2016
Abstract
Gingival enlargements are a common clinical finding and most represent a reactive hyperplasia as a direct result of plaque related inflammatory gingival disease. These generally respond to conservative tissue management and attention to plaque control. Its significant incidence of occurrence (1.5-8%) during pregnancy and warrants the need for a meticulous oral hygiene care so as to reduce and eliminate the exuberant tissue response to local irritation or trauma seen in such cases. The manuscript highlights one such case report seen in our department.
Keywords: Gingival hyperplasia; Gingival enlargement; Pregnancy tumor
Introduction
Pregnancy tumor appears often during 2nd or 3rd month of pregnancy presenting clinically [1] as a tumor like gingival enlargement due to an exaggerated conditioned response to minor trauma [2]. It manifests as a painless, sessile or pedunculated, ulcerated lesion sized a few millimeters to several centimeters with a smooth or lobulated surface and red to deep blue color according to the vascularity [3,4]. These lesions are due to the hormonal variations during pregnancy which induces change in the vascular permeability leading to gingival edema.
Case Report
A 29 years old pregnant patient was referred from the outpatient department, Department of Obstetrics and Gynaecology, to the outpatient department, Department of Periodontics, Pravara institute of medical sciences, with a complaint of swollen gums (overgrowth) in upper left back teeth, since a period of 2 months. Small at onset the swelling had grown rapidly over the last one month to attain its present size, accompanied by dull, continuous pain. It was causing her considerable discomfort during mastication. She was in her 2nd trimester (5th month) of pregnancy. Poor oral hygiene was appreciated during the clinical examination (Figure 1).
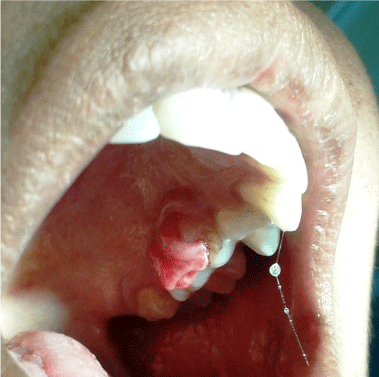
Figure 1: Preoperative view.
The growth in this region has considerably increased adding to her discomfort. The patient did not have any other systemic disease. Systemic examination revealed an exophytic, pedunculated roughly square shape red swelling on the left posterior maxilla, extending only lingually. The lesion measured approximately 10 mm (length) and 7 mm (width) on the lingual aspect. The swelling was tender, fibrotic with a firm base and an ulcerated surface (Figure 2).
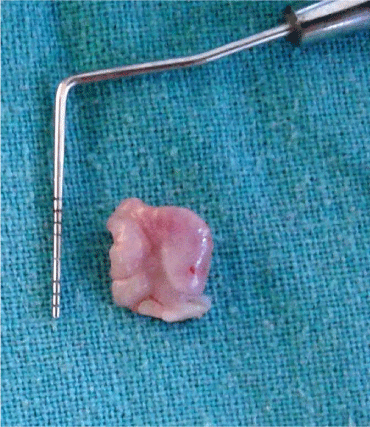
Figure 2: Excised gingival overgrowth.
Radiographic examination revealed little bone loss and widened periodontal ligament space and hazy trabecular pattern. Ethical committee clearance was taken and the patient was taken for surgery.
Excision of the lesion was done with a wide margin and the excised specimen was sent for histopathologial evaluation. The histopathological section showed epithelium encircling the major part of fibrovascular stroma and at one end ulcerated epithelium was evident under higher magnification. Epithelium was of stratified squamous parakeratinized type showing pseudo-epitheliomatous hyperplasia. The stroma showed numerous dense bundles of collagen fibres with areas of hyalinization. Numerous endothelial lined blood vessels with Red Blood Corpuscles (RBCs) and capillaries were seen. Numerous chronic inflammatory cells predominantly lymphocytes and a few plasma cells were seen. These features were consistent with a histopathological diagnosis of pyogenic granuloma (Figure 3).
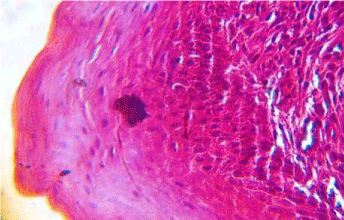
Figure 3: Histopathological examination under high power magnification
(40X).
Evaluation of the patients at recall visits revealed uneventful healing with no recurrence of the lesion.
Discussion
This conditioned gingival enlargement seen in pregnancy demonstrates a definite exacerbated response of the tissues to local irritants attributed to an underlying increase in circulating female sex hormones as occurring in pregnancy.
Gingiva is a common site for either neoplastic or non-neoplastic lesions. The great majority of localized overgrowths of gingiva are considered to be reactive and non-neoplastic lesions which are usually inflammatory or represent a reaction to trauma or low-grade injury [4].
These lesions show a predilection for the interdental papillae region, maxillary anterior region being affected the most [5]. These lesions however, have been confused in the past to clinically similar enlargements seen in non-pregnant females as well as males [6]. These lesions have been coined by the term pyogenic granulomas.
Comparison of histopathological features of the two conditions reveals that the surface epithelium in pregnancy enlargements tends to be thickened with prominent rete pegs in contrast to an atrophic rete pegs seen in pyogenic granuloma, though the clinical appearance of the two is strikingly similar. Another differentiating feature between the two conditions is the increased levels of the pigmented rods. Prevotella intermedia in the gingival crevice of areas showing the enlargement in pregnant individuals. This gram negative anaerobic rod is known to utilize the increased steroid levels as a source of nourishment and growth and the inflammatory factors released by it may be partly responsible for eliciting the exacerbated response.
Treatment of such enlargements consists of elimination of irritating local factors and conservative surgical excision, which is usually curative. In the present case, poor oral hygiene and malpositioning of teeth were the precipitating factors. Therefore, scaling and excision of lesion was performed. Furthermore, oral prophylaxis and oral hygiene instructions were reinforced to avoid recurrence of the lesion as pyogenic granuloma has a relatively high rate of recurrence (15%).This is true especially in pregnant patients [2].
Conclusion
The pyogenic granuloma though benign in nature may grow to an alarming size and cause pain and discomfort to the patient. Thus early intervention through reinforcement of adequate oral hygiene measures along with surgical excision of the lesion is deemed necessary.
References
- Jafarzadeh H, Sanatkhani M, Mohtasham N. Oral pyogenic granuloma: J Oral Sci. 2006; 48: 167-175.
- Amirchaghmaghi M, Falaki F, Mohtasham N, Mozafari PM. Extragingival pyogenic granuloma: A case report. Cases J. 2008; 1: 371.
- Koman KS, Loesche WJ. The subgingival microflora during pregnancy. J Periodontal Res.1980; 15: 111.
- Raber-Durlacher JE, van Steenbergen TJ, Van der Velden U, de Graaff J, Abraham-Inpijn L. Experimental gingivitis during pregnancy and postpartum: Clinical, Endocrinological and microbiological aspects. J Clin Periodontol. 1994; 21: 549-558.
- Karthikeya Patil, VG Mahima, K Lahiri. Extragingival pyogenic granuloma. Indian Journal of Dental Resarch. 2006; 17: 199-202.
- Ababneh KT. Biopsied gingival lesions in Northern Jordanians: A retrospective analysis over 10 years. Int J Periodontics Restorative Dent. 2006; 26: 387- 393.