
Case Report
J Dent & Oral Disord. 2017; 3(2): 1058.
Full Mouth Rehabilitation with Modified Andrew’s Bridge Following Le Fort Osteotomy for a Patient with Maxillary Retrognathia
Saumyendra SV¹, Gaurav B¹, Varun B¹, Kumar SK², Kamleshwar S¹ and Deeksha A*¹
¹Department of Prosthodontics & Dental Material Sciences, K.G. Medical University, India
²Department of Plastic Surgery, K.G. Medical University, India
*Corresponding author: Deeksha Arya, Department of Prosthodontics & Dental Material Sciences, F.O.D.S, K.G. Medical University, Lucknow, India
Received: April 03, 2017; Accepted: April 26, 2017; Published: May 03, 2017
Abstract
Oro-facial trauma may lead to irreversible soft and hard tissue loss requiring complex multidisciplinary intervention for satisfactory functional and esthetic rehabilitation. This requires efficient diagnosis and an elaborate treatment plan to optimize stomatognathic function, health and esthetics which translates to patient comfort and satisfaction. This case report describes such a rehabilitation of a 38 year old female who lost her anterior teeth with adjacent bone in an accident. An interdisciplinary approach using an intentional Le forte 1 osteotomy and an Andrew’s fixed partial denture was used to successfully rehabilitate the patient.
Keywords: Andrew’s bridge; Full mouth rehabilitation; Le Fort osteotomy; Retrognathia
Introduction
Trauma to the facial structures affects a patient physically as well as mentally. The personality, personal & social life and confidence levels may be badly affected as a result of the disfigurement. Such esthetic challenges often require a complex and well defined treatment plan involving various specialties to achieve a successful conclusion with an ultimate treatment goal to achieve normal function and appearance [1].
The area of soft tissue and teeth displayed when a patient smiles is referred to as the esthetic zone and normally includes the teeth in the maxillary arch till the second premolar. Tooth and tissue replacement in this area presents a challenge especially when the loss includes significant amounts of alveolar bone and accompanying tissue. At the same time, designing a method for achieving reasonable esthetics in such cases can be most rewarding [2].
Restoration of esthetics, comfort, and function should be the major focus of oral rehabilitation. The term ‘esthetic’ refers to theory and philosophy relating to beauty and the beautiful, and in dentistry, this term applies especially to the appearance of the dental restoration, achieved through form and/ or color [3].
The prosthetic options for replacement of missing anterior teeth are resin-bonded partial dentures, conventional Fixed Partial Dentures (FPDs), removable partial dentures and implant-supported fixed prostheses [4,5]. In this clinical report, because of prevailing limitations, a full mouth rehabilitation after a Le forte-1 osteotomy, utilizing an anterior removable-fixed prosthesis was done [6].
Case Presentation
A 38-year-old woman presented with the complaint of depressed middle face and missing anterior teeth 3 years back. She gave a history of having visited several clinicians for a solution to her problem before coming to us. Dental history of the patient revealed that the patient fell from a roof 7 years earlier, when she lost her upper anterior teeth and adjacent bone with a Le forte-1 fracture. She also lost her mandibular central incisors. Later on, the missing maxillary teeth were replaced with a fixed partial denture but the patient was not satisfied with the esthetic results obtained because of depressed mid face and insufficient upper lip support. Extraoral examination of profile of the patient was straight with depressed premaxilla (Figue 1&2). Clinical examination revealed an asymmetric edentulous space in the maxillary incisor region consisting of missing 11, 12, 21 and 22 (Figure 3a). The other teeth that were missing were 17, 31 and 41. Silver amalgam restorations were present in 18 and 48. Crown preparations had been done previously on 13, 23, 24 and 33, 32, 42, 43 (Figure 3a). 33, 32, 42 and 43 had tilted labially because of no antagonist contact, with gingival recession on 32 and 42. The patient presented with a fixed partial denture replacing the upper missing teeth but was not satisfied with this restoration and therefore had left the previous clinician (who had attended her 3 and a half years ago) before the mandibular fixed partial denture could be completed. She was not wearing any replacement for her remaining missing teeth. Her medical history was non-contributory without contraindications for dental treatment.

Figure 1: (a) Pre rehabilitation and (b) Post rehabilitation frontal views.
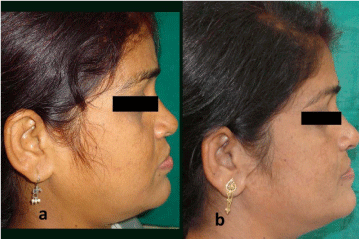
Figure 2: (a) Pre rehabilitation and (b) Post rehabilitation profile views.

Figure 3: (a) Pre rehabilitation view and (b) Intraoral view post cementation
of metal bar and mandibular fixed partial denture.
The case was referred to the Department of Plastic Surgery for correction of horizontal maxillary deficiency. A Le Forte-I osteotomy [7] for maxillary advancement was performed. Two months after discharge and healing the patient reported to us. After completing the necessary clinical and radiographic examination (Figure 4 & 5), the prosthodontic treatment plan of the patient was initiated. At that time, the patient had a disturbed occlusion due to maxillary advancement.
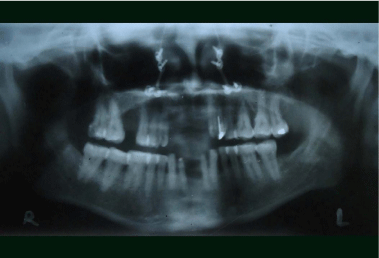
Figure 4: Orthopantogram following osteotomy and removal of upper fixed
partial denture.
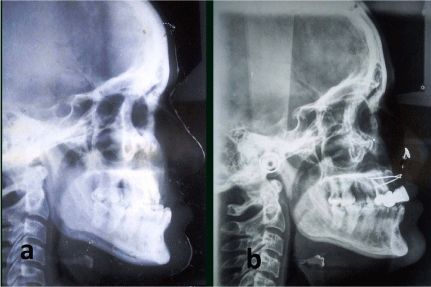
Figure 5: (a) Preosteotomy and (b) Postosteotomy lateral cephalograms.
Sagittal relationship of maxillary residual ridge and mandibular anteriors had definitely improved, but was still not ideal because of maxillary residual ridge resorption and labial tipping of mandibular anteriors, leading to a maxillary retrognathic appearance. The temporomandibular joints were normal.
Preosteotomy and postosteotomy lateral cephalograms were taken. Orthopantogram following osteotomy and removal of upper fixed partial denture was taken. Diagnostic casts, IOPAs and photographs were made.
Preliminary full-arch impressions were made and poured. A face-bow registration was used to mount casts on a semi-adjustable articulator in centric relation. As a result of the surgery, the patient had lost stable stops incentric occlusion. This was addressed using the Pankey Mann Schuyler’s philosophy of full mouth rehabilitation as modified by Dawson [8]. First, diagnostic wax up of the mandibular anteriors was completed as per esthetics and phonetics. A putty index of this was used to fabricate provisionals and permanent porcelain fused to metal restorations of the missing mandibular anterior teeth (33-43). To cover gingival recession on mandibular right and left lateral incisors cervical portion of the prosthesis was made with gingival autopolymerizing acrylic resin (Trevalon, Dentsply Ltd, Gurgaon, India). The advantage of using autopolymerizing resin isthat, it can easily be applied chair side and replaced. The Broadrick’s flag was used to correct and make modifications in mandibular posteriors for correction of occlusal plane.
The missing maxillary right first molar was replaced with a 3 unit fixed partial denture with porcelain facings as per planned occlusal scheme. Occlusal discrepancies were corrected by marking interferences on articulated casts and using these as a guide to correct interferences in the mouth. The end goal was posterior disclusion in protrusion (by the first premolars) and group function in lateral excursions, with disclusion on non working side. Protrusive disclusion was not possible by any tooth anterior to the first premolar as these teeth were either missing or were to support a removable prosthesis.
While restoring the maxillary anterior segment, some modifications were made to the original Andrews bridge system. A vertical precision bar attachment system (Preci-Horix; Ceka Attachments Preci-cline; Alphadent NV, Waregen, Belgium) consisting of a prefabricated bar, length 50 mm, height 4 mm - ø 1.8 mm (male part) and 2 clip (female part) attachments was utilized. The flexible nylon clips in this system gets locked with the bar to provide retention and stability to the prosthesis.
Elective endodontic treatment was done on the maxillary canines and they were prepared to receive cast copings attached to the bar over them. Wax pattern copings were fabricated incorporating the plastic bar attachment. This was cast, finished, polished, checked for fit and luted to the abutments (Figure 3). The space between the bar and ridge was blocked with modeling wax and full maxillary arch impression made. The poured cast was used to wax an anterior teeth setting trial from 13 to 23. Esthetics, phonetics and occlusion were checked and verified during the try in appointment. The prosthesis was then processed and finished in the usual manner and evaluated intraorally. The processed maxillary denture already had space for the bar within it. This area was trimmed a little more (about 0.5 mm). Now, the nylon female parts were seated to the metal bar in the mouth and the space between the bar and ridge again blocked. Autopolymerizing resin was added to the trimmed space in the maxillary denture and the denture seated in position. The denture was removed containing the female part (Figure 6 & 7).
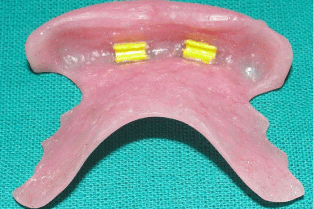
Figure 6: Intaglio view of prosthesis with nylon female parts.
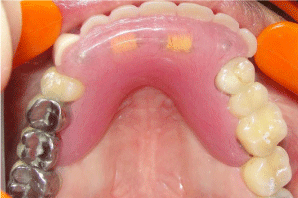
Figure 7: Fully restored maxillary arch.
The patient has been going through routine post insertion appointments and adjustments since the past 3 years. She is more satisfied with her present prosthesis than previous ones but this required meticulous counselling from the start to the present date. The patient would still prefer a fixed prosthesis but has come to terms with her anatomic limitations. The nylon female parts got worn out after an year and had to be replaced. The patient was maintaining good oral hygiene at the time of reporting this case (Figure 1b, 2b, 3b).
Discussion
Le forte I osteotomy is performed for correction of horizontal maxillary defects. Other options for mid facial advancement include distraction osteogenesis after Le forte III or monoblock osteotomy [9]. Some minor complications may occur with Le forte I osteotomy such as buckling of the nasal septum and reduction in volume of the nasal cavity. “Buckling” of the septum is not seen when proper reduction of the nasal septum and vomer is accompanied with superior repositioning of the maxillary complex. Bell et al stated that the relatively small reduction in the size of the nasal cavity is of no practical consequence and does not have a significant effect on nasal air flow or on speech [10].
The management of missing anterior teeth requires extensive treatment planning, especially when accompanied with maxillary retrognathia and disturbed occlusion. The treatment of choice is always to replace missing teeth with a fixed prosthesis. It has been stated that it may be better to avoid multiple components necessary to support an anterior segment of the removable partial denture by using a fixed prosthesis [11].
While making the treatment plan for the patient, a limiting feature was the patient’s refusal to additional surgical procedures. The treatment options therefore consisted of a removable or fixed partial denture. A purely removable prosthesis was unacceptable to the patient and a purely fixed one was not feasible, considering leverage that would be placed on the abutments by anteriorly placed pontics, as well as forwardly placed mandibular anteriors. Also, such a prosthesis would be extremely bulky, considering the resorbed ridge and anterior placement of pontics (necessary for esthetics), and difficult to maintain hygienically. Implants were ruled out because the patient refused to consider further surgical interventions necessary to augment the maxillary anterior ridge or place implants. Orthodontic correction was not preferred due to lack of adequate anchorage and patient did not want because of the treatment duration. A treatment option was needed that would allow successful rehabilitation, while taking into consideration the anatomical limitations and patient acceptance. So, the modified Andrew’s bridge system was used for restoration of the maxillary anterior region in this condition.
The Andrews bridge system was introduced by Dr James Andrews of Amite, Louisiana and consisted of a metal bar and sleeve. The bar was soldered to the retainers. The pontic portion of the fixed-removable partial denture is removable and permits access to the underlying tissues for cleaning purposes, allowing tissue rest and lesser non continuous forces on underlying teeth/tissues [12]. The major technical problem in the original system was soldering of bar to the retainers6. We modified this technique by using a precast bar & coping connector with an attachment system which was meant to be used as part of an extracoronal attachment in removable partial dentures. This fixed-removable prosthesis provided physiologic advantage of effective oral hygiene maintenance and increased stability by splinting abutment teeth. The long term disadvantage of using the nylon clips and bar assembly is that the clips wear out after a period of 1 to 2 years and need to be replaced.
Orofacial trauma with irreversible soft and hard tissue loss can be successfully managed by an interdisciplinary approach. Structural and functional harmony can be restored if proper diagnosis and sequential treatment plan is followed. Surgical intervention combined with full mouth rehabilitation and modified Andrew’s bridge for this patient with maxillary retrognathia and anterior teeth loss proved to be successful. Proper and comprehensive patient counseling to undergo a long treatment process, with the end result of a semi-fixed prosthesis was a take home point of this report.
References
- Naini FB, Moss JP, Gill DS. The enigma of facial beauty: Esthetics, proportions, deformity, and controversy. Am J Orthodont Dentofac Orthoped. 2006; 130: 277-282.
- Lin S, Levin L , Goldman S, Peled M. Dento-alveolar and maxillofacial injuries–a retrospective study from a level 1 trauma center in Israel. Dent Traumat. 2007; 23: 155-157.
- Samorodnitzky-Naveh GR, Geiger SB, Levin L. Patients' satisfaction with dental esthetics. J Amer Dent Assoc. 2007; 138: 805-808.
- Haralur SB, Shahrani OS. Replacement of Missing Anterior Teeth in a Patient with Temporomandibular Disorder. Case Report Dentistry vol. 2014.
- Haralur SB, Al- Qahtani AS. Replacement of Missing Anterior Teeth in a Patient with Chronic Mouth Breathing and Tongue Thrusting. Case Report Dentistry vol. 2013.
- Gubrellay P, Gubrellay P, Vyas R. Andrews Bridge System – A literature Review. Int J Res Dent. 2014; 4: 59-62.
- Kramer FJ, Baethge C, Swennen G, Teltzrow T, Schulze A, Berten J et al. Intra- and perioperative complications of the LeFort I osteotomy: a prospective evaluation of 1000 patients. J Craniofac Surg. 2004;15: 971-977.
- Baid GC, Lakshman SD, Marilingaiah A, Lunkad H. Comprehensive treatment of compromised dentition: An interdisciplinary approach. J Interdiscipl Dent. 2012; 2: 205-210.
- Sinha R, Menon PS, Venugopal MG. A clinical evaluation of midface advancement using intraoral distractors in management of bone stock deficiencies. MJAFI. 2011; 67: 245-252.
- Bell C, Thrash WJ, Zysset MK. Incidence of maxillary sinusitis following Le Fort I maxillary osteotomy. J Oral Maxillofac Surg. 1986; 44: 100-103.
- Witter DJ, Gerritsen AE, de Baat C, Creugers NH. Prosthetic replacement of missing teeth. Indications for fixed and removable dental prostheses. Ned Tijdschr Tandheelkd. 2014 ; 121: 45-56.
- Muthuvignesh J, Swamikkanu B, Egammai S, Donapati NR. Improving Facial Esthetics with an Andrew’s Bridge: A Clinical Report. Ind J Multidiscipl Dent. 2013;4: 884-887