
Research Article
J Dent & Oral Disord. 2017; 3(5): 1072.
Prevalence of Early Childhood Caries among Children at Two Community Health Centers in Hawaii
Logigian JL¹* and Okuji DM²
¹NYU Lutheran Advanced Education in Pediatric Dentistry-Hawaii, USA
²NYU Langone Health System, New York, USA
*Corresponding author: Jennifer L. Logigian, NYU Lutheran Advanced Education in Pediatric Dentistry- Hawaii, USA
Received: June 28, 2017; Accepted: August 03, 2017; Published: August 10, 2017
Abstract
Purpose: The purpose of this cross-sectional study was to compare the prevalence of Early Childhood Caries (ECC) among children under age 6 in two Federally Qualified Community Health Centers (FQHC) in Hawaii, one urban and one rural.
Methods: Thirty-seven children who met inclusion criteria received a clinical examination and had their Decayed, Missing and Filled Teeth Index (DMFT) score recorded. The parent of each child filled out a self-administered ten-question survey regarding caries risk factors, oral health practices and demographic information.
Results: The average number of decayed teeth per child was 5.6, with the urban average being lower (4.2) than the rural (7.5) DMFT scores were not normally distributed so Wilcoxon-Mann-Whitney and Kruskal Wallis tests were performed to test for differences between mean values of scores; the data showed slight difference in prevalence of ECC between sex, race and among children born outside of the United States, but these were not statistically significant. The hypothesis that children in the rural FQHC would have higher median DMFT scores than those in the urban FQHC was supported by the data (p=0.03).
Conclusion: Children in the rural FQHC had a higher prevalence of DMFT than children in the urban FQHC. Parent-reported habits and home care practices did not seem to accurately correspond to patients’ DMFT score and clinical presentation, indicating that many parents may have inaccurately reported on the self-administered questionnaire.
Keywords: Early childhood caries; Community health; Dental
Abbreviations
ECC: Early Childhood Caries; S-ECC: Severe Early Childhood Caries; FQHC: Federally Qualified Community Health Centers; KKV: Kokua Kalihi Valley Comprehensive Family Services; LCHC: Lanai Community Health Center; DMFT: Decayed, Missing, Filled Teeth; AAPD: American Academy of Pediatric Dentistry
Introduction
The state of Hawaii is unique both in its population make-up and its geographic location. While many think of Hawaii as simply a vacation destination, there are over1.4 million residents who call the islands home, and close to 22% of these residents are children under the age of 18 [1]. Data from the 2010-2014 United State Census indicates that Native Hawaiians, Asians and Pacific Islanders make up the majority of the population of the Hawaiian Islands; this is in contrast to population and demographic data from the other 49 states, of which non-Hispanic whites, non-Hispanic blacks, and Hispanics or Latinos compromise the racial majorities [1,2]. The number of Native Hawaiians living in Hawaii has continued to increase over the past century as well [3]. Likewise, the geography of Hawaii is particularly distinct from other states, in that it is comprised of eight main islands, seven of which are inhabited. Each island has a different racial/ethnic makeup as well as varying degrees of access to medical and dental care.
Unfortunately, Hawaii has continued to rank among the worst performing states in terms of oral health. In 2015 Hawaii was one of only three states to receive a score of “F” on its oral health report card published by The Pew Center on the States, marking the fifth year in a row it received the lowest possible grade [4]. A 2015 report on oral health issued by the Hawaii State Department of Health: Family Health Services Division found that adults living outside of Honolulu County were less likely to have seen a dentist in the past year than those living within Honolulu County. In order to access dental services, residents often have to travel between islands to find providers and specialists who can provide needed care. In 2009 3,633 people were transported from their home island to Honolulu for dental services, at a cost of $1.2 million; of these, 87% (3,153) were children [5].
Clearly, there is a need for improved oral health education and access to care in Hawaii, however it is also essential to take into consideration that the racial and ethnic background of the population varies significantly from the rest of the country. It might then be inferred that oral health habits as well as childhood caries prevalence may vary significantly from island to island, depending upon cultural factors and resources available. Understanding these attitudes and challenges can allow us to better tailor preventative and early education programs to the different populations in Hawaii.
In addition, there is quite a bit of existing literature that has demonstrated a link between geographic location – as well as access to dental care – and the prevalence of Early Childhood Caries (ECC). Similar research has been conducted in India, Africa and Australia that has found a greater prevalence of ECC among children in rural areas where access to dental services is often limited.
The purpose of this cross-sectional study was to compare the prevalence of ECC among children under age 6 in two Federally Qualified Community Health Centers (FQHC) in Hawaii, one urban and one rural.
Materials and Methods
The Institutional Review Board of NYU Lutheran Medical Center as well as the executive directors of Kokua Kalihi Valley Comprehensive Family Services (KKV) and Lanai Community Health Center (LCHC) approved the survey and informed consent protocol.
KKV is a health center located in urban Honolulu on the island of Oahu, the most populous island in Hawaii (almost 1 million residents); LCHC is the only community health center on rural Lanai Island, the second least populated island (just over 3,000 residents) and the second smallest island of the inhabited islands of Hawaii. Study participants were selected on the basis of location and had to be patients of one of two federally qualified health centers either KKV or LCHC. Participants were also selected on the basis of age and had to be 71 months or younger at the time the survey was completed, in accordance with the American Academy of Pediatric Dentistry definition of early childhood caries [6]. Children of both sexes and from all ethnic backgrounds were eligible to participate in this study. Exclusion criteria were limited to children who were not patients of either KKV or LCHC and who were older than 71 months of age. No attempts were made to seek out participants who met the inclusion criteria; rather patients who presented for regularly scheduled exams were screened at the time of check-in for eligibility to participate in the study.
Data was collected at KKV over the course of 6 weeks in February- March 2016 and at LCHC over the course of 4 weeks in April 2016.
Questionnaire
A questionnaire was created that sought to address issues related to maternal understanding of oral health, children’s home care habits and diet and past dental history [7,8]. Much literature exists to support a strong relationship between high caries risk in children and low educational attainment in the parent as well as low socioeconomic status [9-11]. Published studies conducted to assess correlation between caries prevalence and risk factors among children were referenced [12-20]. The questionnaire also utilized questions that were adapted from existing published studies that had been previously standardized and/or validated or from existing caries risk indicators [21-24].
Verbal and written consent was obtained from the parent(s) at the time of the exam. In the instance that a parent was not fluent in English, an on-site interpreter was available. This was only necessary in one of the thirty-seven cases; the preferred language was Chuukese and a native speaker was utilized to verbally interpret the consent and the survey for the parent.
The questionnaire was distributed to the parent of each study participant and was self-administered.
Examination
The criteria for Early Childhood Caries (ECC) and Severe Early Childhood Caries (S-ECC) were taken from The American Academy of Pediatric Dentistry (AAPD).ECC is defined as, “…the presence of 1 or more decayed (noncavitated or cavitated lesions), missing (due to caries), or filled tooth surfaces in any primary tooth in a child 71 months of age or younger.” S-ECC is any sign of smooth-surface caries in a child younger than 3 or, “From ages 3 through 5, 1 or more cavitated, missing (due to caries), or filled smooth surfaces in primary maxillary anterior teeth or a decayed, missing, or filled score of =4 (age 3), =5 (age 4), or =6 (age 5) surface” [6].
A clinical examination was completed on participants who presented to the clinics for scheduled examinations (ADA dental codes: D0145, D0120, D0150). Findings were based only on visual examination and using the decayed, missing, filled index according to the process outlined by the World Health Organization [21,25]. Identification of carious and white-spot lesions was completed using the evidenced-based recommendations published by an expert panel convened by the American Dental Association Council on Scientific Affairs in 2008 [26]. Visual examination was completed after cleaning and drying the teeth. Additional criteria for identifying carious lesions were taken from the Association of State and Territorial Dental Directors and the textbook Pediatric Dentistry: Infancy through Adolescence [8,27]. No invasive or irreversible procedures were completed as part of the examination. A Single Licensed Dentist (JLL) completed all examinations.
Results
A total of thirty-seven children were included in the study, 60% (n=22) of these children were from the urban (KKV) clinic and 40% (n=15) from the rural (LCHC) clinic. The mean age was 3.16 years old, with a younger mean age at KKV (2.7) than at LCHC (3.8). While the gender distribution was relatively even overall (46% female, 53% male), and was somewhat similarly represented at KKV (59% female, 41% male), LCHC had a much different gender distribution and males were better represented in the study sample than females (27% female, 73% male). The majority of children identified as Filipino (30%), Native Hawaiian (27%) or Other Pacific Islander (24%), though there was a greater percentage of Filipino (36%) and Other Pacific Islander (36%) patients at KKV than at LCHC, where the majority (60%) were Native Hawaiian. At both clinics the vast majority of children (n=35, 95%) were born in the US. There were a much higher number of parents with graduate-level education at KKV (45.5% compared with 13% at LCHC); this may be due to study wording and is discussed in the limitations section below (Figure 1.).
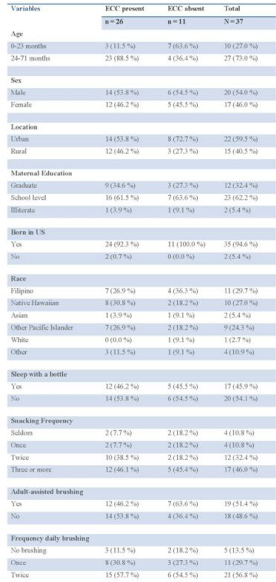
Figure 1: Variables Study.
Interestingly, whether or not a child was put to bed with a bottle varied between the clinics. 27% of patients were put to bed with bottle at some point at KKV, yet 73% were put to bed with a bottle at LCHC. More parents reported adult-assisted brushing at KKV (64%) than at LCHC (33%), and families at KKV were less likely to report no brushing (5%) than at LCHC (27%). Fewer patients at KKV had difficulty accessing dental care (23%) than at LCHC (33%), which is not surprising considering the rural location of LCHC.
The average number of decayed teeth per child was 5.6, though the average at KKV was much lower (4.2) than at LCHC (7.5). The average number of missing teeth overall was 0.5, and this remained relatively consistent between the two clinics (KKV=0.4, LCHC=0.6). Generally, the average number of previously filled teeth was 1.3, with 0.6 average at KKV and 2.3 at LCHC. The mean number of decayed teeth was 5.57± 6.49 (mean ± standard deviation); the mean number of missing teeth was 0.49± 0.99; the mean number of filled teeth was 1.3± 2.8.
DMFT scores were not normally distributed (Figure 2) so t-tests or ANOVA tests could not be appropriately applied. Alternatively, Wilcoxon-Mann-Whitney and Kruskal Wallis tests were performed to test for differences between median values of scores; these are essentially non-parametric analogs to the independent samples t-test/ANOVA. The data indicated that urban parents have a significantly lower rate of putting their child to bed with a bottle than rural parents. In addition, there was also a difference of borderline statistical significance (p=.07) demonstrating that urban parents had higher rates of helping their child brush than did rural parents as well as a difference of borderline statistical significance (p=.08) wherein urban children had a lower number of filled teeth than rural children. Most notably, the main hypothesis that there would be differences in DMFT scores between the rural and urban clinics was also supported by the data (p=0.03).

Figure 2: Distribution of DMFT Score.
Discussion
Similar studies have been conducted worldwide to examine caries risk and caries prevalence in urban and rural populations to understand how geographic location can affect oral health and access to care. While children in urban settings can and do have high DMFT scores, it is often the case that their rural-based counterparts tend to have a higher prevalence of ECC, often attributed to lack of resources and adequate available dental care.
A total of 37 children were screened for this study. The prevalence of ECC in both locations was 70%. When broken down, 64% of children at the urban KKV clinic had ECC and 80% of children at rural LCHC had ECC. This corresponds with the main hypothesis of this study as well as with other existing literature regarding ECC and geographic location.
Many of the responses to the oral health variables included in the questionnaire that related to home care and diet did not seem to correspond as expected to clinical findings. For example, of the children with ECC, the majorities (53.8%) of them were not put to bed with a bottle and also did report brushing their teeth at least twice a day (57.7%). Of the children without ECC, the majority (45.4%) of them ate 3 or more sugary snacks or beverages per day. Children who fell asleep with a bottle had a DMFT score of 0.4, in contrast with 2.3 for children who weren’t put to sleep with a bottle. Likewise, those children whose parent reported brushing twice per day had a DMFT score of 2.1, whereas those whose parents reported no brushing at all have a DMFT score of 0.These parent-reported variables all appear to be quite opposite from what might be expected of these groups and bring into question the validity of the parent-reported responses to the self-administered questionnaire. Nevertheless, the present study supports previous data that has demonstrated an increase in ECC prevalence among children in rural America [28].
Conclusion
Based on the results of this study, it can be concluded that the prevalence of early childhood caries in Hawaii is higher in the rural sample population on the island of Lanai than the urban sample population on the island of Oahu. This contributes to the existing data that has shown a correlation between geographic location (and possibly population demographics) and access to care for pediatric patients in the state of Hawaii.
Limitations
LCHC was in the process of building and opening a new community health center at the time of this research proposal (summer 2015). Dental services were also being added, something that had not previously been offered. Though the anticipated start date for the dental clinic was September 2015, the first patients were not seen and/or screened until early spring 2016. This led to a significantly smaller number of subjects than was initially anticipated. Also because of the structure of the clinic schedule for the year, the primary examiner had only a limited amount of time at each of the two clinics during which to collect data.
Another limitation that became apparent from the start was confusion over parental interpretation of some of the study questions. While every effort was made to implement previously validated questions, it appeared as if there was misunderstanding regarding certain definitions based upon the responder’s background. For example, many Filipino parents checked “graduate level” as a response to highest education level, when, upon inquiry, they were referring to having graduated from primary or high school. Also, many parents were not born and educated in the United States, so those who graduated from a foreign university may have received a different education from those who graduated from a US-based 4-year university.
Similarly, it appears that many parents in both clinics might have checked responses to questions that they believed were the “correct” or expected answers, rather than those that were accurate. Comments made during the clinical exams – as well as the clinical presentation of the patients and clinical findings – did not always align with questionnaire responses. This raises serious concerns about the validity of many of the survey responses.
One last confounder is related to the expectations of the dental clinic at LCHC regarding level of patient need on the island. During initial screening exams at the local school on Lanai, it appeared to many of the pediatric dentists that a significant portion of the children had limited dental needs and/or had already received dental care for restorative needs elsewhere (e.g.: off island by dentists on Maui, Oahu, etc.). This led us to believe that the population we would encounter at LCHC would have a low DMFT score overall. However, when the clinic first opened the majority of the initial pediatric encounters were those patients who had more acute dental needs; these were patients who had not seen a dentist in many years and therefore had high caries risks and scored much high on the DMFT scale. As a result, the data may have been skewed toward a higher prevalence of DMFT; the initial patients who were seen at LCHC during data collection for this survey may not have been representative of the general pediatric population on the island.
There is much useful information to be gained from a study of this kind. More long-term studies are needed to be better understand the risk factors and oral hygiene practices of children in the state of Hawaii, particularly those on the outer islands who may have more difficulty accessing oral health care services and oral hygiene education. It would be beneficial to modify the questionnaire and possibly administer it face-to-face with an examiner for clarification. It would also be advantageous to have more licensed dental examiners available who can conduct the study over a longer period of time to allow for a greater number of participants and a better picture of both populations.
References
- United States Census Bureau. State and County QuickFacts: Hawaii. 2014.
- Hawaii State Department of Business, Economic Development & Tourism. Hawaii Population Characteristics 2014. 2014.
- Kehaulani Goo, S. After 200 years, Native Hawaiians make a comeback. 2015.
- The Pew Charitable Trust. Pew Study Shows Little Progress on Proven Oral Health Strategy. 2015.
- Hawaii State Department of Health. Hawaii Oral Health: Key Findings. 2015.
- American Academy of Pediatric Dentistry. Policy on Early Childhood Caries (ECC): Classifications, Consequences, and Preventive Strategies. AAPD Reference Manual. 2013; 35: 50-52.
- Weintraub JA, Prakash P, Shain SG, Laccabue M, & Gansky SA. Mothers’ Caries Risk Increases Odds of Children’s Caries. J Dent Res. 2010; 89: 954- 958.
- Association of State and Territorial Dental Directors. Basic Screening Surveys: an approach to monitoring community oral health. 2008.
- Moimaz SA, Fadel CB, Lolli LF, Garbin CA, Garbin AJ, Saliba NA. Social aspects of dental caries in the context of mother-child pairs. J Appl Oral Sci. 2013; 22: 73-88.
- American Academy of Pediatric Dentistry. Guidelines on Caries-risk Assessment and Management for Infants, Children and Adolescents. AAPD Reference Manual. 2014; 36: 127-134.
- American Academy of Pediatric Dentistry. Guidelines on Infant Oral Health Care. AAPD Reference Manual. 2014: 36: 141-145.
- de Souza PM, Mello Proenca MA, Franco MM, Rodrigues VP. m Costa JF, Costa EL. Association between early childhood caries and maternal caries status: A cross-sectional study in Sao Luis, Maranhao, Brazil. Eur J Dent. 2015; 9: 122-126.
- Folayan M, Kolawole K, Oziegbe E, Ovedele T, Oshomoji O, Chukwumah N, et al. Prevalence, and early childhood caries risk indicators in preschool children in suburban Nigeria. BMC Oral Health. 2015; 15: 72.
- Jain M, Namdev R, Bodh M, Dutta S, Singhal P, Kumar A. Social and Behavioral Determinants for Early Childhood Caries among Preschool Children in India. J Dent Res Dent Clin Dent Prospects. 2015; 9: 115-120.
- Nakayama Y, Mori M. Association between nocturnal breastfeeding and snacking habits and the risk of early childhood caries in 18- to 23-month-old Japanese children. J Epidemiol. 2015; 25: 142-147.
- Olatosi O, Inem V, Sofola O, Prakash P, Sote E. The prevalence of early childhood caries and its associated risk factors among preschool children referred to a tertiary care institution. Niger J Clin Pract. 2015; 18: 493-501.
- Perera PJ, Fernando MP, Warnakulasooriya TD, Ranathungs N. Effect of feeding practices on dental caries among preschool children: a hospital based analytical cross sectional study. Asia Pac J Clin Nutr. 2014; 23: 272-277.
- Prakash P, Subramaniam P, Durgesh B, & Konde S. Prevalence of early childhood caries and associated risk factors in preschool children of urban Bangalore, India: A cross-sectional study. Eur J Dent. 2012; 6: 141-152.
- Ramos-Gomez F, Crall J, Gansky S, Slayton R, Featherstone JDB. Caries risk assessment appropriate for age 1 dental visit (infants and toddlers). J Calif Dent Assoc. 2007; 35: 687-702.
- Borges HC, Garbin CA., Saliba O, Saliba NA, Moimaz SA. Socio-behavioral factors influence prevalence and severity of dental caries in children with primary dentition. Brazilian Oral Research. 2012; 26: 564-570.
- World Health Organization. Oral health surveys: basic methods. 4th ed. Geneva. 1997.
- American Academy of Pediatric Dentistry. Pediatric Medical History. AAPD Reference Manual. 2011; 35: 14-15.
- Stephen A, Krishnan R, Ramesh M, Kumar VS. Prevalence of early childhood caries and its risk factors in 18-72 month old children in Salem, Tamil Nadu. J Int Soc Prev Community Dent. 2015; 5: 95-102.
- Chong MJ, Kim Seow W, Purdie DM., Cheng E. & Wan V. Visual-tactile Examination Compared With Conventional Radiography, Digital Radiography, and Diagnodent in the Diagnosis of Occlusal Occult Caries in Extracted Premolars. Pediatr Dent. 2003; 25: 341-347.
- World Health Organization. Standardization of Reporting of Dental Diseases and Conditions: report of an expert committee on dental health. 1962.
- Beauchamp J, Caufield PW, Crall JJ, Donly K, Feigal R., Gooch B, et al. Evidence-Based Clinical Recommendations for the Use of Pit-and-Fissure Sealants: A Report of the American Dental Association Council on Scientific Affairs. J Am Dent Assoc. 2008; 139: 257-268.
- Casamassimo PS, Fields Jr, HW, McTigue DJ, Nowak AJ. Pediatric Dentistry: Infancy through Adolescence. St. Louis, MO: Elsevier Saunders. 2013.
- Skillman SM, Doescher MP, Mouradian WE, Brunson DK. The challenge to delivering oral health services in rural America. J Public Health Dent. 2010; 70: S49–57.