
Case Report
Austin J Dermatolog. 2015; 2(2): 1041.
Birt-Hogg-Dube Syndrome Masked by Neurofibromatosis Type 1: A Co-Occurrence with Overlapping Skin Findings
Ashraf MA1, Notaro ER2, Tavakkol Z3, Virgin J4, and Vary JC5*
1Department of Anesthesiology, University of North Carolina, USA
2School of Medicine, University of Washington, USA
3The Everett Clinic, USA
4Pathology and Laboratory Medicine, Veterans Affairs Puget Sound Health Care System, USA
5Division of Dermatology, University of Washington, USA
*Corresponding author: Jay C. Vary, Division of Dermatology, University of Washington, USA
Received: July 10, 2015; Accepted: December 15, 2015; Published: December 17, 2015
Abstract
We describe here in a case in which a man with known Neurofibromatosis 1 (NF1) was found to also have Birt-Hogg-Dube Syndrome (BHDS), due to likely independent mutations both on chromosome 17. A 75 year-old non-smoking man with a history of NF1 presented with chest pain. CT angiogram revealed multiple, medial-basilar pulmonary cysts of varying sizes suspicious for BHDS. This patient had a longstanding history of NF1 with multiple biopsy-confirmed cutaneous neurofibromas on the face and trunk and a family history of NF1. The lung findings in conjunction with biopsy-confirmed fibrofolliculoma and genetic testing confirmed BHDS. Aside from the coincidental intersection of two unique skin genodermatoses in one person, this case illustrates how the presence of one genodermatosis made the other phenotype less recognizable.
Keywords: Neurofibromatosis; Fibrofolliculoma; Genodermatosis
Abbreviations/Acronyms
BHDS – Birt-Hogg-Dube syndrome; NF1 – Neurofibromatosis type 1; FLCN – Folliculin
Introduction
Birt-Hogg-Dube Syndrome (BHDS) is a genodermatosis of unknown incidence characterized by skin fibrofolliculomas, trichodiscomas, and acrochordons as well as pulmonary cysts, spontaneous Pneumothorax and renal tumors. Skin findings appear as flesh-colored, dome-shaped papules on the face, neck and trunk [1]. BHDS is diagnosed by the presence of at least 5 facial or truncal papules with at least one histologically confirmed fibrofolliculoma [2].
Neurofibromatosis type 1 (NF1) is another genodermatosis affecting 1/3500 births, recognized clinically by several specific physical exam findings, many limited to the skin [3]. NF1 is diagnosed by the presence of two of the following features: six or more café-au-lait spots, intertriginous freckling, two or more cutaneous neurofibromas or one plexiform neurofibroma, an optic nerve glioma, characteristic bony lesion, iris Lisch nodule or a first degree relative with NF1[3].
We describe here in a case in which a man with known NF1 was found to also have BHDS, due to likely independent mutations both on chromosome 17. This case clearly illustrates how the presence of one genodermatosis made the other less recognizable.
Case Presentation
A 75 year-old non-smoking man with a history of NF1 presented with chest pain. A CT angiogram revealed multiple medial-basilar pulmonary cysts of varying sizes. The lung parenchyma between the cysts was normal. The portions of the kidneys that were visible appeared to be normal. The patient’s CT findings were highly suspicious for BHDS due to their characteristic appearance and have been separately reported by Rahbar, et al. [4].
This patient had a longstanding history of NF1 with numerous biopsy-confirmed cutaneous neurofibromas on the face and trunk and a family history of NF1 to establish the diagnosis.
In addition to neurofibromas, the patient’s skin examination revealed numerous flat-topped, skin-colored papules on the cheeks, nose, chin and forehead, which were longstanding and asymptomatic (Figure 1). A punch biopsy of a representative flat-topped papule from the face revealed changes most consistent with a fibrofolliculoma (Figure 2). Pedunculated papules in the axillae were clinically consistent with acrochordons.
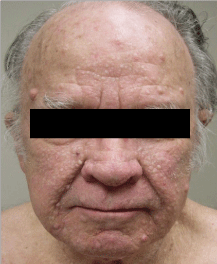
Figure 1: Skin-colored papules of NF1 on the temples and jaw line and those
of BHDS on the cheeks, nose, and chin
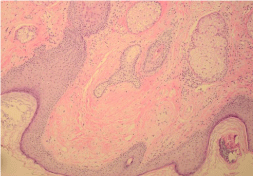
Figure 2: Pathology specimen from a facial papule showing changes of the
fibrofolliculoma/trichodiscomas spectrum of histology. 100 x magnification.
The lung findings in conjunction with biopsy-confirmed fibrofolliculoma supported a diagnosis of BHDS. Genetic testing showed positive heterozygous duplication of 28 nucleotides of the FLCN gene in exon 9, leading to a premature stop codon and predicted loss of normal function. This duplication has been previously published by Nickerson, et al. in another family with BHDS (family 228 in the reference) [5]. Surveillance renal ultrasound was performed at time of diagnosis and revealed kidneys of normal size and shape and a 16.6mm complex cyst in the lower pole of the right kidney which has remained stable on imaging for 10 years.
Discussion
BHDS is an autosomal dominant genodermatosis caused by germline or de novo mutations in the FLCN gene. FLCN encodes Folliculin, whose function is unknown but may act as a tumor suppressor. NF1 is also an autosomal dominant condition due to mutations in NF1, which encodes the putative tumor suppressor, neurofibromin [3]. The Folliculin and neurofibromin genes are both located on chromosome 17, nearly equidistant from the centromere at opposite ends of the chromosome (17q11.2 versus 17p11.2, respectively) [6,7].
Approximately 90% of NF1 cases are attributable to fully penetrant point mutations within the NF1 gene, which results in a truncated protein [6]. Several mutations can lead to a dysfunctional FLCN gene product, particularly slippage within exon 11 during DNA replication, a mechanism common to NF1 mutations as well [7]. However, a duplication was identified in exon 9 in this patient. It is most likely that two separate gene mutations in chromosome 17 caused this unique co-occurrence as opposed to a pericentromeric inversion.
Aside from the coincidental intersection of two unique skin genodermatoses in one person, the most clinically important aspect of this case is that the diagnosis was made difficult by phenotypically similar skin changes. The patient’s fibrofolliculomas on the face weren’t recognized until suspicion for BHDS was raised by the discovery of extracutaneous manifestations, as they were superimposed amongst the longstanding NF1-related neurofibromas.
Figure 1 demonstrates multiple cutaneous neurofibromas, recognized as skin-colored, pedunculated and sessile masses of various sizes on the forehead and jaw lines. Multiple fibrofolliculomas are also pictured in Figure 1, readily seen as whitish to flesh-colored domelike papules concentrated mostly within the central forehead and nasolabial folds. As NF1 may be marked by hundreds of neurofibromas with a range of appearances, these fibrofolliculomas were presumed to be early neurofibromas.
The dermatologic manifestations of BHDS can be subtle, particularly in the setting of another genodermatosis such as NF1. Given his longstanding history of NF1, one may surmise how the skin lesions of NF1 and BHDS on this patient’s face were not initially seen as two distinct processes. We report a unique co-occurrence in a patient meeting criteria for both disorders.
References
- López V, Jordá E, Monteagudo C. Birt-Hogg-Dube syndrome: an update. Actas Dermosifiliogr. 2012; 103: 198-206.
- Toro JR, Glenn G, Duray P. Birt-Hogg-Dube syndrome: a novel marker of kidney neoplasia. Arch Dermatol. 1999; 135: 1195-1202.
- Boyd KP, Korf BR, Theos A. Neurofibromatosis type 1. J Am Acad Dermatol. 2009; 61: 1-14.
- Rahbar H, Tavakkol Z, Bhargava P. Characteristic CT appearance of lung cysts prompting the diagnosis of a rare genodermatosis. Brit J Radiol. 2012; 85: 93-95.
- Nickerson ML, Warren MB, Toro JR. Mutations in a novel gene lead to kidney tumors, lung wall defects, and benign tumors of the hair follicle in patients with the Birt-Hogg-Dube syndrome. Cancer Cell. 2002; 2: 157-164.
- Abramowicz A, Gos M. Neurofibromin in neurofibromatosis type 1 - mutations in NF1gene as a cause of disease. Dev Period Med. 2014; 18: 297-306.
- Khoo SK, Giraud K, Kahnoski J. Clinical and genetic studies of Birt-Hogg-Dubé syndrome. J Med Genet 2002; 39: 906–912.