
Review Article
Ann Hematol Oncol. 2016; 3(10): 1117.
Umbilical Cord Blood Infusion in Addition to Immunosuppressive Therapy in a Patient with Relapsed and Refractory Severe Aplastic Anemia
Xiu L, Huina L, Bing X, Aibin L and Yi Ding*
Department of Hematology, Tongji University School of Medicine, China
*Corresponding author: Yi Ding, Department of Hematology, Tongji Hospital, Tongji University School of Medicine, Shanghai 200092, China
Received: September 07, 2016; Accepted: October 18, 2016; Published: October 21, 2016
Abstract
Background: Acquired severe aplastic anemia is a life-threatening bone marrow failure disorder characterized by pancytopenia and a hypocellular bone marrow. The optimal therapeutic strategies for SAA remain challenging in clinical settings. Here, we reported the use of umbilical cord blood infusion in a relapsed and refractory case of SAA.
Case Presentation: A 25 year-old patient was not able to receive allogenic hematopoietic stem cell transplantation from HLA identical sibling donors and was relapsed to common immunosuppressive therapy. We applied the IST plus UCBI remedy for this patient. Interestingly, the patient achieved not only complete recovery of hemopoietic function and hemogram indexes but also successful engraftment of stem cells into the bone marrow.
Conclusions: We suggest that IST plus UCBI may be a safe and effective remedy for patients with relapsed and refractory SAA.
Keywords: Severe aplastic anemia; Umbilical cord blood infusion; Immunosuppressive therapy
Introduction
Acquired Severe Aplastic Anemia (SAA) is one of the most serious and complicated hematological disorders [1]. For young SAA patients who are not able to receive allo-HSCT, combined Immunosuppressive Therapy (IST) is the first-line conditioning regimen [2-4]. However, still up to 20-40% of SAA patients can’t obtain hematologic remission from IST or resist to IST [5,6]. It remains challenging to optimize treatment for these refractory SAA patients [7-10]. Recently emerged evidences have demonstrated that Umbilical Cord Blood Infusion (UCBI) in addition to common IST remedy provide additional benefits in treating SAA [11]. Herein, we report the successful use of Umbilical Cord Blood (UCB) in a young patient with relapsed and refractory SAA.
Case Presentation
A 25 year-old female who presented with dizziness and fatigue over the prior 4 months was admitted to our department. Routine Blood Examination at admission as follows: erythrocytes (RBC) count was 1.1x1012/L, Hemoglobin (Hb) count was 3.8 g/dL, reticulocyte count was 11x109/L, White Blood Cell (WBC) count was 2600/mm3, neutrophils(ANC) count was 450/mm3, and platelets(PLT) count was 4x109/L. Subsequent bone marrow examination on January 28, 2014, demonstrated extremely reduced hematopoietic tissue, severely hypoplastic bone marrow and normal chromosome karyotyping in bone marrow cells. According to the acute onset, the normal chromosome karyotyping, and the results of bone marrow biopsy and peripheral hemogram, a diagnose of SAA type I was established.
The patient failed to undergo allo-HSCT as no siblings or fully matched HLA donors were available. She received oral cyclosporine (CsA, 5 mg/kg, q12h) treatment after diagnosis. The trough concentrations of CsA were maintained between 150 and 250 ng/ ml. Intermittent composition transfusions of red blood cells, platelets and subcutaneous injection of granulocyte colony stimulating factor(Lenograstim, 5 mg/kg) were administered. However, blood values did not noticeably recover after these measures.
Since February 11, 2014, the patient received combined IST. The conditioning regimen included continuous oral CsA and 2.5 mg/kg/ day ATG from day -5 to day -1 (Figure 1A). Blood counts began to recover on April 23, 2014, with erythrocytes 2.0x1012/L, Hemoglobin 7.1g/dL, reticulocytes 86x109/L, WBC 1900/mm3, neutrophils 700/mm3, and platelets 20x109L. Blood transfusion therapy was terminated accordingly. On May 7, 2014, the peripheral hemogram indexes showed the largest improvement with erythrocytes 2.1 x 1012/L, Hemoglobin 7.3 g/dL, reticulocytes 96.6x109L, white blood cell 2200/mm3, neutrophils 1800/mm3, and platelets 36x109L (Figure 2A, B and C).
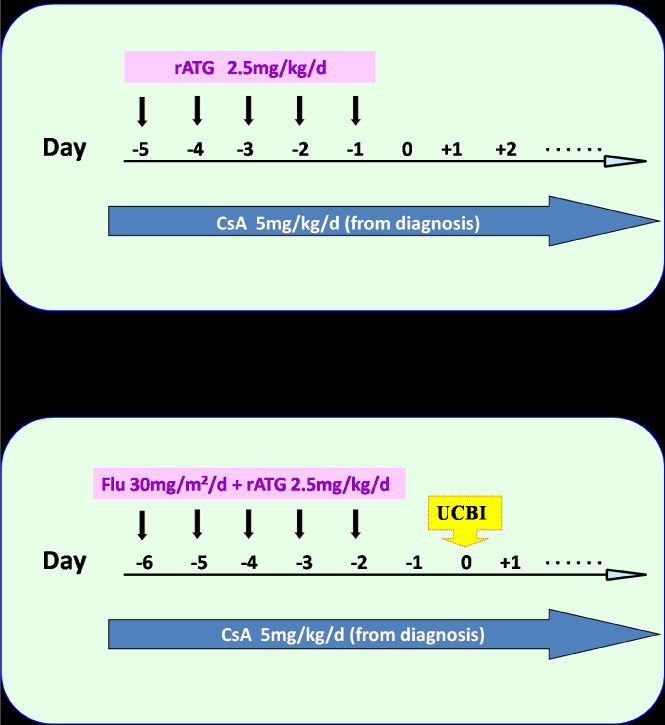
Figure 1: Overall survival, autologous stem cell transplant (ASCT) versus no ASCT (p=0.12).
The therapeutic efficacy was maintained for approximately 1 month, and thereafter, the peripheral hemogram declined to a level similar to that at the beginning of treatment (Figure 2A, B and C) due to an acute upper respiratory infection. Blood transfusion was restarted once again. A diagnosis of SAA relapse was established. According to our previous experience, we further attempted the combined therapy of IST plus Umbilical cord blood transfusion. The formula for IST was continuous oral CsA + 2.5 mg/kg/day ATG from day-6 to day-2 + 30 mg/m2/day fludarabine from day-6 to day- 2. Allogeneic 6/6 HLA-matched UCB was transfused on November 22, 2014 (day 0), and the total number of 1.49x107/kg nucleated cells (TNC) and 0.25 x 105/kg CD34 + cells were transfused.
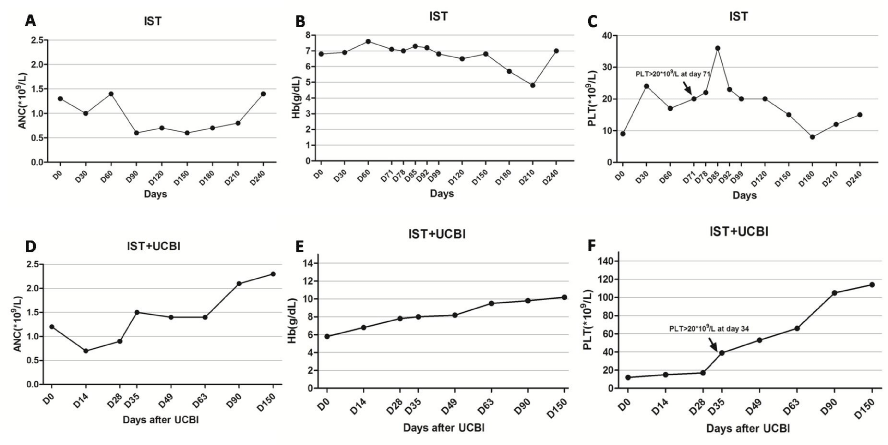
Figure 2: Overall survival, autologous stem cell transplant (ASCT) versus no ASCT (p=0.12).
After 1 month combination therapy of IST and UCBI, clinical symptoms were significantly improved. Blood counts began to rise on November 17, 2014, with erythrocytes 2.4 x 1012/L, Hb 7.8g/dL, WBC 3100/mm3, neutrophils 2200/mm3l, and platelets 21 x 109/L. Blood counts were normal until December 24 with erythrocytes 2.9 x 1012/L, Hb 9.8 g/dL, WBC 2400/mm3, neutrophils 1400/mm3, and platelets 112x109/L (Figure 2D, E and F), which indicated complete clinical remission. Blood ounts were maintained at normal levels thereafter.
Interestingly, the cord blood marrow chimerism increased continuously after UCBI (1 w 0%, 2 w 35%, 3 w 42%, 4 w 56%, 2 m 90% and 5 m 95%) (Figure 3), indicating that the majority of cord blood stem cells were effectively engrafted, and the hematopoietic function was greatly restored. Oral CsA (5 mg/kg, q12h) was continued after discharge. At the 5-month follow-up, the patient showed complete remission of clinical symptoms and normal blood counts. The dose of CsA was gradually reduced one year thereafter.
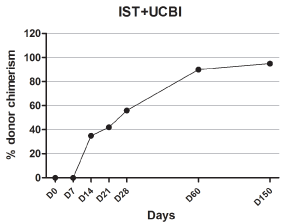
Figure 3: Overall survival, autologous stem cell transplant (ASCT) versus no ASCT (p=0.12).
Discussion
Aplastic Anemia (AA) is a serious clinical disorder characterized by bone marrow failure and peripheral pancytopenia [1]. SAA is the most life-threatening and complicated subtype of AA, which remains challenging in clinic [2,4]. For SAA patients <40-years-old, allo- HSCT from HLA identical sibling donors is the preferred treatment [3]. However, it is usually limited by a lack of donors and high cost of treatment in the clinic [12]. A large number of SAA patients have to undergo other treatments. ATG and CsA-based IST is the first-line conditioning regimen for SAA patients without a matched related donor [6,13]. Yet, up to 20-40% of SAA patients do not achieve hematologic remission from IST [5,14]. It is a challenge to optimize treatment for those who are not able to receive allo-HSCT and are refractory to IST [6,9].
This case was a 29-year-old female who was diagnosed with type-I SAA according to the clinical manifestations, the results of bone marrow biopsy and peripheral hemogram. According to the 2009 UK AA treatment guidelines, allo-HSCT from fully matched compatriots was of the first-line recommendation [3]. However, she was without HLA-matched donors and had to undergo IST instead. After 2.5 months of IST, the hemogram demonstrated a shortterm improvement, but declined thereafter and did not recover. A diagnosis of SAA relapse was established.
IST plus UCBI is a recently emerged therapeutic strategy for SAA patients, with a 70-80% reported efficacy and faster recovery of hematopoietic function [11,15]. Our center has applied this treatment regimen on many SAA patients since 2013, and has achieved profound clinical efficacy. According to our experience, we employed IST plus UCBI as a second round treatment for the patient. Hemogram indexes began to rise one month later and blood transfusion was terminated. Blood counts rose continuously and the platelet reached desired levels three months later. Five months thereafter, the patient exhibited normal hemogram with a CR grade of efficacy assessment, and a 90% chimerism in the bone marrow.
We suspect that the stem cells and hemopoietic stimulating factors in UCB might have restored hemopoietic function in this SAA patient [16,17]. In addition, multiple rounds of IST might have contributed to the easily engraftment of cord blood stem cells into bone marrow, which further stimulated hematopoiesis and contributed to final therapeutic efficacy. Because UCB is less immunogenic than peripheral blood, it does not increase the risk for patients after strict HLA matching. Moreover, because UCB is abundantly available, only six HLA loci are needed for matching, and 4/6 match meet the clinical requirements, UCBI therapy may better reach these clinical requirements.
In this case, we treated a SAA patient refractory to IST with a combination regimen of IST and UCBI. The patient obtained complete recovery of hematopoietic function and successful implantation of stem cells from UCB. We provide additional evidence that UCB may be an effective remedial therapy for those are unable to receive allo- HSCT and are refractory to IST.
References
- Kojima S, Frickhofen N, Deeg HJ, Okamoto S, Marsh J, Teramura M, et al. Aplastic anemia. Int J Hematol. 2005; 82: 408-411.
- Scheinberg P, Young NS. How I treat acquired aplastic anemia. Blood. 2012; 120: 1185-1196.
- Marsh JC, Ball SE, Cavenagh J, Darbyshire P, Dokal I, Gordon-Smith EC, et al. Guidelines for the diagnosis and management of aplastic anaemia. Br J Haematol. 2009; 147: 43-70.
- Miano M, Dufour C. The diagnosis and treatment of aplastic anemia: a review. Int J Hematol. 2015; 101: 527-535.
- Dufour C, Pillon M, Passweg J, Socie G, Bacigalupo A, Franceschetto G, et al. Outcomeof aplastic anemia in adolescence: a survey of the Severe Aplastic Anemia Working Party of the European Group for Blood and Marrow Transplantation. Haematologica. 2014; 99: 1574-1581.
- Peinemann F, Labeit AM. Stem cell transplantation of matched sibling donors compared with immunosuppressive therapy for acquired severe aplastic anaemia: a Cochrane systematic review. BMJ Open. 2014; 4: e005039.
- Fureder W, Valent P. Treatment of refractory or relapsed acquired aplastic anemia: review of established and experimental approaches. Leuk Lymphoma. 2011; 52: 1435-1445.
- Fu Y, Wang Q, Zhou J, Liu S, Fang B, Wei X, et al. Reduced intensity conditioning andco-transplantation of unrelated peripheral stem cells combined with umbilical cord mesenchymal stem/stroma cells for young patients with refractory severe aplastic anemia. Int J Hematol. 2013; 98: 658-663.
- Marsh JC, Kulasekararaj AG. Management of the refractory aplastic anemia patient: what are the options? Blood. 2013; 122: 3561-3567.
- Metcalf D. A promising new treatment for refractory aplastic anemia. N Engl J Med. 2012; 367: 74-75.
- Liu HL, Sun ZM, Geng LQ, Wang XB, Ding KY, Tang BI, et al. Unrelated cord blood transplantation for newly diagnosed patients with severe acquired aplastic anemia using a reduced-intensity conditioning: high graft rejection, but good survival. Bone Marrow Transplant. 2012; 47: 1186-1190.
- Dufour C, Pillon M, Socie G, Rovo A, Carraro E, Bacigalupo A, et al. Outcome of aplastic anaemia in children. A study by the severe aplastic anaemia and paediatric disease working parties of the European group blood and bone marrow transplant. Br J Haematol. 2015; 169: 565-573.
- Peinemann F, Bartel C, Grouven U. First-line allogeneic hematopoietic stem cell transplantation of HLA-matched sibling donors compared with first-line ciclosporin and/or antithymocyte or antilymphocyte globulin for acquired severe aplastic anemia. Cochrane Database Syst Rev. 2013; 7: CD006407.
- Jalaeikhoo H, Khajeh-Mehrizi A. Immunosuppressive therapy in patients with aplastic anemia: a single-center retrospective study. PLoS One. 2015; 10: e0126925.
- Li Y, Sheng Z, Niu S, Ge L, Ren C, Zou Y. Rapid and complete reconstitution of autologous haemopoiesis after cord blood infusion in treatment-naive patients with severe aplastic anemia receiving high-dose cyclophosphamide/ATG therapy. Eur J Haematol. 2013; 90: 45-50.
- Luan C, Chen R, Chen B, Ding J, Ni M. Umbilical cord blood transplantation supplemented with the infusion of mesenchymal stem cell for an adolescent patient with severe aplastic anemia: a case report and review of literature. Patient Prefer Adherence. 2015; 9: 759-765.
- Peffault de Latour R, Rocha V, Socie G. Cord blood transplantation in aplastic anemia. Bone Marrow Transplant. 2013; 48: 201-202.