
Clinical Image
Ann Hematol Oncol. 2017; 4(8): 1166.
Retroperitoneal Extramedullary Relapse after Blinatumomab in Acute Lymphoblastic Leukemia Failing a Haplo-Identical Bone Marrow Transplantation
Marano L¹, Venetucci P², Macera A², Beneduce G¹, Grimaldi F¹ and Risitano AM¹*
¹Hematology and BMT Unit, Department of Clinical Medicine and Surgery, Federico II University of Naples, Italy
²Interventional Radiology, Department of Advanced Biomedical Sciences, Federico II University of Naples, Italy
*Corresponding author: Antonio M. Risitano, Head of BMT Unit, Department of Clinical Medicine and Surgery, Federico II University of Naples, Via Pansini 5 80131 Naples, Italy
Received: July 03, 2017; Accepted: July 17, 2017; Published: August 04, 2017
Clinical Image
CT scan (Figure 1A) and fine-needle aspirate (Figure 1B) of retroperitoneal lesions in an acute B-cell lymphoblastic leukemia (B-ALL) patient treated with blinatumomab for post-transplant relapse. This 43 year old man has received allogeneic hematopoietic stem cell transplantation (HSCT) from a haplo-identical donor (according to the Genoa’s protocol exploiting high dose posttransplant cyclophosphamide); due to early hematological relapse he received further chemotherapy, followed by 4 courses of blinatumomab, achieving complete hematological response (including no detectable minimal residual disease [MRD] by flow cytometry). Due to the high risk of relapse, he then received two donor lymphocyte infusions (1x106/kg and 5x106/kg, with a 4 week interval). One week after the second DLI (while MRD became 0.06%), he developed grade II graft versus host disease (GvHD; skin II, liver I) with severe abdominal pain, raising the differential diagnosis between intestinal involvement of GvHD and other conditions. CT scans (Figure 1A) showed multiple intra and retro peritoneal soft tissue lesions some of which with a clear nodular appearance without any fluid collection. The white arrow indicates the retroperitoneal target lesion of FNAB. The fine-needle aspirate showed a solid tissue, which at the May-Grünwald-Giemsa staining appeared entirely formed by mid-size lymphoblasts (Figure 1B); immunophenotype was the same of initial diagnosis (including CD19 expression). The final diagnosis of extramedullary relapse was made, and the patient started a salvage treatment, which could not prevent disease progression and death.
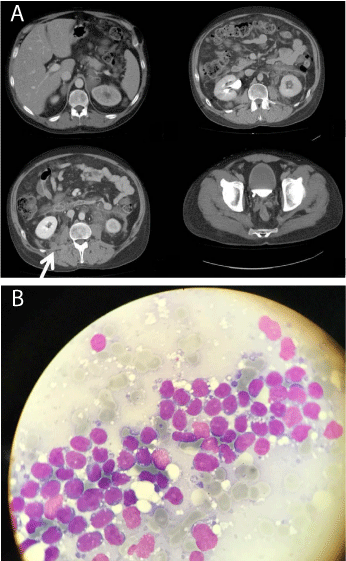
Figure 1:
The CD19/CD3 bispecific T-cell engager (BiTe) blinatumomabis an emerging treatment option for relapsed B-ALL [1] even after allogeneic HSCT. At our knowledge, isolated extramedullary relapses have not been described so far, and the concern of possible extrahematological disease has not been fully addressed in previous registration trials and subsequent follow up studies [1]. Since BiTes exert their activity through the recruitment of T-cells (usually autologous, or eventually allogeneic after HSCT), it seems conceivable that the control of extramedullary disease may be reduced exactly as with HSCT and graft versus leukemia. Our observation may serve as an alert to carefully consider atypical relapse presentation in B-ALL patients treated with blinatumomab, especially after HSCT.
Author Contribution
LM, GB, FG and AMR were in charge of the clinical management of the case; PV and AM performed the CT scan and the FNAB. LM and AMR prepared the figures and wrote the manuscript, which was critically reviewed by all the remaining authors.
References