
Case Report
Ann Hematol Oncol. 2018; 5(1): 1186.
Acute Lymphoblastic Leukaemia Presenting with Bone Marrow Necrosis
Chuan Ng¹*, Alessandri A¹, Bowen AC² and Ramachandran S¹
¹Department of Haematology-Oncology and Blood and Marrow Transplantation, Child and Adolescent Health Services, Princess Margaret Hospital, Australia
²Department of Infectious Diseases, Child and Adolescent Health Services, Princess Margaret Hospital for Children, Australia
*Corresponding author: Chuan Ng, Department of Haematology-Oncology and Blood and Marrow Transplantation, Child and Adolescent Health Services, Princess Margaret Hospital, Perth, Australia
Received: November 04, 2017; Accepted: January 10, 2018; Published: January 24, 2018
Keypoints
1. Cardinal features of bone marrow necrosis are bone pain and fever.
2. Bone marrow necrosis is a rare presentation of childhood ALL and does not confer an adverse prognostic factor.
3. Radiological findings of patients with Acute Lymphoblastic Leukaemia presenting with bone marrow necrosis are increased T2 hypertensity on MRI. The characteristic abnormal signal intensities are usually diffuse and extensive.
Case Presentation
Case 1
A previously healthy 15-year-oldfemale presented to the emergency department (ED) in June 2013 with a two month history of fever and pain in her right thigh and buttock. On examination, she was febrile at 39°C. She had tenderness at the right sacroiliac joint but full range of hip and knee joint movements. The remainder of her examination was unremarkable, in particular, no evidence of hepatosplenomegaly, petechiae or lymphadenopathy.
Her initial blood tests showed mild hypochromic, microcytic anaemia with a haemoglobin of 105 g/L (normal range: 110-145 g/L), normal white cell count 6.8 X 109/L (normal range: 5-17 X 109/L) and platelets 224 X 109/L (normal range: 150-400 X 109/L). Her inflammatory markers were markedly elevated, erythrocyte sedimentation rate (ESR) 82 mm/hr (normal <15 mm/hr) and C-reactive protein (CRP) 68 mg/L (normal <10 mg/L). Her liver function tests and lactate dehydrogenase (LDH) were normal. She also had a pelvic X- ray which did not reveal any abnormalities.
She was admitted under the orthopaedic team with a presumed chronic skeletal infection. Her bone scan showed irregular increased uptake at multiple sites including the right sacroiliac joint, right femur, multiple ribs and multiple areas within the thoracic spine. Chronic recurrent multifocal osteomyelitis (CRMO) was added to the differential diagnosis. Magnetic Resonance Imaging (MRI) showed multifocal areas of T2 hyperintensity in the right ilium, right ischial tuberosity, right intertrochanteric region, right and left sacral alae and left posterior acetabulum suggestive of osteonecrosis or infection. Diffuse abnormal marrow signal with symmetric areas of sparing in the proximal femoral regions were in keeping with extensive red marrow conversion on the MRI.
She was treated for chronic multifocal osteomyelitis with intravenous antibiotics for 1 week without improvement. She subsequently underwent bilateral iliac biopsies for bone marrow aspirate and trephine. The bone marrow aspirates were very difficult to obtain and while there was an obvious abnormal infiltrate, the flow cytometry sample was too diluted to yield any reliable results. The trephine biopsy revealed complete replacement of the bone marrow with a neoplastic cell infiltrate. The immunohistochemical stains confirmed the neoplastic cells were in keeping with precursor-B cell Acute Lymphoblastic Leukaemia (ALL). A further bone marrow sample identified the poor prognosis iAMP 21 abnormality in her leukaemic cells. She had complete resolution of her symptoms of pain and fever once chemotherapy was commenced for high-risk ALL.
She completed all chemotherapy in October 2015 and on follow up remains in remission.
Case 2
A previously well 6-year-old boy presented to the ED in January 2015 with a 9-day history of back pain associated with lethargy, anorexia, abdominal pain and intermittent low-grade fever. He had generalised abdominal tenderness without hepatosplenomegaly and mildly increased work of breathing. His chest was clear on auscultation.
Inflammatory markers and LDH were elevated: CRP 45 mg/L, ESR 55 mm/hrand LDH of 1970 U/L (normal range: 470-900 U/L) respectively with a normal full blood count. MRI spine showed an abnormal, diffuse T2 hyperintensity with enhancement of the C6 vertebral body and the L2 spinous process. Skeletal infection and CRMO were considered. He was commenced on intravenous antibiotics with analgesia without resolution of pain or fever. Repeat MRI spine performed one week later showed progression of T2 hyperintensity throughout his spine and both ilia. A CT-guided biopsy of the T2 spinal lesion was performed. No obvious malignant infiltrate or atypical lymphoid population were seen. Histopathology confirmed features consistent with osteomyelitis with a necrotising component.
Despitebroad-spectrumantimicrobials, his symptoms progressed with rising inflammatory markers. A third MRI spine at one month since his initial presentation showed an extensive osseous involvement with central necrosis throughout the cervical, thoracic, lumbar and sacral spine, bony pelvis, proximal right femur, right shoulder girdle, humerus and right sided ribs. A second CT guided bone biopsy and a bilateral bone marrow examination were performed. The bone biopsy samples were insufficient for histopathological examination. The bone marrow examination confirmed a diagnosis of precursor-B cell ALL. At this point, his repeat full blood count showed mild microcytic, hypochromicanaemia with a Hb of 79 g/L, WCC of 5.7 X 109/L (ANC 0.02, lymphocytes 2.94, monocyte 0.23) and platelet count of 245 X 109/L. Notably, there were no peripheral circulating blasts.
Symptom resolution promptly followed commencement of chemotherapy.
He had a morphological remission andhis minimal residual disease (MRD) at the end of induction phase by flow cytometry was <0.1%. His repeat MRI spine, pelvis and right humerus at the end of consolidation phase of therapy showed general improvement in multiple bone lesions.
He is currently receiving the maintenance phase of chemotherapy.
Discussion
Bone marrow necrosis (BMN) can be seen inneoplastic conditions such as ALL, metastatic malignancies such as neuroblastoma, and non-neoplastic conditions such as skeletal infection (septic arthritis and osteomyelitis) and inflammatory CRMO. Debilitating bone pain and fever are the hallmark features of BMN. It is paramount to exclude neoplastic causes in patients when these symptoms persist. A high index of suspicion is required, as BMN can be a rare presenting symptom of childhood ALL, and can often be confused with skeletal infection/inflammation which are more common.
Both of our patients were initially treated for presumed osteomyelitis without improvement. The diagnosis was complicated by the fact that the initial full blood picture, bone biopsies and bone marrow investigations were unable to detect any malignant cells. Once a diagnosis of ALL was confirmed in both patients, antimicrobial treatment was ceased and symptoms resolved rapidly with the institution of appropriate chemotherapy.
Bone marrow necrosis (BMN) is characterised by necrosis of both medullary stroma and myeloid tissue components of the marrow space [1-4]. The exact pathophysiology of BMN is incompletely understood, but failure of microcirculation is thought to be the critical event. This microcirculation occlusion may be due to tumour emboli, tumour compression, and fibrin thrombi, or cytotoxic injury. Due to the relative rarity of BMN, there are only case reports of paediatric ALL presenting with BMN published in the literature. Nirmish R. Shah, et al. [1] reviewed all published reports of paediatric ALL with BMN described in the literature between 1965 and 2009 and summarised the clinical presentations, laboratory values, and outcomes. The cardinal features of BMN are bone pain (90%) and fever (75%), which were seen in both of our patients. The most common laboratory investigation abnormalities were anaemia (90%) and leucopaenia (68%), with 37% of patients presenting with pancytopaenia. All patients had raised LDH.
Radiological investigations were not included in the previously published review [1]. CT & MRI would not have been available in the earlier decades of the study and may have been of limited value in the later years. Certainly, such investigations were of limited diagnostic value in our patients at presentation. However it might be different in the future as the quality of imaging modalities such as MRI continues to improve. We do know that histologic examination of the marrow remains essential for the diagnosis of leukaemia. Radiologic changes in patients with ALL are more common in the younger age group. Rogalsky, et al. studied 107 patients with leukaemia presenting with orthopaedic manifestations; about 50% of patients had abnormal radiologic findings and 70-90% developed abnormalities during the course of treatment [5]. Similar bony lesions are seen in metastatic malignancies such as neuroblastoma, Ewing sarcoma, rhabdomyosarcoma, retinoblastoma and non-Hodgkin Lymphoma [5,6]. The radiologic findings can also be seen in non-neoplastic conditions such as osteomyelitis, Langerhans cell histiocytosis and brown tumour of hyperparathyroidism masking definitive diagnosis [7,8].
Tang, et al. highlighted MRI changes in BMN in 6 case reports and found that the unifying MRI feature in patients with BMN was the characteristic diffuse, extensive, and geographic pattern of signal abnormalities [9]. BMN is anatomically more extensive, diffusely involving the marrow of the spine and pelvis. There may be varying appearances of signal intensity in areas of BMN which may reflect different stages of this pathological process. In the earliest stage, T1 hyperintensity signify fatty infiltration. The next stage is T1 and T2 hyperintensity which is characteristic of blood and haemorrhage [10]. Furthermore, the lesions of BMN do not progress to vertebral body collapse. In our report, both patients had multiple areas of signal abnormalities of T2 hyperintensity which is strongly suggestive of abnormal bone marrow activity.
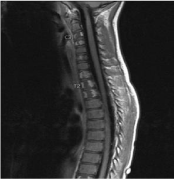
Figure 1: Sagittal view of MRI spine of case 2.
T2 hyperintensity and peripheral serpiginous enhancement involving C3-
C6, T1,T2,T3 and T11 vertebral bodies. Many of the lesions demonstrate
significant central necrosis.
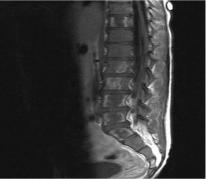
Figure 2: Sagittal view of MRI lumbar spine of case 2.
There is T2 hyperintensity which involves L2, L3, L4, L5, S1 and S4 vertebral
bodies.
Historically, BMN in patients with ALL was believed to be a poor prognostic factor. However, recent studies showed that outcome in acute lymphoblastic leukaemia is predominantly related to the biological features of the leukaemic cells and response to therapy measured by minimal residual disease (MRD) in the bone marrow either by flow cytometry (for aberrant immunophenotypes) and PCR amplification (for leukaemia-specific immunoglobulin and T-receptor genes or fusion transcripts) [11-13]. Macfarlene and Tauro reported 4 children with BMN and ALL, of whom 3 presenting in the 1970 are died, whereas the child presenting in 1982 remained in remission 40 months after diagnosis. They postulated that BMN might be a marker for other prognostic factors in ALL. However in subsequent studies BMN has not been proven to alter the long-term outcomes of patients with ALL. This finding is supported by the fact that both of our patients remain in remission.
In conclusion, in patients who present with bone pain and fever and have abnormal MRI changes suggestive of BMN, a more thorough investigation for malignant bone marrow diseases should be promptly considered. Delays in commencing chemotherapy can result in prolonged symptoms and the potential for adverse outcome. Albeit rare, BMN is a entity known to be associated with underlying malignancy and other non-malignant conditions. It can also occur after chemotherapy or at recurrence of disease. A high index of suspicion for malignant disease is of paramount importance especially in patients who do not respond to the usual antimicrobial therapy within a reasonable timeframe.
References
- Shah NR, Landi DB, Kreissman SG, Kulbachi E, Moran C. Presentation and outcomes for children with bone marrow necrosis and acute lymphoblastic leukaemia: a literature review. J Pediatric Hematology Oncology. 2011; 33: e316-e319.
- Pui CH, Stass S, Green A. Bone marrow necrosis in Children with malignant disease. Cancer. 1985; 56: 1522-1525.
- Susumu Inoue, Ranjan Monga, Nkechi Onwuzurike. Bone marrow necrosis as a presenting feature of childhood acute lymphoblastic leukaemia. Pediatric Blood Cancer. 2007; 49: 367-368.
- Nies BA, Kundel DW, Thomas LB, Freireich EJ. Leukopenia, bone pain, and bone necrosis in patients with acute leukemia: a clinicopathologic complex. Ann Intern Med. 1965; 62: 698-705.
- Rogalsky RJ, Black GB, Reed MH. Orthopedic manifestations of leukemia in children. J Bone Joint Surg Am. 1986; 68: 494-501.
- Watt I. Disorders of the lymphoreticular system. In: Sutton D, editor. Textbook of radiology and imaging. 5th Ed, New York, Churchill Livingstone Publishers, 1993; 196-198.
- Chapman S, Nakielry R. Bones. In: Chapman S, Nakielry, editors. Aids to radiological differential diagnosis, 3rd Ed. London, WB Saunders publisher, 1995: 22-23.
- Jassens AM, Offner FC, Van Hove WZ. Bone marrow necrosis. Cancer. 2000; 88: 1769-1780.
- Tang YM, Jeavons S, Stuckey S, Middleton H, Gill D. MRI features of bone marrow necrosis. AJR. 2007; 188: 509-514.
- Mitchell DG, Rao VM, Dalinka MK, Spritzer CE, Alavi A, Steinberg ME, et al. Femoral head avascular necrosis: correlation of MRI, radiographic staging, radionuclide imaging, and clinical findings. Radiology. 1987; 162: 709-715.
- Marion RR, Ethan SS, Athimalaipet VR. Chronic recurrent multifocal osteomyelitis in children and adults: current understanding and areas for development. Rheumatology. 2017.
- Campana D, Pui CH. Minimal residual disease-guided therapy in childhood acute lymphoblastic leukaemia. Blood. 2017; 129: 1913-1918.
- Inaba H, Greaves M, Mullighan CG. Acute lymphoblastic leukaemia. Lancet. 2013; 381: 1943-1955.