Case Report
Austin J Med Oncol. 2014;1(1): 3.
Appendiceal Mucocele Caused by Adenocarcinoma in Ulcerative Colitis
Nishikawa T1*, Yokoyama T2, Tanaka T1, Tanaka J1, Kiyomatsu T1, Kawai K1, Hata K1, Kazama S1, Nozawa H1, Yamaguchi H1, Ishihara S1, Sunami E1 and Watanabe T1
1Department of Surgical Oncology, the University of Tokyo, Tokyo, Japan
2Yokoyama hospital for gastroenterological diseases, Aichi, Japan
*Corresponding author: Nishikawa T, Department of Surgical Oncology, the University of Tokyo, 7-3-1 Hongo Bunkyo-ku, Tokyo, 113-8655, Japan
Received: August 11, 2014; Accepted: September 27, 2014; Published: September 29, 2014
Abstract
Ulcerative colitis (UC) is a chronic inflammatory bowel disease associated with an increased risk of colorectal cancer. We report a case of adenocarcinoma of the appendix, not detectable although of meticulous colonoscopy performed by an experienced colonoscopist, but diagnosed by the complementary examination of the patient with UC. The case was a 44-year old man with a 21- year history of UC (pancolitis), who was followed in another specialized service, and was introduced to our service because of increased serum carbohydrate antigen 19-9 (CA19-9). The finding of the surveillance colonoscopy was compatible with UC in remission, including the orifice of the appendix. However, the positron emission tomography / computed tomography revealed an appendiceal mucocele of 80 mm diameter and 18-fluorodeoxyglucose uptake in the middle portion of appendix. Based on these findings, malignant tumor of the appendix was suspected, and the laparoscopic appendectomy was indicated as a minimally invasive diagnostic procedure. Histopathological examination revealed adenocarcinoma with mucinous component beyond the serosa in the middle portion of the appendix. This case strongly suggested the need of careful surveillance of patients with UC involving the whole body of appendix to avoid missing malignant tumors, which, although a rare condition, may be of higher risk in patients with pancolitis type of UC.
Keywords: Inflammatory bowel disease; Ulcerative colitis; Appendiceal adenocarcinoma; Appendiceal mucocele
Abbreviations
UC: Ulcerative Colitis; IBD: Inflammatory Bowel Disease; CRC: Colorectal Cancer; AM: Appendiceal Mucocele; CT: Computed Tomography; PET: Positron Emission Tomography; 18-FDG: 18-Fluorodeoxyglucose
Introduction
Ulcerative colitis (UC) is a chronic inflammatory bowel disease (IBD) associated with an increased risk of colorectal cancer (CRC). However, UC-associated early CRC may be missed during colonoscopy, even by experienced colonoscopists, dependent on the flat and unclear border between cancer and the mucosal inflammatory changes caused by the disease. Therefore, surveillance colonoscopy with multiple biopsies is recommended for the early detection of dysplasia or cancer within the mucosal changes caused by UC. The well-known risk factors for UC-associated CRC are the duration and extent of disease. In surveillance colonoscopy, biopsy specimens should be taken every 10 cm in 4 quadrants and additional biopsies should be taken of strictures and mass lesions other than pseudopolyps. Recently, targeted biopsy, high-magnification chromoscopic colonoscopy, NBI (narrow-band imaging) or AFI (autofluorescence imaging) is reported to be useful for the earlier diagnosis of dysplasia or cancer [1-5]. However, it is difficult to diagnose the dysplasia or cancer of the vermiform appendix not involving its orifice. Appendiceal involvement in UC has been documented in more than half of patients with pancolitis [6]. Therefore, the appendix, which is an organ both derived from the cecum and composed of similar colonic-type epithelium, may also be at risk of neoplastic transformation when affected in UC [6]. Here, we report a case of adenocarcinoma of appendiceal mucocele (AM) in a patient with a long-term history of UC, in whom the surveillance colonoscopy revealed no cancer at the orifice of the appendix or other portions of the colon.
Case Report
The case was a 44-year old man with a 21-year history of UC (pancolitis), who was followed at another specialized service, and was introduced to our hospital because of increased serum carbohydrate antigen 19-9 (CA19-9, 152.5U/ml) at the general checkup examination. Clinical remission of the UC had been maintained by treatment with 2g oral intake of Salazosulfapyridine daily for more than 5 years. Physical examination of the abdomen revealed no palpable mass or localized tenderness. Laboratory data showed no inflammatory reaction. The finding of surveillance colonoscopy was compatible with UC in remission, including the orifice of the appendix and showed no inflammation at the orifice of the appendix (Figure 1). Abdominal computed tomography (CT) revealed an AM of 80 mm diameter and positron emission tomography (PET) / CT revealed 18-fluorodeoxyglucose (18-FDG) uptake in the middle portion of the appendix, but not in the compartment of mucocele (Figure 2). Based on these findings, the patient was highly suspected as neoplasm of appendiceal mucocele, and the diagnostic / therapeutic laparotomy was planned. Adequate information concerning the risks and the benefits of the different kinds of therapeutic modalities was given, the patient chose the laparoscopic appendectomy, as the minimally invasive diagnostic procedure. By laparoscopy, an enlarged appendix (approximately 85 x 40 mm in size) was observed. The macroscopic findings revealed thickness of the wall in the middle portion of the appendix and mucocele in the distal end (Figure 3A). Microscopic examination revealed adenocarcinoma with mucinous component beyond the serosa in the middle portion of the appendix, which was the probable cause of mucocele of the distal portion (Figure 3B). Based on the histopathological diagnosis, right hemicolectomy was performed and histopathological examination revealed three periappendiceal lymph nodes involved with adenocarcinoma. The patient’s postoperative course was uneventful.
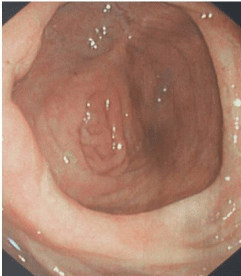
Figure 1: Remission status was observed, including the orifice of appendix at surveillance colonoscopy.
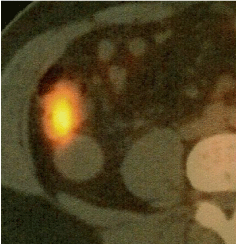
Figure 2: PET revealed 18-FDG uptake in the middle of appendix, not in the compartment of mucocele.
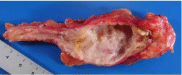
Figure 3A: Macroscopic findings showed thickness of the wall in the middle of the appendix and mucocele in the distal end.
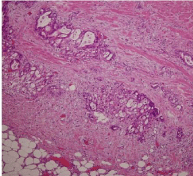
Figure 3B: Histopathological findings revealed adenocarcinoma with mucinous component beyond serosa in the middle of appendix.
Discussion
Expert opinion panels often recommend that the appendix may be a priming site in the development of UC [7], as evidenced by the fact that patients with UC have lower prevalence of appendectomy compared to those with Crohn’s disease or colonic carcinoma. More than half of patients with pancolitis UC have involvement of the appendix [6]. Previously, adenocarcinoma of the appendix involved with chronic UC has been reported [6,8], but the evident association between appendiceal cancer and UC could not be demonstrated because dysplasia was not detected in the colonic mucosa, leading them to speculate that both are unrelated diseases [8]. And, based on these facts, it has been suggested that the surveillance program for the early detection of cancer of the appendix in patients with long-standing UC is not mandatory [8]. In a recently conducted case-control study, Orta L et al. [9] demonstrated that the incidence of appendiceal cystadenomas was not significantly different between IBD cases and non-IBD controls, but appendiceal cystadenomas were 15-fold more prevalent among IBD cases with synchronous colorectal neoplasia compared with controls. And Matsushita et al. [10] analyzed the results of that study and recognized that cystadenomas were more prevalent among patients with UC, compared with patients with Crohn’s disease. Taking these facts together, that are, the lower prevalence of appendectomy, the higher prevalence of appendiceal cystadenomas, and the higher appendiceal involvement in patients with UC, in addition to the various reported cases of adenocarcinoma of the appendix in patients with UC, we can speculate that the prevalence of appendiceal neoplasms may be quite higher in UC patients compared with patient’s with Crohn’s disease or non-IBD individuals. And we must be carefully checked the appendix during the surveillance examination.
AM is a rare entity, with the incidence of 0.2-0.4 % among the cases receiving appendectomy [11]. Also the detection of AM in patients with UC has been reported [12,13]. AM is the progressive dilatation of the vermiform appendix caused by the intraluminal accumulation of the mucoid substance. Two major pathologic mechanisms are considered to be responsible for the formation of an AM: Elevated appendiceal pressure due to luminal obstruction caused by 1) prior inflammation, mucosal hyperplasia, or appendiceal lesions such as endometriosis or fecaliths; and 2) appendiceal tumors (i.e., carcinoid, cystadenoma, cystadenocarcinoma) (12). Preoperative diagnosis is important for the decision on the surgical procedure (appendectomy or colectomy), since the unintended rupture of the tumor during surgery must be avoided to prevent the development of pseudomyxoma perionei. Although the diagnosis may be difficult by the imaging studies (up to 60 % of the cases may be only diagnosed during operations for some other disease) [13], abdominal sonography and computed tomography seem to be of some value [11,14]. Surgical resection is the preferred treatment modality in the management of AM. Although open surgery was the most indicated, laparoscopic resection of AM was also reported [15]. However, in case of laparoscopic resection, there is the risk of rupture of the appendix, dependent on the manipulations such as the grasping of the organs with instruments, or during the evisceration through the small abdominal wall incisions, which may result in severe complications such as pneumoperitoneum, bacterial pneumonitis, or the peritoneal dissemination of the appendiceal mucinous tumor. Therefore, the careful manipulation of surgical instruments as well as of the tumor itself should be considered during the laparoscopic surgery. The prognosis of cystoadenocarcinomas without peritoneal or adjacent organ involvement is essentially good after surgical resection, but when pseudomyxoma peritonei develops, the 5-year survival rate drops to 25 %, most of the deaths being attributed to intestinal obstruction or renal failure [16].
In the present case, although the clinical remission of UC had been maintained, the noticeable increase of tumor marker was observed, and the PET / CT imaging successfully detected the appendiceal adenocarcinoma in the middle of appendix. While serum CA19-9 is one of the most widely applied markers in gastrointestinal malignancy, e.g. CRC, benign conditions also may cause CA 19-9 elevation. Thus, although it does not provide a definitive diagnosis of CRC, it may help suspecting the condition. In the present case, PET / CT followed increase of serum CA19-9 led us to suspect of an adenocarcinoma in the appendix causing AM in UC patient. Recent literature demonstrated that PET may be a sensitive tool for evaluating the inflammation in the UC regardless of cancer [17]. PET can also detect inflammatory activity in the colon despite negative colonoscopic, histologic and symptom assessment [17]. However, PET is an expensive examination, and also the accurate evaluation is necessary to determine whether 18-FDG uptake was due to tumor or inflammation, especially in the remission period of the UC.
The present case was a patient with a long-term history of UC, in whom the surveillance colonoscopy revealed no alterations of the colonic mucosa, including the orifice of the appendix, however, an adenocarcinoma of AM was fortuitously detected by the meticulous follow-up by other complementary tests, including serological tumor markers. Although not a frequent complication, appendiceal adenocarcinoma must be kept in mind during the surveillance of UC patients, even when the colonoscopic examination, performed by an expert colonoscopist, reveals no alterations of the colonic mucosa. In case abnormality is found in any of the serological tests, a more expensive yet sensitive tool such as PET/CT should be considered for the early detection of CRC.
In conclusion, this case strongly suggested the need of careful surveillance of patients with UC involving the whole body of the vermiform appendix to avoid missing malignant tumors of the appendix, which although a rare condition, may be at higher risk in UC patients, especially those of pancolitis type.
References
- Hurlstone DP, Sanders DS, Lobo AJ, McAlindon ME, Cross SS. Indigo carmine-assisted high-magnification chromoscopic colonoscopy for the detection and characterization of intraepithelial neoplasia in ulcerative colitis: A prospective evaluation. Endoscopy 2005; 37: 1186-1192.
- Rutter MD, Saunders BP, Schofield G, Forbes A, Price AB, et al. Pancolonic indigo carmine dye spraying for the detection of dysplasia in ulcerative colitis. Gut 2004; 53: 256-260.
- Kiesslich R, Goetz M, Lammersdorf K, Schneider C, Burg J, et al. Chromoscopy-guided endomicroscopy increases the diagnostic yield of intraepithelial neoplasia in ulcerative colitis. Gastroenterology 2007; 132: 874-882.
- Dekker E, van den Broek FJ, Reitsma JB, Hardwick JC, Offerhaus GJ, et al. Narrow-band imaging compared with conventional colonoscopy for the detection of dysplasia in patients with longstanding ulcerative colitis. Endoscopy 2007; 39: 216-221.
- Matsumoto T, Moriyama T, Yao T, Mibu R, Iida M. Autofluorescence imaging colonoscopy for the diagnosis of dysplasia in ulcerative colitis. Inflamm Bowel Dis 2007; 13: 640-641.
- Odze RD, Medline P, Cohen Z. Adenocarcinoma arising in an appendix involved with chronic ulcerative colitis. Am J Gastroenterol. 1997; 89: 1905-1907.
- Matsushita M, Uchida K, Okazaki K. Role of the appendix in the pathogenesis of ulcerative colitis. Inflammopharmacology. 2007; 15: 154-157.
- Zannoni U, Masci C, Bazzocchi R, Gandolfo F, Pezzi A, et al. Cancer of the appendix in long-standing ulcerative colitis: a case report. Tumori. 1997; 83: 958-959.
- Orta L, Trindade AJ, Luo J, Harpaz N. Appendiceal Mucinous Cystadenoma is a Neoplastic Complication of IBD: Case-Control Study of Primary Appendiceal Neoplasms. Inflamm Bowel Dis. 2009; 15: 415-421.
- Matsushita M, Tanaka T, Omiya M, Okazaki K. Significant association of the appendiceal neoplasms and ulcerative colitis rather than Crohn’s disease. Inflamm Bowel Dis. 2010; 16: 735.
- Caspi B, Cassif E, Auslender R, Herman A, Hagay Z, et al. The onion skin sign: A specific sonographic marker of appendiceal mucocele. J Ultrasound Med. 2004; 23: 117-121.
- Takeda Y, Nakase H, Mikami S, Inoue T, Satou S, et al. Possible link between ulcerative colitis and in situ adenocarcinoma of an appendiceal mucocele: Importance of Inflammation in the appendiceal orifice related to UC. Inflamm Bowel Dis. 2008; 14: 873-874.
- Lakatos PL, Gyori G, Halasz J, Fuszek P, Papp J, et al. Mucocele of the appendix: An unusual cause of lower abdominal pain in a patient with ulcerative colitis. A case report and review of literature. World J Gastroenterol. 2005; 11: 457-459.
- Ghosh T, Chalmers A, Verbeke C, Saunders R, Everett SM. Appendiceal mucocele in ulcerative colitis. Endscopy 2010; 42: E105-E106.
- Behranwala KA, Agarwal T, El-Sharkawi D, Shorvon D, Chang A. Laparoscopic resection of mucinous cystadenoma of appendix: a careful decision. Surg Laparosc Endosc Percutan Tech. 2006; 15: 347-348.
- Ruiz-Tovar J, Teruel DG, Castiñeiras VM, Dehesa AS, Quindós PL, et al. Mucocele of the appendix. World J Surg. 2007; 31: 542-548.
- Rubin DT, Surma BL, Gavzy SJ, Schnell KM, Bunnag AP, et al. Positron emission tomography (PET) used to image subclinical inflammation associated with ulcerative colitis (UC) in remission. Inflamm Bowel Dis. 2009; 15: 750-755.