Case Report
Austin J Med Oncol. 2014;1(2): 2.
Primary Intracranial Leiomyosarcoma of the Cavernous Sinus: Case Report
Saito N*, Aoki K, Hirai N, Ishii M, Fujita S, Hiramoto Y, Iwama J, Tani M, Sato K, Nakayama H, Harashina J, Izukura H, Ito K, Kimura H, Sakurai T and Iwabuchi S
Department of Neurosurgery, Toho University Ohashi Medical Center, Japan
*Corresponding author: Saito N, Department of Neurosurgery, Toho University Ohashi Medical Center, 2-17-6, Ohashi, Meguro, Tokyo, Japan
Received: September 23, 2014; Accepted: November 01, 2014; Published: November 03, 2014
Abstract
Primary intracranial leiomyosarcoma is extremely rare. Herein, we describe a case of primary intracranial leiomyosarcoma of the cavernous sinus in which stereotaxic radiotherapy was effective. A 75-year-old woman presented with acute-onset left eye pain and ptosis of the left eyelid. MR images revealed a hypointense homogeneous lesion in the left cavernous sinus, which was subsequently diagnosed via biopsy as leiomyosarcoma. Stereotaxic radiation with a fractionated Cyberknife radiosurgery was conducted. Following the treatment, a marked reduction in the tumor size was observed. Thereafter, the patient had local recurrence and died after a course of 44 months. Primary intracranial leiomyosarcoma is extremely rare and the prognosis is relatively poor. Cyberknife radiosurgery may be a useful treatment for unresectable primary intracranial leiomyosarcoma.
Keywords: Intracranial leiomyosarcoma; Cyberknife; Cavernous sinus
Introduction
Primary intracranial leiomyosarcoma is extremely rare; most intracranial leiomyosarcomas are metastases from extracranial organs. The mesenchymal cells of the dura mater and brain blood vessels are known to be the intracranial sites of origin of this sarcoma. Recently, an increasing number of intracranial sarcomas have been reported in patients infected with HIV or the Epstein–Barr virus. Because primary intracranial leiomyosarcoma is often characterized by apparent attachment to the meninges or skull base, differentiation from meningioma by means of preoperative image analysis is difficult; therefore, immunohistological staining is useful for diagnosis. Postoperative radiotherapy or chemotherapy is administered in many cases; however, there is no standard treatment regimen for primary intracranial leiomyosarcoma and the prognosis is poor. Treatment of leiomyosarcoma depends on the site, and extent, of the tumor present, and is multidisciplinary. Historically, surgery has been the primary treatment strategy, with the objective being to obtain negative surgical margins. To maintain local control of the tumor, radiation therapy has also been used as an adjunct to surgical resection. In recent years, increasing evidence has supported the efficacy of stereotactic radio surgery for the treatment of brain tumors [1,2]. Herein, we describe a case of primary intracranial leiomyosarcoma of the cavernous sinus in which stereotaxic radiotherapy was effective.
Case Presentation
A 75-year-old woman who was being treated on an outpatient basis for a previous cerebral infarction with occlusion of the left internal carotid artery presented with acute-onset left eye pain and ptosis of the left eyelid. One month after the onset of these symptoms, she was hospitalized for comprehensive examination and treatment. On admission, her consciousness was clear, and anisocoria (left eye, 4 mm; right eye, 2.5 mm), ptosis of the left eyelid, and paralyses of the left abducens nerve were noted. Blood examination revealed no significant abnormality.
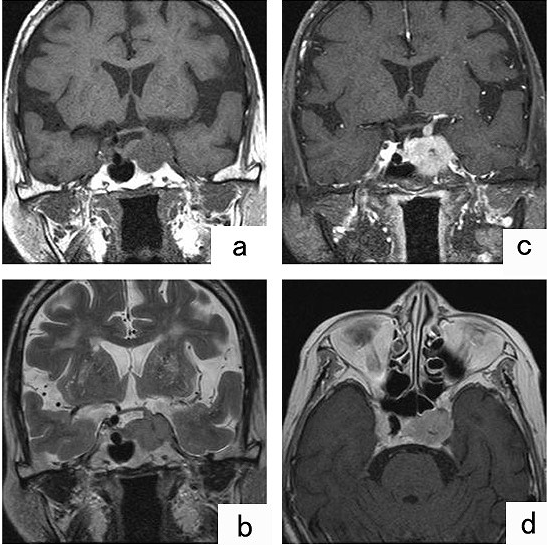
TI- and T2-weighted MR images of the head revealed a hypointense homogeneous region indicating a tumor in the area from the sellar region to the left cavernous sinus, with infiltration along the left internal carotid artery to the left middle cerebral artery (Figure 1). Metastatic malignant meningioma was tentatively diagnosed.
Figure 1: MRI showing TI-and T2-weighted MR images of the head revealed a hypointense homogeneous region (A and B). Gadolinium-enhanced MRI showed evidence of an enhanced lesion from the sellar region to the left cavernous sinus.
A biopsy was performed using a trans-sphenoidal approach. Pathological examination revealed complicated patterns of malignant spindle cells that were positive for vimentin and alpha-smooth muscle actin on immunostaining (Figure 2), indicating leiomyosarcoma. A subsequent general examination revealed no other primary lesion, and primary intracranial leiomyosarcoma of the left cavernous sinus was thus the conclusive diagnosis. Because of the difficulty of surgical excision, radiotherapy was selected. There is no standard treatment regimen for primary intracranial leiomyosarcoma, there are some report that Stereotaxic radiosurgery as a therapeutic strategy. We conducted stereotaxic radiation with a fractionated Cyberknife radiosurgery, 3Gy×5 days, to a total dose of 15 Gy. The treatment improved the patient’s symptoms and significantly reduced the size of the tumor (Figure 3). Thereafter, the patient had local recurrence and died after a course of 44 months.
Figure 2: Pathological features. Histopathological examination revealed complicated patterns of malignant spindle cells that were positive for alphasmooth muscle actin. (A: hematoxylin and eosin staining. B: SMA staining).
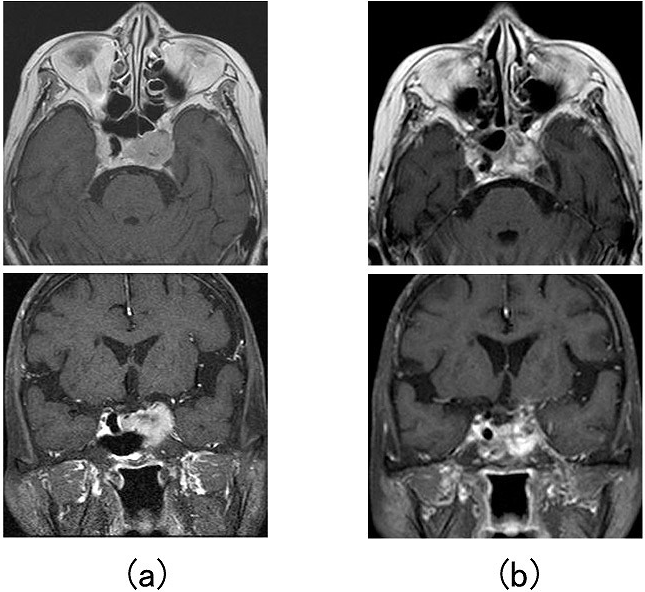
Figure 3: MRI showing (a) the tumor prior to CyberKnife radiotherapy and (b) the marked reduction in the tumour size following CyberKnife radiotherapy.
Discussion
Intracranial leiomyosarcoma is rare and is most likely to result in brain metastases, which are usually hematogenous [3]. A report on 3829 cases of intracranial soft-tissue sarcoma noted 19 cases of brain metastasis [4]. To the best of our knowledge, only 29 cases of primary intracranial sarcoma were reported to exhibit a high degree of differentiation of the smooth-muscle component. The origin was reported to be meninges and endothelial cells in vessels of the brain; this remains unclear at present [3,5,6]. In the present case, MR images revealed infiltration along the internal carotid artery, which suggests that the origin was indeed the endothelium of the vessel.
Primary intracranial leiomyosarcoma usually occurs in the cavernous sinus, cerebellopontine angle, the skull base or spine. On MR images, primary intracranial leiomyosarcoma is characterized by a lesion of strong contrast, a dural tail sign, and a dumbbell appearance. In many cases, however, it is diagnosed as a meningioma or neurilemoma [7]. MRI is the main imaging study for these lesions. Occasionally angiography to define vessel involvement or CT to evaluate bone destruction may be valuable. A thorough search for a primary sarcoma outside CNS is recommended [1,2].
A diagnosis of leiomyosarcoma is based on detection of smooth-muscle components confirmed by and immunohistological finding. In differential diagnosis, histopathological findings suggestive of leiomyosarcoma include complicated patterns of malignant spindled cells and rich cellular components. The spindle cells have longitudinally running acidophilic myofibrils in the cytoplasm and long, narrow heteromorphic nuclei. On immunostaining, the present case was positive for smooth muscle antigen and vimentin. On the basis of these findings, as well as those obtained from MRI findings and histopathology, and the fact that no extracranial primary lesion was found on general examination, primary intracranial leiomyosarcoma was the conclusive diagnosis for this case.
The prognosis for primary intracranial leiomyosarcoma is relatively poor: the longest period of survival was 32 months [8,9]. This is mainly due to the difficulty of surgical excision, and the difficulty of administering an adequate dose of radiation. In the present case, the primary lesion was present in the cavernous sinus, which is adjacent to the optic nerve. Stereotaxic radiation using a Cyberknife was conducted in 3 doses, for a total dose of 15 Gy. This therapy significantly reduced the size of the tumor and improved the patient’s symptoms. The advantage of this type of radiosurgery is unclear since the patient died 44 months after surgery, in patients, like ours, who are at a high risk for conventional radiation therapy, stereotaxic radiotherapy may be a useful treatment [1,2].
In conclusion, the present study reports the feasibility of Stereotaxic radiation using a Cyberknife for primary intracranial leiomyosarcoma. Our result indicates that this therapy may be a useful treatment for unresectable primary intracranial leiomyosarcoma.
References
- Zhang H, Dong L, Huang Y, Zhang B, Ma H, et al. Primary intracranial leiomyosarcoma: review of the literature and presentation of a case. Onkologie 2012; 35: 609-616.
- Alijani B, Yousefzade S, Aramnia A, Mesbah A. Primary intracranial leiomyosarcoma. Arch Iran Med 2013; 16: 606-607.
- Paulus W, Slowik F, Jellinger K, Primary intracranial sarcomas: histopathological features of 19 cases, Histopathology 1991; 18: 395–402.
- Haykal HA, Wang AM, Zamani A, Leiomyosarcoma metastatic to the brain: CT features and review, AJNR Am J Neuroradiol 1987; 8: 911–912.
- Lee TT, Page LK, Primary cerebral leiomyosarcoma, Clin Neurol Neurosurg 1997; 99: 210–212.
- Hussain S, Nanda A, Fowler M, Ampil FL, Burton GV. Primary intracranial leiomyosarcoma: report of a case and review of the literature. Sarcoma 2006: 52140.
- Lerdlum S, Lalitanantpong S, Numkarunarunrote N, Chaowanapanja P, Suankratay C, et al. MR imaging of CNS leiomyosarcoma in AIDS patients. J Med Assoc Thai 2004; 87: S152-S160.
- Espat NJ, Bilsky M, Lewis JJ, Leung D, Brennan MF, Soft tissue sarcoma brain metastases: prevalence in a cohort of 3829 patients, Cancer 2002; 94: 2706–2711.
- Louis DN, Richardson EP Jr, Dickersin GR, Petrucci DA, Rosenberg AE, et al. Primary intracranial leiomyosarcoma. Case report, J Neurosurg 1989; 71: 279–282.