
Case Report
Austin J Med Oncol. 2015;2(1): 1011.
Pure Ground Glass Opacity -Potential for Overdiagnosis?
Haseem Ashraf1, 2*, Gustav Peter Blom3, Espen Ruud1 and Arne Borthne1
1Centre for Diagnostic Imaging - Thoracic Section, Akershus University Hospital, Loerenskog, Norway
2Department of Respiratory Medicine, Gentofte University Hospital, Denmark
3Department of Pathology, Akershus University Hospital, Loerenskog, Norway
*Corresponding author: Haseem Ashraf, Centre for Diagnostic Imaging - Thoracic Section, Akershus University Hospital, Loerenskog, Norway
Received: October 31, 2014; Accepted: February 21, 2015; Published: February 23, 2015
Case Presentation
An active and healthy non-smoking 75 year old woman was referred to a regular chest x-ray because of unintentional weight loss over time. Chest x ray (Figure 1) showed diffuse consolidation in the right lower lobe, and the patient was referred to a Computerized Tomography (CT) scan of thorax (Figure 2) within the next month. CT scan showed a 15 x 13 mm indeterminate ground glass opacity lesion in the right lower lobe. Because of possible malignant outcome, the patient was referred to CT guided lung biopsy (Figure 3). Duringthe biopsy, the patient development a right sided pneumothorax which regressed after treatment with surgical tube.
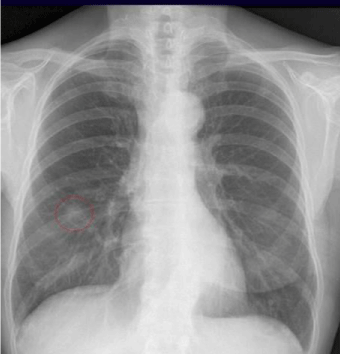
Figure 1: Initial chest x-ray showing diffuse consolidation (red ring).
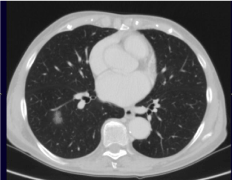
Figure 2: CT scan showing ground glass nodule in the right lower lobe.
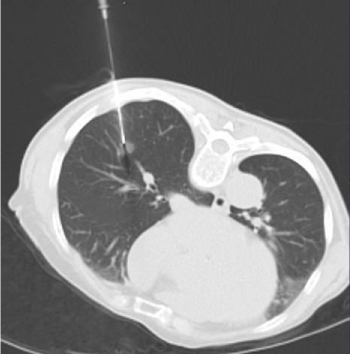
Figure 3: CT guided biopsy of right lower lobe nodule.
Histopathological diagnosis
Resected lower lobe (right) with adenocarcinoma in situ, nonmucinous. Centrally located lesion, 14 mm. Free resection margins. AJCC1/ UICC2 pathological stage: pTis. (in situ) (Figure 4 and Figure 5).
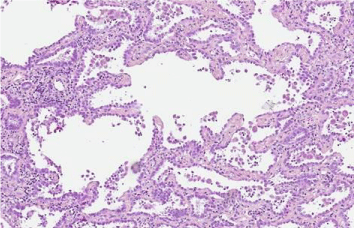
Figure 4: Histology from the peripheral part of the tumor. Low grade neoplastic
cells growing along pre-existing alveolar structures. (Haematoxylin/Eosin/
Safran x20).
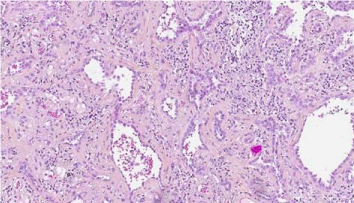
Figure 5: Histology from the central part of tumor. Neoplastic cells lining
alveoli with sclerosis and collaps of alveloar walls. No convincing invasive
growth. (Haematoxylin/Eosin/Safran x20)
Treatment
The patient received surgical treatment with right sided lower lobe thoracascopic lobectomy. The patient was hereafter follow-up with annual CT thorax scan.
Discussion
Ground glass opacity lesions often represent slow growing indeterminate lesions with malignant potential [1]. Some literature suggests that ground glass opacity lesions are associated with female sex [2]. The pathological classification of these lesions is still under debate[3]. We here refer to the new classification not yet incorporated in the WHO classification [4].
Ground glass opacity lesions have been described as a histological continuum from atypical adenomatous hyperplasia via adenocarcinoma in situ (bronchioloalveolar carcinoma) to adenocarcinoma with predominantly lepidic growth [5]. It is often difficult for the pathologist to differentiate between these diagnoses from a needle biopsy sample. Even from the resection specimen from this case there was still some uncertainty as to whether or not the lesion was invasive carcinoma. Longer follow-up of pure ground glass opacity lesions is recommended before conducting invasive diagnostic treatment [6]. Pure ground glass opacity < 5 mm require no follow-up; persisting ground glass nodule >5 mm are recommended annual follow for at least 3 years [7]. Positron emission tomography scan of pure ground glass opacity has limited value and may be misleading is therefore not recommended [7]. Solid transformation or rapid growth of pure ground glass opacity lesions are indicators of malignancy [8], in these cases biopsy or surgical resection should be considered.
Conclusions
The malignant potential of pure ground glass opacity lesions is still not well understood. Not all may ground glass nodules may develop into clinical significant malignant disease, and may therefore potentially represent overdiagnosis [9].
1American Joint Committee on Cancer
2Union for International Cancer Control
References
- Hasegawa M, Sone S, Takashima S. Growth rate of small lung cancers detected on mass CT screening.The British Journal of Radiology 2000;73:1252-1259.
- Tae JK, Jin MG, Kyung WL. Clinical, pathological and thin-section CT features of persistent multiple ground-glass opacity nodules: Comparison with solitary ground-glass opacity nodule. Lung Cancer 2009; 171-178.
- Jin N, Sloane PJ. Evaluation of pure ground glass pulmonary nodule: a case report. J Community Hosp Intern Med Perspect 2014; 4.
- Tumours of the lung - WHO Classification: https://www.iarc.fr/en/publications/pdfs-online/pat-gen/bb10/bb10-chap1.pdf.
- Travis WD, Brambilla E, Noguchi M, Nicholson AG, Geisinger K, et al. Diagnosis of lung adenocarcinoma in resected specimens: implications of the 2011 International Association for the Study of Lung Cancer/American Thoracic Society/European Respiratory Society classification. Arch Pathol Lab Med 2013; 137: 685-705.
- MacMahon H, Austin JH, Gamsu G, Herold CJ, Jett JR, et al.Guidelines for Management of Small Pulmonary Nodules Detected on CT Scans:A Statement from the Fleischner Society. Radiology 2005; 237:395-340.
- Masao N, Hideyuki S, Ichiro T. Focal Ground-Glass Opacity Detected by Low-Dose Helical CT. Chest 2002; 121; 1464-1467.
- Truong MT1, Ko JP, Rossi SE, Rossi I, Viswanathan C, et al. Update in the Evaluation of the Solitary Pulmonary Nodule. RadioGraphics 2014; 34:1658–1679.
- Goo JM, Park CM, Lee HJ. Ground-glass nodules on chest CT as imaging biomarkers in the management of lung adenocarcinoma.AJR Am J Roentgenol 2011; 196: 533-543.