
Case Report
Austin J Med Oncol. 2015; 2(2): 1018.
Primary Pancreatic Lymphoma, A Case Report and Review of Literature
Ettahri H1,2*, Elkabous M1,2, Laanaz S1,2, Layachi M1,2, Laamarti L1,2, Elghissassi I1,2 and Errihani H1,2
1Department of Medical Oncology, National Institute of Oncology, Morocco
2Mohammed V University at Souissi, Morocco
*Corresponding author: Hamza Ettahri, Department of Medical Oncology, National Institute of Oncology, Rabat 10000, Morocco
Received: July 29, 2015; Accepted: September 02, 2015; Published: September 10, 2015
Abstract
Background: Primary pancreatic lymphomas (PPL) are extremely rare, comprising less than 0.5% of pancreatic tumors. Usually, primary pancreatic lymphoma appears with symptoms of carcinoma of the pancreatic head.
Case Presentation: This case report describes the presentation of primary pancreatic lymphomas. A 74-year-old man has presented history of intermittent abdominal pain associated with intermittent vomiting, anorexia, weight loss and major asthenia. On physical examination we found abdominal distention associated with painful epigastric mass. Abdominal computed tomography (CT) revealed an irregular solid lesion of head and body of the pancreas associated with mesenteric and retroperitoneal lymph nodes, and signs of portal hypertension. The biopsy with immunohistochemical stains of lymph nodes was compatible with diffuse large B-cell lymphoma. The patient was provided to be treated by RCHOP regimen chemotherapy; unfortunately, he died before starting the first cycle.
Discussion: Primary pancreatic lymphoma (PPL) is an extremely rare disease that can be revealed as an isolated mass mimicking pancreatic carcinoma. The clinical presentation is not specific, furthermore, signs suggesting lymphomatous involvement are also rare and the diagnosis is based on imaging, and pathologic examination with immunochemical stain. Chemotherapy is the treatment of choice for most patients with pancreatic lymphoma.
Conclusion: PPL is a rare clinical entity, histopathologic examination is required for establish diagnosis. Management of patients with PPL is based on chemotherapy treatment and has a much better prognosis than those with adenocarcinoma.
Keywords: Pancreas; Lymphoma; Adenocarcinoma
Introduction
Primary pancreatic lymphoma (PPL) is an unusual clinical entity. Clinically, patients often present symptoms of carcinoma of the pancreatic head, and it occurs with predilection in the elderly patients, with a strong male predominance [1]. Radiological signs are often not specific, and mimics adenocarcinoma, the role of histological diagnosis is essential to initiate an appropriate treatment.
We report a case of a 74 years old man with primary pancreatic lymphoma, revealed as a pancreatic mass.
Case Presentation
We report a case of 74 years old man, without medical history, who presents two months ago a history of intermittent abdominal pain associated with intermittent vomiting, anorexia, weight loss and major asthenia.
On the physical examination, the patient had normal blood pressure and pulse rate; his abdomen was distended with presence of painful epigastric mass. The patient’s superficial lymph nodes were not palpable.
The biochemical results were: WBC count 13300/mm³; hemoglobin level 13.0 g/dL; AST 27 IU/L; ALT 14 IU/L; total bilirubin level, 7.6 mg/dL; lactate dehydrogenase (LDH) 425 IU/L (reference range, 25-125 IU/L). The levels of lipase, carcinoembryonic antigen and CA19-9 were within normal limits.
Abdominal computed tomography (CT) scan has found an irregular solid lesion of approximately 76 x 58 mm in diameter accompanied by a gradual increase of contrast in the head and body of the pancreas, which suggests an advanced pancreatic adenocarcinoma, associated with hepatosplenomegaly, mesenteric and retroperitoneal lymph nodes, and signs of portal hypertension (Figure 1).
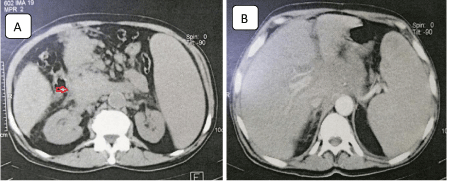
Figure 1: Computed tomography scan of the abdomen reveals important
pancreatic mass (red arrow in A) and hepatosplenomegaly (B).
Abdominal lymph node biopsy was performed, and pathology demonstrated the presence of malignant lymphoma dominated by large cells.
Immunochemical staining was positive for the CD20 B-cell marker and Bcl2 marker, although it was negative for the CD5, CD10 and CD30-cell markers. The Ki67 proliferative index was 80%. Pathologic examination was compatible with diffuse large B-cell lymphoma (Figure 2). The bone marrow biopsy was not infiltrated.
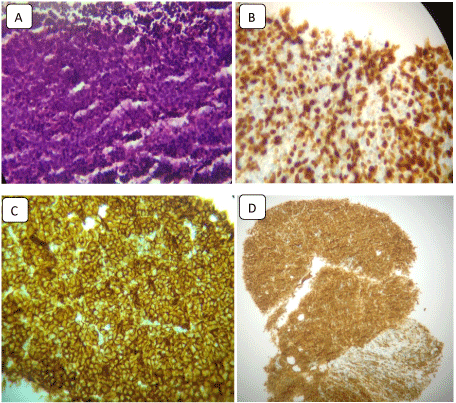
Figure 2: Histological examination of the lymph node biopsy (hematoxylineosin)
with immunohistochemical stains.
(A) Lymph node cells proliferation shows large mononuclear cells, consistent
with diffuse large B-cell lymphoma (H&E stain, �200); (B) The specimen
shows immunoreactivity for Ki-67; (C) Immunochemical staining was positive
for CD20; (D) Immunochemical staining was positive for BCL2.
The patient was provided to be treated with 6 cycles of R-CHOP chemotherapy regimen (Rituximab, Cyclophosphamide, Doxorubicin, Vincristine and Prednisone) unfortunately, he died before starting the first cycle.
Discussion
Non-Hodgkin lymphoma (NHL) can develops in extranodal sites; approximately 50% of patients have extranodal involvement. The gastrointestinal tract is the most commonly involved extranodal site; accounting for about half of such cases [1]. Stomach and the small intestine constitute the most common gastrointestinal sites. NHL is a rare cause of pancreatic masses. Less than 2% of extranodal malignant lymphomas and 0.5% of all pancreatic masses constitute PPL, Freeman and et al. reported that only 9 of 1,497 cases (0.6%) of extranodal malignant lymphoma coming from the pancreas [2]. Secondary involvement of the pancreas by NHL is also rare. Only 1.25% to 2.2% of all patients with NHL have pancreatic involvement at presentation [1,3-5].
Primary pancreatic lymphoma (PPL) is an extremely rare disease [6]. PPL can be presented as an isolated mass mimicking pancreatic carcinoma. However, unlike carcinomas, PPL are potentially treatable [7]. Pancreatic lymphoma is categorized as a non-epithelial tumor of the pancreas. Although rare, these tumors need to be considered in the differential diagnosis of a pancreatic mass [1].
The clinical presentation of primary pancreatic lymphoma is nonspecific; some clinical signs may suggest the clinical suspicion of lymphoma rather than pancreatic carcinoma. Abdominal pain is the most common presenting symptom (83%), followed by abdominal mass (58%), weight loss (50%), jaundice (37%), acute pancreatitis (12%), small bowel obstruction (12%), and diarrhea (12%) (Table 1) [8-11]. Other clinical symptoms may include anorexia, or early satiety. Obstructive jaundice seems to be less frequent than in pancreatic adenocarcinoma [1,9,10]. PPL rarely presents with the typical symptoms observed in lymphoma (i.e., weight loss, fever, or night sweats) [1,5,12].
Symptoms
Sign incidence
Abdominal pain
83%
Abdominal mass
58%
Weight loss
50%
Jaundice
37%
Nausea
34%
Vomiting
18%
Diarrhea
12%
Pancreatitis
12%
Bowel obstruction
12%
Fatigue
9%
Fever, chills, night sweats
2-7%
Gastrointestinal bleeding
2%
Gastric outlet obstruction
2%
Table 1: Common manifestations of primary pancreatic lymphoma [1].
Head of the pancreas is the most common location of PPL (more than 80%), though tumor can be found in the body and tail region [8,13]. The size of the tumor varies between 2 and 15 cm in greatest dimension, with the mean dimension of 8.0 cm as evaluated on the radiological scans [1,8].
The LDH level can be elevated in certain lymphoproliferative disorders including NHL, although LDH elevation is not necessarily a feature of PPL [14]. As for pancreatic adenocarcinoma, LDH was elevated in only 12.5% of 621 patients; LDH elevations up to 1,400 IU/L were reported. The serum CA19-9 level in patients with PPL is usually normal and sometimes slightly elevated when biliary obstruction is present [5,15].
In our case, the elevated LDH level (425 IU/L), and normal CA19-9 levels suggested that this was not advanced pancreatic adenocarcinoma.
Imaging plays a key role in the diagnosis and staging of pancreatic masses. Percutaneous ultrasound (US), endoscopic ultrasound (EUS) and computed tomography (CT) scan are well-established procedures to evaluate pancreatic masses. Imaging procedures can suggest a diagnosis of PPL, but a cytohistological diagnosis is mandatory for diagnosis and treatment planning of patients with suspected pancreatic mass [1].
The CT scan is by far the most common imaging technique used in the detection and characterization of primary pancreatic lymphoma; it tends to be more homogenous with less contrast enhancement on CT scan relative to pancreatic adenocarcinoma.
Two different morphologic patterns of pancreatic involvement are seen in patients with PPL [1,16]:
1. A localized, well-circumscribed tumoral form; and
2. A diffuse enlargement infiltrating or replacing most of the pancreatic gland.
Certain radiological findings have been found to be beneficial to differentiate PPL from the more common pancreatic adenocarcinoma [1,16]:
a. The combination of a bulky localized tumor in the pancreatic head without significant dilatation of the main pancreatic duct strengthens a diagnosis of pancreatic lymphoma over adenocarcinoma;
b. Enlarged lymph nodes below the level of the renal veins; and
c. Invasive tumor growth not respecting anatomic boundaries and infiltrating retroperitoneal or upper abdominal organs and the gastrointestinal tract are additional reliable signs for PPL.
In the present case, a solid homogenous lesion with marginal enhancement was observed in head and body of the pancreas, associated with hepatosplenomegaly, mesenteric and retroperitoneal lymph nodes.
In general, bile and pancreatic ductal dilatation can be easily assessed with MR (magnetic resonance) imaging using MR cholangiopancreatography. Furthermore, MR imaging is equivalent to CT regarding information about the peri-pancreatic vessels and enlarged lymph nodes. Additional information is obtained when MR angiography is used [1].
PET scan plays an ever-increasing role in the management of patients with lymphoma. It is useful at the initial diagnosis and workup to help in disease staging. It can also be very helpful in evaluation of response to therapy; it has also been proven to be superior to the conventional imaging modalities in some circumstances. Many studies have reported very high sensitivity and specificity of PET in the diagnosis of lymphoma and the identification of metabolically active lesions [17].
A definitive diagnosis of PPL is impossible from imaging alone, and pathologic examination is necessary. US- and CT-guided biopsy techniques can easily provide sufficient diagnostic tissue, as in our case we made a CT-guided lymph node biopsy, the fine needle aspiration of the pancreas has not been performed, although the clinical and paraclinical presentation suggests diagnosis of PPL.
Pathological diagnosis of PPL may be extremely difficult on haematoxylin-eosin stains alone, and resemble poorly differentiated carcinoma and reticulum cell sarcoma [18], thus immunohistochemical stains and flow cytometry are essential [19,20].
The management and prognosis of PPL depends on the stage and grade of the tumor. Most PPL tumors are diffuse large B-cell lineage. According to recent reports, long-term remission in several cases of PPL has been obtained with chemotherapy alone [14]. Laparotomy is performed only when a histopathologic diagnosis cannot be obtained. A chemotherapeutic regimen involving cyclophosphamide, doxorubicin, vincristine and prednisolone has become the first-line therapy. In the case of CD20-positive diffuse large B-cell lymphoma, rituximab is added to chemotherapy regimen, and an increase in the rate of remission is confirmed. [1,5,14] The combination of radiation therapy with chemotherapy has been reported, but its effectiveness remains to be determined. Local radiotherapy up to total 40 Gray has been used as consolidation for management of PPL [1].
Patients with PPL managed by chemotherapy-based treatment have a much better prognosis than those with pancreatic adenocarcinoma. According to many studies, 5 year survival rates of patients with PPL vary from 26 to 66% [1,5].
Conclusion
PPL is a rare neoplasm that mimics pancreatic adenocarcinoma in many aspects, but it is different in terms of treatment options and prognosis. The clinical and radiological findings are not pathognomonic and the diagnosis is established only after histopathologic examination. Patients with PPL require a chemotherapy-based treatment and have a much better prognosis than those with adenocarcinoma.
References
- Saif MW: Primary pancreatic lymphomas. JOP. 2006; 7: 262-273.
- Zucca E, Roggero E, Bertoni F, Cavalli F. Primary extranodal non-Hodgkin's lymphomas. Part 1: Gastrointestinal, cutaneous and genitourinary lymphomas. Ann Oncol. 1997; 8:727-37.
- Glazer HS, Lee JK, Balfe DM, Mauro MA, Griffith R, Sagel SS. Non-Hodgkin lymphoma: Computed tomographic demonstration of unusual extranodal involvement. Radiology. 1983; 149: 211-217.
- Webb TH, Lillemoe KD, Pitt HA. Pancreatic lymphoma. Is surgery mandatory for diagnosis or treatment? Ann Surg. 1989; 209:25-30.
- Fukita Y, Asaki T, Adachi S, Yasuda I, Toyomizu M, Katakura Y. Non-Hodgkin lymphoma mimicking pancreatic adenocarcinoma and peritoneal carcinomatosis. J Clin Onco. 2013; 31: 373-376.
- Joly I, David A, Payan MJ, Sahel J, Sarles H. A case of primary non-Hodgkin's lymphoma of the pancreas. Pancreas. 1992; 7:118-20.
- Baylor SM, Berg JW. Cross classification and survival characteristics of 5,000 cases of cancer of the pancreas. J Surg Oncol. 1973; 5:335-8.
- Nayer H, Weir EG, Sheth S, Ali SZ. Primary pancreatic lymphoma. Cancer. 2004; 102:315-21.
- James JA, Milligan DW, Morgan GJ, Crocker J. Familial pancreatic lymphoma. J Clin Pathol. 1998; 51:80-2.
- Nishimura R, Takakuwa T, Hoshida Y, Tsujimoto M, Aozasa K. Primary pancreatic lymphoma: clinicopathological analysis of 19 cases from Japan and review of the literature. Oncology. 2001; 60: 322-9.
- Arcari A, Anselmi E, Bernuzzi P, Berte R, Lazzaro A, Moroni CF, et al. Primary pancreatic lymphoma. Report of five cases. Haematologica. 2005; 90: ECR09.
- Rock J, Bloomston M, Lozanski G, Frankel WL. The spectrum of hematologic malignancies involving the pancreas: Potential clinical mimics of pancreatic adenocarcinoma. Am J Clin Pathol. 2012; 137: 414-422.
- Islam S, Callery MP. Primary pancreatic lymphoma-a diagnosis to remember. Surgery. 2001; 129: 380-3.
- Du X, Zhao Y, Zhang T, Liao Q, Dai M, Liu Z, et al: Primary pancreatic lymphoma: A clinical quandary of diagnosis and treatment. Pancreas. 2011; 40: 30-36.
- Stocken DD, Hassan AB, Altman DG, Billingham LJ, Bramhall SR, Johnson PJ, et al. Modelling prognostic factors in advanced pancreatic cancer. Br J Cancer. 2008; 99: 883-893.
- Merkle EM, Bender GN, Brambs HJ. Imaging findings in pancreatic lymphoma: differential aspects. AJR Am J Roentgenol. 2000; 174: 671-5.
- Saif MW, Tzannou I, Makrilia N, Syrigos K. Role and cost effectiveness of pet/ct in management of patients with cancer. Yale J Bio Med. 2010; 83: 53-65.
- Ackerman NB, Aust JC, Bredenberg CE, Hanson VA Jr, Rogers LS. Problems in differentiating between pancreatic lymphoma and anaplastic carcinoma and their management. Ann Surg. 1976; 184: 705-708.
- Nayer H, Weir EG, Sheth S, Ali SZ. Primary pancreatic lymphomas: a cytopathologic analysis of a rare malignancy. Cancer. 2004; 102: 315-321.
- Grimison PS, Chin MT, Harrison ML, Goldstein D. Primary pancreatic lymphoma – pancreatic tumours that are potentially curable without resection, a retrospective review of four cases. BMC Cancer. 2006; 6: 117.