Research Article
Austin J Mult Scler & Neuroimmunol. 2014;1(1): 5.
Impact of Extracranial Veins Endovascular Procedures on the Quality of Life in Patients with Multiple Sclerosis - Follow Up After 1 Year
Denislic M1,2*, Zorc M1,2, Ravnik J2,6, Milosevic Z3, Tiric Campara M4, Al-Hashel JY5, Zorc Pleskovic R1 and Ravnik D1
1University of Ljubljana, Slovenia
2MC Medicor, Slovenia
3University Clinical Centre Ljubljana, Slovenia
4Neurološka Klinika, BIH
5Neurology Department Ibn Sina, Kuwait
6Mathematics and Physics, University of Ljubljana, Slovenia
*Corresponding author: Denislic M, University of Ljubljana, Korytkova 2, SI-1000 Ljubljana, Slovenia
Received: September 30, 2014; Accepted: December 02, 2014; Published: December 05, 2014
Abstract
Background: Chronic cerebrospinal venous insufficiency is a new term which highlights the role of extracranial venous anomalies. Stenoses of the jugular and the azygous veins hinder venous drainage and may influence brain perfusion and cerebrospinal fluid flow.
Materials and Methods: In patients with relapsing-remitting and progressive course of multiple sclerosis with a proven obstruction of neck veins percutaneous transluminal angioplasty was performed. We evaluated the clinical disability and quality of life in terms of fatigue, cognitive, psychosocial and bladder dysfunction one year after angioplasty.
Results: In the relapsing-remitting group of patients an improvement of disability was observed, whereas in patients with the progressive course of the disease a stable clinical status was noticed. Both patient groups showed a significant improvement of fatigue. Cognitive and psychosocial impact on the quality of life showed better outcome in patients with advanced course of the disease than in less affected patients. Important amelioration of bladder dysfunction was achieved in both groups.
Conclusion: Endovascular procedures of extracranial venous anomalies demonstrated an encouraging effect in patients with relapsing-remitting and progressive course of the disease. It seems that the removal of vein obstructions improves many non-motor symptoms which importantly contribute to the quality of life in MS patients.
Keywords: Chronic cerebrospinal venous insufficiency; Percutaneous transluminal angioplasty; Clinical disability; Fatigue; Cognitive function; Micturition disturbance
Introduction
Chronic cerebrospinal venous insufficiency (CCSVI) is a new paradigm which provides at present still controversial insight into the vascular role of multiple sclerosis (MS). By contrast, numerous studies are endeavoring to elucidate the role of CCSVI and its influence on the course of MS [1-5]. CCSVI is a syndrome characterized by stenoses or obstructions of the internal jugular (IJV) and/or azygous (AZ) veins. Venous narrowings are related to intraluminal defects such as webs, fixed valve leaflet, membrane, inverted valve position or congenital segmental hypoplasia [6,7]. The relationship between global hypoperfusion of the brain and deficient blood drainage due to venous anomalies in MS patients is discussed [8]. Due to venous occlusions, the amount of toxic radicals in the central nervous system (CNS) accumulates and enhances the process of inflammation.
MS is a chronic inflammatory progressive immune-mediated demyelinating disease of CNS characterized by inflammation, demyelination, diffuse axonal damage and neuronal loss. The cause and pathogenesis of MS are still unknown. Most of the patients have a relapsing-remitting (RR) course of the disease. About 15% of patients start with a primary progressive form of the disease (PP). After 10-15 years, a large proportion of RR patients develop a secondary progressive (SP) course of the disease [9]. An interaction between genetic and environmental factors is considered as a determinant of susceptibility, whereas immune mechanisms are implicated as the effector of inflammatory demyelination and neurodegeneration. Hypothesis that MS has an autoimmune pathogenesis is based on inflammatory changes, intrathecal immunoglobulin production, and T-cell - mediated immunopathology and autoimmune-initiated demyelination [10-12]. The variable clinical course and heterogeneity of active demyelinating lesions support the view that MS is not a single entity [9,10]. The most common of four immunohistopathological - pattern II demyelination in MS lesion suggests antibody-dependent and complement-dependent pathogenicity [10]. The absence of a MS specific biomarker makes therapeutic trial difficult. The target antigen of MS remains still elusive [13]. Although the role of vascular impact on the course of MS is denied by many authors [14-16], there are several studies reporting a marked symptomatic improvement after endovascular procedures [17-19].
The purpose of the study was to evaluate the effect of percutaneous transluminal angioplasty (PTA) on the clinical disability and quality of life (QoL) in MS patients 1year after the procedure.
Materials and Methods
MS patients included in our study trial were diagnosed by revised McDonald criteria [20]. The disability was assessed by the Expanded Disability Status Scale - EDSS [21]. Disability between 1.0 and 3.0 is considered as mild, 3.0 to 6.0 as moderate and more than 6.0 as severe requiring intermittent/unilateral constant assistance to walk ~ 100m. The condition for performing a catheter venography (CV) was the fulfilling of two or more of 5 proposed criteria obtained by Doppler sonography required for CCSVI [1,2,22]. Informed consent was obtained from the participating subjects and the study was approved by the National Medical Ethics Committee.
All patients recruited in the study underwent PTA. Before CV, the MS patients received low-molecular-weight heparin subcutaneously (Heparin 5000 IE). Coronary catheter was introduced into the right femoral vein under local anaesthesia and mild sedation. The catheter was first placed into the AZV and positioned at the junction with the hemiazygous vein. After examination of the AZV and lumbar veins, the catheter was placed into the right and then into the left IJV. The exact procedure of CV has been described in our previous article [19]. A luminal diameter reduction of 50% is used as a threshold for angioplasty.
Fatigue was assessed by the Fatigue Severity Scale (FSS). FSS is a unidimensional scale [23], has a physical impact and consists of 9 items on a seven-point scale (range 1-7) and is scored by computing the average ratings [24]. A lower score indicates less fatigue. Three items are related to physical status, three items to the psychosocial environment and three are more generic [25]. The FSS was scored on the day preceding vascular procedure, and at 3, 6 and 12 months after angioplasty. An FSS score ≤4 was considered as status of "non-fatigue", scores between 4.1 and 4.9 as "doubtful fatigue" and scores ≥5 as status of fatigue [26,27].
At the same time as the FSS, an assessment of Modified Fatigue Impact Scale (MFIS) was performed, as recommended by the Multiple Sclerosis Council for Clinical Practice Guidelines [28]. It consists of 21 items assessing impact on: physical status (nine items, pMFIS); cognitive status (ten items, cMFIS); and psychosocial functional status (two items, psMFIS). Finally, the total- global score is calculated (gMFIS). The maximal score is 84 [29]. MS patients with depression and major illnesses which can influence fatigue were excluded.
QoL was evaluated by a simple Visual Analogue Scale (VAS) by pointing the filling on a vertical 100 mm scale (range 0-100). The patient is asked to label on the line the point that best indicates her/ his feeling. A higher score is compatible with better life performance. Additionally, QoL was assessed by Multiple Sclerosis Impact Scale 29 - MSIS-29 scale [30]. The MSIS-29 contains 29 items on 2 subscales: physical impact (PHY, 20 items) and psychological impact (PSY, 9 items).
The bladder dysfunction was assessed by Overactive Bladder Self-Administered Questionnaire (OAB-V8). The 8-item validated questionnaire (Pfizer) reflects micturition function (Table 1). How bothered the patients are by bladder problems is calculated on a 6-point scale ranging from 0 (not at all) to 5 (a very great deal). Patients add 2 points if they are male.
Frequent urination during the daytime hours?
0
1
2
3
4
5
An uncomfortable urge to urinate?
0
1
2
3
4
5
A sudden urge to urinate with little or no warning?
0
1
2
3
4
5
Accidental loss of small amounts of urine?
0
1
2
3
4
5
Nighttime urination?
0
1
2
3
4
5
Waking up at night because you had to urinate?
0
1
2
3
4
5
An uncontrollable urge to urinate?
0
1
2
3
4
5
Urine loss associated with a stronge desire to urinate?
0
1
2
3
4
5
Table 1: Overactive bladder questionnaire.
FSS, MFIS, VAS, MSIS-29 and OAB-V8 scales were evaluated at baseline and 12 months after PTA.
All testing was performed by a well-trained neurologist.
Statistical Analysis
Parametric results are expressed as mean values with standard deviation for each group. An independent Student's t-test was performed to analyse the values of subscales of MSIS-29 scale. The efficacy of angioplasty on the changes of EDSS, FSS, MFIS, VAS and OAB-V8 at the start and after follow-up in the RR and SP-PP groups of patients was evaluated by a paired Student's t-test. A p-value of <0.05 was considered as significant.
Result
In our study 72 patients - 20 with RR and 52 with SP-PP - were enrolled. The group of RR patients was significantly younger, duration of disease was shorter and the degree of disability lower than in SP and PP patients (p = 0.001). There was no important differrence in age, duration of disease and clinical disability between SP and PP groups of patients. Therefore, further evaluation included the comparison between the two groups of patients - RR and SP-PP. The demographic data of these two groups of patients are depicted in Table 2.
N
Gender
Age (years)
Duration (years)
EDSS
RR
20
14/6 (F/M)
31.45 ± 8.72
4.65 ± 4.08
3.05 ± 2.05
SP-PP
52
27/25(F/M)
46.29 ± 11.26
12.58 ± 7.42
5.53 ± 1.61
Table 2: Demographic and clinical data of RR and SP-PP groups of patients before PTA.
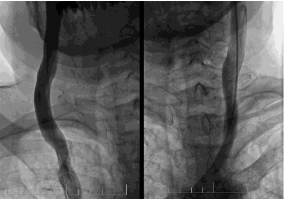
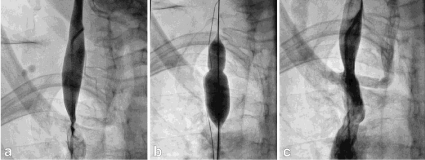
Venous stenoses were found in all MS patients included in the study. A case of non-MS person with normal jugular veins, and an MS patient with severe jugular stenosis before and after dilation are presented in Figures 1 and 2, respectively.
Figure 1: Normal configuration of the jugular veins in a non-MS subject.
Figure 2: (a) Severe stenosis of the right jugular vein, (b) angioplastic balloon and ''cutting'' wire close to balloon and (c) improved flow after dilatation.
Disability measured by the EDSS scale showed a significant (25%) improvement in RR patients (p < 0.001). In the SP-PP group of MS patients with higher disability (mean 5.53, SD 1.61) comparing to RR group (mean 3.05, SD 2.05) before PTA after angioplasty changes were not observed. It is important to add that duration of disease in SP-PP group (mean 12.58, SD 7.42) was significantly longer (p < 0.001) than in RR group (mean 4.65, SD 4.08). In addition, disability in patients with progressive course was higher (Table 2). The both conditions influenced clinical outcome after PTA.
The mean value of FSS score in RR group decreased significantly from 3.68 (SD 1.82) to 2.60 (SD 1.11) after PTA procedures (p < 0.001). In contrast to RR group SP-PP groups of MS patients higher starting-point of fatigue was noted - mean value 5.15 (SD 1.43). Also in this group of patient significant amelioration of fatigue was recorded (p < 0.001).
FSS score showed important improvement of all 9 items, especially changes of item 2 - exercise brings on my fatigue, item 3 - I am easily fatigued and item 8 - fatigue is among my three most disabling symptoms, mostly contributed to the lowering of fatigue. Compared with baseline of fatigue, the FSS score after 1 year remained stable indicating long lasting PTA efficacy. Fatigue was more frequent in SP-PP patients (40%) than in RR group (30%).
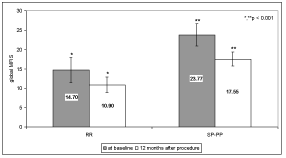
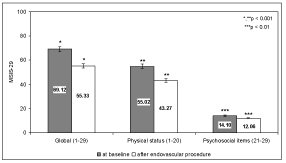
In the RR group of patients an improvement of physical subscales (12.9 ± 1.99 before and 9.70 ± 1.60 after PTA, p < 0.01) whereas cognitive and psychosocial scores were unchanged. In addition, important amelioration of global score in RR and SP-PP groups was achieved (p < 0.01, Figure 3). By contrast, in the SP-PP group of patients marked improvement of all three subscales was observed (p < 0.001). Correlation between the FSS, the physical MFIS and the global MFIS scores in both groups was very strong (p < 0.001).
Figure 3: MFIS in RR and SP-PP patient groups (mean ± SE). RR - relapsing remitting patients; SP-PP - secondary progressive and primary progressive groups of patients.
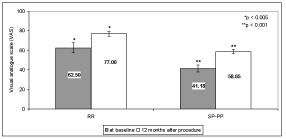
QoL was first assessed by simple and very understandable VAS scale which reflects a more subjective being. In the both groups of patients a significant efficacy of PTA was obtained. The results of QoL in RR and SP-PP groups of patients assessed by VAS are demonstrated in Figure 4. An important amelioration of VAS was obtained in the RR group (p < 0.005) as well as in the SP-PP group (p < 0.001).
Figure 4: Quality of life assessed by VAS in the RR and SP-PP groups of MS patients (mean ± SE). RR - relapsing remitting patients; SP-PP - secondary progressive and primary progressive groups of patients.
QoL assessed by the MSIS-29 scale in SP-PP patients showed amelioration of PHY (p < 0.001), PSY (p < 0.01) and global impact scores (p < 0.001) (Figure 5). In the RR group of patients with the lower degree of disability (Table 2) the evaluation of the MSIS-29 scale did not demonstrate any changes.
Figure 5: MSIS-29 values in SP-PP group of patients (mean ± SE).
Frequency and urination urgency decreased markedly after vascular procedures. Likewise, an urge to urinate was less disturbing. Uncontrolled loss of small amount of urine occurred rarely than before PTA. Nocturia was less prominent. Six patients avoided intermittent catheterization.
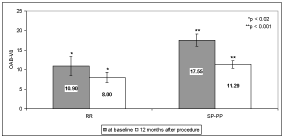
The results of testing bladder dysfunction using OAB-V8 questionnaire are shown in Figure 6. There was an important decrease of bladder dysfunction in both groups of patients (RR group p < 0.02 and in SP-PP group p < 0.001).
Figure 6: Bladder dysfunction assessed by the OAB-V8 questionnaire in both patient groups (mean ± SE). RR - relapsing remitting patients; SP-PP - secondary progressive and primary progressive groups of patients.
Discussion
The role of CCSVI in the etiology of MS is still obscure. Abnormalities of extracranial veins - IJV and AV are considered often as an anatomical variant and not as congenital or acquired anomalies which might influence the course of disease [3,5,14]. Many physicians exclusively consider the decrease in relapse rate as the most important effect of disease - modifying therapy. Neurologists are inclined to ignore the importance of many other symptoms such as fatigue, cognitive impairment, behavior disturbances and bladder dysfunction. However, these are the symptoms that mostly affect the behavior and daily life of MS patients.
In the study, an important improvement was achieved in the clinical disability of RR patients after 12 months of PTA (mean EDSS 3.05 ± 2.05 vs. 2.29 ± 2.23). The most marked improvement in the EDSS score was 3 months after angioplasty. Similar findings were published after 2 years of PTA, and the role of improved global hypoperfusion was discussed [31]. During 1 year follow-up in the RR group, relapses were observed in two patients. Analysing the annual relapse rate in this small group of patients seems incorrect. Considering EDSS in patients with the progressive form of the disease, no changes in disability was observed. Neurodegeneration is a leading process which might explain the unchanged EDSS in this group of patients [9,10]. However, 1 year after angioplasty no increase disability in the SP-PP MS group was noticed.
Fatigue is one of the most frequent and disabling complaints in MS patients. In a third of patients with MS, fatigue is a leading symptom. It can importantly interfere with daily activity and quality of life [32]. Fatigue is independent of age and duration of the disease [33]. The definitive pathogenesis of fatigue is poorly understood, despite different studies. Fatigue after CCSVI treatment, assessed by the FSS scale, showed amelioration in both groups of patients. Fatigue was present in 38% of all MS patients. Similar to other studies, we found a higher percentage of fatigue in SP-PP than in RR patients [25,33]. A decrease in fatigue was reported 3 months after PTA, with a slightly upward trend past 1 year. There was no difference in fatigue between immunomodulatory treated and untreated patients. Similar observation was reported by Flachenecker et al. [33]. Using the MFIS scale, an improvement of the physical and global score in RR patients was observed. A better impact of pMFIS was more pronounced in the SP-PP of patients than in the RR group. By contrast, the score of all three subscales and global score of MFIS in patients with an advanced course of the disease demonstrated a significant improvement after PTA. Shorter disease duration and lower disability in the RR group reflect a milder affect of cognitive and psychosocial impact. An amelioration of cognitive function in MS cases after angioplasty was published recently [34]. The FSS score strongly correlated with the global MFIS score, as reported in other study [26]. Some authors concluded that FSS reflects the impact of fatigue on physical aspect and that cognitive and psychosocial functions are better analysed by MFIS [26,33].
Evaluating QoL by the MSIS-29 questionnaire, global score and both subscales, demonstrated a significant effect of PTA in advanced cases of MS. In the RR group using the MSIS-29 scale no change in QoL was observed. This finding could be explained by the shorter disease duration and lower disability in the RR group which mirror a milder effect on daily life. Using the simple VAS, patients of both groups reported better QoL.
It is well known that the disturbance of bladder storage and emptying is a common and very disabling feature in MS patients. In more than 75% of patients, urgency, abnormal voiding, hesitancy and an interrupted flow with the sensation of incomplete emptying are the leading symptoms which influence the patients' daily activities and QoL [35]. Dysfunctions of micturition and sexual function have an important impact on the relationship of MS patients with their partners. Using OAB-V8 questionnaire, the micturition disturbance improved markedly in both patient groups. There is a great deal to decrease the micturition disturbance after angioplasty. Many of our patients pointed out the positive effect on urinary function as the most important impact of angioplasty. The improvement of urinary dysfunction contributed to better QoL in MS patients.
There is no doubt that the treatment of MS is still deficient. The proposed first-line disease-modifying therapy - interferon beta and glatiramer acetate, has approximately 29-32% of efficacy in the treatment of RR patients [36]. Furthermore, there is no proper treatment for the progressive course of MS. It is important to declare that the endovascular procedures are safe with rare side effects [37].
The major shortcoming of our pilot study is that it was not blinded and there was no control group. The number of included patients is too small to draw distinct conclusions. However, the efficacy of endovascular procedures is promising, and further multicentre studies are recommended.
Conclusion
The deficient immunomodulatory treatment of MS is a challenging factor to search for an additional way to prevent and slow the course and the disability of this very debilitating disease. Improving the cerebral venous drainage is a promising step in the amelioration of the CNS function. There is no doubt that the achievement of better mobility of patients is the most important factor in the treatment of MS patients. However, QoL is yet another but not negligible aspect in the daily life of MS patients. The non-motor symptoms of MS like fatigue, cognitive, psychosocial, bladder and sexual functions, should not be underestimated.
References
- Zamboni P, Galeotti R, Menegatti E, Malagoni AM, Tacconi G, Dall'Ara S, et al. Chronic cerebrospinal venous insufficiency in patients with multiple sclerosis. J Neurol Neurosurg Psychiatry. 2009; 80: 392-399.
- Zamboni P, Galeotti R, Menegatti E, Malagoni AM, Gianesini S, Bartolomei I, et al. A prospective open-label study of endovascular treatment of chronic cerebrospinal venous insufficiency. J Vasc Surg. 2009; 50: 1348-1358.
- Khan O, Filippi M, Freedman MS, Barkhof F, Dore-Duffy P, Lassmann H, et al. Chronic cerebrospinal venous insufficiency and multiple sclerosis. Ann Neurol. 2010; 67: 286-290.
- Mayer CA, Pfeilschifter W, Lorenz MW, Nedelmann M, Bechmann I, Steinmetz H, et al. The perfect crime? CCSVI not leaving a trace in MS. J Neurol Neurosurg Psychiatry. 2011; 82: 436-440.
- Ghezzi A, Comi G, Federico A. Chronic cerebro-spinal venous insufficiency (CCSVI) and multiple sclerosis. Neurol Sci. 2011; 32: 17-21.
- Zivadinov R, Galeotti R, Hojnacki D, Menegatti E, Dwyer MG, Schirda C, et al. Value of MR venography for detection of internal jugular vein anomalies in multiple sclerosis: a pilot longitudinal study. AJNR Am J Neuroradiol. 2011; 32: 938-946.
- Al-Omari MH, Rousan LA. Internal jugular vein morphology and hemodynamics in patients with multiple sclerosis. Int Angiol. 2010; 29: 115-120.
- D'haeseleer M, Cambron M, Vanopdenbosch L, De Keyser J. Vascular aspects of multiple sclerosis. Lancet Neurol. 2011; 10: 657-666.
- Noseworthy JH, Lucchinetti C, Rodriguez M, Weinshenker BG. Multiple sclerosis. N Engl J Med. 2000; 343: 938-952.
- Lucchinetti CF, Brueck W, Rodriguez M, Lassmann H. Multiple sclerosis: lessons from neuropathology. Semin Neurol. 1998; 18: 337-349.
- Compston A, Coles A. Multiple sclerosis. Lancet. 2008; 372: 1502-1517.
- Ascherio A, Munger KL. Environmental risk factors for multiple sclerosis. Part I: the role of infection. Ann Neurol. 2007; 61: 288-299.
- Brickshawana A, Hinson SR, Romero MF, Lucchinetti CF, Guo Y, Buttmann M, et al. Investigation of the KIR4.1 potassium channel as a putative antigen in patients with multiple sclerosis: a comparative study. Lancet Neurol. 2014; 13: 795-806.
- Doepp F, Paul F, Valdueza JM, Schmierer K, Schreiber SJ. No cerebrocervical venous congestion in patients with multiple sclerosis. Ann Neurol. 2010; 68: 173-183.
- Krogias C, Schröder A, Wiendl H, Hohlfeld R, Gold R. "Chronic cerebrospinal venous insufficiency" and multiple sclerosis: critical analysis and first observation in an unselected cohort of MS patients. Nervenarzt. 2010; 81: 740-746.
- Baracchini C, Perini P, Calabrese M, Causin F, Rinaldi F, Gallo P. No evidence of chronic cerebrospinal venous insufficiency at multiple sclerosis onset. Ann Neurol. 2011; 69: 90-99.
- Zamboni P, Galeotti R, Weinstock-Guttman B, Kennedy C, Salvi F, Zivadinov R, et al. Venous angioplasty in patients with multiple sclerosis: results of a pilot study. Eur J Vasc Endovasc Surg. 2012; 43: 116-122.
- Beelen R, Maene L, Castenmiller P, Decoene V, Degrieck I. Evolution in quality of life and epidemiological impact after endovascular treatment of chronic cerebro-spinal venous insufficiency in patients with multiple sclerosis. Phlebology. 2012; 27: 187-189.
- Denislic M, Milosevic Z, Zorc M, Zuran I, Ravnik D, Mendiz O. Disability caused by multiple sclerosis is associated with the number of extra cranial venous stenoses: possible improvement by venous angioplasty. Results of a prospective study. Phlebology. 2013; 28: 353-360.
- Polman CH, Reingold SC, Edan G, Filippi M, Hartung HP, Kappos L, et al. Diagnostic criteria for multiple sclerosis: 2005 revisions to the "McDonald Criteria". Ann Neurol. 2005; 58: 840-846.
- Kurtzke JF. Rating neurologic impairment in multiple sclerosis: an expanded disability status scale (EDSS). Neurology. 1983; 33: 1444-1452.
- Simka M, Kostecki J, Zaniewski M, Majewski E, Hartel M. Extracranial Doppler sonographic criteria of chronic cerebrospinal venous insufficiency in the patients with multiple sclerosis. Int Angiol. 2010; 29: 109-114.
- Comi G, Leocani L, Rossi P, Colombo B. Physiopathology and treatment of fatigue in multiple sclerosis. J Neurol. 2001; 248: 174-179.
- Krupp LB, LaRocca NG, Muir-Nash J, Steinberg AD. The fatigue severity scale. Application to patients with multiple sclerosis and systemic lupus erythematosus. Arch Neurol. 1989; 46: 1121-1123.
- Bergamaschi R, Romani A, Versino M, Poli R, Cosi V. Clinical aspects of fatigue in multiple sclerosis. Funct Neurol. 1997; 12: 247-251.
- Téllez N, Río J, Tintoré M, Nos C, Galán I, Montalban X. Does the Modified Fatigue Impact Scale offer a more comprehensive assessment of fatigue in MS? Mult Scler. 2005; 11: 198-202.
- Malagoni AM, Galeotti R, Menegatti E, Manfredini F, Basaglia N, Salvi F, et al. Is chronic fatigue the symptom of venous insufficiency associated with multiple sclerosis? A longitudinal pilot study. Int Angiol. 2010; 29: 176-182.
- Multiple Sclerosis Council for Clinical Practice Guidelines. Fatigue and multiple sclerosis: evidence-based management strategies for fatigue in multiple sclerosis.
- Fisk JD, Pontefract A, Ritvo PG, Archibald CJ, Murray TJ. The impact of fatigue on patients with multiple sclerosis. Can J Neurol Sci. 1994; 21: 9-14.
- Hobart J, Lamping D, Fitzpatrick R, Riazi A, Thompson A. The Multiple Sclerosis Impact Scale (MSIS-29): a new patient-based outcome measure. Brain. 2001; 124: 962-973.
- Salvi F, Bartolomei I, Buccellato E, Galeotti R, Zamboni P. Venous angioplasty in multiple sclerosis: neurological outcome at two years in a cohort of relapsing-remitting patients. Funct Neurol. 2012; 27: 55-59.
- Janardhan V, Bakshi R. Quality of life in patients with multiple sclerosis: the impact of fatigue and depression. J Neurol Sci. 2002; 205: 51-58.
- Flachenecker P, Kümpfel T, Kallmann B, Gottschalk M, Grauer O, Rieckmann P, et al. Fatigue in multiple sclerosis: a comparison of different rating scales and correlation to clinical parameters. Mult Scler. 2002; 8: 523-526.
- De Pasquale C, Pistorio ML, Veroux M, Giaquinta A, Veroux P, Fornaro M. Cognitive functioning and subjective quality of life in relapsing-remitting multiple sclerosis patients before and after percutaneous transluminal angioplasty: a preliminary report. Neuropsychiatr Dis Treat. 2014; 10: 1039-1044.
- Vitkova M, Rosenberger J, Krokavcova M, Szilasiova J, Gdovinova Z, Groothoff JW, et al. Health-related quality of life in multiple sclerosis patients with bladder, bowel and sexual dysfunction. Disabil Rehabil. 2014; 36: 987-992.
- Sorensen PS. New management algorithms in multiple sclerosis. Curr Opin Neurol. 2014; 27: 246-259.
- Mandato KD, Hegener PF, Siskin GP, Haskal ZJ, Englander MJ, Garla S, et al. Safety of endovascular treatment of chronic cerebrospinal venous insufficiency: a report of 240 patients with multiple sclerosis. J Vasc Interv Radiol. 2012; 23: 55-59.