
Research Article
Austin J Mult Scler & Neuroimmunol. 2015;2(3): 1019.
Lack of Evidence for a Temporal Relationship between Fatigue Perception and Physical Activity in Multiple Sclerosis
Selukar S¹, Moriello C², Andersen RE³, Reid RER³ and Mayo NE1,2*
¹School of Physical and Occupational Therapy, McGill University, Canada
²Division of Clinical Epidemiology, McGill University, Canada
³Department of Kinesiology and Physical Education, McGill University, Canada
*Corresponding author: Mayo NE, Division of Clinical Epidemiology, McGill University, Royal Victoria Hospital, 687 pine ave west (R4.17), Montreal, Quebec, H3A-1A1, Canada
Received: April 16, 2015; Accepted: July 01, 2015; Published: July 04, 2015
Abstract
There is inconsistent evidence regarding daily variation of fatigue perception and its association with physical activity. While there is evidence that exercise can reduce fatigue it is not clear whether fatigue is a cause or consequence of physical inactivity.
The global aim of this study is to contribute evidence towards the daily variability in fatigue perception and to delineate the temporal sequence with physical activity in people with MS. This is a longitudinal predictive study over two time periods, immediately after trial entry and after the first exercise prescription (1 week later).
Fatigue perception was measured using a visual analogue scale for everyday at 8am, 12pm, 4pm and 9pm. Physical activity was recorded using an accelerometer for two continuous periods of 7 days.
Data was analyzed using Generalized Estimating Equations to adjust the variance for the clustering of measures within person. Odds ratio (OR) was used to identify peak times of the day for fatigue perception.
The results on 40 participants suggested that the odds of having maximum fatigue increased along the course of the day (lowest in morning, highest at night). Compared to 8:00 hours, the OR associated with having maximum fatigue at 21:00 hours was 5.57 (95% CI: 1.00, 2.44). At neither time period did end-of-day fatigue level impact on next day physical activity as measured by number of steps and the same for activity and perception of fatigue the next day. In this sample of low disability MS, there was no evidence linking fatigue and physical activity.
Keywords: Fatigue; Multiple sclerosis; Physical activity
Abbreviations
MS: Multiple Sclerosis; OR: Odds Ratio; CI: Confidence Interval
Introduction
Fatigue is the most studied symptom of Multiple Sclerosis (MS) in terms of measurement, impact, and treatment. A recent taxonomy of fatigue, separates perceived fatigue from performance fatigability [1], the former being measured using questionnaires, the latter measured with tests of muscle output. For patients, fatigue perception is what they report as distressing and is potentially what they can control by regulating activity and rest. Variation in perceived fatigue over time and with activity, and what this may mean in terms of etiology, impact, and treatment, has not been investigated systematically and evidence of a pattern is inconsistent [2-6].
People with MS consider fatigue as a barrier to take part in physical activity [7], yet the benefits of exercise are well established [8-11]. Despite this evidence, persons with MS show poor long term adherence in exercise programs and are reported to have high dropout rates [12]. The question remains, as to whether, exercise programs should be directed to improve physical activity in order to reduce fatigue, or should management of fatigue be considered first to improve physical activity. The relationship between fatigue and every day physical activity is a “chicken or egg” phenomenon, it is not clear whether fatigue is a cause or a consequence of physical inactivity.
The current longitudinal study aims: (i) to estimate the extent of variability in daily fatigue perception and identify the time of day where fatigue perception is the highest, and (ii) to estimate the temporal sequence between fatigue perception and physical activity.
Materials and Methods
Study design
This is a two-period longitudinal predictive study embedded within an ongoing randomized trial of exercise for people with MS “The Role of Exercise in Modifying outcomes of People with Multiple Sclerosis” (MSTEP) [13]. The fatigue monitoring component occurred over the first 14 days from study entry with the time divided into two consecutive periods of 7 days, one prior to exercise prescription and one after exercise prescription. Ethical consideration for this study was obtained from McGill University Health Centre (MUHC) at the Montreal Neurological Hospital.
Study population
Participants were those agreeing to the trial which recruited from two university hospital MS clinics. To be included, people had to be diagnosed with MS after 1994, aged 19 to 65 years, and capable of walking 100 meters without walking aid (PDDS stage: Early cane). Participants were excluded if they: (i) were already exercising three or more times per week; (ii) had any additional illness that restricted their function; (iii) had experienced a relapse during the past 30 days (included only if they were stable for more than 30 days after relapse); and (iv) showed difficulty reading, understanding, or speaking either English or French. We included only persons diagnosed after 1994 to have a more homogeneous group of people with respect to diagnostic criteria and access to disease modifying therapies (DMT) [14-16].
Measurement
The demographic information such as age, gender, disability status was collected at baseline. The Patient Determined Disease Steps (PDDS) was used as a measure of disability. The PDDS is the patient version of the Expanded Disability Status Scale (EDSS) [17] and shows a high degree of correlation with the clinical measure [18].
Physical activity was measured using a uniaxial accelerometer, ActivPALTM. Accelerometers have been shown to have excellent psychometric properties in persons with MS and are considered a feasible and acceptable tool to measure physical activity in this population [19]. Reliability estimates are 0.85 for vigorous activities and 0.90 on rhythmic activities [19]. Information on average number of steps/day, energy expenditure, time spent sitting/lying, standing, stepping, number of transitions, and cadence was recorded.
Fatigue perception was measured using a 0 to 10 Visual Analogue Scale (VAS) with 0 indicating not at all fatigued and 10 worst fatigues. Participants were provided with a diary to record their VAS rating of fatigue perception on four times every day at 08:00, 12:00, 16:00, and 21:00 hours. As the accelerometer did not distinguish between sitting and lying, participants also recorded in this diary when they went to bed and when they got up to provide an estimate of hours spent lying down.
Procedure
Eligible participants were identified from clinic records and were mailed a post-card about the study. Potential participants contacted the study centre directly or were telephoned by the research coordinator to be informed of the study and, for those interested, an appointment was made for an assessment. At this first visit, the consent was obtained, questionnaires and physical performance tests were completed, and an accelerometer was fixed to the thigh. At a second visit, 7 days later, the accelerometer was retrieved, randomization was carried out, the participants were given their exercise program, and a second accelerometer was put in place. This was to be worn for another seven days and then mailed back in a specially designed and addressed envelope. Thus, participants wore the accelerometer continuously, for a total of 14 days, 7 days pre-exercise prescription and 7 days post-exercise prescription. The analysis focused on linking fatigue perception to physical activity the next day and vice versa as shown in Figure 1.
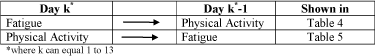
Figure 1: The analysis focused on linking fatigue to physical activity the next
day.
Data analysis
Descriptive statistics were calculated to describe the cohort and summarize, across days and time-periods, fatigue values and all physical activity parameters. The distribution of steps/day was also calculated after a log transformation.
The first analysis linked time of day to highest fatigue perception. For fatigue the maximum number of data points per person is 56 (2 time points X 7 days X 4 times of fatigue measurement every day- 8:00, 12:00, 16:00 and 21:00 hours). For each person, the time of the day where the fatigue was highest was identified and coded “1”, and all other time points were coded “0”. The proportion of persondays with the highest fatigue was calculated for each time point. To estimate the impact of time of day on highest fatigue perception, Generalized Estimating Equations (GEE), a generalized linear model that takes into account when estimating regression parameters that observations are correlated within subject [20], was used. The autoregressive correlation structure was used. The estimates (β) were used to compute odds ratio (OR) along with 95% confidence intervals (CI). The odds of fatigue at 12:00, 16:00, and 21:00 hours were estimated relative to the odds of fatigue at 8:00 hours. Single imputation was used for missing data and all statistical assumptions were accounted for.
GEE was also used to link fatigue perception to physical activity and vice versa as shown in Figure 1. The model also included age, gender, and disability (PDDS). All statistical analysis was carried out using Statistical Analysis System (SAS) Version 9.1, function ‘SAS PROC GENMOD’.
Results and Discussion
Table 1 shows characteristics of the sample. The mean age of the 40 participants was 44 years and 75% were women. The majority had a university degree (62%) and 78% had not changed their work status due to their MS. About 42% of participants had mild sensory symptoms, which did not interfere with their activity levels as seen on Patient Determined Disease Steps (PDDS). Also 25% had difficulty walking, and performing physically demanding activities.
Variables
Mean (SD)
N (%)
Age (years)
44 (9.5)
Women
30 (75%)
Education
High School
3 (8%)
Junior College/ Technical School
11 (30%)
University
23 (62%)
Employment
No change due to MS
29 (78%)
Began to work fewer hours
8 (22%)
6MWT(m)
503.6 (108)
Gait Speed (m/sec)
1.39 (0.30)
<0.8m/sec
1 (3%)
0.8-1.0m/sec
5 (13%)
>1.0 m/sec
31 (84%)
EQ VAS
73.4 (13.3)
PDDS (score)
Normal (0)
17 (42.5%)
Mild Disability (1)
7 (17.5%)
Moderate Disability(2)
7 (17.5%)
Gait Disability/Early cane (3/4)
9 (22.5%)
Table 1: Key characteristics of study participants (n=40).
Table 2 presents mean fatigue perception scores at four different time points during the day, averaged over seven days, pre- and postexercise prescription. Across all persons, at all time points and days, the full range (0-10) of fatigue scores was observed (data not shown). At 8:00 hours, the average fatigue for the pre-exercise prescription period was 1.8 out of 10 (SD: 2.36). There was a trend for increasing fatigue perception over time, both pre- and post-exercise prescription. To express the increase in fatigue perception over time, the time period of highest fatigue perception was identified for each personday, and expressed as a percent. With 40 participants and 14 days of data collection, the total number of person-days is 560 (40x14). The highest fatigue perception was reported at 8:00 hours for 15.2%. In contrast, the highest fatigue perception was reported at 21:00 hours for 34% of person-days. The odds of having highest fatigue at 12:00, 16:00 and 21:00 hours, relative to the odds at 8:00 hours increased with later time points. At 21:00 hours the odds ratio (OR) was 5.70 (95% CI: 2.78 – 11.69).
Time of measurement
Fatigue Pre- exercise prescription
Mean (SD)
Fatigue Post- exercise prescription
Mean (SD)
(%person-days of highest fatigue)
Odds Ratio*
95%CI
08:00 hours
1.8 (2.36)
1.7 (2.13)
15.2%
Referent
12:00 hours
1.8 (2.03)
2.3 (2.21)
18.0%
0.91
0.49, 1.69
16:00 hours
2.7 (2.35)
2.9 (2.38)
32.8%
2.84
1.44, 5.61
21:00 hours
3.1 (2.78)
3.0 (2.57)
34.0%
5.70
2.78, 11.69
*Odds ratio derived from GEE to account for repeated measures of fatigue
Table 2: Mean values of fatigue perception at four time points (averaged over days), pre- and post-exercise prescription, and proportion of person-days per time point with highest level of fatigue perception.
Table 3 shows the average steps/day pre- and post-exercise prescription, which was 6245 and 7317, respectively. The SD was large illustrating a non-normal distribution and, hence, the median, 25%ile (Q1), 75%ile (Q3), and range are presented. To meet the assumptions of the future regression analysis, using steps/day as the outcome variable predicted by fatigue perception the day before (Figure 1), it was log transformed and the values are presented. The median steps/ day for the two time periods did not differ statistically (902; 95% CI: -808, 1130). Also shown are the other parameters of activity obtained from the accelerometer. The results showed that all parameters were stable over this short time period.
Variables (n=40)
Pre-Exercise Prescription (n= 262 person-days)
Post-Exercise Prescription (n= 238 person-days)
Overall Steps/day
Mean (SD)
Median
Q1 – Q3
Range
6245 (3682)
5846
3486 – 8348
0 – 17656
7317 (4314)
6748
4182 – 9880
0 – 20826
Overall Log Steps/day
Mean (SD)
Median
Q1 – Q3
Range
8.58 (0.81)
8.69
8.22 – 9.03
1.79 – 9.78
8.56 (1.33)
8.82
8.37 – 9.20
0.69 – 9.94
Median [IQR]
Difference (95% CI)
Steps/day
5846 (4862)
6748 (5698)
902 (-808, +1130)
Energy Expenditure (MET.h) Time spent
32.9 (2.0)
33.4 (2.4)
0.5 (-0.66, +0.42)
Sleeping (hours)
8.5 (1.6)
8.2 (1.6)
-0.3 (-3, +1.6)
Sitting (hours)*
9.7 (3.5)
9.6 (3.7)
- 0.1 (-0.24, +0.09)
Standing (hours)
4.2 (2.7)
4.4 (2.8)
0.2 (-0.75, +0.57)
Stepping (hours)
1.3 (1.0)
1.5 (1.1)
0.2 (-0.17, +0.14)
Transitioning (sit to stand)
53.0 (33)
55.0 (32)
2 (-3.68, +2.14)
Cadence (steps/min)
Low (0-90)
Moderate (90-100)
High (110-140)
2665 (2242)
1616 (1572)
483 (1672)
2925 (2248)
1891 (1842)
972 (2562)
260 (-623, +291)
275 (-301, +485)
489 (-581, +494)
*Subtracted average hours for sleep
Inter Quartile Range (IQR): is the difference between the value at the 25%ile (Q1) and 75%ile (Q3). E.g. the median for EE is 32.9 with IQR of 2.0. The 25%ile is 30.9 and the 75%ile is 34.9.
Table 3: Steps/day (overall and log transformed), and median values for physical activity parameters, averaged over all days and time points, pre- and post-exercise prescription.
Table 4 shows the impact of end-of-day fatigue perception on physical activity (log steps/day) the next day adjusted for age, gender, and disability. The estimates in this table show the log transformed values for steps/day. For the pre-exercise period, there was no effect of end-of-day fatigue on next-day steps/day (95% CI: -0.04, 0.05). Participants, over 40 years walked an average of 5482 steps/day (SD: 3715), and those under 40 years, walked 6594 steps/day (SD: 4114). There was no difference in average steps/day by age (95% CI: (-0.69, 0.18), nor gender (95% CI: 0.21, 0.34). However, for people with gait disability, there was a statistically significant effect with the higher fatigue perception predicting lower next-day (log) steps/day (-0.48; 95% CI: (-0.96, -0.03). For the post-exercise prescription period, endof- day fatigue perception did not impact on next-day steps/day (95% CI: -0.01, 0.11). Also there was no difference on steps/day by age, gender, or disability.
Parameter
Steps/day
Mean (SD)
Log (Steps/day)
Mean (SD)
Estimates* (95%CI)
Pre-Exercise Prescription
Fatigue
8:00,12:00,16:00 hours
Referent
21:00 hours
0.003 (-0.04, 0.05)
Age
>40 years
5482 (3715)
8.48 (0.89)
Referent
≤40 years
6594 (4114)
8.77 (0.55)
-0.25 (-0.69, 0.18)
Gender
Women
5710 (3984)
8.56 (0.87)
Referent
Men
6378 (3399)
8.62 (0.53)
0.06 (0.21, 0.34)
Disability (PDDS)
Normal
6662 (3924)
8.60 (0.62)
Referent
Mild disability
5583 (4261)
8.33 (1.83)
-0.26 (-0.87, 0.36)
Moderate disability
4939 (4859)
8.38 (0.68)
-0.12 (-0.54, 0.31)
Gait disability/early cane
5157 (2705)
8.40 (0.36)
-0.49 (-0.96, -0.03)
Post-Exercise Prescription
Fatigue
8:00,12:00,16:00 hours
Referent
21:00 hours
0.08 (0.02, 0.14)
Age
>40 years
5990 (4204)
8.48 (1.36)
Referent
≤40 years
6695 (5714)
8.76 (1.24)
-1.01 (-1.9, -0.11)
Gender
Women
6486 (4611)
8.77 (0.67)
Referent
Men
5156 (5222)
7.68 (2.55)
-1.40 (-3.6, 0.80)
Disability (PDDS)
Normal
6460 (4941)
8.45 (1.41)
Referent
Mild disability
5133 (5207)
8.19 (0.37)
0.43 (-0.26, 1.11)
Moderate disability
8745 (5392)
8.53 (0.74)
0.44 (-0.22, 1.10)
Gait disability/early cane
5392 (3264)
8.51 (0.34)
0.86 (-0.39, 2.10)
*Estimates derived from GEE to account for repeated measure of steps/day; all estimates are adjusted for the other variables in the model. PDDS=Patient Determined Disease Steps
Table 4: Results of the regression analysis, pre- and post-exercise prescription, linking end-of-day fatigue perception, age, gender, and disability to physical activity (log steps/day) the next day.
Table 5 presents the distribution of average fatigue perception, pre- and post-exercise prescription and the results of the regression analysis, relating physical activity throughout the day to next-day fatigue perception considering also age, gender, and disability. For the pre-exercise period, there was no effect of physical activity throughout the day on next-day fatigue perception (95% CI: -0.00, 0.00). Post-exercise prescription, physical activity throughout the day did not impact on next-day fatigue perception (95% CI: -0.00, 0.00). Also there was no effect of age, gender, and disability on fatigue perception levels was maintained.
Parameter
Mean (SD)
Estimates* (95% CI)
Pre-Exercise Prescription
1000 Steps/day
0.00 (-0.00, 0.01)
Age
>40 years
2.47 (1.97)
Referent
≤40 years
2.35 (1.86)
0.07 (-0.67, 0.81)
Gender
Women
2.34 (2.05)
Referent
Men
2.44 (1.40)
-0.08 (-0.72, 0.56)
Disability (PDDS)
Normal
2.08 (1.76)
Referent
Mild disability
2.41 (1.87)
0.39 (-0.29, 1.06)
Moderate disability
3.32 (2.96)
1.32 (-0.35, 2.99)
Gait disability/early cane
2.58 (1.49)
0.01 (-0.84, 0.86)
Post-Exercise prescription
1000 Steps/day
0.00 (-0.00, 0.01)
Age
>40 years
2.86 (1.92)
Referent
≤40 years
1.74 (2.03)
0.17 (-0.90, 1.25)
Gender
Women
1.71 (0.02)
Referent
Men
1.67 (1.83)
-0.19 (-1.11, 0.74)
Disability (PDDS)
Normal
2.36 (2.08)
Referent
Mild disability
1.68 (1.91)
-0.69 (-1.80, 0.42)
Moderate disability
4.03 (2.14)
-0.03 (-1.70, 1.64)
Gait disability/early cane
2.55 (1.57)
-0.77 (-1.93, 0.39)
*Estimates derived from GEE to account for repeated measure of fatigue; all estimates are adjusted for the other variables in the model
PDDS: Patient Determined Disease Steps
Table 5: Results of the regression analysis, pre- and post-exercise prescription, linking physical activity throughout the day, age, gender, and disability to fatigue perception the next day.
Discussion and Conclusion
This study confirmed that fatigue perception in MS varies during the day, being lowest in morning and highest at night. People with MS were much more likely to report their highest fatigue perception at 21:00 hours (OR: 5.57; 95%CI: 1.00, 2.44) than at 8:00 hours (Table 2).
Few studies have addressed the longitudinal course of MS fatigue perception. We were able to find five studies that addressed this temporal sequence and salient features of these studies are presented in Table 6. This topic has been addressed over 4 decades with the largest study [21] comprising 102 people. The measures of fatigue perception varied, however, four out of five studies concluded that fatigue perception was highest in the afternoon, and one study demonstrated that fatigue perception was highest in morning; two studies did not record fatigue perception later than the afternoon. The analysis linking fatigue perceptions to time were mainly qualitative. The previous evidence was insufficient to establish a definite pattern in fatigue perception variability because of a number of measurement limitations. In contrast to this, our study which was designed to address these methodological limitations, we found that fatigue perception was highest at night (Table 2). Our results were included in Table 6 for comparison purposes.
Author (Year)
N
Fatigue measures
Results
Drawback
Krupp (1988)
32
Direct question
(When do you experience your highest fatigue?)
Fatigue highest in afternoon
No analysis
No measurement
Morris (2002)
14
Visual Analogue Scale (10:00 and 15:00 hours for one day)
Fatigue increases from morning to afternoon
(t[13]=-3.14, p=0.008)
No recording of fatigue in evening or night
Schwid (2002)
23
Rochester Fatigue Diary (fatigue measured every hour for seven days)
High fatigue in morning and it decreases in afternoon
No analysis
Mills
(2008)
40
Semi-structured Interview
Fatigue highest in afternoon
No measurement
Feys
(2012)
102
Rochester Fatigue Diary (9:00, 12:00, 15:00 hours for one day)
High fatigue at 12:00 and 15:00 hours compared to 9:00 hours
(F[2,100]=38.1; p<0.0001)
No recording of fatigue in evening or night
Selukar
(2015)
40
VAS 0 – 10 (08:00, 12:00, 16:00, 21:00)
Highest fatigue 21:00 (OR: 5.57; 95%CI: 1.00,2.44)
Sample size small, time frame limited to 14 days
Table 6: Literature review on diurnal variation of fatigue in MS.
The second aim of our study was to estimate the temporal relationship between fatigue perception and next-day physical activity measured using an accelerometer. The average step count pre-exercise prescription was 6245 ± 3682. This was similar to the step count reported by Dlugonski et al. on 645 people with MS (5903 ± 3185) [22] and similar to accumulated data from Motl et al. [23] for people with PDDS of 0 to 2, the majority of our patients.
We were concerned that wearing the accelerometer for the first time would increase exercise engagement a participants knew they are being monitored and, as a result, there would be little additional change after exercise prescription. Although the difference in average steps/day pre- and post-exercise prescription was not statistically different, out of 560 person-days, 212 person-days (38%) showed an increase in steps/day by more than 800, which is considered clinically meaningful in MS [24]. While they had only just been given their exercise program, this shows that some people respond early to exercise recommendation and that the novelty of the device may not have been such a stimulus to exercise. While, there is evidence from a systematic review for the monitoring effect [25], the studies included used pedometers, devices that give immediate feedback unlike the accelerometers we used, that do not.
The results did not show any association between fatigue perception and physical activity over time indicating that in this sample of persons, fatigue perception at night was not associated with physical activity the next day and vice versa. Previous crosssectional literature showed weak correlation [21,26-29]. In contrast to the studies conducted in past, the current study used a longitudinal design, fatigue perception was measured several times in a day, physical activity was measured directly, and appropriate statistical approach was used to deal with this non-independence of data.
Evidence supports the role of physical activity in people with MS. In a meta-analysis on 39 randomized controlled trials, Kuspinar et al indicated that exercise reduces fatigue (ES=0.6). In contrast to this, it was previously believed that physical activity will induce fatigue due to rise in body temperature [30]; our study did not find evidence that being physically active has any negative effect on fatigue perception.
This study has several limitations. According to the taxonomy of fatigue, it has the components of perceived fatigue and performance fatigability [1]. This study was only based on the measure of perceived fatigue. For future studies, it is recommended that performance fatigability should also be assessed while measuring perceived fatigue. This study followed up activity levels only after one week postexercise prescription, for the purposes of looking at relationships before alteration with a new exercise program. These results should be confirmed with long term exercise programs. In addition, we only related fatigue on one day to physical activity the next day and vice versa but not at a more granular level such as fatigue after activity or activity after highest time fatigue. While this would be interesting, it is beyond the scope of this paper.
In conclusion, this study contributed evidence for variation of daily fatigue in people with MS. Fatigue perception is lowest in the morning, goes on increasing as the day progresses, and is highest at night. Our study concluded that, over this relatively short time-frame, fatigue and physical activity were independent of each other. This finding should be reassuring to people with MS who wish to increase physical activity but fear negative impacts on fatigue perception.
The current study has several clinical implications. For clinicians, knowing the pattern of daily fatigue perception could be beneficial to provide an idea as to when and how often should this symptom be assessed throughout the day. The above results are also beneficial for providing an effective self-management program. People with MS should be made aware of this pattern of fatigue. This would help them to effectively use techniques like energy conservation and activity pacing. Also since this study confirmed the diurnal variation in fatigue it is recommended for future research that fatigue scores should not be averaged throughout the day as this might not provide true estimates of this construct. These results should be considered before designing a physical activity intervention, and people with MS should be recommended to participate in the exercise programs despite their levels of fatigue perception. With exercise, in long term follow up, it is anticipated that there would not only be an increase in physical activity, but also a reduction in fatigue perception.
References
- Kluger BM, Krupp LB, Enoka RM. Fatigue and fatigability in neurologic illnesses: proposal for a unified taxonomy. Neurology. 2013; 80: 409-416.
- Feys P, Gijbels D, Romberg A, Santoyo C, Gebara B, de Noordhout BM, et al. Effect of time of day on walking capacity and self-reported fatigue in persons with multiple sclerosis: a multi-center trial. Mult Scler. 2012; 18: 351-357.
- Krupp LB, Alvarez LA, LaRocca NG, Scheinberg LC. Fatigue in multiple sclerosis. Arch Neurol. 1988; 45: 435-437.
- Mills RJ, Young CA. A medical definition of fatigue in multiple sclerosis. QJM. 2008; 101: 49-60.
- Morris ME, Cantwell C, Vowels L, Dodd K. Changes in gait and fatigue from morning to afternoon in people with multiple sclerosis. J Neurol Neurosurg Psychiatry. 2002; 72: 361-365.
- Schwid SR, Covington M, Segal BM, Goodman AD. Fatigue in multiple sclerosis: current understanding and future directions. J Rehabil Res Dev. 2002; 39: 211-224.
- Kayes NM, McPherson KM, Taylor D, Schlüter PJ, Kolt GS. Facilitators and barriers to engagement in physical activity for people with multiple sclerosis: a qualitative investigation. Disabil rehabil. 2011; 33: 625-642.
- Asano M, Finlayson ML. Meta-analysis of three different types of fatigue management interventions for people with multiple sclerosis: exercise, education, and medication. Mult Scler Int. 2014; 2014.
- Asano M, Duquette P, Andersen R, Lapierre Y, Mayo NE. Exercise barriers and preferences among women and men with multiple sclerosis. Disabil Rehabil. 2013; 35: 353-361.
- Asano M, Dawes DJ, Arafah A, Moriello C, Mayo NE. What does a structured review of the effectiveness of exercise interventions for persons with multiple sclerosis tell us about the challenges of designing trials? Mult Scler. 2009; 15: 412-421.
- Kuspinar A, Rodriguez AM, Mayo NE. The effects of clinical interventions on health-related quality of life in multiple sclerosis: a meta-analysis. Mult Scler. 2012; 18: 1686-1704.
- Rampello A, Franceschini M, Piepoli M, Antenucci R, Lenti G, Olivieri D, et al. Effect of aerobic training on walking capacity and maximal exercise tolerance in patients with multiple sclerosis: a randomized crossover controlled study. Phys Ther. 2007; 87: 545-555.
- Mayo NE, Bayley M, Duquette P, Lapierre Y, Anderson R, Bartlett S. The role of exercise in modifying outcomes for people with multiple sclerosis: a randomized trial. BMC Neurol. 2013; 13: 69.
- Jacobs LD, Cookfair DL, Rudick RA, Herndon RM, Richert JR, Salazar AM, et al. Intramuscular interferon beta-1a for disease progression in relapsing multiple sclerosis. The Multiple Sclerosis Collaborative Research Group (MSCRG) Ann Neurol. 1996; 39: 285-294.
- Marriott JJ, Miyasaki JM, Gronseth G, O'Connor PW; Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology. Evidence Report: The efficacy and safety of mitoxantrone (Novantrone) in the treatment of multiple sclerosis: Report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology. Neurology. 2010; 74: 1463-1470.
- Polman CH, O'Connor PW, Havrdova E, Hutchinson M, Kappos L, Miller DH, et al. A randomized, placebo-controlled trial of natalizumab for relapsing multiple sclerosis. N Engl J Med. 2006; 354: 899-910.
- Kurtzke JF. Rating neurologic impairment in multiple sclerosis: an expanded disability status scale (EDSS). Neurology. 1983; 33: 1444-1452.
- Learmonth YC, Motl RW, Sandroff BM, Pula JH, Cadavid D. Validation of patient determined disease steps (PDDS) scale scores in persons with multiple sclerosis. BMC Neurol. 2013; 13: 37.
- Kayes NM, Schluter PJ, McPherson KM, Leete M, Mawston G, Taylor D. Exploring actical accelerometers as an objective measure of physical activity in people with multiple sclerosis. Arch Phys Med Rehabil. 2009; 90: 594-601.
- Liang KY, Zeger SL. Longitudinal data analysis using generalized linear models. Biometrika. 1986; 73: 13-22.
- Feys P, Gijbels D, Romberg A, Santoyo C, Gebara B, de Noordhout BM, et al. Effect of time of day on walking capacity and self-reported fatigue in persons with multiple sclerosis: a multi-center trial. Mult Scler. 2012; 18: 351-357.
- Dlugonski D, Pilutti LA, Sandroff BM, Suh Y, Balantrapu S, Motl RW. Steps per day among persons with multiple sclerosis: variation by demographic, clinical, and device characteristics. Arch phys med rehabil. 2013; 94: 1534-1539.
- Motl RW, Pilutti LA, Learmonth YC, Goldman MD, Brown T. Clinical importance of steps taken per day among persons with multiple sclerosis. PLoS One. 2013; 8: e73247.
- Motl RW, Pilutti LA, Learmonth YC, Goldman MD, Brown T. Clinical importance of steps taken per day among persons with multiple sclerosis. PLoS One. 2013; 8: e73247.
- Bravata DM, Smith-Spangler C, Sundaram V, Gienger AL, Lin N, Lewis R, et al. Using pedometers to increase physical activity and improve health: a systematic review. JAMA. 2007; 298: 2296-2304.
- Krupp LB, Alvarez LA, LaRocca NG, Scheinberg LC. Fatigue in multiple sclerosis. Arch Neurol. 1988; 45: 435-437.
- Morris ME, Cantwell C, Vowels L, Dodd K. Changes in gait and fatigue from morning to afternoon in people with multiple sclerosis. J Neurol Neurosurg Psychiatry. 2002; 72: 361-365.
- Schwid SR, Covington M, Segal BM, Goodman AD. Fatigue in multiple sclerosis: current understanding and future directions. J Rehabil Res Dev. 2002; 39: 211-224.
- Mills RJ, Young CA. A medical definition of fatigue in multiple sclerosis. QJM. 2008; 101: 49-60.
- White AT, Wilson TE, Davis SL, Petajan JH. Effect of precooling on physical performance in multiple sclerosis. Mult Scler. 2000; 6: 176-180.