
Research Article
Austin J Mult Scler & Neuroimmunol. 2016; 3(1): 1024.
Comorbidities of Multiple Sclerosis Patients Treated at the Illinois Neurological Institute (INI) Multiple Sclerosis Center
Valenzuela MR¹, Cooley KL², Kimberly L², Gonia L², Taylor AJ¹, Paris BL³ and Asche CV³*
¹Neuro-ophthalmology, Moran Eye center, University of Utah School of Medicine, USA
²Illinois Neurological Institute , OSF Saint Francis Medical Center, USA
³Department of Medicine / Center for Outcomes Research, University of Illinois College of Medicine at Peoria, USA
*Corresponding author: Carl V Asche, University of Illinois College of Medicine at Peoria, One Illini Drive, Peoria, USA
Received: November 12, 2015; Accepted: February 18, 2015; Published: February 22, 2016
Abstract
Background: Multiple sclerosis (MS) is a chronic disease with high costs and impact on quality of life. Understanding the prevalence of comorbidities is important because comorbidities complicate management of MS.
Objective: Describe the comorbidities of MS patients seen at the Illinois Neurological Institute (INI) MS center.
Methods: Retrospective review of MS patients seen at the INI MS center from February 2011 to February 2014. Demographics and comorbidities were compared to a prior study of National Health and Wellness Survey (NHWS) 2009 data (N=549).
Results: A total of 592 patients were included in the study. Most frequent comorbidities were pain (45.0%), high cholesterol (28.8%) and hypertension (27.3%).
Conclusions: Primary care physicians and general neurologists should be aware that comorbidities exist and may complicate treatment.
Keywords: Multiple sclerosis; Prevalence; Retrospective studies; Comorbidity; Adult; Humans
Introduction
An estimated 4,00,000 people in the United States have multiple sclerosis (MS) with approximately 10,000 new cases diagnosed every year [1]. In the US, prevalence of MS ranges from 47.2 to 109.5 per 1,00,000 population, with the rate affected by sunlight exposure, gender, age, and ethnicity [2]. Most individuals with MS experience initial symptoms between the ages of 20 and 40 years; therefore, this disease may have significant impact over time on their health, employment, productivity, and quality of life [3]. Multiple sclerosis is included in the World Health Organization (WHO) top 100 diseases affecting quality of life. Among those with MS, 30% are severely disabled and 70% are unemployed. As a result, the economic costs associated with MS are significant [3]. We spend 445 million USD on direct MS care annually [4], however annual indirect costs exceed 10 billion USD [2,5].
Managing MS requires treatment to help prevent disease progression and control a number of conditions including fatigue, bladder or bowel dysfunction, urinary tract infections, muscular weakness, spasticity, joint contractures, difficulty walking, tremor, vision disturbances, pain, loss of cognition, depression and anxiety, speech and swallowing difficulty, sexual dysfunction, and pressure ulcers [6]. These conditions are related to the progression of MS and may require physical therapy, occupational therapy, pharmacotherapy, medical devices, and counseling. Treating MS is intended to help avoid relapses leading to temporary disability and to delay progression of the disease which leads to permanent disability.
Comorbidities among MS patients complicate management. Cost of illness is higher, and health-related quality of life is lower for MS patients with impaired mobility [5], which is affected by comorbid conditions [7,8]. The prevalence of comorbid conditions with MS is high; 37% of patients with MS had at least one physical comorbidity [9] and 48% of patients with MS had at least one mental comorbidity [10]. Adverse health factors such as smoking and obesity are also common in MS [8,9,11,12]. These comorbidities and lifestyle factors may affect the delay between symptom onset and diagnosis, disability progression, and health related quality of life [7,9,11,12]. Comorbidity in MS adds to complexity of managing the disease.
Multiple studies have reported the prevalence of comorbid conditions in patients with MS [7,9,13-17], but the studies do not use a consistent framework for categorizing comorbidities. An improved understanding of the prevalence and nature of underlying comorbidities among those with MS is merited as it will serve to further develop treatment protocols, thus improving outcomes among MS patients. Population based studies of individuals with MS are needed along with appropriate comparator groups [8]. The objective of this paper is to describe the demographics, geographic patient distribution, and comorbidities of MS patients seen at the INI MS center. To assist the reader in interpreting our data, we compare the individual comorbidity prevalence in the INI MS Center population to the MS comorbidity prevalence reported by Stewart and colleagues [16].
Patients and Methods
This is a retrospective review of MS patients seen at the Illinois Neurological Institute (INI) from February 2011 to February 2014. The INI MS Center serves approximately 600 people living with multiple sclerosis in Central Illinois, many of whom live in rural areas and travel to the city of Peoria for treatment. (Figure 1) shows the geographic area served by the INI MS Center and (Table 1) summarizes the demographic characteristics of patients seen at the INI MS Center (N=593). This study was approved by the IRB. A retrospective review of inpatient and outpatient claims data was undertaken using ICD-9 codes to determine comorbid conditions; these codes are presented in (Table 2).
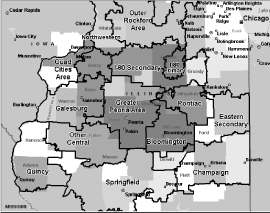
Figure 1: Geographic distribution of patients seen at the INI MS Center.
INI MS Patients
NHWS MS Cohort
P Value
N=592
N=549
n
Mean/ %
n
Mean/ %
Gender
Age (years)
592
50.0
549
48.6
Male
153
25.8%
196
35.7%
<0.0005**
Female
439
74.2%
353
64.3%
<0.0005**
Health History
Use Alcohol
239
40.4%
333
60.7%
<0.0005**
Smoke/Use Tobacco
170
28.7%
177
32.2%
0.196
Health Insurance
Insured
571
96.5%
494
90.0%
<0.0005**
Uninsured
21
3.5%
55
10.0%
<0.0005**
Body Mass Index (BMI)
Underweight
16
2.7%
18
3.3%
0.569
Normal
181
30.6%
161
29.3%
0.645
Overweight
174
29.4%
179
32.6%
0.241
Obese
217
36.7%
177
32.2%
0.116
Declined to report
0
0.0%
14
2.6%
<0.0005**
**statistically significant difference
Table 1: Demographic characteristics of patients seen at the INI MS Center and in the NHWS Cohort.
Type
Comorbidity
ICD-9 Codes (xx=include all subcodes)
Neurologic
Pain
307.8, 307.80, 307.89, 338, 338.1, 338.11, 338.12, 338.18, 338.19, 338.2, 338.21, 338.22, 338.28, 338.29, 338.3, 338.4, 350.2, 379.91, 388.71, 388.72, 440.22, 569.42, 625, 719.4, 719.40, 719.41, 719.42, 719.43, 719.44, 719.45, 719.46, 719.47, 719.48, 719.49, 724.1, 729.5, 780.96, 784.1, 784.92, 786.5, 786.50, 786.51, 786.52, 786.59, 787.3, 788.99, 789.0, 789.00, 789.01, 789.02, 789.03, 789.04, 789.05, 789.06, 789.07, 789.09
Headache
339.00, 339.01, 339.02, 339.03, 339.04, 339.05, 339.09, 339.10, 339.11, 339.12, 339.20, 339.21, 339.22, 339.3, 339.41, 339.42, 339.43, 339.44, 339.81, 339.82, 339.83, 339.84, 339.85, 339.89, 346.00, 346.01, 346.02, 346.03, 346.10, 346.11, 346.12, 346.13, 346.20, 346.21, 346.22, 346.23, 346.30, 346.31, 346.32, 346.33, 346.40, 346.41, 346.42, 346.43, 346.50, 346.51, 346.52, 346.53, 346.70, 346.71, 346.72, 346.73, 346.80, 346.81, 346.82, 346.83, 346.90, 346.91, 346.92, 346.93, 784.0, 346.0, 346.1, 346.2, 346.8, 346.9
Migraine
346.00, .01, .10, .11, .20, .90, .91
Restless Leg Syndrome
333.94
Stroke
337.01, 430, 431, 432.0, 432.1, 432.9, 433.0, 433.00, 433.01, 433.2, 433.20, 433.21, 433.3, 433.30, 433.31, 433.8, 433.80, 433.81, 433.9, 433.90, 433.91, 434.00, 434.01, 434.10, 434.11, 434.90, 434.91, 435.0, 435.1, 435.2, 435.3, 435.8, 435.9, 436, 437.2, 437.5, 437.6, 437.7, 437.8, 437.9, 780.2
Epilepsy
345.00, 345.01, 345.10, 345.11, 345.2, 345.3, 345.40, 345.41, 345.50, 345.51, 345.60, 345.61, 345.70, 345.71, 345.80, 345.81, 345.90, 345.91, 780.31, 780.32, 780.33, 780.39, 345.0, 345.1, 345.4, 345.5, 345.6, 345.7, 345.8, 345.9, 780.3
Dementia
294.20, 331.83, 780.93
Movement Disorders (e.g., Parkinson's Disease)
333.2, 333.3, 333.4, 333.5, 333.6, 333.7, 333.72, 333.79, 333.81, 333.82, 333.83, 333.84, 333.85, 333.89, 333.90, 333.91, 333.93, 333.99, 334.0, 334.1, 334.2, 334.3, 334.4, 334.8, 334.9, 335.0, 335.10, 335.11, 335.19, 335.21, 335.22, 335.23, 335.24, 335.29
Alzheimer's Disease
331.0
Psychiatric
Sleep Difficulties
307.41, 307.42, 307.43, 307.44, 307.45, 307.46, 307.47, 307.48, 307.49, 327.00, 327.01, 327.02, 327.09, 327.10, 327.11, 327.12, 327.13, 327.14, 327.15, 327.19, 327.20, 327.21, 327.22, 327.23, 327.24, 327.25, 327.26, 327.27, 327.29, 327.30, 327.31, 327.32, 327.33, 327.34, 327.35, 327.36, 327.39, 327.40, 327.41, 327.42, 327.43, 327.44, 327.49, 327.51, 327.52, 327.53, 327.59, 327.8, 333.94, 347.00, 347.01, 347.10, 780.02, 780.1, 780.50, 780.51, 780.52, 780.53, 780.54, 780.55, 780.56, 780.57, 780.58, 780.59
Depression
296.20, 296.32, 311
Anxiety
313.21, 313.22, 309.81, 300.00, 300.09, 300.10, 293.84, 300.01, 300.02, 300.20, 300.21, 300.22, 300.23, 300.29, 300.3, 300.5, 300.89, 300.9, 308.0, 308.1, 308.2, 308.3, 308.4, 308.9, 313.0, 313.1, 313.3, 313.82, 313.83
Insomnia
327.00, .01, .02, .09, 780.51, .52
Panic Disorder
300.01
Social Anxiety Disorder
300.23
Bipolar Disorder
296.50, .52, .65, .70, .80
Generalized Anxiety Disorder
300.02
Alcoholism
305.00
Obsessive Compulsive Disorder
300.3
Post-Traumatic Stress Disorder
309.81
Narcolepsy
347.00, .01
Attention Deficit Disorder
314.0, .01
Phobias
300.29
Cardiovascular
Hypertension
401.1, 401.9, 796.2
High Cholesterol
272.0, .1, .2, .3, .4
Angina
413.0, 413.9
Arrythmia
427.9
Mini-Stroke/Transient Ischemic Attack
435.9
Heart Attack
410, 410.0, 410.00, 410.01, 410.02, 410.1, 410.10, 410.11, 410.12, 410.2, 410.20, 410.21, 410.22, 410.3, 410.30, 410.31, 410.32, 410.4, 410.40, 410.41, 410.42, 410.5, 410.50, 410.51, 410.52, 410.6, 410.60, 410.61, 410.62, 410.7, 410.70, 410.71, 410.72, 410.8, 410.80, 410.81, 410.82, 410.9, 410.90, 410.91, 410.92
Deep Vein Thrombosis
453.40, .41, .42
Pulmonary Embolism
415.19
Congestive Heart Failure
428.0, 428.1, 428.20, 428.21, 428.22, 428.23, 428.30, 428.31, 428.32, 428.33, 428.40, 428.41, 428.42, 428.43, 428.9, 398.91
Atrial Fibrillation
427.31
Left Ventricular Hypertrophy
429.3
Peripheral Vascular Disease
443.9
Other comorbidities
Arthritis
716.40, 716.41, 716.42, 716.43, 716.44, 716.45, 716.46, 716.47, 716.48, 716.49, 716.50, 716.51, 716.52, 716.53, 716.54, 716.55, 716.56, 716.57, 716.58, 716.59, 716.60, 716.61, 716.62, 716.63, 716.64, 716.65, 716.66, 716.67, 716.68, 716.80, 716.81, 716.82, 716.83, 716.84, 716.85, 716.86, 716.87, 716.88, 716.89, 716.90, 716.91, 716.92, 716.93, 716.94, 716.95, 716.96, 716.97, 716.98, 716.99, 718.10, 718.11, 718.12, 718.13, 718.14, 718.15, 718.17, 718.18, 718.19
Heartburn
787.1
Over Active Bladder Wet (urinary leakage)
596.51
Abdominal Pain
789.xx
Gastroesophageal Reflux Disease
456.1, 456.21, 530.0, 530.1, 530.10, 530.11, 530.12, 530.13, 530.19, 530.2, 530.20, 530.21, 530.3, 530.4, 530.5, 530.6, 530.8, 530.81, 530.83, 530.84, 530.85, 530.89, 530.9
Abdominal Bloating
787.3, 789.3
Irritable Bowel (constipation and/or diarrhea)
564.1
Chronic Constipation
564.00
Nail Fungus
110.1, 681.02, 681.11
Hay Fever
477.8, 477.9
Asthma
492.22, 493.xx, 786.07
Thyroid Condition
240.0, 240.9, 241.0, 241.1, 241.9, 242.00, 242.01, 242.10, 242.11, 242.20, 242.21, 242.30, 242.31, 242.40, 242.41, 242.80, 242.81, 242.90, 242.91, 243, 244.0, 244.1, 244.2, 244.3, 244.8, 244.9, 245.0, 245.1, 245.2, 245.3, 245.4, 245.8, 245.9, 246.0, 246.1, 246.2, 246.3, 246.8, 246.9, 794.5
Diabetes (Type 1 or Type 2)
249.00, 249.01, 249.10, 249.11, 249.20, 249.21, 249.30, 249.31, 249.40, 249.41, 249.50, 249.51, 249.60, 249.61, 249.70, 249.71, 249.80, 249.81, 249.90, 249.91, 250.00, 250.01, 250.02, 250.03, 250.10, 250.11, 250.12, 250.13, 250.20, 250.21, 250.22, 250.23, 250.30, 250.31, 250.32, 250.33, 250.40, 250.41, 250.42, 250.43, 250.50, 250.51, 250.52, 250.53, 250.60, 250.61, 250.62, 250.63, 250.70, 250.71, 250.72, 250.73, 250.80, 250.81, 250.82, 250.83, 250.90, 250.91, 250.92, 250.93, 790.2, 790.21, 790.22, 790.29, 791.5, 791.6, V45.85, V53.91, V65.46
Diarrhea (frequent)
787.91
Fibromyalgia
729.1
Table 2: ICD-9 Codes used to identify comorbid conditions.
This project includes a comparison to the MS comorbidities analysis from the 2009 (N = 75,000) wave of the National Health and Wellness Survey (NHWS) [16]. The NHWS is an Internetbased annual study of the healthcare attitudes and behaviors of a representative sample of US adults. Stewart and colleagues analyzed physician-diagnosed comorbidities of patients with MS (N=549) and without MS (N=74,451) [16,18]. The NHWS data set included patientreported demographics (age, gender, race/ethnicity, education, income, employment status and health insurance type), health status information (exercise, alcohol use, smoking and Body Mass Index) and comorbid conditions diagnosed by a physician [16,18].
The demographics and clinical characteristics of the INI MS Center patients were compared to the MS patients in the NHWS sample, using the individuals without MS as controls [16]. Demographics, health status, and comorbidities were compared between individuals with diagnosed MS and controls using bivariate analyses. Bivariate analyses were evaluated by chi-square tests for categorical variables and t-tests for continuous variables.
Results
A total of 592 patients were included in the study. We compared the prevalence of clinically documented comorbidities in our study population to the prevalence of self-reported physician-diagnosed comorbidities in the NHWS sample of patients with MS. A p-value of <0.05 was considered statistically significant. Comorbidities such as psychiatric illness, cardiovascular disease, gastrointestinal disease, and endocrine diseases were all significantly lower among the INI MS patients compared to the NHWS MS cohort (p<0.001). There was also a statistically significant difference between insured females and underinsured males (p<0.001). Please refer to (Table 3) for Neurologic comorbidities, (Table 4) for Psychiatric comorbidities, (Table 5) for Cardiovascular comorbidities and (Table 6) for other comorbidities observed in our study population.
Neurologic comorbidity
INI MS Patients
NHWS MS Cohort
p value
N=
593
N=549
n
%
n
%
Pain
267
45.0%
304
56.7%
<0.0005**
Headache
103
17.4%
299
55.8%
<0.0005**
Migraine
40
6.7%
158
29.5%
<0.0005**
Restless Leg Syndrome
22
3.7%
100
18.7%
<0.0005**
Stroke
32
5.4%
28
5.2%
0.823
Epilepsy
29
4.9%
21
3.9%
0.377
Dementia
38
6.4%
11
2.0%
<0.0005**
Movement Disorders (Including Parkinson's Disease)
7
1.2%
11
2.0%
0.269
Alzheimer's Disease
0
0.0%
10
1.9%
0.001**
**statistically significant difference
Table 3: Neurologic comorbidities.
Psychiatric comorbidity
INI MS Patients
NHWS MS Cohort
p value
N=593
N=549
n
%
n
%
Sleep Difficulties
135
22.8%
232
43.3%
<0.0005**
Depression
104
17.5%
213
39.7%
<0.0005**
Anxiety
85
14.3%
177
33.0%
<0.0005**
Insomnia
42
5.3%
153
28.5%
<0.0005**
Panic Disorder
5
0.5%
44
8.2%
<0.0005**
Social Anxiety Disorder
1
0.2%
43
8.0%
<0.0005**
Bipolar Disorder
19
2.2%
42
7.8%
0.001**
Generalized Anxiety Disorder
10
1.5%
38
7.1%
<0.0005**
Alcoholism
3
0.4%
36
6.7%
<0.0005**
Obsessive Compulsive Disorder
1
0.2%
31
5.8%
<0.0005**
Post-Traumatic Stress Disorder
3
0.3%
24
4.5%
<0.0005**
Narcolepsy
1
0.2%
22
4.1%
<0.0005**
Attentions Deficit Disorder
6
1.3%
20
3.7%
0.003**
Phobias
1
0.2%
17
3.2%
<0.0005**
**statistically significant difference
Table 4: Psychiatric comorbidities.
Cardiovascular comorbidities
INI MS Patients
NHWS MS Cohort
p value
N=593
N=549
n
%
n
%
Hypertension
162
27.3%
180
33.6%
0.044**
High Cholesterol
171
28.8%
173
32.3%
0.325
Angina
4
0.7%
26
4.8%
<0.0005**
Arrythmia
6
1.0%
26
4.8%
<0.0005**
Mini-Stroke/Transient Ischemic Attack
8
1.3%
25
4.7%
0.001**
Heart Attack
5
0.8%
19
3.5%
0.002**
Deep Vein Thrombosis
14
2.4%
17
3.2%
0.447
Pulmonary Embolism
9
1.5%
14
2.6%
0.219
Congestive Heart Failure
9
1.5%
12
2.2%
0.404
Atrial Fibrillation
13
2.2%
11
2.0%
0.824
Left Ventricular Hypertrophy
1
0.2%
9
1.7%
0.010**
Peripheral Vascular Disease
12
2.0%
8
1.5%
0.463
**statistically significant difference
Table 5: Cardiovascular comorbidities.
Other comorbidities
INI MS Patients
NHWS MS Cohort
p value
N=593
N=549
n
%
n
%
Arthritis
18
3.0%
158
29.5%
<0.0005**
Heartburn
4
0.7%
150
28.0%
<0.0005**
Over Active Bladder Wet (uriniary leakage)
11
1.9%
124
23.1%
<0.0005**
Abdominal Pain
99
16.7%
98
18.3%
0.606
Gastroeosphageal Reflux Disease
71
12.0%
96
17.9%
0.009**
Abdominal Bloating
14
2.4%
93
17.3%
<0.0005**
Irritable Bowel (with constipation and/or diarrhea)
12
2.0%
88
16.4%
<0.0005**
Chronic Constipation
40
6.7%
80
14.9%
<0.0005**
Nail Fungus
8
1.3%
77
14.4%
<0.0005**
Hay Fever
50
8.4%
72
13.4%
0.011**
Asthma
48
8.1%
71
13.2%
0.008**
Thyroid Condition
94
15.9%
63
11.7%
0.031**
Diabetes (Type 1 or Type 2)
70
11.8%
61
11.4%
0.713
Diarrhea (frequent)
51
8.6%
57
10.6%
0.305
Fibromyalgia
58
9.8%
54
10.1%
0.975
**statistically significant difference
Table 6: Other comorbidities.
Discussion
This study presents findings on comorbidities of MS patients seen at the INI MS center. However, our study does not include assessment of the quality-of-life or costs associated with increasing levels of disability with multiple sclerosis. It is also important to note that the NHWS was a self-reported survey and our study was based on claims data. Variations in study designs between NHWS and our cohort might preclude exact comparisons, however both our study and NHWS looked at different comorbidities associated with multiple sclerosis.
Comorbidity is common in MS and may include conditions such as anxiety, depression, bipolar disorder, other autoimmune disorders, gastrointestinal dysfunction, cardiovascular disease and other endocrine disorders. A study done by Marrie and colleagues assessed the prevalence comorbidities and found that 77% of MS patients had one or more self-reported physical comorbidity, 37% of which were judged to be “very likely to be accurately self-reported” and requiring treatment [9]. In Canada, Warren and colleagues found that the mean number of comorbidities was 1.6 and that 10% have 8 or more comorbidities [19].
Given that INI MS center is a University- based program with an abundance of different medical specialties, our data might be biased towards the occurrence of more comorbidities. Prevalence of dementia and thyroid condition was higher in our clinically-based data than in the self-reported data. Prevalence of bipolar disorder, diabetes, and fibromyalgia were about the same in the self-reported data and our clinically-based data. All other comorbidities compared had a higher prevalence in the self-reported data. The exact reason why comorbidities such as psychiatric illness, cardiovascular disease, and other medical conditions were significantly lower in our MS patients when compared to the NHWS MS cohort is unknown. Although patients may incorrectly report a comorbidity that has not been diagnosed by a clinician in the NHWS, it may also be the case that the INI MS Center record does not reflect comorbidities that were diagnosed and managed by clinicians outside of their health system. However, prevalence of comorbid neurologic conditions including pain, headache, migraine, restless leg syndrome, and Alzheimer’s disease was higher in the NHWS MS cohort than in our MS clinic population.
These findings are surprising and deserves further study. Patients may simply use over-the-counter medications for comorbidities such as hay fever and nail fungus and not mention it to the clinical team. However, comorbidity such depression may not be reflected in the clinical record if the patient was diagnosed and received successful treatment prior to the onset of MS, or it may be unrecognized due to the confluence with MS symptoms [20]. Regardless of the underlying causes of the different rates of comorbidities, our research adds to the existing evidence suggesting that comorbidity is common in patients with MS. Our data shows a variety of comorbidities associated with MS, supporting the need for different subspecialties. Primary care physicians and general neurologists should be aware that comorbidities exist and may complicate treatment. This awareness will inform treatment of MS patients, which should be individualized and tailored to specific needs.
MS is complex to treat since each patient’s clinical course and response/tolerability to Disease Modifying Therapy (DMT) varies. Adding additional comorbidities to the clinical picture further complicates the treatment plan. As mentioned earlier, this study validates that coordination of care among physicians is essential. However, additional opportunities to improve MS care at the bedside exist as well. OSF Saint Francis Medical Center, INI and the Center for Outcomes Research at University of Illinois College of Medicine Peoria are collaborating on the development of an MS Flowsheet Database. We expect that the MS Flowsheet Database will improve dissemination of knowledge among the clinical team about each patient’s individual MS picture. This registry also has the potential to provide outcome data in reportable format, offer an opportunity for future research projects, and promote healthcare cost savings. Perhaps more importantly, the MS Flowsheet Database will provide custom reports about each patient’s individual MS picture and facilitate discussion and understanding between the patient, the clinical team, and other care providers. This data will be used to inform future studies to improve management and health outcomes among MS patients seen at the INI MS center.
Acknowledgement
The authors would like to acknowledge the work of the staff at the INI MS Center in collecting and analyzing the data used for this study, specifically Kim Wankel and Victoria L. Parry. We would also like to thank Mr. Larry Wallden, Dr. Patrick Elwood, Dr. Sara Rusch, Dr. Anthony Avellino, Dr. Jorge Kattah, and Dr. Dennis Garwacki for their ongoing leadership and support of this work.
Funding Acknowledgement
We would like to thank the Central Illinois MS Council for funding this research. The Central Illinois MS Council & MS Clinic Fund is a not-for-profit volunteer organization dedicated to transforming healthcare for MS patients and their families in Central Illinois.
References
- Tullman MJ. Overview of the epidemiology, diagnosis, and disease progression associated with multiple sclerosis. Am J Manag Care. 2013; 19: 15-20.
- Noonan CW, Williamson DM, Henry JP, Indian R, Lynch SG, Neuberger JS. The prevalence of multiple sclerosis in 3 US communities. 2010; 7: 12.
- NIH, National Institute of Neurological Disorders and Stroke. Multiple Sclerosis: Hope Through Research. 2015.
- Lad SP, Chapman CH, Vaninetti M, Steinman L, Green A, Boakye M. Socioeconomic trends in hospitalization for multiple sclerosis. 2010; 35: 93- 99.
- Coleman CI, Sidovar MF, Roberts MS, Kohn C. Impact of mobility impairment on indirect costs and health-related quality of life in multiple sclerosis. 2013; 8: 54756.
- NICE, National Institute for Health and Care Excellence. Multiple sclerosis Clinical guideline 186: Management of multiple sclerosis in primary and secondary care. 2014.
- Marrie RA, Horwitz R, Cutter G, Tyry T, Campagnolo D, Vollmer T. Comorbidity delays diagnosis and increases disability at diagnosis in MS. 2009; 72: 117-124.
- Marrie RA, Horwitz RI. Emerging effects of comorbidities on multiple sclerosis. 2010; 9: 820-828.
- Marrie R, Horwitz R, Cutter G, Tyry T, Campagnolo D, Vollmer T. Comorbidity, socioeconomic status and multiple sclerosis. 2008; 14: 1091-1098.
- Marrie RA, Horwitz R, Cutter G, Tyry T, Campagnolo D, Vollmer T. The burden of mental comorbidity in multiple sclerosis: frequent, underdiagnosed, and undertreated. 2009; 15: 385-392.
- Kang JH, Chen YH, Lin HC. Comorbidities amongst patients with multiple sclerosis: a population-based controlled study. 2010; 17: 1215-1219.
- Marrie RA, Horwitz R, Cutter G, Tyry T, Vollmer T. Association between comorbidity and clinical characteristics of MS. 2011; 124: 135-141.
- Kister I, Caminero AB, Monteith TS, Soliman A, Bacon TE, Bacon JH. Migraine is comorbid with multiple sclerosis and associated with a more symptomatic MS course. 2010; 11: 417-425.
- Li Y, Munger KL, Batool-Anwar S, De Vito K, Ascherio A, Gao X. Association of multiple sclerosis with restless legs syndrome and other sleep disorders in women. 2012; 78: 1500-1506.
- Marrie RA, Hanwell H. General health issues in multiple sclerosis: comorbidities, secondary conditions, and health behaviors. Continuum (Minneap Minn) 2013; 19: 1046-1057.
- Comorbid illness among individuals with multiple sclerosis. AAN; 2011.
- Bamer AM, Cetin K, Johnson KL, Gibbons LE, Ehde DM. Validation study of prevalence and correlates of depressive symptomatology in multiple sclerosis. 2008; 30: 311-317.
- Pomerantz D. Discussion of NHWS MS Sample Methodology with Dave Pomerantz, Senior Vice President Client Consulting at Kantar Health. 2014.
- Warren SA, Turpin KVL, Pohar SL, Jones CA, Warren KG. Comorbidity and Health-Related Quality of Life in People with Multiple Sclerosis. 2015; 11: 6-16.
- Majmudar S, Schiffer RB. Why Depression Goes Unrecognized in Multiple Sclerosis Patients. 2015;11: 154-159.