Letter to the Editor
Austin J Nephrol Hypertens. 2014;1(2): 1006.
A Unique Case of Hypophosphatemia in the Setting of Oliguric Acute Kidney Injury
Kamel M1*, Thajudeen B1, Popovtzer M2
1Department of Nephrology, University of Arizona medical center, USA
2Department of Nephrology, Southern Arizona Veterans Affairs Health Care System, USA
*Corresponding author: Mahmoud Kamel, Department Of Nephrology, University of Arizona medical center, 1501, N Campbell Avenue, Tucson, AZ, 85724, USA
Received: July 07, 2014; Accepted: July 09, 2014; Published: July 11, 2014
Keywords
Hypophosphatemia; Acute kidney injury; Refeeding syndrome
Hypophosphatemia is a frequently encountered electrolyte disorder in critically ill patients with acute kidney injury (AKI) and usually occurs in the background of renal replacement therapy [1]. It is associated with high mortality in these patients. Although hypophosphatemia associated with refeeding syndrome is common in critically ill patients, its occurrence in the presence of acute kidney injury is uncommon [2]. We report a case of hypophosphatemia in a critically ill patient with AKI during the course of hospitalization. A 65 year old male patient was admitted with generalized weakness, fatigue and frequent falls. His past medical history was significant for alcoholic cirrhosis. Social history was significant for heavy alcohol drinking (6 beers every day for at least 30 years). He was cachectic, pale and weak. Rest of the examination was unremarkable except for diminished breath sounds at both lung bases, distended abdomen with fluid thrill and 3+ pitting edema of lower extremities. Pertinent laboratory tests at the time of admission showed hemoglobin 8.9 gm/dl, serum creatinine 1 mg/dl, sodium 141mmol/L, phosphorus 3.2 mg/dl, and ammonia 86mcg/dl. Although initial diagnosis was decompensated liver disease, he subsequently developed respiratory failure due to aspiration pneumonia and was placed on mechanical ventilation. During his stay in intensive care unit (ICU), he developed oliguric AKI. On the third day of ICU stay, high calorie, and low protein enteral tube feeding was started. In next few days decrease in serum phosphorus was noted (Table 1). He did not have any diarrhea during this period His medications included meropenem, pantoprazole, thiamine, albumin, azithromycin, fluconazole, and folic acid. In the absence of definite renal as well as gastrointestinal loses and in the background of malnutrition as well as history of alcoholism, hypophosphatemia secondary to refeeding syndrome was suspected. Although he was treated with intravenous phosphate as well as oral phosphorus, phosphate level continued to drop. Hence high calorie formula was stopped and tube feeding was reinitiated at lower caloric dose which was gradually increased over the next few days reaching the goal over a week. This along with supplementation with intravenous and oral phosphate stabilized and normalized the serum phosphorus. Renal function subsequently improved and creatinine returned to baseline (Table 1).
BUN
mg/dl
Cr
mg/dl
K
mmol/L
HCO3
mmol/L
Corrected Calcium
mg/dl
PO4
mg/dl
25-OH vitamin D
PTH
Admission day
16
1
3.7
21
8.4
3.2
ICU Day 1
22
1.2
3.9
21
8.4
3.3
ICU Day 3 #
30
1.8
4.1
19
8.0
3.9
ICU Day 5
34
2.4
4.4
18
7.8
2.2
37
70
ICU Day 7
50
2.7
4.4
20
7.6
1.7
ICU Day 9
49
2.7
4.5
20
7.8
1.1
Discharge day
20
1.1
3.9
23
8.6
3.6
Table 1: Serum chemistries at admission and during the course in ICU.
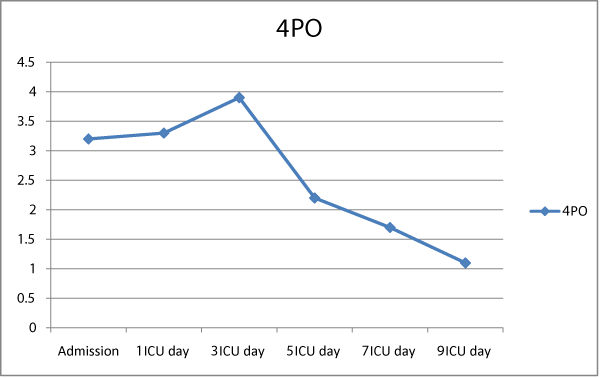
The use of high calorie, low protein tube feeds used in this patient might be responsible for the induction of refeeding syndrome [3,4]. The high carbohydrate content will stimulate insulin secretion shifting the phosphorus intracellularly. There is paucity of data on how to carry out feeding in these patients who are deemed to be at risk for metabolic complications. A stepped up feeding regimen which is balanced in calories and protein should be used. Initial calorie intake should be restricted to 10cal/kg/day with increase to normal over a week [5]. In addition to keeping a close eye on the levels it is recommended to supplement electrolytes including phosphorus either in the tube feeds or intravenously based on the serum levels. (Figure 1)
Figure 1: Serum PO4 from admission till day 9.
References
- Yang Y, Zhang P, Cui Y, Lang XB, Yuan J, Jiang H, et al. Hypophosphatemia during continuous veno-venous hemofiltration is associated with mortality in critically ill patients with acute kidney injury. Crit Care. 2013; 17: R205.
- Walmsley RS. Refeeding syndrome: screening, incidence, and treatment during parenteral nutrition. J Gastroenterol Hepatol. 2013; 28: 113-117.
- Fiaccadori E, Parenti E, Maggiore U. Nutritional support in acute kidney injury. J Nephrol. 2008; 21: 645-656.
- McCarthy MS, Phipps SC. Special nutrition challenges: current approach to acute kidney injury. NutrClinPract. 2014; 29: 56-62.
- Bunge PD, Frank LL. A case of refeeding syndrome in a marine recruit. Mil Med. 2013; 178: 511-515.