Clinical Image
Austin Neurosurg Open Access. 2014;1(1): 1002.
Teaching Neuroimages: Sagittal Sinus Pseudo-Occlusion: a Case of Bilateral AVM
Beckman JM, Van Gompel JJ and Kan P*
Department of Neurosurgery and Brain Repair, University of South Florida, USA
*Corresponding author: Peter Kan, Department of Neurosurgery and Brain Repair, USF Health South Health Tampa Center, 2 Tampa General Circle, Tampa, Florida 33606
Received: March 10, 2014; Accepted: April 06, 2014; Published: April 08, 2014
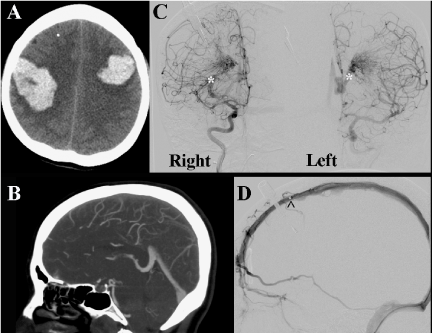
A 49–year–old female presented with sudden onset headache and rapidly declined to a GCS of 4T. Head CT demonstrated bilateral posterior frontal hemorrhages suggestive of sagittal venous thrombosis (Figure 1). CT venogram suggested absence of sagittal sinus flow consistent with occlusion. DSA showed bilateral thalamic AVMs with a patent superior sagittal sinus as explored by venous catherization (Figure 1). Bilateral symmetrical cerebral AVMs are extremely rare [1]. In this case, classically bilateral parenchymal hemorrhages are suggestive of venous thrombosis, here supported by CTV, however definitive DSA demonstrated sinus patency. This case serves as an example of AVM shunting mimicking thrombosis on CTV imaging.
Figure 1: (A) Bilateral hemorrhages suspicious for venous occlusion (axial CT) B) Absence of sagital sinus filling (CTV). C) ICA injections demonstrating bilateral thalamic AVM with high flow features. (∗ectactic venous drainage with arterial phase) D) Sagital sinus patency as demonstrated by venous catheter (^ shows distal tines of catheter).
References