
Research Article
Austin Neurosurg Open Access. 2015; 2(4): 1039.
Imaging of Cranial Nerves
Tanrikulu L1,2*, Hastreiter P¹, Buchfelder M¹ and Naraghi R1,3
¹Department of Neurosurgery, University of Erlangen- Nuremberg, Germany
²Department of Neurosurgery, Hannover Nordstadt Hospital, Germany
³Department of Neurosurgery, Bundeswehrkrankenhaus Ulm, Germany
*Corresponding author: Levent Tanrikulu, Department of Neurosurgery, Hannover Nordstadt Hospital, Haltenhoffstr, Germany
Received: August 24, 2015; Accepted: September 25, 2015; Published: September 28, 2015
Abstract
Objective: In this study we present our experience in imaging and image processing of the anatomy of the cranial nerves V-XI and their relationships to corresponding vasculature. The objective of this study was to show the possibility and the technique of 3D visualization of cranial nerve anatomy and corresponding vessels in the posterior fossa. The relationships of the cranial nerves at the brainstem to the tiny vessel were examined with high-resolution magnetic resonance imaging.
Material and Methods: We present the technique of imaging and image processing by 1.5 Tesla high-resolution magnetic resonance imaging and threedimensional (3D) visualization by direct volume rendering. The cranial nerve anatomy is visualized referring the root exit/entry zones of the cranial nerves, anatomical courses within the cisterns of the posterior cranial fossa and the corresponding vessels. Patients with trigeminal neuralgia, hemi facial spasm and glosso pharyngeal neuralgia were studied.
Results: With highly-resolute MR imaging and 3D visualization by direct volume rendering the anatomy of the cranial nerves V, VI, VII, VIII, IX, X and XI were delineated non-invasively in the pre- and intraoperative setup of the surgical domain. There were no disturbances in anatomical visualization.
Conclusion: Cranial nerve imaging by highly resolute MR imaging and 3D visualization by direct volume rendering gives the opportunity for non-invasive anatomical analysis of cranial nerve topography and corresponding vasculature and brainstem. This contributes for diagnostic and therapeutic decisions and for surgical-anatomical teaching.
Keywords: Cranial nerves; Imaging; Image processing; Neuroanatomy
Abbreviations
2D: Two-Dimensional; 3D: Three-Dimensional
Introduction
Cranial nerve anatomy and corresponding vasculature still remains a challenging field for surgeons. There is a need for noninvasive anatomical visualization of the complex topographical details of the cranial nerves and corresponding vessels especially in patients with trigeminal neuralgia, hemi facial spasm, and glosso pharyngeal neuralgia and for patients with tumors within the posterior fossa such as acoustic neuronal, meningiomas or metastases. The objective of this study was to show the possibility and the technique of 3D visualization of cranial nerve anatomy and corresponding vessels in the posterior fossa. The relationships of the cranial nerves at the brainstem to the tiny vessel were examined with high-resolution magnetic resonance imaging. The goal of this article is to present our experience in imaging of cranial nerve anatomy and corresponding vessels and the ability to transfer acquired two-dimensional (2D) anatomical data into more interesting three-dimensional (3D) visualization in order to get a maximum of anatomical information on the individual cranial nerve anatomy prior and during surgery.
Material and Methods
From the years 2003 until 2006 we routinely examined and treated patients with cranial nerve dysfunctions such as trigeminal neuralgia (41 patients), hemi facial spasm (25 patients) and glosso pharyngeal neuralgia (2 patients) [1-3]. All patients underwent high-resolution 1.5 Tesla magnetic resonance (Siemens Magnetom Sonata, Erlangen, Germany) imaging described as constructive interference in the steady state (MRI-CISS, Figure 1a-c) [4,5]. In MRI-CISS sequences the cisterns filled with Cerebrospinal Fluid (CSF) are depicted with highest intensity and the containing anatomical structures such as the interesting cranial nerves and corresponding vessels are delineated hypo intensely (Figure 1). Therefore the individual threedimensional anatomy of cranial nerves, vessels and the brainstem is visualized in each patient non-invasively and the position of the anatomical structures can be varied into all directions. The MRICISS sequences undergo segmentation (Figure 2) and subsequent 3D visualization by direct volume rendering (Figure 3) [4]. The result is a 3D objects representing the real, individual patient anatomy with topographical details of cranial nerves and surrounding structures as the brainstem and vessels (Figure 4). Our patients underwent micro vascular decompression after sub occipital, retro sigmoid craniotomy as described by Jannetta [6].
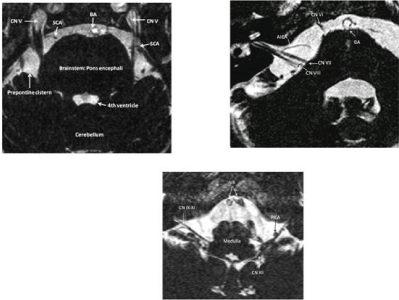
Figure 1: Slice of original high-resolution MR CISS (Constructive
interference in the steady state) image. Note: the CSF space (prepontine
cistern, fourth ventricle) are delineated highly hyper intense, so that the
containing cranial nerves (CN V: trigeminal nerves, CN VI: adducent
nerve, CN VII: facial nerve, CN VIII: vestibulocochlear nerve, CN IX: gloss
pharyngeal nerve, CN X: vagus nerve, CN XI: accessory nerve, CN XII:
hypoglossal nerve), vessels (AICA: Anterior Inferior Cerebellar Artery, BA:
Basilar Artery, SCA: Superior Cerebellar Artery, PICA: Posterior Inferior
Cerebellar Artery, VA: Vertebral Artery) and the brainstem (Pons encephali)
are depicted hypo intensely, so that a clear differentiation between these
structures are obtained.
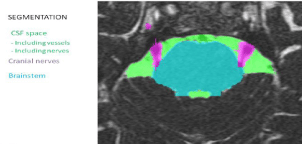
Figure 2: Original procedure of Segmentation. The CSF spaces are
segmented semi automatically (green color) with the corresponding vessels,
the cranial nerves (purple color) and the brainstem (turquoise color) in each
patient. After this procedure the obtained segmented data is processed
by direct volume rendering where the segmented volumes CSF space,
cranial nerves and brainstem are transferred to opacity/transparency values
and different colors. The CSF space is transferred to a high opacity/low
transparency volume, so that the containing vessels are visualized and
the brainstem and the cranial nerves are transferred to high opacity/low
transparency volumes.
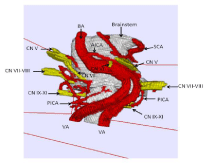
Figure 3: Resulting original 3D visualization generated after direct volume
rendering from segmentation. Note: One can vary the position of the
3D object into each direction in the space. The cranial nerves V-XI, the
corresponding vessels and the brainstem are visualized in a non-invasive
way. (CN V: trigeminal nerve, CN VI: abducent nerve, CN VII: facial nerve,
CN VIII: vestibulocochlear nerve, CN IX: gloss pharyngeal nerve, CN X: vagus
nerve, CN XI: accessory nerve, BA: Basilar Artery, SCA: Superior Cerebellar
Artery, AICA: Anterior Inferior Cerebellar Artery, VA: Vertebral Artery, PICA:
Posterior Inferior Cerebellar Artery).
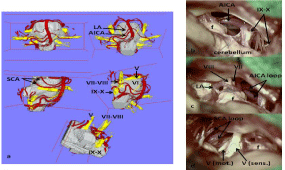
Figure 4: Real, original, individual 3D visualization in a patient with right
sided trigeminal neuralgia containing the interesting cranial nerves and
corresponding vessels. Figure 4a shows the variation of the position of 3D
visualization in correspondence to the surgical domain (V: trigeminal nerve,
VI: abducent nerve, VII: facial nerve, VIII: vestibulocochlear nerve, IX: gloss
pharyngeal nerve, X: vagus nerve, XI: accessory nerve, BA: Basilar Artery,
VA: Vertebral Artery, SCA: Superior Cerebellar Artery, LA: Labyrinthine
Artery, AICA: Anterior Inferior Cerebellar Artery, f: Floccules’ Cerebelli, mot.:
Motor Division of Trigeminal Nerve, sens.: Sensory Division of Trigeminal
Nerve).
Results
We were able to visualize the cranial nerves (V, VI, VII, VIII, IX, X, and XI), the brainstem and the corresponding vasculature in all examined patients (100%) without any medical or technical disturbances such as major pulsation artifacts. All patients underwent surgery (micro vascular decompression) and 3D visualization of the neurovascular conflicts were applied to the pre- and intraoperative setup without any disturbance. The surgeon was able to see preand intraoperative in addition to the available 2D MRI imaging the real, individual cranial nerve anatomy in a 3D object with possible variation of its position into each direction, so that the coaxial view into the surgical domain could always be compared to the noninvasively reproduced 3D visualization of the patient.
Discussion
Two-dimensional images by magnetic resonance imaging do not contribute for the complex and detailed anatomical characteristics and relationships between the brainstem, cranial nerves and corresponding vessels in the posterior cranial fossa. With 3D visualization of the 2D imaged with direct volume rendering we were able to generate real, individual, anatomical representations of our examined patients prior to surgery. MRI CISS is surely superior in detailed anatomical imaging to “routine” MR sequences where the cranial nerve anatomy cannot be visualized sufficiently [5], because MRI-CISS allows a clear differentiation of nerves and vessels within the CSF spaces. One limitation of our method is the existence of pulsation artifacts induced by the pulsation of the basilar and vertebral arteries, while these artifacts could be deleted within the segmentation process by manual corrections in order to have a clear view over the surface of the brainstem. Image fusion of the original MRI-CISS with MRI-TOF (time of flight angiography) is also possible to enhance the vascular visualization of the arteries to optimize detailed delineation of the arterial courses within the posterior fossa. The 3D visualization acts as a non-invasive original anatomical visualization of original patientbased data, so that the surgeon can view the expected surgical and topographical neurovascular conflicts of the individual patient from the routinely acquired magnetic resonance imaging. In all cases the 3D visualizations of the applied MRI-CISS data were compared to the intraoperative surgical field and the anatomy could be verified in all examined patients. This shows that the MRI-CISS data was definitely useful and predictive and the data from intraoperative findings to the preoperative evaluation was very useful. This ensures anatomical and clinical diagnostics and extensively supports the intraoperative procedures of micro vascular decompression to achieve sufficient vascular decompression of the entire root entry/exit zone of the regarding cranial nerve. The 3D representations can be viewed from all directions, so that the observer can see the global anatomical environment of the cranial nerves especially with interesting focus on corresponding vasculature. Segmentation demands high anatomical knowledge on the topography of the posterior cranial fossa. Therefore it also extends anatomical knowledge on the individual patient anatomy. The position of the 3D representations can be manipulated and zoomed to all directions, so that it acts as a neuroendoscopic tool, where the surgeon can non-invasively observe the individual patient anatomy from each angle with a panoramic view. The 3D visualization represented a precondition for detailed anatomical analysis and understanding of volumetric data from the MR imaging. We were able to draw classifications of the neurovascular anatomy of facialvestibulocochlear- nerve complex in patients with hemi facial spasm [4], because we routinely applied the technique of intraoperative 3D visualization during micro vascular decompression in the operating theatre. This provided us a very advantageous possibility of anatomical information before and during surgery and contributed for anatomical and operative safety and clinical outcome of the patient. 3D visualization could also be applied for the visualization of other disease such as pituitary tumors for the visualization of the optic nerves and the optic chiasm. Further studies should be implemented to a more spectrum of neurological/neurosurgical diseases with the focus on non-invasive, high-end anatomical, three-dimensional visualization.
Conclusion
With 3D visualization we were able to show the real, individual cranial nerve anatomy and corresponding vasculature and the brainstem in patients with neurovascular compression syndromes. This method of non-invasive anatomical exploration of the cranial nerves and vessels is very useful for topographical analysis and classifications of the variable vascular compression courses within the posterior cranial fossa. This method also contributes to diagnostic and therapeutic decisions in patient care and to surgical-anatomical teaching.
References
- Naraghi R, Tanrikulu L, Troescher-Weber R, Bischoff B, Hecht M, Buchfelder M, et al. Classification of neurovascular compression in typical hemi facial spasm: three-dimensional visualization of the facial and the vestibulocochlear nerves. Neurosurg J. 2007; 107: 1154-1163.
- Tanrikulu L, Hastreiter P, Troescher-Weber R, Buchfelder M, Naraghi R. Intraoperative three-dimensional visualization in micro vascular decompression. J Neurosurg. 2007; 107: 1137-1143.
- Tanrikulu L, Hastreiter P, Richter G, Doerfler A, Naraghi R. Virtual neuroendoscopic: MRI-based three-dimensional visualization of the cranial nerves in the posterior cranial fossa. Br J Neurosurg. 2008; 22: 207-212.
- Hastreiter P, Naraghi R, Tomandl B, Bonk A, Fahlbusch R. Analysis and 3-dimensional visualization of neurovascular compression syndromes. Acad Radiol. 2003; 10: 1369-1379.
- Tomandl BF, Hastreiter P, Rezk-Salama C, Engel K, Ertl T, Huk WJ, et al. Local and remote visualization techniques for interactive direct volume rendering in neuroradiology. RadioGraphics 2001; 21: 1561-1572.
- Jannetta PJ. Trigeminal neuralgia. Neurosurgery. 1986; 18: 677.