
Case Report
Austin Neurosurg Open Access. 2016; 3(1): 1044.
Persistent Sinus Thrombosis Caused By Superior Sagittal Sinus Stenosis Following an Open Depressed Skull Fracture
Huseyin Ozevrena* and Adnan Cevizb
Departments of Neurosurgery, Dicle University School of Medicine, Turkey
*Corresponding author: Huseyin Ozevren, Departments of Neurosurgery, Dicle University School of Medicine, Diyarbakir, Turkey
Received: November 12, 2015; Accepted: February 03, 2016; Published: February 05, 2016
Abstract
Background: Head injuries caused by falls from height are not uncommon in developing countries due to a lack of safety standards. Herein, a unique case of this injury a tile fragment that penetrated the Superior Sagittal Sinus (SSS) and its surgical management are described.
Case Description: The case of a 17-year-old male with a depressed skull fracture overlying the posterior third of the superior sagittal sinus is presented. Emergent exploration was performed to prevent complications such as infection, sinus thrombosis and delayed development of intracranial hypertension.
Conclusion: Depressed skull fractures overlying the major venous sinuses, particularly in the midline, should always be considered a potential source of sinus injury. Although a compound depressed fracture of the SSS was managed to remove the contaminated wound and bone fragments in spite of the risk of fatal venous hemorrhage, the unique nature of this injury warranted surgical management. This case indicates that, in such a scenario, adherence to neurosurgical principles can ensure a good outcome. Furthermore, an MRI venography is recommended for all patients who have an open depressed skull fracture overlying the SSS because of the potential risk for venous sinus stenosis and thrombosis, which may be developed at a later date.
Keywords: Depressed skull fracture; Tile fragment; 3D-CT reconstruction; Superior sagittal sinus
Abbreviations
SSS: Superior Sagittal Sinus; GCS: Glasgow Coma Scale; MRI: Magnetic Resonance Imaging; 3D-CT: Three-Dimensional Computed Tomography
Introduction
Head injuries are one of the most common causes of mortality and morbidity, particularly in developing countries. They usually manifest as skull fractures involving cranial bones. They are commonly seen after fall from heights, road traffic accidents, physical attacks and other injuries [1,2]. Skull fractures are roughly classified into linear, depressed and compound types. Linear fractures are the most common, followed by depressed skull fractures [3]. Compound fractures may be associated with venous sinus laceration or compression in approximately 10% of cases [4].
Various foreign bodies penetrating the cranium have been described, often requiring operative intervention. However, the management of compound depressed fractures of the Superior Sagittal Sinus (SSS) is generally nonoperative because of the high possibility of death due to uncontrollable bleeding from the venous sinuses [5]. Herein, a unique case of injury (due to a tile fragment causing a depressed skull fracture over the SSS) and its surgical management and follow-up are described.
Case Report
A 17-year-old male presented with a history of fall of a tile fragment from the roof of construction zone with a height of 12 feet three hours prior to presentation. He had a history of transient loss of consciousness. On examination, vital signs were stable. His eyes were opened upon pain, he had no verbal response and he was bilaterally localizing to noxious stimuli with a GCS score of eight (E2V1M5). His pupils were equally round and reactive to light. Laboratory studies revealed electrolytes within normal limits. There was no evidence of anemia, thrombocytopenia or thrombocytosis. Routine coagulation studies, including Prothrombin Time/Internationalized Normalized Ratio (PT/INR) and Partial Thromboplastin Time (PTT) were normal. Further laboratory investigation was performed, accounting for antithrombin III activity, protein C level and activity, protein S (free and total) level and activity, fibrinogen level, activated protein C resistance, anticardiolipin antibody level and prothrombin level. Test results were within normal limits. Computed Tomography (CT) of the brain was normal, but 3D-CT (Three-Dimensional Computed Tomography) reconstruction of the bony windows of the cranial vault showed a depressed skull fracture of the middle occipital bone just anterior to the lambdoid suture (Figure 1). Although bleeding from the SSS posed a problem, the head was positioned appropriately. Continuous saline irrigation was conducted while a burr hole opening and craniectomy were performed around the bone fragment. There was a subgaleal clot around the bone fragment. When the fragment was carefully removed, bleeding occurred from the SSS. The roof of the sinus was reconstructed using inverted dural flaps controlled with Gel foam, Surgical and pressure. The wound was washed and closed in layers over a drain during the operation. This ensured a favorable outcome. The surgical procedure was considered successful (Figure 2), and the patient was awakened from general anesthesia in the operating room. The postoperative period was uneventful, and he had no neurological deficits or evidence of infection or symptoms of raised intracranial pressure at the time of discharge (the tenth day after surgery). No anticoagulant therapy was used in the peri- or postoperative periods. One month after the operation, the patient was re-examined due to a disabling headache and vomiting. Fundoscopy demonstrated bilateral papilloedema, and the follow-up MRI venography showed secondary thrombosis of the middle third of the sagittal sinus and stenosis of the posterior third of the SSS (Figure 3). The patient is currently continuing to receive anticoagulant therapy, antiedema agents and acetazolamide.
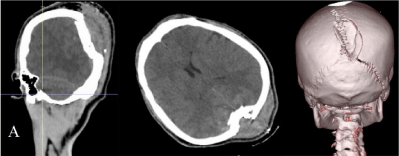
Figure 1: Sagittal, axial and 3D-CT (three-dimensional) reconstruction of the
bony windows of the cranial tomography showed a depressed skull fracture of
the middle occipital bone just anterior to the lambdoid suture.
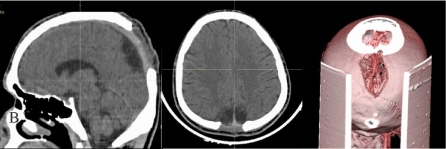
Figure 2: Sagittal, axial and three-dimensional computed tomography
showing postoperative images of depressed occipital skull fracture overlying
posterior third of the SSS.
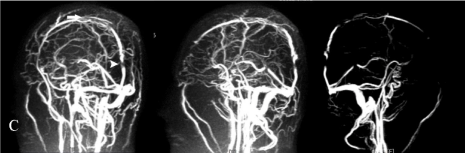
Figure 3: In the control cranial MRI venography examination carried out after
one month of the operation; although the superior sagittal sinus is clearly
monitored, there were marked stenosis in the posterior portion which was site
of the operation (arrowhead) and irregular thinning in contours of the sinus at
the level of vertex, compatible with chronic venous sinus thrombosis (arrow).
Discussion
The association of venous sinus injury with depressed skull fractures was underlined for the first time by Holmes and Sargent [6] in their classic thesis from World War I. The venous sinus may be easily injured by overlying skull fractures because there is only a single layer of dura between the bone and the sinus lumen. Clinical manifestations vary from headache only [7-9] to seizures [10], confusion with [10-12] or without neurologic deficits [13] and death [14]. Depressed fractures are often associated with an underlying dural injury that can result in intraoperative, significant blood loss related to the major dural venous sinus. Attempts to repair sinus damage can cause thrombosis, stenosis or complete occlusion of the sinus. In the posterior third part of the SSS, this will often result in venous hypertension, thrombosis and venous infarction. Therefore, in most cases, nonoperative treatment is widely considered the therapy of choice in the absence of associated hematoma or cerebrospinal fluid fistula [5,8,15].
Elevating depressed fractures overlying SSS is considered hazardous. Reported rates of severe hemorrhagic complications in patients undergoing operative treatment for depressed skull fractures over a venous sinus are 23 and 20% respectively, according to Lefeuvre et al. [16] and Miller et al. [17]. In most cases, more conservative therapy is recommended because of the high possibility of death due to uncontrollable bleeding from the venous sinus [18]. Nevertheless, SSS stenosis may cause venous hypertension and SSS thrombosis, leading to blood flow obstruction [19].
Early diagnosis and the appropriate treatment of depressed fractures over a venous sinus of the skull can minimize the risk of complications. Once physiologic stability has been provided, laboratory and radiological evaluations are vital in determining the extent of injury. Radiographic assessment may consist of a CT scan, skull series, angiography and magnetic resonance imaging. CT scans can detect the path and location of the embedded foreign body, bone or metal debris fragments and the extent of intracranial damage [20-23]. The most useful modalities for a neuroradiological assessment of SSS obliteration are CT scans using thinly sliced bone windows with sagittal and coronal reconstruction, MRI and MRI venography to study venous return in the SSS. Surgical intervention may be necessary if a post-operative study reveals SSS compression in a patient with typical clinical symptoms [8,9,12,13,24]. The sagittal sinus must be repaired in its middle and posterior one-third. A bone island surrounding the fragment bone can be created with the help of a high speed drill, and the SSS can be mobilized distally and proximally. This can be followed by a direct repair of the SSS. It is also possible to resect the SSS and replace it with a vein or dural graft, though it is technically demanding [25-27]. Reconstruction techniques have been described for the SSS, such as direct suturing, graft patching or bypass using venous graft or silicone tubing [28]. Inverted dura was used as an autograft patch for reconstruction in this patient.
Medical treatment of SSS thrombosis may include good hydration, antiedema agents, acetazolamide, fibrinolytic infusion and heparin [12,29,30]. In this case, anticoagulant or fibrinolytic drugs were used because the patient did not respond well to CSF draining and acetazolamide [12,29-31].
Conclusion
Depressed skull fractures overlying major venous sinuses, particularly in the midline, should always be considered a potential source of sinus injury. Depressed skull fractures overlying the major venous sinuses are often managed nonoperative because of the high associated risks of surgery in these locations, such as hemorrhage, air embolism, thrombosis and stenosis. However, in the presence of clinical and radiographic evidence of sinus occlusion, surgical therapy may be necessary. An MRI venography is recommended for all patients who have an open depressed skull fracture overlying the SSS because of the potential risk for venous sinus stenosis and thrombosis, which may develop at a later date.
References
- Jennett B. Epidemiology of head injury. J Neurol Neurosurg Psychiatry. 1996; 60: 362-369.
- Golfinos JG, Cooper PR. Skull fracture and post-traumatic cerebrospinal fluid fistula. Cooper PR, Golfinos JG, editors. In: Head Injury. 4th Edn. New York: McGraw-Hill. 2000; 155.
- Geisler FH. Skull fractures. Wilkins RH, Regachary SS, editors. In: Neurosurgery. 2nd Edn. New York: McGraw-Hill. 1996: 2741-55.
- Steinbok P, Flodmark O, Martens D, Germann ET. Management of simple depressed skull fractures in children. J Neurosurg. 1987; 66: 506-510.
- Gudeman SK, Young HF, Miller JD, Ward JD, Becker DP. Indications for operative treatment and operative technique in closed head injury. Becker DP, Gudeman SK, editors. In: Textbook of Head Injury. Philadelphia: WB Saunders. 1989; 138-181.
- Holmes G, Sargent P. Injuries of the Superior Longitudinal Sinus. Br Med J. 1915; 2: 493-498.
- Meltzer H, LoSasso B, Sobo EJ. Depressed occipital skull fracture with associated sagittal sinus occlusion. J Trauma. 2000; 49: 981.
- Uzan M, Ciplak N, Dashti SGR, Bozkus H, Erdincler P, Akman C. Depressed skull fracture overlying the superior sagittal sinus as a cause of benign intracranial hypertension. J Neurosurg. 1998; 88: 598-600.
- Van den Brink W, Pieterman H, Avezaat CJJ. Sagittal sinus occlusion, caused by an overlying depressed cranial fracture, presenting with late signs and symptoms of intracranial hypertension: case report. Neurosurgery. 1996; 38: 1044-1046.
- Kaplan A. Compound depressed fractures of the skull involving the superior longitudinal sinus. Am J Surg. 1947; 74: 80-85.
- Carlucci GA. Injury to the longitudinal sinus accompanying a depressed fracture of the skull. Am J Surg 1939; 45: 120-124.
- du Plessis JJ. Depressed skull fracture involving the superior sagittal sinus as a cause of persistent raised intracranial pressure: a case report. J Trauma. 1993; 34: 290-292.
- Caudill CM, French LA, Haines GL. Increased intracranial pressure following compression of the superior sagittal sinus. Neurology. 1953; 3: 231-233.
- Mohindra S, Mukherjee KK, Chhabra R, Khosla VK. Subgaleal suction drain leading to fatal sagittal sinus haemorrhage. Br J Neurosurg. 2005; 19: 352-354.
- Cooper PR. Skull fracture and traumatic cerebrospinal fluid fistulas. Cooper PR, editor. In: Head Injury. 3rd Edn. Baltimore: Williams & Wilkins. 1993; 115-136.
- LeFeuvre D, Taylor A, Peter JC. Compound depressed skull fractures involving a venous sinus. Surg Neurol. 2004; 62: 121-125.
- Miller JD, Jennett WB. Complications of depressed skull fracture. Lancet. 1968; 2: 991-995.
- Fuentes S, Metellus P, Levrier O, Adetchessi T, Dufour H, Grisoli F. Depressed skull fracture overlying the superior sagittal sinus causing benign intracranial hypertension. Description of two cases and review of the literature. Br J Neurosurg. 2005; 19: 438-442.
- Donovan DJ. Simple depressed skull fracture causing sagittal sinus stenosis and increased intracranial pressure: case report and review of the literature. Surg Neurol. 2005; 63: 380-383.
- Aarabi B, Cook J. Missile wounds of the head. Reilly PL, Bullock R, editors. In: Head Injury: Pathophysiology and Management. 2nd Edn. UK: Hodder Arnold Publishing. 2005; 384-403.
- Tibbs RE, Lee DC, Parent AD. Depressed skull fracture. Batjer HH, Loftus CM, editors. In: Textbook of Neurological Surgery: Principles and Practice. Philadelphia: Lippincott Williams and Wilkins. 2003; 1082-1095.
- Valadka AB. Penetrating Cranial Trauma. Batjer HH, Loftus CM, editors. In: Textbook of Neurological Surgery: Principles and Practice. Philadelphia: Lippincott Williams and Wilkins. 2003; 2851-2859.
- Dutcher S, Sood S, Ham S, Canady AI. Depressed Skull Fractures. McLone DG, editor. In: Pediatrics Neurosurgery: Surgery of the Developing Nervous System. 4th Edn. USA: WB Saunders. 2001; 584-586.
- Binder DK, Horton JC, Lawton MT, McDermott MW. Idiopathic intracranial hypertension. Neurosurgery. 2004; 54: 538-551.
- Bederson JB, Eisenberg MB. Resection and replacement of the superior sagittal sinus for treatment of a parasagittal meningioma: technical case report. Neurosurgery. 1995; 37: 1015-1018.
- Bonnal J, Brotchi J. Surgery of the superior sagittal sinus in parasagittal meningiomas. J Neurosurg. 1978; 48: 935-945.
- Caroli E, Orlando ER, Mastronardi L, Ferrante L. Meningiomas infiltrating the superior sagittal sinus: surgical considerations of 328 cases. Neurosurg Rev. 2006; 29: 236-241.
- Sindou MP, Alvernia JE. Results of attempted radical tumor removal and venous repair in 100 consecutive meningiomas involving the major dural sinuses. J Neurosurg. 2006; 105: 514-525.
- Kinal ME. Traumatic thrombosis of dural venous sinus. Van Bogart L, Radermecker J, editors. In: Neurological Surgery: Proceedings of the First International Congress of Neurological Science. New York, Pergon. 1959; 2: 178-188.
- van den Heever CM, van der Merwe DJ. Management of depressed skull fractures. Selective conservative management of nonmissile injuries. J Neurosurg. 1989; 71: 186-190.
- van der Sande JJ, Veltkamp JJ, Boekhout-Mussert RJ, Bouwhuis-Hoogerwerf ML. Head injury and coagulation disorders. J Neurosurg. 1978; 49: 357-365.