
Research Article
Austin Neurosurg Open Access. 2017; 4(1): 1055.
The Medial Cord –Anterior Upper Trunk (MC-aUT) Nerve Transfer in Brachial Plexus Injuries. Technique and Results
Ferraresi S*, Basso E, Maistrello L, Lucchin F and Di Pasquale P
Department of Neurosurgery, Ospedale Santa Maria della Misericordia, Italy
*Corresponding author: Stefano Ferraresi, Head Department of Neurosurgery, Ospedale Santa Maria della Misericordia, Rovigo, Italy
Received: February 21, 2017; Accepted: April 19, 2017; Published: April 26, 2017
Abstract
Aim of this paper is to report on a technical variant of the Medial Cord to the Musculocutaneous (MCMc) nerve transfer. The MCMc is a new type of neurotization that we described in 2014, capable of reanimating the elbow flexion in multilevel avulsive injuries of the upper and middle plexus.
In the over mentioned procedure the reinnervation of the musculocutaneous nerve is obtained via a nerve transfer from the medial cord. The selected fascicles are those directed principally to the flexor carpi radial is, ulnaris, and to a lesser degree the flexor digitorum profundus.
They are located in the inverted V-shaped bifurcation between the internal contribution of the median nerve and the ulnar nerve.
The results of this technique are excellent. There are no failures and no complications when the hand shows a normal wrist and finger flexion and a normal intrinsic function, namely in C5-C6 or C5-C6-C7 avulsive injuries of the brachial plexus.
However, the sole problem appears with an agenesia of the musculocutaneous nerve (4% of our series).
In these patients, the lateral cord tapers directly into the median nerve one or more branches entering directly the biceps and the brachialis muscles at the upper third of the arm. This arrangement is hostile to the MCMc nerve transfer so as it was originally conceived.
The present paper reports the results of a technical variant of the MCMc technique, namely the targeting, as recipient, of the anterior contribution of the upper trunk, cut and rerouted under the clavicle to reach the donor medial cord.
Keywords: Brachial plexus; Nerve transfer; Musculocutaneous nerve; Biceps muscle; Brachialis muscle; Root avulsion
Introduction
Since the onset of the microsurgical era of brachial plexus repair [1,2], until the early nineties [3-7] the treatment of an avulsive injury of C5-C6 or of C5-C6-C7 was a great challenge for the microsurgeon.
Several techniques had been attempted over the years to restore elbow flexion but none of them [8-12] with the exception of the medial pectoral nerves [13-16] offered a constant and reliable muscle power. The lower pectoral nerves, however, are available in number of two and, when used both, entailed a remarkable loss of strength in the pectoralis major. Moreover, the feasibility of their use as a direct nerve transfer is unpredictable, since from time to time they require short grafts. The extraplexual donors, namely the phrenic nerve [17,18], the accessory nerve [19-26] the intercostals nerves [27-37] the motor cervical rami [38,39] and the hypoglossal nerve [40,41] were also variably used to restore elbow flexion but none of them can count on constant and reproducible results. So, in spite of the presence of a normal hand function, this kind of lesions rather often ended with a heavily disabled arm due to a poor quality of recovery in the biceps-brachialis complex.
The typical patient had great difficulty in lifting even moderately heavy objects and the condition was futherly worsened by an unstable shoulder due to the denervation of the rhomboids and serratus anterior muscles.
In 1993 and 1994 the pioneering work of C. Oberlin [42] announced a true revolution in the treatment of C5-C6 avulsive injuries of the brachial plexus. In his original paper he described a successful selective reinnervation of the biceps branches via a fascicular neurotization from the ulnar nerve. However, his merit went far beyond the pure technique he described. He opened in various directions the mind of the microsurgeons, showing to the scientific world that a neurotization from fascicles of a sound nerve yielded results better than ever and without threatening the overall function of the donor.
This gave rise to the by-pass or nerve transfer era [43,44], which has been, by far, the recent major advance in the field of brachial plexus reconstructive surgery. Many different ingenious transfers are currently used by the microsurgeons [3,5,45-61] and the direct reinnervation (without interposition of grafts) of the paralyzed nerves with motor branches coming from an intact part of the brachial plexus has gained worldwide acceptance.
Among the available techniques, the Authors have recently published (2014) an original technique, called the MCMc nerve transfer [48], which has shown constant, reproducible and, so far, unparalleled results on biceps and brachialis muscle recovery.
With this technique the entire plexus is, as always, explored via the combined supraclavicular and infraclavicular approach. The philosophy is to assess the level and the entity of the damage to exclude an unexpected integrity of the upper plexus and check for a possible two-stage distal lesion of the musculocutaneous and the axillary nerves.
The musculocutaneous nerve is cut at its exit from the lateral cord and reinnervated via one or two fascicles aimed at the flexor carpi radialis or ulnaris, usually selected from the medial contribution of the median nerve at the division with the ulnar nerve (Figure 1).
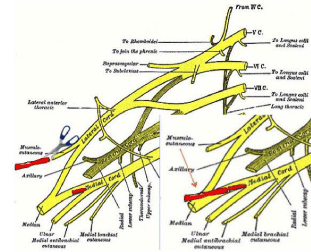
Figure 1: The original MCMc transfer technique as described in Neurosurgical
Review 2014.
This technique also offers, differently from the Oberlin’s, a second occasion at a more distal level in case of failure of the first procedure. As a matter of fact, a reinnervation of the biceps distal branches can yet be attempted from the ulnar nerve since its function has not been weakened during the first attempt.
However, in 4% of our patients, the MCMc nerve transfer cannot be carried out so as it was originally conceived, because of an anatomical variant, namely the agenesia of the musculocutaneous nerve from the lateral cord, with the MC nerve coming out of the median nerve at arm level (Figure 2). Instead of resorting to an Oberlin procedure which is, as already explained, a “terminal” operation, the Authors have developed a further evolution of their MCMc nerve transfer.
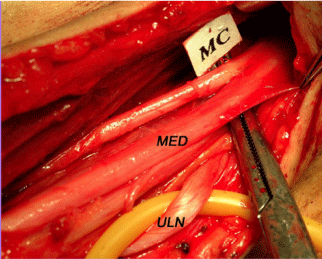
Figure 2: Agenesia of the musculocutaneous at the infraclavicular lateral
cord. The division is found in the upper third of the arm.
Patients and Methods
Four patients, three males and one female, below 40 years of age, had a C5-C6-(C7) root avulsive injury of the brachial plexus and, due to the absence of the musculocutaneous nerve in the lateral cord, were obvious candidates for this new type of neurotization.
Surgical technique
The upper trunk is prepared and its anterior contribution is cut immediately after the trifurcation of the Upper Trunk. Please note how the illustrations in the books are misleading because, due to the orientation of the brachial plexus on three planes, the anterior contribution of the upper trunk in the reality lies in the more medial position (Figure 3).
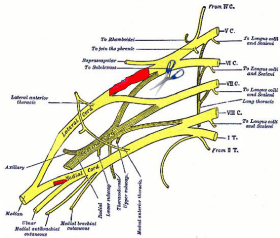
Figure 3: Medial cord (donor) to anterior Upper Trunk (recipient): draft of the
new MC-aUT transfer.
An extensive dissection of all the connections with the lateral cord, namely the anterior and posterior divisions of the C7 root and the afferent and efferent connection to and from the middle trunk, is mandatory. At the end, after rerouting under the clavicle, the anterior contribution of the upper trunk (aUT) is brought at the level of the Medial Cord and coapted, without tension (Figure 4). In only one occasion the anterior contribution of C7 had to be interrupted to allow mobilization of the anterior upper trunk (aUT). This case was uneventful because of an avulsive injury of C7, but any effort in dissection should be made in case of integrity of the C7 root. The epineurium of the medial cord is then opened and an intraneural inspection is undertaken. The procedure is painstaking but it is imperative to repeatedly check at low intensity (0,2 and 0,3 mA) the area of division of the medial cord. Particular attention is focused to the medial contribution of the median nerve at the level of the take off with the ulnar nerve. Here, only the fascicles aimed at the flexor carpi radialis or, rarely, the ulnaris are selected. They are usually made of one single large voluminous fascicle or two smaller fascicles. The area to be cut is usually clearly defined and matches exactly with the section of the receiving anterior Upper Trunk. The sutures are made of 9-0 Nylon and fibrin glue.
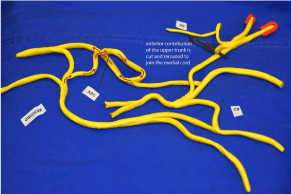
Figure 4: In avulsive injuries of C5 and C6 with agenesia of the
musculocutaneous nerve the anterior upper trunk, medially located, is cut,
rerouted and connected to donor fascicles in the medial cord. Red arrows
indicate the direction of axon sprouting towards the biceps.
Results
In all the cases excellent functions (M4) in the biceps and the brachialis have been obtained (Video 1). The pectoralis major showed an unequivocal better function in two patients. This technique, in fact, due to the more proximal location of the recipient, entails the possibility to reinnervate the proximal pectoral nerve loop, not attainable with the MCMc transfer.
All the patients retained a normal wrist and finger function at hand level. The time of reinnervation was not overly longer in comparison to the formerly described MCMc transfer, lasting some 1-2 months more, namely 7-8 months. The low number of patients doesn’t permit a statistical significance, but, in any case, this obvious delay is not deemed important and it is explained at light of the longer distance to be covered by the sprouting axons.
Discussion
This variant shares the same basic idea of the medial cord technique (MCMc) which is very effective and shows constant and reproducible results in patients in whom the hand functions, or at least its flexor and intrinsic power is completely retained. The absence of wrist and finger dorsiflexion never impacts on the final result.
A hostile anatomy of the lateral cord would be the only limitation of the MCMc transfer if compared to the classical Oberlin procedure, but this refinement of the technique shows basically the same results, in spite of the low number of cases. As a target, the anterior Upper Trunk seems to be even more selective than the entire musculocutaneous nerve carrying a lesser sensory component.
The technical procedure is delicate but does not require a special skill or a particular learning curve for an experienced plexus surgeon.
The procedure is straightforward in course of a standard exploration of the plexus and doesn’t need additional incisions in the arm. The mobilization of the upper and middle plexus can be a little bit awkward, but it is very important to reroute the anterior contribution of the upper trunk (aUT) and reach the medial cord without any tension.
Denervation pain in the territory of the median or ulnar nerve has never been observed. We had, on the contrary, a case of long lasting pain in the ulnar territory with denervation and reflex sympathetic dystrophy after a double Oberlin’s operation (one fascicle from the ulnar n. to biceps motor branches and one motor fascicle of the median nerve to brachialis motor branches).
In case of a weaker ulnar nerve function (M3 hand) the medial cord technique offers more choice than the Oberlin procedure. The surgeon disposes of a wider selection among proximal fascicles directed to the Flexor Carpi Radialis or Flexor Carpi Ulnaris while, in the arm, one can select only one nerve at the time (either the median or the ulnar).
The Medial Cord–anterior Upper Trunk procedure (MC-aUT) also appears to be by far the more appropriate technique in the presence of a residual function of the musculocutaneous nerve usually sustained by fibers coming from C7. When C5 and C6 are unequivocally avulsed, in fact, the residual function of the biceps comes from C7. A nerve transfer to the distal MC nerve would sacrifice that function, while the neurotization to the anterior upper trunk selectively replaces only the fibers intended to come from C5 and C6, leaving those from C7 intact. The Oberlin type of nerve transfer also would force to a definitive choice, entailing the section of the distal branches of the Musculocutaneous nerve in the arm even if they show some function.
T?he frequency and the power of reinnervation, thanks to the participation of the biceps and the brachialis, is stronger than with the simple Oberlin technique.
References
- Millesi H. Brachial plexus injuries. Management and Results. Clin Plast Surg. 1984; 11: 115-120.
- Narakas AO. Thoughts on neurotization or nerve transfers in irreparable nerve lesions. Clin Plast Surg. 1984; 11: 153-159.
- Chuang DC. Neurotization procedures for brachial plexus injuries. Hand Clin. 1995; 11: 633-645.
- Ferraresi S, Garozzo D, Buffatti P. Reinnervation of the biceps in C5-C7 brachial plexus avulsion injuries. Results after distal bypass surgery. Neurosurg. Focus. 2004; 16: E6.
- Kawai H, Kawabata H, Masada K, Ono K, Yamamoto K, Tsuyuguchi Y, et al. Nerve repairs for traumatic brachial plexus palsy with root avulsion. Clin Orthop. 1988; 237: 75-86.
- Terzis JK, Papakonstantinou KC. The surgical treatment of brachial plexus injuries in adults. Plast Reconstr Surg. 2000; 106: 1097-1122.
- Tung TH, Mackinnon SE. Brachial plexus injuries. Clin Plast Surg. 2003; 30: 269-287.
- Friedman AH, Nunley JA, Goldner RD, Oakes WJ, Goldner JL, Urbaniak JR. Nerve transposition for the restoration of elbow flexion following brachial plexus avulsion injuries. J Neurosurg. 1990; 72: 59-64.
- Samii M, Carvalho GA, Nikkhah G, Penkert G. Surgical reconstruction of the musculocutaneous nerve in traumatic brachial plexus injuries. J Neurosurg. 1997; 87: 881-886.
- Sedel L. The results of surgical repair of brachial plexus injuries. J Bone Joint Surg Br. 1982; 64: 54-66.
- Songcharoen P. Brachial plexus injury in Thailand: a report of 520 cases. Microsurgery. 1995; 16: 35-39.
- Terzis JK, Vekris MD, Soucacos PN. Outcomes of brachial plexus reconstruction in 204 patients with devastating paralysis. Plast Reconstr Surg. 1999; 104: 1221-1240.
- Aszmann OC, Rab M, Kamolz L, Frey M. The anatomy of the pectoral nerves and their significance in brachial plexus reconstruction. J Hand Surg Am. 2000; 25: 942-947.
- Blaauw G, Slooff AC. Transfer of pectoral nerves to the musculocutaneous nerve in obstetric upper brachial plexus palsy. Neurosurgery. 2003; 53: 338-342.
- Hansasuta A, Tubbs RS, Grabb PA. Surgical relationship of the medial pectoral nerve to the musculocutaneous nerve: a cadaveric study. Neurosurgery. 2001; 48: 203-207.
- Samardzic M, Grujicic D, Rasulic L, Bacetic D. Transfer of the medial pectoral nerve: myth or reality? Neurosurgery. 2002; 50: 1277-1282.
- Luedemann W, Hamm M, Blömer U, Samii M, Tatagiba M. Brachial plexus neurotization with donor phrenic nerves and its effect on pulmonary function. J Neurosurg. 2002; 96: 523-526.
- Viterbo F, Franciosi LF, Palhares A. Nerve graftings and end-to-side neurorrhaphies connecting the phrenic nerve to the brachial plexus. Plast Reconstr Surg. 1995; 96: 494-495.
- Allieu Y, Privat JM, Bonnel F. Neurotization with the spinal nerve (nervusaccessorius) in avulsions of roots of the brachial plexus. Neurochirurgie. 1982; 28: 115-120.
- Allieu Y, Privat JM, Bonnel F. Paralysis in root avulsion of the brachial plexus: neurotization by the spinal accessory nerve. Terzis JK. In: Microreconstruction of Nerve Injuries. WB Saunders Philadelphia.1987; 415-423.
- Hattori Y, Doi K, Toh S, Baliarsing AS. Surgical approach to the spinal accessory nerve for brachial plexus reconstruction. J Hand Surg Am. 2001; 26: 1073-1076.
- Kierner AC, Zelenka I, Heller S, Burian M. Surgical anatomy of the spinal accessory nerve and the trapezius branches of the cervical plexus. Arch Surg. 2000; 135: 1428-1431.
- Samardzic M, Grujicic D, Antunovic V, Joksimovic M. Reinnervation of avulsed brachial plexus using the spinal accessory nerve. Surg Neurol. 1990; 33: 7-11.
- Samii A, Carvalho GA, Samii M. Brachial plexus injury: factors affecting functional outcome in spinal accessory nerve transfer for the restoration of elbow flexion. J Neurosurg. 2003; 98: 307-312.
- Songcharoen P, Mahaisavariya B, Chotigavanich C. Spinal accessory neurotization for restoration of elbow flexion in avulsion injuries of the brachial plexus. J Hand Surg Am. 1996; 21: 387-390.
- Songcharoen P, Mahaisavariya B, Chotigavanich C. Spinal accessory neurotization for restoration of elbow flexion in avulsion injuries of the brachial plexus. J Hand Surg Am. 1996; 21: 387-390.
- Asfazadourian H, Tramond B, Dauge MC, Oberlin C. Morphometric study of the upper intercostal nerves: practical application for neurotizations in traumatic brachial plexus palsies. Chir Main. 1999; 18: 243-253.
- Giddins GE, Kakkar N, Alltree J, Birch R. The effect of unilateral intercostal nerve transfer upon lung function. J Hand Surg Br.1995; 20: 675-676.
- Hattori Y, Doi K, Fuchigami Y, Abe Y, Kawai S. Experimental study on donor nerves for brachial plexus injury: comparison between the spinal accessory nerve and the intercostal nerve. Plast Reconstr Surg. 1997; 100: 900-906.
- Kawabata H, Shibata T, Matsui Y, Yasui N. Use of intercostal nerves for neurotization of the musculocutaneous nerve in infants with birth-related brachial plexus palsy. J Neurosurg. 2001; 94: 386-391.
- Malessy MJ, Thomeer RT. Evaluation of intercostal to musculocutaneous nerve transfer in reconstructive brachial plexus surgery. J Neurosurg. 1998; 88: 266-271.
- Malessy MJ, van der Kamp W, Thomeer RT, van Dijk JG. Cortical excitability of the biceps muscle after intercostal-to-musculocutaneous nerve transfer. Neurosurgery. 1998; 42:787-795.
- Mano Y, Nakamuro T, Tamura R, Takayanagi T, Kawanishi K, Tamai S, et al. Central motor reorganization after anastomosis of the musculocutaneous and intercostal nerves following cervical root avulsion. Ann Neurol. 1995; 38: 15-20.
- Merrell GA, Barrie KA, Katz DL, Wolfe SW. Results of nerve transfer techniques for restoration of shoulder and elbow function in the context of a meta-analysis of the English literature. J Hand Surg Am. 2001; 26: 303-314.
- Minami M, Ishii S. Satisfactory elbow flexion in complete (preganglionic) brachial plexus injuries: produced by suture of third and fourth intercostal nerves to musculocutaneous nerve. J Hand Surg Am. 1987; 12: 1114-1118.
- Nagano A, Yamamoto S, Mikami Y. Intercostal nerve transfer to restore upper extremity functions after brachial plexus injury. Ann Acad Med Singapore. 1995; 24: 42-45.
- Ruch DS, Friedman A, Nunley JA. The restoration of elbow flexion with intercostal nerve transfers. Clin Orthop Relat Res. 1995; 314: 95-103.
- Brunelli G, Monini L. Neurotization of avulsed roots of brachial plexus by means of anterior nerves of cervical plexus. ClinPlastSurg. 1984; 11: 149-152.
- Yamada S, Peterson GW, Soloniuk DS, Will AD. Coaptation of the anterior rami of C-3 and C-4 to the upper trunk of the brachial plexus for cervical nerve root avulsion. J Neurosurg. 1991; 74: 171-177.
- Ferraresi S, Garozzo D, Ravenni R, Dainese R, De Grandis D, Buffatti P. Hemihypoglossal nerve transfer in brachial plexus repair: technique and results. Neurosurgery. 2002; 50: 332-335.
- Malessy MJ, Hoffmann CF, Thomeer RT. Initial report on the limited value of hypoglossal nerve transfer to treat brachial plexus root avulsions. J Neurosurg. 1999; 91: 601-604.
- Oberlin C, Beal D, Leechavengvongs S, Salon A, Dauge MC, Sarcy JJ. Nerve transfer to biceps muscle using a part of ulnar nerve for C5-C6 avulsion of the brachial plexus: anatomical study and report of four cases. J Hand Surg Am. 1994; 19: 232-237.
- El-Gammal TA, Fathi NA. Outcomes of surgical treatment of brachial plexus injuries using nerve grafting and nerve transfers. J Reconstr Microsurg. 2002; 18: 7-15.
- Midha R. Emerging techniques for nerve repair: nerve transfers and nerve guidance tubes. Clin Neurosurg. 2006; 53: 185-190.
- Bertelli JA, Ghizoni MF. Reconstruction of C5 and C6 brachial plexus avulsion injury by multiple nerve transfers: spinal accessory to suprascapular, ulnar fascicles to biceps branch, and triceps long or lateral head branch to axillary nerve. J Hand Surg Am. 2004: 29: 131-139.
- Brandt KE, Mackinnon SE. A technique for maximizing biceps recovery in brachial plexus reconstruction. J Hand Surg Am. 1993; 18: 726-733.
- Chuang DC, Lee GW, Hashem F, Wei FC. Restoration of shoulder abduction by nerve transfer in avulsed brachial plexus injury: evaluation of 99 patients with various nerve transfers. PlastReconstrSurg. 1995; 96: 122-128.
- Ferraresi S, Garozzo D, Basso E, Maistrello L, Lucchin F, Di Pasquale P. The Medial Cord to Musculocutaneous (MCMc) nerve transfer: a new method to reanimate elbow flexion after C5-C6-C7-(C8) avulsive injuries of the brachial plexus--technique and results. Neurosurg Rev. 2014; 37: 321-329.
- Gu YD, Cai PQ, Xu F, Peng F, Chen L. Clinical application of ipsilateral C7 nerve root transfer for treatment of C5 and C6 avulsion of brachial plexus. Microsurgery. 2003; 23: 105-108.
- Gutowski KA, Orenstein HH. Restoration of elbow flexion after brachial plexus injury: the role of nerve and muscle transfers. PlastReconstrSurg. 2000; 106: 1348-1357.
- Hou Z, Xu Z. Nerve transfer for treatment of brachial plexus injury: comparison study between the transfer of partial median and ulnar nerves and that of phrenic and spinal accessary nerves. Chin J Traumatol. 2002; 5: 263-266.
- Leechavengvongs S, Witoonchart K, Uerpairojkit C, Thuvasethakul P, Ketmalasiri W. Nerve transfer to biceps muscle using a part of the ulnar nerve in brachial plexus injury (upper arm type): a report of 32 cases. J Hand Surg Am.1998; 23: 711-716.
- Leechavengvongs S, Witoonchart K, Uerpairojkit C, Thuvasethakul P. Nerve transfer to deltoid muscle using the nerve to the long head of the triceps, part II: a report of 7 cases. J Hand Surg Am. 2003; 28: 633-638.
- Loy S, Bhatia A, Asfazadourian H, Oberlin C. Ulnar nerve fascicle transfer onto to the biceps muscle nerve in C5-C6 or C5- C6-C7 avulsions of the brachial plexus. Eighteen cases. Ann Chir Main Memb Super (Fre). 1997; 16: 275-284.
- Samardzic M, Rasulic L, Grujicic D, Milicic B. Results of nerve transfers to the musculocutaneous and axillary nerves. Neurosurgery. 2000; 46: 93-101.
- Sungpet A, Suphachatwong C, Kawinwonggowit V. One-fascicle median nerve transfer to biceps muscle in C5 and C6 root avulsions of brachial plexus injury. Microsurgery. 2003; 23: 10-13.
- Sungpet A, Suphachatwong C, Kawinwonggowit V. Surgical anatomy of bicipital branch of musculocutaneous nerve. J Med Assoc Thai. 1998; 81: 532-535.
- Sungpet A, Suphachatwong C, Kawinwonggowit V, Patradul A. Transfer of a single fascicle from the ulnar nerve to the biceps muscle after avulsions of upper roots of the brachial plexus. J Hand Surg Br. 2000; 25: 325-328.
- Tung TH, Novak CB, Mackinnon SE. Nerve transfers to the biceps and brachialis branches to improve elbow flexion strength after brachial plexus injuries. J Neurosurg. 2003; 98: 313-318.
- Witoonchart K, Leechavengvongs S, Uerpairojkit C, Thuvasethakul P, Wongnopsuwan V. Nerve transfer to deltoid muscle using the nerve to the long head of the triceps, part I: an anatomic feasibility study. J Hand Surg Am. 2003; 28: 628-632.
- Yamada S, Lonser RR, Iacono RP, Morenski JD, Bailey L. Bypass coaptation procedures for cervical nerve root avulsion. Neurosurgery. 1996; 38: 1145-1152.