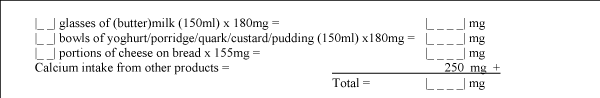Research Article
Austin J Nutri Food Sci. 2014;2(3): 1019.
Validity of a Calcium Intake List to Estimate Calcium Intake in Patients with Osteoporosis
LA Rasch1,2*, MAE de van der Schueren2, LHD van Tuyl1, IM Bultink1 and WF Lems1
1Department of Rheumatology, VU University Medical Center, Amsterdam, Netherlands
2Department of Nutrition and Dietetics, Internal Medicine, VU University Medical Center, Amsterdam, Netherlands
*Corresponding author: :LA Rasch, Department of Rheumatology and Department of Nutrition and Dietetics, VU University Medical Center, 1081 HV Amsterdam, Netherlands
Received: January 23, 2014; Accepted: March 11, 2014; Published: March 19, 2014
Abstract
Background: Calcium supplements are widely used for prevention and treatment of osteoporosis. Literature suggests an association between a too high calcium supplementation and cardiovascular events.
Objectives: The aim of this study was to validate an existing calcium intake list which is used as a basis for prescription of calcium supplementation in patients with osteoporosis. We hypothesized that the calcium intake list is not a valid method to estimate dietary calcium intake.
Methods: The calcium intake list estimates calcium by portions of milk, yoghurt, cheese (180 mg, 180 mg, and 155 mg per portion respectively), and 250 mg calcium from other products. A dietary history (DH) with specific focus on calcium products provided the reference method. A difference of ≥250 mg calcium between both methods was formulated as clinically relevant.
Conclusions: The calcium intake list is not a valid method to estimate calcium intake.
Abbreviations
RCT: Randomised Controlled Trial; DH: Dietary History.
Introduction
Calcium supplements are widely used for the prevention and treatment of osteoporosis, the latter usually along with antiosteoporotic drugs such as bisphosphonates. However, recent literature suggests that too much calcium supplementation may be harmful. A five year “randomised controlled trial (RCT)” of Bolland et al. [1] concluded that calcium supplements (1000 mg on top of a dietary intake of approximately 850 mg) were associated with an increased risk of cardiovascular events. In contrast, Lewis et al. found no evidence that calcium supplements increased the risk of cardiovascular diseases after administrating 1200 mg calcium per day or identical placebo tablets, in addition to an intake of around 950 mg dietary calcium daily [2].
At this moment, calcium supplementation and its possible adverse effects is an item frequently debated by professionals, as well as by patients. Although there is no indisputable evidence for an association between calcium supplements and cardiovascular risks, the rumour persists and prescribing too much calcium supplementation is not desirable until adverse effects are contradicted with certainty. Therefore, it is important to have an adequate estimation of the dietary calcium intake of the patients, to be able to prescribe the right dose of calcium supplementation (to reach the recommended levels of 1000 to 1200 mg per day) without a possible increase of the risk of cardiovascular disease.
If patients have an insufficient dietary intake of calcium, physicians prescribe additional calcium supplementation to patients with osteoporosis. In our hospital, physicians use a short calcium intake list, based on three questions, as the basis for additional calcium prescriptions, to reach the recommended calcium intake levels of the Dutch Institute for Health Care Improvement for osteoporosis patients of 1000 to 1200 mg per day [3] without a possible increase of the risk of cardiovascular diseases. However, the calcium intake list has not been validated and exact portion sizes have not been checked. Moreover, the ‘rest’ group of 250 mg calcium has not beenquantified. Therefore, this study aims to determine the difference in daily dietary calcium intake when estimated by the calcium intake list, and by a reference method, a “dietary history (DH)” with specific focus on calcium products. We hypothesize a difference in dietary calcium intake between both methods, because the calcium intake list provides only a rough calculation of the calcium intake and exact portion sizes have not been checked.
Methods
Study population
This cross–sectional study included all consecutive patients that attended the outpatient rheumatology department at the VUmc in Amsterdam (a university hospital with a large osteoporosis outpatient clinic) for the treatment of primary or secondary osteoporosis between 26th of September 2011 and 18th of November 2011.
Inclusion criteria for all patients
- 18 years or older
- Under treatment for at least three months
- A stable medication regimen
Inclusion criteria for the subset of patients with primary osteoporosis
- Diagnosed with and treated for osteoporosis (T–score <–2.5 in hip and⁄or lumbar spine).
- Inclusion criteria for the subset of patients with secondary osteoporosis:
- Diagnosed with a rheumatic disorder by a rheumatologist.
- Diagnosed with and treated for osteoporosis (T–score <–2.5 in hip and/or lumbar spine).
- Diagnosed with and treated for osteopenia (T–score <–1 in hip and/or lumbar spine) with chronic use of prednisone.
- Diagnosed with and treated for osteopenia (T–score <–1 in hip and/or lumbar spine) with thoracic or lumbar vertebral fractures, defined as a reduction of 25% or more of the vertebral body height.
- Bolland MJ, Barber PA, Doughty RN, Mason B, Horne A, et al. Vascular events in healthy older women receiving calcium supplementation: randomized controlled trial. BMJ. 2008; 336: 262-266.
- Lewis JR, Calver J, Zhu K, Flicker L, Prince RL. Calcium supplementation and the risks of atherosclerotic vascular disease in older women: results of a 5-year RCT and a 4.5-year follow-up. J Bone Miner Res. 2011; 26: 35-41.
- CBO Guideline Osteoporosis and fracture prevention. Dutch Institute for Health Care Improvement; 2011.
- Rolfes SR, Pinna K, Whitney E (2006) Nutrition and Care Assessment. In: Understanding Normal and Clinical Nutrition (Sharon Rady Rolfes, Kathryn Pinna, Ellie Whitney, eds), pp 586-590. California: Thomson Wadsworth.
- Thompson FE, Byers T. Dietary assessment resource manual. J Nutr. 1994; 124: 2245-2317.
- Bolland MJ, Grey A, Avenell A, Gamble GD, Reid IR. Calcium supplements with or without vitamin D and risk of cardiovascular events: reanalysis of the Women's Health Initiative limited access dataset and meta-analysis. BMJ. 2011; 342: d2040.
- Bolland MJ, Avenell A, Baron JA, Grey A, MacLennan GS. Effect of calcium supplements on risk of myocardial infarction and cardiovascular events: meta-analysis. BMJ. 2010; 341: c3691.
- Paik J, Curhan G, Rexrode K, Manson J, Eric R, et al. (2012) A prospective study of calcium supplement intake and risk of cardiovascular disease in women. ASBMR 2012.
- Pereira GA, Genaro PS, Santos LC, Sarkis KS, Pinheiro MM. Validation of a food frequency questionnaire for women with osteoporosis. J Nutr Health Aging. 2009; 13: 403-407.
- Uenishi K, Ishida H, Nakamura K. Development of a simple food frequency questionnaire to estimate intakes of calcium and other nutrients for the prevention and management of osteoporosis. J Nutr Sci Vitaminol (Tokyo). 2008; 54: 25-29.
- Buzzard M (1998) 24-hour dietary recall and food record methods. In: Nutritional Epidemiology (Willett W, ed). New York: Oxford University Press.
- https://www.sfk.nl/nieuws-publicaties/PW/2013/calcium-en-vitamine-d-in-de-lift.
and
or
or
Exclusion criteria
Pregnant women, cognitively impaired persons, or patients who did not speak the Dutch language were excluded from this study. A flowchart of all patients in– and excluded in the study is provided in Figure 1.The study was approved by the local Ethics Committee. All patients provided informed consent for their participation.
Figure 1: Flowchart of patients.
Measurements
Calcium intake
A short calcium intake list was used to estimate the daily intake of calcium via food (Figure 2). The sum of the calculations constituted the outcome of the calcium intake list, which is the basis for the amount of calcium supplementation that is prescribed to the patients. A DH with specific focus on calcium products was performed by an experienced dietician–researcher (LR), based on the long–term usual dietary intake of the subject, and provided the reference method [4,5]. This reference method takes day–to–day variation into account, determines frequency of food consumption as well as portion sizes [5], which, in this study, were determined reasonably accurate using samples of cups (100, 150, 220, 275, and 300 ml), glasses (100, 150, 200, 220, and 300 ml), bowls (100, 200, 250, and 450 ml), and slices of cheese (7, 10, 14, and 25 grams). The DH was meal–based, which means that food consumption was inquired per meal. This mealbased approach is thought to be more accurate and requires more time than a food–based approach, where the subject has to mention food consumption over the entire day [5]. Furthermore, because subjects often forget to mention different products [4], the researcher probed until all food items were mentioned. The specific focus on calcium products was performed by doing a cross–check with special attention for products containing calcium. Performing the DH took about 60 minutes per patient, without processing time. Beforehand, a difference of at least 250 mg calcium between both methods was formulated as clinically relevant.
Figure 2: Calcium intake list used to estimate daily dietary calcium intake.
General characteristics
Demographic (age, gender, race, weight, height) and lifestyle characteristics (smoking status, alcohol use), and disorder related factors (previous clinical fractures) were assessed during the appointment with the researcher. Information about medication and supplements used by the subjects was initially obtained from the medical charts. In addition, subjects were asked to give details on amounts of prescribed calcium and vitamin D supplements taken (to check compliance to the prescriptions), and the use of other (overthe– counter) supplements on own initiative.
Statistical analysis
Nutrient information was obtained from the nutrient database of NEVO–online (version 2011⁄3.0, RIVM, Bilthoven) and nutrient calculation programs Komeet (version 4.0.58, BaS Nutrition Software, Arnhem and The Netherlands) and Orion (version 4.0.27, BaS Nutrition Software, Arnhem, The Netherlands). Data were analyzed using SPSS for Windows (version 15.0, SPSS Inc., Chicago, IL, USA). Data was checked for data entry errors prior to analysis. Descriptive statistics were used to calculate means, frequencies, and percentages. To compare the means of continuous variables, independent sample T–tests were used when data were normally distributed. For data that was not normally distributed, the Mann–Whitney U test was used instead. For categorical variables, the Chi–square test was used. To compare the two methods for measuring calcium intake, paired sample T–tests and the Bland–Altman plot were used. To compare mean calcium intake with the recommended calcium intake, one sample T–test was used. Continuous data are given as mean ± SD. P–values <0.05 were considered to be significant. The limits of agreement used during the Bland–Altman analysis were defined as mean difference ± 1.96 standard deviations of the difference.
Results
General characteristics
In this study, 31 subjects with primary osteoporosis and 35 subjects with secondary osteoporosis associated with a rheumatic disorder were included. The general characteristics of the subjects, subdivided by primary and secondary osteoporosis, are depicted in Table 1.
Total
(n=66)
Primary osteoporosis
(n=31)
Secondary osteoporosis
(n=35)
Socio-demographic factors
Age (years)
64.3 ± 14.3
69.9 ± 8.8
59.3 ± 16.6 *
Gender female (n, (%))
58 (87.9)
27 (87.1)
31 (88.6)
Caucasian (n, (%))
58 (87.9)
30 (96.8)
28 (80.0)
Clinical fractures >25 years of age (n, (%))
46 (69.7)
27 (87.1)
19 (54.3) *
Body Mass Index (kg/m2)1
23.7 ± 3.6
23.3 ± 3.4
24.0 ± 3.9
Disease related factors
Lumbar spine (T-score) 1
-2.6 ± 1.0
-3.0 ± 0.7
-2.2 ± 1.1 *
Total hip (T-score) 2
-1.9 ± 0.9
-2.1 ± 0.9
-1.8 ± 0.9
Current mean prednisolone use (mg/day)
3.1 ± 5.3
0.2 ± 0.9
5.7 ± 6.1 *
Calcium supplements3:
- No prescription (n, (%))
- Prescription of 500 mg/day (n, (%))
- Prescription of 1000 mg/day (n, (%))
- Other amount of prescription (n, (%))
- Mean intake via prescribed supplements (mg/day)
5 (7.6)
46 (69.7)
13 (19.7)
1 (1.5)
524 ± 292
3 (9.7)
23 (74.2)
4 (12.9)
0 (0)
475 ± 281
2 (5.7)
23 (65.7)
9 (25.7)
1 (2.9)
566 ± 298
Vitamin D supplements3:
- No prescription (n, (%))
- Prescription of 400 IU/day (n, (%))
- Prescription of 800 IU/day (n, (%))
- Other amount of prescription (n, (%))
- Mean intake via prescribed supplements (IU/day)
3 (4.5)
18 (27.3)
39 (59.1)
5 (7.5)
609 ± 273
2 (6.5)
10 (32.3)
16 (51.6)
2 (6.4)
538 ± 283
1 (2.9)
8 (22.9)
23 (65.7)
3 (8.6)
670 ± 252 *
Dietary calcium intake
Calcium intake via calcium intake list (mg/day)
824.5 ± 259.4
882.9 ± 284.7
772.7 ± 226.5
Calcium intake via dietary history (mg/day)
1113.0 ± 423.6
1201.6 ± 413.1
1034.5 ± 423.1
Difference in calcium intake between calcium intake list and dietary history (mg/day)
288.5 ± 345.5 �
318.7 ± 346.2
261.8 ± 347.7
Table 1: General characteristics.
Validation of the calcium intake list
The mean difference between the calcium intake list and the DH was 288.5 ± 345.5 mg calcium per day (p<0.001). Compared to the DH as reference method, the calcium intake list underestimated dietary calcium intake with 250 mg or more in 37 of the 66 patients (56.1%), whereas it overestimated dietary calcium intake with 250 mg or more in only 4 patients (6.1%). Thus, in 62% of the subjects there was a clinically relevant discrepancy between the calcium intake list and the DH. This is displayed in the Bland–Altman plot in Figure 3. This plot also indicates that the calcium intake list underestimates calcium intake more often in patients with a higher calcium intake.
Figure 3: Difference versus mean calcium intake (mg⁄day): Bland–Altman plot. The solid line represents the mean difference in calcium intake (−288.5 mg⁄day). The dotted lines are the limits of agreement defined as ±1.96 standard deviations of the difference. In grey, the area of non–clinically relevant difference (−250 to 250 mg⁄day) is displayed.
The calcium intake list used fixed portion sizes of 150 ml for milk, yoghurt, quark, custard, pudding, and porridge, 20 grams for cheese, and a ‘rest’ group of 250 mg calcium from other products. After having performed the DH’s, we also quantified the actual portion sizes according to the DH. These turned out to be higher for milk products (250 ml) and for yoghurt, quark, custard, pudding, and porridge (200 ml). No difference was observed for the portion size of cheese. According to the DH, the ‘rest’ group contained 340 mg calcium per day.
In addition, we calculated which products contributed most too dietary calcium intake per day. Dairy products accumulated for approximately 62% in total calcium intake (seven out of ten products were dairy products and cheese). The other three product categories were vegetables (6.3%), water (3.1%), and tea (3.0%). The calcium concentration of these products is low compared to the calcium concentration of dairy products and cheese, but because of the high number of servings, their contribution to the total calcium intake is worth mentioning.
In addition to the dietary calcium and the prescribed calcium supplements, 32 subjects used other (over–the–counter) micronutrient supplements on own initiative. Seventeen of them (25.8%) used overthe– counter supplements containing calcium, with a mean extra calcium intake of 254.0±354.4 mg per day.
The mean total intake of calcium per day (nutrition plus (all) supplements) was significantly higher than the upper limit of the current Dutch recommendation of 1200 mg calcium per day in 55 out of 66 subjects (83.3%). Only 6.5% of the subjects (n=5) did not reach the lower limit of the recommendation of 1000 mg calcium per day.
For total dietary intake, no differences were found between patients with primary and secondary osteoporosis. Also no differences were found between patients using prednisolone or not, neither for dietary intake of calcium (p=0.660) nor for prescribed calcium supplements (p=0.464). Although dietary intake of calcium showed no difference between younger and older subjects (p=0.105), the total intake of calcium was lower in older than in younger subjects (p=0.022). A trend was shown for a lower prescription of calcium supplements to older subjects (p=0.060). Furthermore, subjects with the lowest T–score of the lumbar spine (T–score ≤ 3.4) had a higher total calcium intake compared to other subjects (p=0.043), which was not shown for subjects with the lowest T–score of the hip.
Comparison of the amounts of prescribed calcium and vitamin D supplements taken, showed a higher intake of vitamin D for patients with secondary osteoporosis (p=0.030), probably explained by more regular consultations with the rheumatologist.
Discussion
The main conclusion from this study is that the currently used calcium intake list results in a substantial and clinically relevant underestimation of at least 250 mg calcium per day in 56% of osteoporosis patients, and a clinically relevant overestimation of at least 250 mg calcium per day in 6% of osteoporosis patients. As a result, in the majority of patients calcium supplements were prescribed in higher doses than needed, leading to a calcium intake higher than the upper limit of the current Dutch recommendation of 1200 mg calcium per day in 83% of patients.
We identified two possible explanations for the underestimation of calcium intake by the calcium intake list: the standardized portion sizes were too small and the calcium content of the ‘rest’ group was higher than 250 mg. The underestimation was found to be clinically relevant, which might result in too high calcium supplement prescriptions.
The recent commotion around a too high intake of calcium supplements, which was the reason for this validation study, arose from one RCT and two meta–analyses of Bolland et al. [1,6,7]. All three studies found an association between calcium supplements and an increased risk of myocardial infarction. The circumstances described in these studies are much in accordance with our study: the majority of the participants were female, they were predominantly postmenopausal, and the prescription of calcium supplements was 500 mg per day or more. In contrast, the RCT of Lewis et al. [2] and results presented by Paik et al. [8] did not demonstrate an association between the use of calcium supplements and an increased cardiovascular risk. Thus, these studies show conflicting conclusions, and the rumour about the possible relationship between calcium supplements and cardiovascular risks persists. Therefore, it continues to be important to make an accurate estimation of the dietary calcium intake, to be able to prescribe the adequate amounts of calcium supplementation to reach the recommendation of 1000 to 1200 mg calcium per day, without increasing the possible risk of cardiovascular events.
There are few alternatives for a ‘quick and easy’ estimation of dietary calcium intake. A DH is not feasible for daily practice since performing and processing one DH takes about 90 minutes per patient and the DH has to be conducted by an experienced dietician. As surrogate, several food frequency questionnaires have been developed which have been validated for calcium intake of osteoporosis patients. These questionnaires take less time and can be performed by nondieticians, but they are still too time–consuming for busy clinical practice of rheumatologists, since they contain between 28 and 60 items [9,10]. Therefore, a valid short calcium intake list would be the most suitable option for physicians to estimate calcium intake of their osteoporosis patients. Unfortunately, the list validated in this study turned out not to be valid.
To validate the calcium intake list, the best method would have been a dietary record collected over several days, in a larger study population [11]. However, this was not feasible, due to constraints in time, number of patients, and burden for the patients. A food frequency questionnaire [5] validated for calcium intake, was not an eligible reference method, since this questionnaire measures calcium intake more or less in the same way as the short calcium intake list, resulting in the same errors. Therefore, in this study we chose to use a DH with specific focus on calcium. The most important limitations of the DH as reference method are the perception of portion sizes and the reliability on memory. We tried to reduce these limitations by paying extra attention to portion sizes (using samples of cups, glasses, bowls, and slices of cheese) and by excluding patients with cognitive impairment.
One of the limitations of this study is that, although we work on the optimization of the estimation of dietary calcium intake, we do realize that there are inter–individual differences in intestinal calcium absorption. However, more sophisticated methods, for instance with isotopes, are expensive, difficult to perform, and therefore not widely applicable. Another issue is that we cannot quantify the amount of calcium in the blood that is incorporated in the bone. Nevertheless, we have the impression that improving the estimation of dietary calcium intake is important for more than one reason: besides the aforementioned possibly increased risk of cardiovascular events, also constipation, flatulence, diarrhoea, and nausea are regularly encountered side–effects when using calcium supplements. Last but not least, accurate calcium prescriptions might lead to the reduction of health costs. In 2012, the total costs of calcium supplements in the Netherlands were around 50 million Euros [12], which might be reduced in the future when calcium supplements are prescribed more accurately. Therefore, we suggest designing a new short calcium intake list, which needs to be validated additionally.
The conclusion of this study is that the current short calcium intake list is not valid, as it gives a substantial and clinically relevant difference of dietary calcium intake in 62% of patients treated for osteoporosis. In 56% of the patients, this was a clinically relevant underestimation, since there is a purported association between a too high overall calcium intake and an increased risk of cardiovascular events. This study shows that estimation of dietary calcium intake needs to take portion sizes into account. More research is needed to develop and validate a short calcium intake list for use in clinical practice.
References