
Case Report
Austin J Orthopade & Rheumatol. 2015;2(1): 1013.
Traumatic Posterior Hip Dislocation in a 5-Year-Old: A Case Report and Review of the Literature
Adam D. Bitterman¹*, Brett Auerbach¹, Shalin Shah³ and Francisco Javier Laplaza²
Department of Orthopedic Surgery, Plainview Hospital,USA
New York Institute of Technology College of Osteopathic Medicine, USA
Department of Pediatric Orthopaedic Surgery, Cohen Children’s Medical Center, USA
*Corresponding author: Adam D. Bitterman,Department of Orthopaedic Surgery, Department of Medical Education, NS/LIJ Plainview Hospital, 888 Old Country Road, 25 Building, Plainview, NY 11803, USA, Tel: (516) 719-2546; Fax: (516) 719-2766; Email: Adam.Bitterman@gmail.com
Received: November 20, 2014; Accepted: March 19, 2015; Published: March 26, 2015
Abstract
Traumatic hip dislocations in children are uncommon, yet constitute an orthopaedic emergency. Furthermore, the insignificant mechanism of injury oftentimes leads to a potential miss or delay in diagnosis. The nature of the injury may seem minor so as to not pursue further workup. For this reason it is imperative to have a high index of suspicion, as clinical assessment and judicious imaging are key to obtaining the patient’s correct diagnosis. Although there are various complications that may result from such an injury, the most commonly encountered and most catastrophic is Avascular Necrosis (AVN), of the femoral head; early concentric reduction is crucial in minimizing this risk and optimizing patient outcomes.
Case Report
This is a case of a 5-year-old, Caucasian male with no significant medical history, who presented with severe left hip pain as well as a deformed left lower extremity. His parents reported that he was playing with his cousin when he suddenly fell and was no longer to able to bear weight on his left leg. The injury occurred roughly thirtyfive minutes prior to arrival at the emergency department.
Upon physical examination his left lower extremity was flexed at the hip, internally rotated and slightly adducted. He had no sensory or motor deficits and his pulses were palpable at the dorsalis pedis and posterior tibial arteries. His foot was warm and well-perfused. Radiographic evaluation of the pelvis and hip demonstrated a posterior native hip dislocation without any obvious fractures (Figure 1,2).
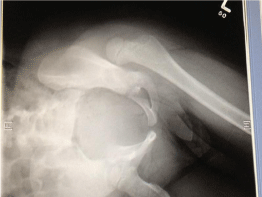
Figure 1: AP radiograph of the left hip demonstrating gross dislocation.

Figure 2: Clinical picture of the child’s left leg position while in bed in the ED.
He was taken to the operating room emergently, approximately two hours after initial presentation and 2.5 hours post-injury, where general anesthesia was initiated. Using fluoroscopy the left hip was closed reduced using gentle manipulation. Post-procedural radiographs confirmed the reduction and demonstrated a concentric left hip joint (Figure 3). A well-padded one-and-a-half leg hip spica was applied for additional stability.
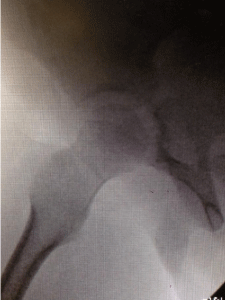
Figure 3: Fluoroscopic image of the left hip demonstrating a concentric
reduction of the hip joint after a closed reduction was performed under
general anesthesia.
He was discharged home on post-procedural day two after appropriate arrangements for home care and home schooling were coordinated. He remained in the spica cast for a total of four weeks. Upon his six-week follow-up, his hip was found to have maintained a concentric reduction. Clinically he was ambulating with a slight limp but had no ill effects from the injury. His most recent follow-up at three months post-injury, the patient is ambulating without any limp and has no pain from his native left hip dislocation. His parents were alerted of the high risk of avascular necrosis associated with this injury and were instructed to return to the clinic should his pain return. He was released to full activity without any restrictions.
Discussion
The disabling effects of a dislocated hip in children were clearly described by Hippocrates circa 400 BC, but its etiology was poorly understood [1]. The rare nature of this injury was subsequently documented in 1922, when a review of all hip dislocations treated at the Rizzoli Orthopedic Institute revealed only 3 pediatric cases out of a total 1,842 [2]. As in adults, traumatic hip dislocations in children are most often posterior in nature, with a clear predominance of male individuals [3,4]. Many of these patients present with the classic clinical picture of a shortened limb with the hip flexed, adducted, and internally rotated. It is important to note that the patient may present exclusively with referred knee pain, demonstrating a need for suspicion of underlying hip pathology [5,6]. With regards to radiographic evaluation, anteroposterior (AP), and cross-table lateral radiographs can detect the majority of cases. Additionally, these images are well-tolerated, readily available, and show the relevant osseous anatomy [5,7].
Of the potential complications, the most commonly encountered and also the most catastrophic is avascular necrosis of the femoral head. Although necrotic bone was described as far back as 400 B.C., early medical literature only recognized it in the setting of osteomyelitis. The first case report of AVN, attributed particularly to disruption of blood flow, was subsequently documented in 1870 by Francis Paget [8]. The basis of the repair of such osteonecrotic bone came to light several decades later in 1930, where Phemister et al. concluded that the contact of necrotic bone with living bone stimulates an ingrowth of vessels and osteogenic tissue into the dead tissue [9].
AVN is defined by the death of bone tissue due to a lack of blood supply. In the case of hip dislocations, the medial and lateral femoral circumflex arteries are susceptible to such disruption. Radiographs may not show evidence of necrosis for several weeks; however, MRI and bone scan can be used for earlier detection. Interestingly, a review of several cases show that the changes noted on radiographs are strikingly similar to those of Legg-Calve-Perthes disease; this refers to the sclerosis, initial flattening of the epiphysis, along with early fragmentation [5,3,6,10].
The significance of early reduction is stressed by studies that showed the incidence of AVN rises to over 65%, from the average 8-10%, if reduction is delayed 24 hours after dislocation [6,11]. The classic report by Mehlman et al. concluded that patients whose hips were reduced more than 6 hours after injury had a 20-fold increase in the risk of developing avascular necrosis [12]. Moreover, AVN may develop up to 3 years after the inciting injury [5]. Delays in diagnosis are commonly encountered not only due to the rarity and minimal amount of trauma that may be involved, but also to the presence of other injuries that may divert attention from the hip injury [4,10].
Several reports confirm that there is a direct correlation between AVN and time to reduction rather than with time to weight bearing. It is important to note that a reduction in less than 6 hours does not preclude the risk of avascular necrosis [5]. This is supported by Chung’s study on normal hips depicting that 23% of autopsied children had incomplete anastomotic networks and only 1.3% had transepiphyseal vessels [13]. Other complications that are not as commonly encountered but important to keep in mind include myositis ossificans, post-traumatic osteoarthritis, premature physeal fusion, and sciatic nerve injury [14].
Incidences and outcomes
The relatively rare nature of pediatric hip dislocations is depicted by the fact that they consist of less than 5% of all traumatic hip dislocations, including those in adults [5,14]. The immature skeleton of a child predisposes itself to such injuries from both clear and seemingly unremarkable mechanisms. The provoking event may range from simple playground activities, to competitive sports. Several studies stratified the patient populations into two groups, younger and older, with the magnitude of force producing the injury shown to increase with age. The younger group, ranging from 2 to 8 years of age, yielded dislocations from lower energy trauma compared to those in the older group, which was defined as older than 10 years of age [14-16]. This difference was attributed to the greater degree of ligamentous laxity in younger children. With increasing age, joint laxity decreases, and growth cartilage calcifies resulting in a diminished cartilage to bone ratio [3,4,10,11,17]. For this reason, children also have fewer associated injuries compared to adults, who commonly present with concomitant acetabular fractures. This provides us with reasoning that older children may sustain associated fractures compared to the younger pediatric population with greater bone plasticity. Considering this population’s exquisite remodeling potential, if managed in a timely manner, the outcomes are markedly favorable and many patients may continue to participate in high intensity activities.
Treatment
Prompt closed reduction under general anesthesia is key to the patient’s long-term prognosis, ideally within 6 hours of the inciting injury. The significance of a concentric reduction is based on the concept that proper anatomic placement serves as a stimulus for growth of the pelvis and the femur. This prevents deformity and maintains proper limb length [11]. Muscular relaxation may also be crucial, as older children are at risk for fracturing their physis with such reduction maneuvers [3]. Additionally, pain management is essential, and a quick and effective method reported for use in the emergency department is intranasal fentanyl administration [5].
The maneuvers used for closed reduction in adult dislocations can be utilized for pediatric patients as well, including the Allis, Bigelow, and Stimson maneuvers [5,17]. It has also been suggested that aspiration of the joint after closed reduction should be done to drain the hemarthrosis in an attempt to improve the vascular supply and decrease capsular distention [15]. If closed reduction cannot be achieved after one or two attempts, then open reduction should be performed [5,11]. Furthermore, interposition of particular structures such as labrum, capsule, or osteochondral fragments may limit a complete reduction. This would manifest as articular widening and incongruency on post-reduction radiographs, which also requires surgical intervention [3,16]. Additional indications for surgical exploration and intervention include associated fractures of the femoral neck or acetabulum, and those patients that present late. As each minute delays a favorable prognosis, many of these patients are almost guaranteed to have avascular necrosis. Nonetheless, there is still significant functional improvement following operative intervention [5,10]. An analysis by Hung suggests that if the patient presents over 3 weeks after a dislocation, the surgical intervention may include releasing the adductor longus, lengthening the psoas tendon, and inserting a Kirschner wire to secure the hip into the joint [18]. If both closed and open reductions fail, salvage procedures including arthrodesis, osteotomy, and excisional arthroplasty are additional options in managing these patients [10,19].
It is important to follow up the hip reduction with quality radiographs. Not only does this allow for comparing congruency between joint spaces, but also rules out fractures or other conditions that may further interfere with the patient’s recovery [4,17]. A postreduction joint space asymmetry of 3 mm or greater is an indication for a CT scan [5,12]. Although there have been no definitive conclusions, several studies have proven that 6 weeks of immobilization in a spica cast is sufficient to precede weight bearing of the affected limb [4,17].
Conclusion
Our case presentation emphasizes the importance of maintaining a high degree of suspicion when evaluating a child with a potential hip injury – especially because traumatic dislocations are 25 times less common in children than in adults [10,11]. As children are active by nature, their immature skeletons predispose them to this orthopaedic emergency [20]. There seems to be a proportional increase in the force necessary to cause dislocation with increasing age [3,5,16]. Having a familiarity with management is key to improving patient prognosis and limiting further morbidity. Timely reduction, ideally within 6 hours of the inciting injury, is the standard used to prevent the disabling complications, of greatest importance being avascular necrosis of the femoral head.
References
- Bowen JR, Kotzias-Neto A. Developmental dysplasia of the hip. 5th edn. Brooklandville, Md. Data Trace Publishing Company. 2006.
- Mason ML. Traumatic dislocation of the hip in childhood: Report of a case. J Bone Joint Surg Br. 1954; 36: 630-632.
- Herrera-Soto JA, Price CT. Traumatic hip dislocations in children and adolescents: pitfalls and complications. J Am Acad Orthop Surg. 2009; 17: 15-21.
- Zrig M, Mnif H, Koubaa M, Abid A. Traumatic hip dislocation in children. Acta Orthopaedica Belgica. 2009; 75: 328-333.
- Bressan S, Steiner IP, Shavit I. Emergency department diagnosis and treatment of traumatic hip dislocations in children under the age of 7 years: a 10-year review. Emerg Med J. 2014; 31: 425-431.
- Singhal R, Perry D, Cohen D, Bruce C. Delayed diagnosis of traumatic hip dislocation mimicking Perthes disease in a child. BMJ Case Reports. 2011.
- Haverstock JP, Sanders DW, Bartley DL, Lim RK. Traumatic Pediatric Hip Dislocation in a Toddler. J Emerg Med. 2013; 45: 91-94.
- Bishop AT, Pelzer M. Avascular necrosis. Berger RA, Weiss APC, editors. In: Hand Surgery. Philadelphia, PA: Lippincott Williams & Wilkins. 2004; 549-575.
- Phemister DB. Repair of bone in the presence of aseptic necrosis resulting from fractures, transplantations and vascular obstruction. J Bone Joint Surg Am. 2005; 87: 672.
- Kumar S, Jain AK. Neglected traumatic hip dislocation in children. Clin Orthop Relat Res. 2005; 9-13.
- Coll GF, Del Rio LT, Nuno LG, Burniol JR, Carol RH. Traumatic hip dislocation in childhood. Hip Int. 2010; 20: 524-528.
- Mehlman CT, Hubbard GW, Crawford AH, Roy DR, Wall EJ. Traumatic hip dislocation in children: Long-term follow-up of 42 patients. Clin Orthop Relat Res. 2000; 68-79.
- Chung SM: The arterial supply of the developing proximal end of the human femur. J Bone Joint Surg Am. 1976; 58: 961-970.
- Hamilton PR, Broughton NS. Traumatic hip dislocation in childhood. J Pediatr Orthop. 1998; 18: 691-694.
- Reiger H, Penning D, Klein W, Grunert J. Traumatic dislocations of the hip in young children. Arch Orthop Trauma Surg. 1991; 110: 114-117.
- Vialle R, Odent T, Pannier S, Pauthier F, Laumonier F, Glorion C. Traumatic hip dislocation in childhood. J Pediatr Orthop. 2005; 25: 138-144.
- Meena S, Kishanpuria T, Gangari SK, Sharma P. Traumatic posterior hip dislocation in a 16-month-old child: a case report and review of literature. Chin J Traumatol. 2012; 15: 382-384.
- Hung NN. Traumatic hip dislocation in children. J Pediatr Orthop. 2012; 21: 542-551.
- Banskota AK, Spiegel DA, Shrestha S, Shrestha OP, Rajbhandary T. Open reduction for neglected traumatic hip dislocation in children and adolescents. J Pediatr Orthop. 2007; 27: 187-191.
- Kumar JN, Hazra S, Yun HH. Redislocation after treatment of traumatic dislocation of hip in children: a report of two cases and literature review. Arch Orthop Trauma Surg. 2009; 29: 823-826.