
Research Article
Austin J Orthopade & Rheumatol. 2015;2(2): 1014.
A Pilot Study of a Novel Treatment Method for Refractory Painful Plantar Fibromas
Mihir M. Patel*, Sahvan M. Patel, Sia S. Patel and Jacob Daynes
Department of Orthopedic Surgery, OrthoIndy, USA
*Corresponding author: Mihir M Patel, Department of Orthopedic Surgery, OrthoIndy 8450 Northwest Blvd, Indianapolis, Indiana 46278, USA
Received: March 18, 2015; Accepted: April 22, 2015; Published: April 22, 2015
Abstract
Introduction: Painful plantar fibromas may make ambulation difficult for patients. They may recur and can make shoe wear difficult to purchase. Treatment modalities may include conservative care, modified shoe wear, injections and orthotics. Surgical treatment may include open excision. The TX1A probe by Tenex Inc may be a useful alternative treatment modality for these painful lesions.
Materials and Methods: From 2011 through 2014, eight patients who had painful plantar fibromas elected to undergo definitive treatment for the fibromas. They all had had conservative care including modifications of shoes and either over the counter orthotics or custom orthotics. They all had advanced imaging tests (MRI or CT) preoperatively to help delineate the lesions. The definitive treatment utilized arthroscopy and the TX1A probe and was performed on an outpatient basis.
Results: Preoperative AOFAS score was 30.8 (20-36). Postoperative AOFAS score was 90.1 (85-92). Average time of resolution of symptoms was 63.5 days (30-112) and average follow-up was 2.5 years. One patient had another lesion become painful but it was in a different location than the index operation. No others have had a recurrence to date. Pathology specimens were all negative for malignancy. All patients were discharged from care. No infections were recorded.
Conclusion: The TX1A probe by Tenex Health appears to be a safe, effective method for removing painful plantar fibromas in patients who have failed all conservative measures. Surveillance is ongoing.
Keywords: Plantar fibroma; Plantar fibromatosis
Introduction
Fibromas often occur in the plantar aspect of the foot. Many of these patients may have noticed a lump for a number of years for which they wish to be evaluated. The condition may be related to Dupuytren contracture in the hand and Peyronie’s disease [1]. Risk factors of developing this may include Scandinavian descent [1,2]. These lesions in the majority of cases are painless and no treatment is required besides observation. [2] However, in a subset of these patients, the fibromas within the foot may become painful. In those instances, patients will seek further treatment to diminish the pain to help continue active, or even routine, lifestyles.
Materials and Methods
In the senior author’s referral practice, from 2011 through 2014, 127 patients were seen with fibromas. They all had had conservative care including modifications of shoes and either over the counter orthotics, modified padding on the insole, custom orthotics, physical therapy or an injection with lidocaine/20 mg of depo medrol based on previous treatment modalities from referring physicians. Physical therapy consisted of external deep tissue massage, passive and active stretching, attempting to reduce the size of the fibroma. These referring physicians may have included their primary care physician, orthopedic surgeon, or rheumatologist. They all had advanced imaging tests (MRI or CT based on comorbidities) preoperatively to help delineate the lesions and to rule out potential malignant characteristics. The advanced imaging tests were reported by board certified radiologists. Eight of these patients who had solitary painful plantar fibromas utilizing the TX1A probe elected to undergo definitive treatment for the fibroma when conservative care failed.
The TX1A device
The equipment consists of an energy module, a pump /suction cassette for delivering the irrigation and suction through the probe, and a probe itself, the TX1A, which is the size of an 18 gauge needle that delivers the ultrasound energy. The cassette is inserted into the energy module and the ultrasound energy probe is primed so it will deliver the irrigation fluid, normal saline. . The safety features of the energy module are such that no energy is expended unless the system is properly irrigating and aspirating the diseased tissue [3] Figures 1, 2.

Figure 1: Tenex Health TX1A Probe. The TX1A probe is attached to a
cassette that inserts into the console.

Figure 2: Tenex health console. Settings on the console were placed on
medium for the removal of the fibromas.
Definitive treatment utilizing arthroscopy and the TX1A probe (Figures 1, 3) was in an outpatient basis. Specimens were sent to pathology to confirm fibrotic tissue and no malignancy. Immediately postoperatively, patients were partial weight bearing as tolerated in a postoperative shoe following the procedure until the incision healed. They were then weight bearing as tolerated. Follow-up was until discharged from care and call backs were made at time of data collection. Preoperative and postoperative AOFAS scores were obtained. Physical therapy was offered to patients postoperatively.
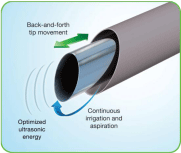
Figure 2: Tx1A Probe. The tip of the probe delivers the ultrasonic energy with
continuous irrigation and aspiration to remove the diseased tissue.
Results
The average age of patient was 51.3 years (17-71) and time of painful symptoms was 15.1 months (3-36). Six patients had MRIs which were negative for malignant features and one patient had two CT scans due to a spinal cord stimulator. All of the advanced imaging tests were negative for malignant features. The preoperative AOFAS score was 30.8 (20-36) despite all having had modified footwear and orthotics. Following the procedure, the average time of resolution of symptoms was 63.5 days (30-112), resulting in a mean postoperative AOFAS score was 90.1 (85-92). One patient had another lesion become painful but it was in a different location on the foot than the index operation. This particular patient had a new painful fibroma develop distal to the original site on the midfoot. The second site on the forefoot had not been painful at the index operation so observation had continued until it became painful and conservative care had failed for that lesion as well. No recurrences have occurred since the index operation. Pathology specimens were obtained in all and none revealed any evidence of malignancy by board certified pathologists. There were no wound complications or deep infections following the procedure. None of the patients developed postoperative painful scarring at the site of the lesion. All patients were discharged from care.
Discussion
Our experience with fibromas reflects the published literature as most are painless and no intervention is required. [2,4]. The majority of these lesions are superficial growths which are painless and no further treatment is needed beyond conservative care [1]. However, when patients present with a painful mass in the plantar aspect of the foot, potential malignancy is a paramount consideration of both the physician and patient. Kirby et al showed eight-seven percent of soft tissue tumors and tumor like lesions were benign, with ganglion cysts and plantar fibromas being the most common. Thirteen percent were malignant tumors, of which forty-five percent were synovial sarcomas [5]. Radiographs, ultrasound and MRI may help to distinguish the benign from the malignant lesion [6]. Synovial cell carcinoma may show calcifications on a plain radiograph and MRI may show the lesion. Melanoma may show a nodule on the plantar aspect of the foot with clinical signs that may include bleeding, itchiness, tenderness, and /or pain. Alternative conservative care for fibromas may possibly include collagenase injections [7]. When all conservative management fails, surgery is considered. However, concern with the morbidity and potential recurrence are limiting factors when considering this modality. Complications of an open procedure may include painful scarring from the incision on the plantar aspect of the foot, residual paresthesias from injury to the digital nerves, and ruptures of tendons or of the plantar fascia [8]. Sammarco et al described the operative staging system which correlated well with postoperative wound healing, skin necrosis, and recurrence [9]. With arthroscopy, the TX1A probe from Tenex Health, Inc. provides a reliable minimal invasive solution for removal of the superficial painful lesion to help avoid complications of larger, open procedures. Physician preference may include utilizing ultrasound instead of, or in addition to, arthroscopy to image the lesion when using the TX1A probe [3]. Additionally, zero recurrence rates of the lesion with the TX1A probe compare favorably to the larger, open procedures (8,10). Although this pilot study is encouraging, future studies will be required to fully demonstrate the ultimate effectiveness of this modality.
Conclusion
The TX1A probe by Tenex Health seems to be a safe, effective well tolerated outpatient method comparable to formal surgical excision ,but with considerable less morbidity, for removing painful plantar fibromas in patients who have failed all conservative measures.
References
- Gudmundsson KG, Jonsson T, Arngrimsson R. Association of Mobrus Ledderhose with Dupuytren’s contracture. Foot Ankle Int. 2013; 34: 841-845.
- Veith NT, Tschernig T, Histing T, Madry H. Plantar fibrmastosis – topical review. Foot and Ankle Int. 2013; 34: 1742-1746.
- Koh JS, Mohan PC, Howe TS, Lee BP, Chia SL, Yang Z, et al. Fasciotomy and surgical tenotomy for recalcitrant lateral elbow tendinopathy: early clinical experience with a novel device for minimally invasive percutaneous microresection. Am J Sports Med. 2013; 41: 636-644.
- Aluisio FV, Mair SD, Hall RL. Plantar fibromatosis: treatment of primary and recurrent lesions and factors associated with recurrence. Foot Ankle Int. 1996; 17: 672-678.
- Kirby EJ, Shereff MJ, Lewis MM. Soft-tissue tumors and tumor-like lesions of the foot. An analysis of eighty-three cases. JBJS Am. 1989; 71: 621-626.
- McNally EG, Shetty S. Plantar fascia: imaging diagnosis and guided treatment. Semin Musculoskeltal Radiology. 2010; 14: 334-343.
- Hammoudeh ZS. Collagenase Clostribdium histolyticum injection for plantar fibromatosis (Ledderhose disease). Plast Reconstruc Surg. 2014; 134: 497e-498e.
- AOFAS. Plantar Fibroma and Plantar Fibromatosis.
- Sammarco GJ, Mangone PG. Classification and treatment of plantar fibromatosis. Foot Ankle Int. 2000; 21: 563-569.
- Van der Veer WM, Hamburg SM, de Gast A, Niessen FB. Recurrence of plantar fibromatosis after plantar frasciectomy: single-center long-term results. Plast Reconstr Surg. 2008; 122: 486-491.