Clinical Image
Austin J Orthopade & Rheumatol. 2015;2(2): 1015.
Posterior Vertebral Scalloping in Neurofibromatosis
Vela P* and Andrés M
Department of Rheumatology, Hospital General Universitario de Alicante, University Miguel Hernandez, Spain
*Corresponding author: Paloma Vela Casasempere, Department of Rheumatology, Hospital General Universitario de Alicante, University Miguel Hernandez, Maestro Alonso 109, Alicante, Spain 03010
Received: May 17, 2015; Accepted: May 18, 2015; Published: May 26, 2015
Keywords
Neurofibromatosis type 1; Von Recklinghausen’s disease; Myelomeningocele
Clinical Image
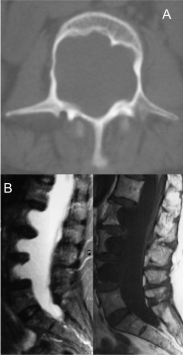
A 51-year-old woman complained of sudden-onset low back pain. Physical exam did not reveal any abnormality, except for the presence of multiple café-au-lait macules and cutaneous neurofibromas in the context of a known neurofibromatosis type 1. An X-ray showed marked L2-L4 posterior vertebral body scalloping (Figure 1); CT (a) and MRI (b) confirmed the absence of the posterior aspect of the vertebral bodies and an anterior meningocele (Figure 2); no paraspinal neurofibromas were detected. Back pain resolved shortly with analgesic and muscle relaxant. No other measures were taken, and ten-year follow-up has confirmed the incidental finding of this case. Neurofibromatosis type 1 associates with spinal malformations and neural tube defects - such as dural ectasia or myelomeningocele - and is the most common cause of radiological vertebral scalloping [1,2]. These abnormalities associate with mechanical back pain, limb weakness or sphincter incontinences, but in some patients can be asymptomatic and incidentally diagnosed.
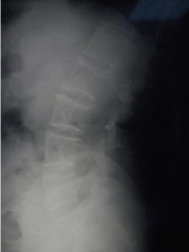
Figure 1: L2-L4 posterior vertebral body scalloping.