
Case Report
Austin J Orthopade & Rheumatol. 2015; 2(3): 1022.
Acute Pancreatitis Complicated with Acute Respiratory Distress Syndrome Following Lumbar Spinal Kyphoplasty, Instrumentation and Bone Cement Injection
Mahmoodi SM1*, Salwa AMI2, and Sujanith T3
1Department of Orthopedic Surgery, Gulf Medical Univerity, UAE
2Department of Internal Medicine, Gulf Medical Univerity, UAE
3Department of Anesthesiology, Gulf Medical Univerity, UAE
*Corresponding author: Mahmoodi SM, Department of Orthopedic Surgery, Gulf Medical Univerity/Thumbay Hospital, Al Qusais, Dubai, UAE
Received: September 02, 2015; Accepted: November 19, 2015; Published: November 27, 2015
Abstract
A 69 years old female patient stopped walking for two months after fall. She had severe back and legs pain with right leg weakness.MRI lumbar spine revealed L3 burst fracture with severe spinal canal stenosis. She was operated by spinal jack kyphoplasty, bone cement injection, laminectomy and pedicular screw fixation. Second postoperative day she developed acute pancreatitis that was complicated with Acute Respiratory Distress Syndrome (ARDS). Acute pancreatitis following lumbar kyphoplasty complicated with ARDS is not reported yet. Details of the case and management are discussed, and the literature is reviewed.
Keywords: Lumbar spine; Acute pancreatitis; Acute respiratory distress syndrome; Laminectomy; Kyphoplasty
Case Presentation
The mortality rate for acute pancreatitis in patients more than 55 years old is 20.63% [1] and is higher if the patient is overweight [2]. Postoperative pancreatitis is a relatively frequent complication after open biliary tract and gastric surgery [3] and is a recognized complication after spinal fusion in scoliosis [4] but it is rare after other spine surgeries [3]. We report the first case of acute pancreatitis following lumbar kyphoplasty, complicated with ARDS.
A female patient of 69 years old stopped walking for two months after she had a fall while she was walking at home. She had no complaints of bowel or bladder dysfunctions. She was not smoking and did not consume alcohol. Her past medical history was significant for diabetes and hypertension for 4 years duration. She was on Perindopril Erbumine (Coversyl) for hypertension and human insulin (Actrapid) for diabetes. Clinical Examination showed patient on wheelchair, height 155 cm, weight 70 kg, BMI 29.1, with severe low back pain radiating to her both legs, more to the right side. The right ankle and foot dorsiflexion forces were 3 out of 5 with bilateral sluggish ankle jerks. Due to right leg weakness and pain in the back
and legs, she was not able to stand or walk. Her CBC, kidney and liver function tests and lipid profiles, creatinine, PT. aPTT, ESR, CRP and urine test were normal. Lumbar spine X-rays and CT scan revealed healed L3 compression fracture (Figure 1). Magnetic Resonance Imaging (MRI) of the lumbar spine demonstrated burst fracture of vertebra L3 with posterior angulations and diffuse posterior disc bulge at L2-L3 causing severe spinal canal stenosis and compression upon theca and cauda equina. There was also diffuse posterior disc bulge at L3-L4 causing compression upon theca and corresponding nerve root exits (Figure 1).
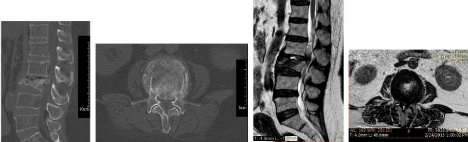
Figure 1: Preoperative sagittal and axial CT and MRI scans: healed compression fracture of L3 with retropulsed fragment and severe spinal canal stenosis.
She was operated on 03.03.2015 by bilateral transpedicular Romeo® spinal jack for L3 fracture along with Cohesion® bone cement injections (kyphoplasty). Laminectomy L2 to L5 and Spineart® pedicular screw fixation of L2 to L4 were done and the dura was covered by Oxiplex® adhesion barrier. Bilateral bone grafts were inserted posterolaterally after bony decortications.
She was admitted to ICU postoperatively, where she recovered from anesthesia uneventfully; was conscious, oriented and painfree, taking soft diet. Next day she developed epigastric pain that was
She was admitted to ICU postoperatively, where she recovered from anesthesia uneventfully; was conscious, oriented and painfree, taking soft diet. Next day she developed epigastric pain that was aggravating in intensity. Serum Amylase raised to 529 U/L (reference range 28-100 U/L), WBC count to 37.9x103/uL (reference range 4-10 x103/uL), lipase to 6003 U/L (reference range 73-393 U/L) and CRP to 315 mg/L (reference range less than 5 mg/L). CT scan and ultrasound abdomen showed acute pancreatitis with pancreatic enlargement, fuzzy inflamed peripancreatic fat and extension of the fat to the left lumbar and hypochondriac regions associated with loculated collection of fluid and mild to moderate ascites. There was no evidence of intra or extra hepatic dilatations. She was kept NPO and nasogastric tube was inserted. Lactate dehydrogenase, aspartate amino transferase, alkaline phosphatase, bilirubin, alanine amino transferase, blood urea nitrogen, creatinine, cholesterol, triglycerides, thyroid function tests and urinary output were normal. Her antibiotic (Ceftriaxone injection) was changed to Imipenem/ Cilastatin, Metronidazole and Fluconazole injections. Optimum glycemic control was maintained using intravenous insulin injections throughout her stay in the ICU. Blood and urine cultures were done, reported as negative after 48 hours. Deep vein thrombosis prophylaxis with sequential compression inflatable device was applied and Enoxaparin was stared. Central venous catheter was inserted for central venous pressure monitoring. Next day the amylase increased to 994 U/L and she developed respiratory distress with: tachypnea 26/min, heart rate 118/min and95% Spo2.Noninvasive ventilation (CPAP) was started but she could not tolerate it more than a day. On 06.03.2015 the respiratory rate increased to 40/min. Her electrolytes, proteins and blood sugar were deteriorated (Table 1) and arterial blood gas showed metabolic acidosis with impaired gas exchange (Table 2). X-ray and CT scan of chest showed bilateral basal pleural thickening, basal congestion with mild right pleural effusion.
Test
Result
Reference Range
Na
131.2 mmol/L
135-148 mmol/L
K+
3.1 mmol/L
3.5-4.5 mmol/L
Ca2+
0.55 mmol/L
1.12-1.32 mmol/L
Total protein
5 g/dL
6.6-8.7 g/dL
Albumin
2.8 g/dL
3.5-5.2 g/dL
Globulin
2.2 g/dL
2.3-3.5 g/dL
Fasting Blood Sugar
144 mg/dL
70-105 g/dL
Table 1: Electrolytes, proteins and blood sugar, third postoperative day.
Test
Result
Reference Range
pH
7.28
7.35-7.45
PaO2
71.7 mmHg
80-100 mmHg
cHCO3
14.30 mmol/L
22-29 mmol/L
PCO2
31.1 mmHg
35-45 mmHg
FiO2
0.4
-
Table 2: Arterial blood gas, third postoperative day.
Diagnosed as moderate ARDS with PaO2/FiO2 ratio 179.25, she was intubated for invasive Pressure-Controlled Synchronized Intermittent Mandatory Ventilation (PC-SIMV). The patient was sedated with Midazolam and Fentanyl infusions throughout her ventilator support. After ensuring bowel movements, nasogastric feeding was started with good absorption of the feeds. Aseptic precautions were adhered during her stay in the ICU for all
consultations and procedures. Brain CT scan was done that was normal. On 07.03.2015 her hemoglobin dropped down to 8.9 g/ dL from 12.4 g/dL that was reported on second postoperative day. Blood was transfused. Amylase returned back to normal after four days from operation date. The ventilator support was continued till 10.03.2015 when she started desaturating up to 84%. Clinical exam and chest X-ray revealed left lung collapse. Fiber-optic bronchoscopy was done to remove mucus plug and the lung expanded, maintaining good gas exchange.
Finally she was extubated on 17.03.2015 and mobilization was started. Postoperative CT scan showed kyphotic angle restored and anterior vertebral height regained, with no cement leakage (Figure 2). She has been followed for 6 months. She has got no new spinal symptoms and the pancreatitis has not relapsed.
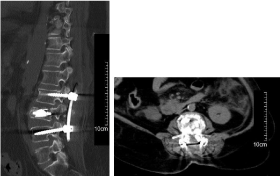
Figure 2: Postoperative sagittal and axial CT scan: wide laminectomy,
kyphotic angle restored, anterior vertebral height regained with no cement
leakage.
Conclusion
Postoperative pancreatitis, especially when it is complicated with respiratory distress syndrome, is associated with an increased incidence and severity of complications [5]. In 2014 Tauchi et al. have reported the first case of acute pancreatitis after posterior lumbar inter-body fusion for spondylolisthesis [3]. Laminectomy leading to acute pancreatitis is not reported in human being. Spriggs et al. have reported pancreatitis 19 days after L3-L4 hemilaminectomy in a binturong (Arctictis binturong) [6]. Still it is not clear why patients develop pancreatitis after surgeries remote from pancreas. Suboptimal positioning of the patient, prolonged surgical time, intraoperative blood loss [3] and drugs [7] are listed as possible causes. Also bone cement implantation may play a role in pancreatic tissue damage [8- 10].
Since the operation was done posteriorly, we kept the patient prone on positioning pads. The procedure duration was 5.5 hours. Considering her hypertension history and old age, the systolic blood pressure was maintained at around 120 mmHg and there was no hypotension during surgery. Blood loss was 300 mL with no need for blood transfusion. More than 130 drugs are implicated by case reports as causing acute pancreatitis [7]. Recently Scott Tenner has critically studied the role of drugs on acute pancreatitis. He believes the vast majority of drugs that have been supposed to cause acute pancreatitis, probably do not. Class Ia and Ib have the strongest evidence support for causing acute pancreatitis (Table 3) but other classes may not be, because in the studies the other causes are not ruled out [7]. Our patient did not take any of the class Ia and Ib medications, before or during surgery but she was given 200 mg Diprivan (Propofol) injection for anesthesia induction, that is in class II list. Araújo et al. have detected genotoxic effect for Polymethyl Methacrylate (PMMA) vapor on rats one day after exposure but have not found it evidently genotoxic after 5 days [8]. Pikis et al. have hypostatized PMMA thermal damage and/or chemical toxicity as the cause of cranial neuropathies and encephalopathies after cranioplasty on four patients [9]. Albrektsson and Linder have found immediate PMMA monomer effects, mainly vascular with blood flow disturbances, blood flow standstill, and intravascular hemolysis in animals studied for 350 days. The most striking finding in this study was that the extent of vascular disturbance was related to the type of tissue afflicted: in fatty marrow the effects were widespread, and in bone or fibrous tissue they were very limited [10].
Classification
Drug List
Class Ia: At least 1 case report with positive rechallenge, excluding all other causes, such as alcohol, hypertriglyceridemia, gallstones, and other drugs
Azodisalicylate, Bezafibrate, Cannabis, Carbimazole, Codeine, Cytosine, Arabinoside, Dapsone, Enalapril, Furosemide, Isoniazid, Mesalamine, Metronidazole, Pentamidine, Pravastatin, Procainamide, Pyritonol, Simvastatin, Stibogluconate, Sulfamethoxazole, Sulindac, Tetracycline, Valproic acid
Class Ib: At least 1 case report with positive rechallenge; but other causes, such as alcohol, hypertriglyceridemia, gallstones, and other drugs were not ruled out
All trans-retinoic acid, Amiodarone, Azathioprine, Clomiphene, Dexamethasone, Ifosfamide, Lamivudine, Losartan, Lynesternol/methoxyethinylestradiol, 6-mercaptopurine, Meglumine, Methimazole, Nelfinavir, Norethindronate/mestranol, Omeprazole, Premarin, Sulfamethazole, Trimethoprimsulfamethazole
Class II: At least 4 cases in the literature, consistent latency (75% of cases)
Acetaminophen, Chlorothiazide, Clozapine, Dideoxyinosine, Erythromycin, Estrogen, L-asparaginase, Pegaspargase, Propofol, Tamoxifen
Class III: At least 2 cases in the literature, no consistent latency among cases, no rechallenge
Alendronate, Captopril, Carbamazepine, Ceftriaxone, Cimetidine, Clarithromycin, Chlorthalidone, Cyclosporine, Gold, Hydrochlorothiazide, Indomethacin, Interferon and Interferon/ribavirin, Isotretinoin, Ketorolac, Lisinopril, Metolazone, Metformin, Mirtazapine, Naproxen, Paclitaxel
Class IV: Drugs not fitting into the earlier-described classes, single case report published in medical literature, without rechallenge
Ampicillin, Bendroflumethiazide, Benazepril, Betamethasone/Roxithromycin, Capecitabine, Colchicine, Cyproheptadine, Danazol, Diazoxide, Diclofenac, Ergotamine, Ethacrynic acid, Famciclovir, Finasteride, Fluvastatin, Ketoprofen, Lovastatin, Mefenamic acid, Nitrofurantoin, Octreotide, Oxyphenbutazone, Penicillin, Phenolphthalein, Propoxyphene, Ramipril, Ranitidine, Rifampin, Risperidone, Ritonavir, Sertraline, Strychnine, Tacrolimus, Vigabatrin/Lamotrigine
Table 3: Classification and list of drugs inducing pancreatitis.
We are reporting acute pancreatitis following lumbar kyphoplasty complicated with ARDS for the first time. The exact cause of acute pancreatitis is not clear in our case. Three possible causes are prolonged surgery, single Propofol injection and bone cement chemical effect. Spinal surgeons need to be vigilant to the possibility of postoperative pancreatitis and its complications. They have to have an expert and capable multidisciplinary supporting team, to manage such serious and fatal complication.
References
- Malik AM. Biliary pancreatitis. Deadly threat to the elderly. Is it a real threat? Int J Health Sci. 2015; 9: 35-39.
- Katuchova J, Bober J, Harbulak P, Hudak A, Gajdzik T, Kalanin R, et al. Obesity as a risk factor for severe acute pancreatitis patients. Wien Klin Wochenschr. 2014; 126: 223-227.
- Tauchi R, Imagama S, Ito Z, Ando K, Hirano K, Ukai J, et al. Acute pancreatitis after spine surgery: a case report and review of literature. Eur J Orthop Surg Traumatol. 2014; 1: S305-309.
- Borkhuu B, Nagaraju D, Miller F, Moamed Ali MH, Pressel D, Adelizzi-Delany J, et al. Prevalence and risk factors in postoperative pancreatitis after spine fusion in patients with cerebral palsy. J Pediatr Orthop. 2009; 29: 256-262.
- Bragg LE, Thompson JS, Burnett DA, Hodgson PE, Rikkers LF. Increased incidence of pancreas related complications in patients with postoperative pancreatitis. Am J Surg. 1985; 150: 694-697.
- Spriggs M, Arble J, Myers G. Intervertebral disc extrusion and spinal decompression in a binturong (Arctictis binturong). J Zoo Wildl Med. 2007; 38: 135-138.
- Tenner S. Drug induced acute pancreatitis: Does it exist? World J Gastroenterol. 2014; 20: 16529-16534.
- Araújo AM, Alves GR, Avanço GT, Parizi JL, Nai GA. Assessment of methyl methacrylate genotoxicity by the micronucleus test. Braz Oral Res. 2013; 27: 31-36.
- Pikis S, Goldstein J, Spektor S. Potential neurotoxic effects of polymethylmethacrylate during cranioplasty. J Clin Neurosci. 2015; 22: 139- 143.
- Albrektsson T, Linder L. Bone injury caused by curing bone cement. A vital microscopic study in the rabbit tibia. Clin Orthop Relat Res. 1984; 183: 280- 287.