
Review Article
Austin J Orthopade & Rheumatol. 2015; 2(3): 1023.
Arthroscopic Management of Soft Tissue Problems Aroud the Hip
Parodi D*, Lara J, Haydar MJ and Tobar C
Departamento de Ortopedia y Traumat ología, Universidad Austral de Chile, Chile
*Corresponding author: Parodi D, Department of Ortopedia y Traumat ología, Universidad Austral de Chile, Luis Pasteur 5259, Vitacura, Santiago, Chile
Received: September 23, 2015; Accepted: November 26, 2015; Published: November 27, 2015
Abstract
Peritrochanteric diseases are recurrent cause of lateral hip pain that usually affects middle age and active women. Despite questionable results, classically they have been treated in a conservative way. Surgical techniques are preferred for those who had unsatisfactory results with conservative treatment. In these patients we have developed an arthroscopic surgical treatment that included the bursa resection and the parcial release of the iliotibial band, showing satisfactory results. This article describes the surgical technique.
Introduction
With the development of hip arthroscopy, more attention has been focused on peritrochanteric diseases. Despite the questionable results, classic treatment options include therapeutic exercise, physical modalities, several corticosteroid injections, extracorporeal shock wave therapy, and regenerative injection therapies [1,2]. In thirtyfive patients with peritrochanteric disease, that didn´t responded to classic therapy, we have used surgical treatment and they have showed satisfactory results. This article describes the surgical technique that we have used.
Peritrochanteric diseases can be divided in two large groups: Lateral coxa saltans (snapping hip) and Greater trochanteric pain syndrome.
Lateral coxa saltans (Snapping Hip)
Corresponds to a clinical situation in which young patients, between 15 and 25 years old and 9/10 times women, have sliding of tensor fascia lata over the greater trochanter in a voluntary or involuntary form. This snapping occurs when the standing patient makes lateral movement of the hip, an adduction of the extremity, and most of the time during internal rotation. At this moment, the fascia lata goes abruptly from the anterior to posterior position in relation to the greater to chanter, making a visible snapping in the lateral face of the hip. Sometimes, it is accompanied by a clear snapping sound and pain.
In those patients that conservative treatment fails, surgery to release the fascia is proposed. There are multiple surgical techniques for this procedure [3]. The technique that we use is explained as follows.
Iliotibial band release: Technical Iliotibial Band Release from inside to outside
If the procedure is associated with arthroscopy of the medial compartment, we place the patient in supine position over an orthopedic traction table, but without traction ; if not, we place the patient over an operating radio lucid table; so the greater trochanter is identified, and we use the mid-superior and mid-inferior peritrochanteric portals (Figure 1A) [4].
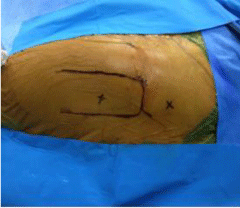
Figure 1a: Peritrochanteric portals.
A 70º optic camera is used through the lower portal, crossing the fascia lata in this step to enter in the peritrochanteric space. Once inside, we proceed to infiltrate the space with saline solution to distend it. After this, the superior portal is performed, first by inserting a needle guide until it is visible (Figure 1B), and second by expanding the portal with the dilators and introducing a non aggressive shaver and electrosurgical system to clean the peritrochanteric space [5,6].
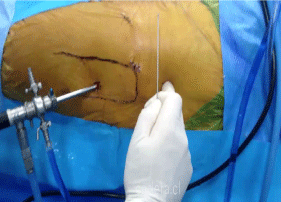
Figure 1b: The superior portal is performed, first by inserting a needle guide.
Once the peritrochanteric space is clear, a hypertrophic bursa may be present and must be removed. Anatomical points to be repaired are identified: greater trochanter, vastus lateralis, and the area of insertion of the gluteus maximus posterior to the vast us lateral is (Figure 2).
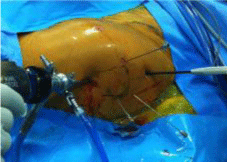
Figure 2: Reference points for the cruciform fasciotomy.
Once we have identified the (lateral) fascia lata, we proceed to mark reference points for make the fasciotomy in cruciform shape (Figures 3). The reference points (portals) are then joined when we perform the BIT fasciotomy, first completing the horizontal/ longitudinal portion, followed by the vertical (transverse) portion. This procedure is performed using radiofrequency and/or an arthroscopic shaver.
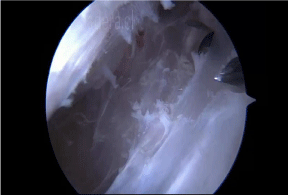
Figure 3: Completing the horizontal/longitudinal portion, followed by the
vertical portion.
Care should be taken to carry out correct hemostasis to avoid post operative hematoma. Rehabilitation begins the same day of surgery, with physical therapy that lasts for about 3-6 weeks depending on the patient response.
Greater trochanter pain syndrome
Frequent diagnoses include myofascial pain, trochanteric bursitis, tendinosis and rupture of the gluteus medius and minimus tendon. Furthermore, nerve entrapment like the piriformis syndrome must be considered.
Diagnoses of these pathologies are clinical, using imaging, typically high resolution hip Magnetic Resonance Imaging (MRI) of the hip. Gluteus medius and minimus injuries, and bursitis share common symptoms of pain in the lateral aspect of the hip, with pain radiating towards the lateral thigh, and into an ill-defined posterior gluteal zone [7,8]. An important clinical difference of gluteus medius injuries, where the insufficiency to stand monopodal, produces a Trendelenburg gait after a few seconds of being in this position (20- 30 sec).
MRI will distinguish between these similar clinical pathologies
Their management is initially conservative, but patients who do not respond should consider for surgical procedures [9]. In cases of bursitis (most frequent), surgical treatment includes arthroscopic resection of the bursa and the opening of the Iliotibial band longitudinally, similar to the coxa saltans, but only the longitudinal part of the fasciotomy is performed.
In the case of an injury to the tendon of the gluteus medius, it must be repaired, and can be identified at the time of exploration. The arthroscopic technique used is similar to that used with the coxa saltans, using the same portals when entering the peritrochanteric space. Once the gluteus medius injury is identified (Figure 4), we proceed to move it distally to its original position, and fix it with a suture technique that uses two-track anchors (Figures 5).
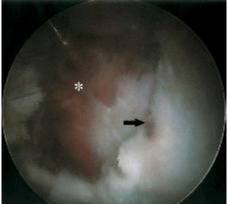
Figure 4: Gluteus medius injury identification.
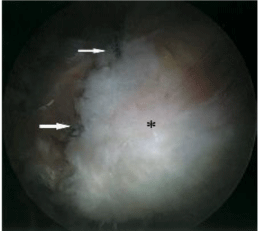
Figure 5: Gluteus medius fixing with suture with two-track anchors.
Prior to these anchors we cruented the bone in order to get a “ bleeding bed” where the tendon could heal, Post operative management of the reattachments includes the use of two crunches for 12 and avoid weight bearing as much as possible during this period
Conclusion
As this is a technical note, we could say as conclusion, that with the development of the hip arthroscopy a great number of soft tissue pathologies, that were treated as one in the past, have appear and each one has its own clinical presentation and imagine pattern. And with the arthroscopy of the hip we can treat each one of these different soft tissue pathologies with great success, low complication rate and very efficient way. The hip arthroscopy it is the way to treat them instead of open classic way.
References
- Brinks A, van Rijn RM, Willemsen SP, Bohnen AM, Verhaar JA, Koes BW, et al. Corticosteroid injections for greater trochanteric pain syndrome: a randomized controlled trial in primary care. Ann Fam Med. 2011; 9: 226-234.
- Shbeeb MI, O’Duffy JD, Michet CJ Jr, O’Fallon WM, Matteson EL. Evaluation of glucocorticosteroid injection for the treatment of trochanteric bursitis. J Rheumatol. 1996; 23: 2104-2106.
- Ilizaliturri VM Jr, Villalobos FE Jr, Chaidez PA, Valero FS, Aguilera JM. Internal snapping hip syndrome: treatment by endoscopic release of the iliopsoas tendon. Arthroscopy. 2005; 21: 1375-1380.
- Smart LR, Oetgen M, Noonan B, Medvecky M. Beginning hip arthroscopy: indications, positioning, portals, basic techniques, and complications. Arthroscopy. 2007; 23: 1348-1353.
- Verhelst L, Guevara V, De Schepper J, Van Melkebeek J, Pattyn C, Audenaert EA. Extra-articular hip endoscopy: A review of the literature. Bone Joint Res. 2012; 1: 324-332.
- Ilizaliturri VM Jr, Martinez-Escalante FA, Chaidez PA, Camacho-Galindo J. Endoscopic iliotibial band release for external snapping hip syndrome. Arthroscopy. 2006; 22: 505-510.
- Strauss EJ, Nho SJ, Kelly BT. Greater trochanteric pain syndrome. Sports Med Arthrosc. 2010; 18: 113-119.
- Gollwitzer H, Opitz G, Gerdesmeyer L, Hauschild M. [Greater trochanteric pain syndrome]. Orthopade. 2014; 43: 105-116.
- Domínguez A, Seijas R, Ares O, Sallent A, Cuscó X, Cugat R. Clinical outcomes of trochanteric syndrome endoscopically treated. Arch Orthop Trauma Surg. 2015; 135: 89-94.