
Case Report
Austin J Orthopade & Rheumatol. 2016; 3(2): 1034.
Penetrating Metalic Rod in the Nose: A Case Report
Byaruhanga R¹*, NAkasagga E², Nakku D² and Nyaiteera V²
¹Department of ENT, School of Medicine, College of Health Sciences, Makerere University, Uganda
²Department of ENT, Mbarara University of Science and Technology, Uganda
*Corresponding author: Richard Byaruhanga, Department of ENT, School of Medicine, College of Health Sciences, Makerere University, Uganda
Received: July 26, 2016; Accepted: August 03, 2016; Published: August 05, 2016
Abstract
Background: Nasal foreign bodies are commonly encountered in emergency departments. Although more frequently seen in children, they can also sometimes be found in adults, especially those with mental retardation or psychiatric illness. Foreign bodies can be classified as either inorganic or organic.
Case Summary: We present an interesting case report of a 3 year old female from Western Uganda who was admitted on 3rd September 2014 with a metallic rod in the right nostril which was accidentally inserted by the younger sibling while she was sleeping 12hrs prior to admission. She had had two failed attempts at removal without anaesthesia from private clinics. On arrival, we noted a fully awake child who was irritable and in pain with a rusted metallic rod hanging from the right nasal cavity, mild right sided infraorbital swelling and blood stained epiphora.
A facial reconstruction CT scan was done which confirmed a metallic rod extending from the nasal cavity at the level of the middle meatus bent 90 degrees traversing the ethmoid sinuses and penetrating the right lamina papyrecia into the floor of the orbit. An Ophthalmologist was consulted and an approach for removal was discussed and agreed upon. The foreign body was then removed under general anaesthesia. Postoperatively, the child was put on steroid nasal drops, antihistamine, antibiotics and analgesics. She was also given a tetanus toxoid to prevent tetanus infection. On 2nd postoperative day, the child was reevaluated and on finding no complication to either her nose or right eye was discharged on treatment.
Conclusion: We recommend that an ENT Specialist should be consulted when there is failure to remove an FB in the nose at the first attempt. Secondly, if the patient is a child and he/she is uncooperative, the patient should be sedated before an attempt is made to remove the FB.
Keywords: Case report; Child; Nasal foreign body; CT scan
Introduction
Nasal foreign bodies are commonly encountered in emergency departments. Although more frequently seen in children, they can also sometimes be found in adults, especially those with mental retardation or psychiatric illness. Children”s interests in exploring their bodies make them more prone to lodging foreign bodies in their nasal cavities. Nasal foreign bodies harbour the potential for morbidity due to mucosal damage, or when they penetrate into other surrounding tissues and even mortality, if the object is dislodged into the airway.
Foreign bodies can be classified as either inorganic or organic. Inorganic materials are typically plastic or metal. Common examples include beads, small stones and parts of ear rings. These materials are often asymptomatic and may be discovered incidentally. Organic foreign bodies, including food, rubber, wood, and sponge, tend to be more irritating to the nasal mucosa and thus may produce earlier symptoms. Peas, beans, and nuts are among the more common organic nasal foreign bodies [1]. Organic foreign bodies tend to swell and are usually more symptomatic than are inorganic foreign bodies.
We have written up this case report, to show that it is possible to remove nasal foreign bodies, even when they are complicated, with simple medical equipment in resource limited settings. We also emphasise the need for a referral medical system in order to handle difficult or complicated medical cases.
Case Presentation
We present an interesting case report of a 3 year old female from Western Uganda who was admitted on 3rd September 2014 with a metallic rod in the right nasal cavity which was accidentally inserted by the younger sibling while she was sleeping 12hrs prior to admission. She was complaining of nasal pain and epistaxis with right eye pain especially on manipulation of the rod.
She had had two attempts at removal without anaesthesia from private clinics with no success which prompted the mother to bring the child to Mbarara Regional Referral Hospital (this hospital is located in Western Uganda).
On arrival, we noted a fully awake child of preschool going age, irritable and in pain with a rusted metallic rod hanging from the right nostril, mild right sided infraorbital swelling and blood stained Epiphora (Figure 1).
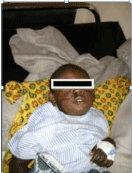
Figure 1: Child with metalic FB in situ.
The rod was seen to be curved on the lateral wall of the nose at the level of the middle turbinate and the pointed end was palpable around the midpoint of the lower eyelid however child had symmetrical extraocular eye movement with normal vision. Noted some ulceration and excoriation around the right nostril with mucoid nasal discharge that was blood stained.
Diagnosis of penetrating right nasal trauma with right orbital extension from a metallic rod was made.
A facial reconstruction CT scan was done on request by the medical team; this confirmed a metallic rod extending from the nasal cavity at the level of the middle meatus bent 90 degrees traversing the ethmoid sinuses and penetrating the right lamina papyrecia into the floor of the orbit (Figures 2-4).
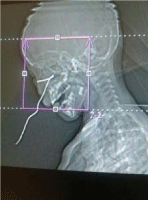
Figure 2: Reconstructed PNS CT scan.
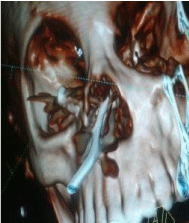
Figure 3: Reconstructed PNS CT scan.
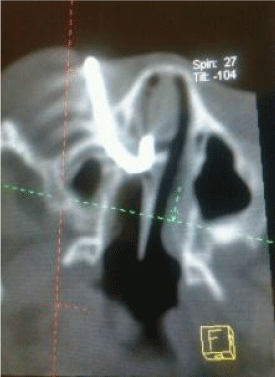
Figure 4: Reconstructed PNS CT scan.
An Ophthalmologist was consulted and an approach for removal was discussed and agreed upon by both teams. (ophthalmology and ENT).
We obtained assent from the mother and under general anaesthesia with endotracheal intubation, the metallic rod was removed by manipulation (traction force) using a mosquito forceps and a bayonet forceps in an infero-medial direction, away from the orbit and care was taken not to traumatise the nasal septum, (Figure 5).

Figure 5: Instruments used and the metalic FB.
Anterior rhinoscopy under anaesthesia was immediately carried out, found mild bleeding from the right nasal cavity from a lateral nasal wall laceration around the middle meatus with oedematous mucosa over the inferior turbinate, mid-septal mucosal bruise was also noted.
The eye was intact except for hyperaemia around the lower eyelid and, mild conjuctival haemorrhage. Haemostasis was achieved with a few pledgets of gel-foam.
Child was put on steroid nasal drops, antihistamine, antibiotics and analgesics. She was also given a tetanus toxoid to prevent tetanus infection.
On the 2nd postoperative day, the child was re-evaluated by both the Opthalmology and ENT teams (using a flexible fibreoptic nasopharyngoscope) and on finding no complication to either her nose or right eye was discharged on oral antibiotics and analgesics, saline nasal drops and steam inhalations. The mother was asked to bring back the child for review after one week, but they were lost to follow-up.
Discussion
Whereas a study by Svider et al. [2] indicated that jewelry beads are the most common nasal FBs prompting emergency department visits in the United States, with paper products and toys being the next most common objects, in our setting, bean seeds closely followed by maize seeds are the most common nasal FBs (Unpublished data from ENT dept, Mulago National Referral hospital).Our patient had an FB of a metallic rod, which even in our practice is a rare occurrence.
Some studies have demonstrated a greater prevalence of nasal foreign bodies in males than in females (ie, 58% males [3] ) however, this trend has not been universal and our patient was a female. Among children, those aged 2-5 years have the highest incidence of nasal foreign bodies, which could possibly be so in theory because children develop their pincer grip at about age 9 months.
In terms of complications, bleeding is the most common complication reported in patients with nasal foreign bodies, although it is characteristically minimal and resolves with simple pressure.
The foreign body itself may cause irritation to the patient; however, morbidity is primarily caused by the resulting inflammation, mucosal damage, and extension into adjacent structures. Our patient had epistaxis and was complaining of pain, especially on trying to manipulate the FB. The epistaxis was due to the injury caused by the penetration of the FB into the lateral nasal wall and into the orbit, however the bleeding could have been exacerbated by the attempts made by the medical workers in the peripheral clinics before sending the child to the referral hospital. Sometimes these attempts made by unqualified colleagues worsen the problem and can lead to worse complications. Reported complications include the following:
• Sinusitis
• Acute otitis media
• Nasal septal perforation
• Periorbital cellulitis
• Meningitis
• Acute epiglottitis
• Diphtheria
• Tetanus
A delay in the diagnosis of complications of these FBs, such as sinusitis and acute otitis media, can result in prolonged morbidity. This can be avoided by performing a thorough examination and by reexamining the nasal cavity after removal of the FBs. In the case of our patient, there was a short time of delay (12hours) between insertion of the foreign body and coming to the referral hospital for specialized care. We believe that in this short time, inspite of the metallic rod being rusted and having had two failed attempts at removing it, she had not yet got an infection. Nevertheless, she was put on antibiotic treatment and given tetanus toxoid as prophylaxis.
In most cases, the insertion of the nasal foreign body is witnessed, as was in our case and the dilemma of diagnosis is eliminated. In one study, presentations over 48 hours after the time of insertion accounted for 14% of all cases [4]. Among the delayed presentations, the most common clinical scenario is unilateral nasal discharge. Nevertheless, clinicians must entertain the diagnosis of nasal foreign body in all patients with nasal irritation, epistaxis, sneezing, snoring, sinusitis, stridor, wheezing, or fever.
The physical examination is the main diagnostic tool, and a cooperative patient is essential for success. Parents and staff may be needed to comfort and immobilize a child to allow for a thorough otorhinolaryngologic examination. Sedation is often helpful in the pediatric population. Maximal visualization of the nasal cavity is obtained by wearing a headlamp. A nasal speculum may also help to view the nasal cavity, although some authors report less patient anxiety and equally good visualization by using one”s thumb to pull the nose upward. In our case it was easy to visualise the FB, since it was clearly protruding from the nasal cavity, although any trial at manipulating the metallic object would elicit tenderness and then the child would become afraid and uncooperative.
The object can be found in any area of the nasal cavity, though objects are most predictably below the inferior turbinate or immediately anterior to the middle turbinate [5] occasionally, evidence of local trauma may exist, with erythema, edema, bleeding, or a combination thereof, as was in the case we have presented.
The extent of the workup depends on the clinical scenario. For most isolated nasal foreign bodies, no diagnostic testing is indicated. With the exception of metallic or calcified objects, most nasal foreign bodies are radiolucent. In our case we needed to carry out the CT scan to be able to tell the extent of the penetration and damage of the surrounding tissues by the FB. Indeed we found out that it had penetrated through the lateral nasal wall and lamina papyracea into the right eye. The patient had normal eye movements though which meant that her extraocular muscles had not been damaged.
Nasal foreign body removal may be attempted by an experienced medical worker if the object is near and can easily be extracted but if doubt exists about the reasonable probability of extraction, an otolaryngologist should be consulted. Repeated attempts at removal may result in increased trauma and potential movement of the item into a less favorable location, as could have happened with our patient where attempts were made by a medical officer to remove it and failed. Removal should not be performed without adequate sedation in an uncooperative patient whose head cannot be secured and safely stabilized. In our case, the child was put under general anaesthesia with endotracheal intubation to ensure that the surgeons had adequate time to remove the FB with the child”s head completely stabilized. One study reported a very high success rate (95%) and a low complication rate with the use of procedural sedation, even among patients who had undergone prior, unsuccessful removal attempts [6].
Many authors have suggested using various techniques to remove FBs in the nose , some of which include using hooked probes, the “hook-scope” technique (using a flexible endoscope to visualize the FB and the using it as a hook to pull out the object), using snares, balloon catherisation, just to mention but a few [5,7-11,12]. In our case, the most feasible way to remove this FB was by using a bayonet forceps and a mosquito forceps.
Conclusion
We recommend that an otolaryngologic specialist should be promptly consulted for cases of failed removal or if a nasal foreign body is complicated by significant damage to adjacent structures. Secondly, even in the proper setting, if the patient with the foreign body is uncooperative, adequate sedation should be used before the attempt to remove the foreign body is done.
Authors” Contributions
RB did literature review and wrote the manuscript. EN, DN and VN did the initial work-up and the operation and contributed to the literature review.
Consent
Written informed consent was obtained from the patient for publication of this Case report and any accompanying images.
References
- Kiger JR, Brenkert TE, Losek JD. Nasal foreign body removal in children. Pediatr Emerg Care. 2008; 24: 785-792.
- Svider PF, Sheyn A, Folbe E, Sekhsaria V, Zuliani G, Eloy JA, et al. How did that get there? A population-based analysis of nasal foreign bodies. Int Forum Allergy Rhinol. 2014; 4: 944-999.
- Srinivas Moorthy PN, Srivalli M, Rau GV, Prasanth C. Study on clinical presentation of ear and nose foreign bodies. Indian J Otolaryngol Head Neck Surg. 2012; 64: 31-35.
- Hong D, Chu YF, Tong KM, Hsiao CJ. Button batteries as foreign bodies in the nasal cavities. Int J Pediatr Otorhinolaryngol. 1987; 14: 15-19.
- DeWeese DD, Saunders AH. Acute and chronic diseases of the nose. Textbook of Otolaryngology. St. Louis: Mosby. 1982.
- Tong MC, Ying SY, van Hasselt CA. Nasal foreign bodies in children. Int J Pediatr Otorhinolaryngol. 1996; 35: 207-211.
- Kadish HA, Corneli HM. Removal of nasal foreign bodies in the pediatric population. Am J Emerg Med. 1997; 15: 54-56.
- Fundakowski CE, Moon S, Torres L. The snare technique: a novel atraumatic method for the removal of difficult nasal foreign bodies. J Emerg Med. 2013; 44: 104-106.
- Brown L, Denmark TK, Wittlake WA, Vargas EJ, Watson T, Crabb JW. Procedural sedation use in the ED: management of pediatric ear and nose foreign bodies. Am J Emerg Med. 2004; 22: 310-314.
- McMaster WC. Removal of foreign body from the nose. JAMA. 1970; 213: 1905.
- Giourgos G, Matti E, Pagella F. Endoscopic removal of a nasal foreign body with the “hook-scope” technique. Eur Arch Otorhinolaryngol. 2009; 266: 1663-1665.
- Botma M, Bader R, Kubba H. A parent”s kiss”: evaluating an unusual method for removing nasal foreign bodies in children. J Laryngol Otol. 2000; 114: 598-600.