
Research Article
Austin J Orthopade & Rheumatol. 2016; 3(4): 1041.
Correlation between TGF-Beta1 and IGF-1 Plasma Values and Functional Clinical Scales in Knee Osteoarthritis after an Infiltration with Platelet-Rich Plasma
Villarreal-Villarreal GA¹, Vilchez-Cavazos JF¹, Lara-Arias J¹, Pea-Martinez VM¹, Cardenas- Estrada E² and Acosta-Olivo CA¹*
¹Department or Orthopaedics and Traumatology, Universidad Autonoma de Nuevo Leon, Mexico
²Centro de Investigacion y Desarrollo en Ciencias de la Salud, Universidad Autonoma de Nuevo Leon, Mexico
*Corresponding author: Acosta-Olivo CA, Department or Orthopaedics and Traumatology, Universidad Autonoma de Nuevo Leon, Mexico
Received: September 08, 2016; Accepted: October 10, 2016; Published: October 14, 2016
Abstract
Introduction: Platelet-Rich Plasma (PRP) is an autologous volume of plasma with a higher number of platelets than the basal level and has served as a treatment for Osteoarthrosis (OA). These platelets have growth factors with multiple functions, such as Transforming Growth Factor (TGF)-beta1 and Insulin-like Growth Factor (IGF)-1, that are related to articular cartilage repair. Objective: To treat patients with knee OA grade I and II with PRP infiltration, generating a correlation between scales (the Visual Analogue Scale [VAS], the Western Ontario and McMaster Universities Arthritis Index [WOMAC] and the Knee Society Score [KSS]) and TGF-β1 and IGF-1 values in the plasma. Materials and methods: A total of 29 patients with OA (grade II) were treated with 1 infiltration of 5 ml of PRP. Growth factors (TGF-beta1, IGF-1) were analyzed with 1 ml of PRP using Western Blot. A follow-up was conducted at 6 months with an exit survey of 8 questions. Results: Clinical improvement was observed in the VAS the following month, obtaining a >60% reduction in pain (P=<0.010). An improvement of >50% (P=<0.00) was obtained in the WOMAC. Constant and statistically significant correlations were detected between pain and IGF-1 at 14, 21 and 30 days of follow-up (P=<0.027, 0.037 and 0.034, respectively). Conclusion: PRP treatment in OA patients results in clinical and functional improvement in the short-term. We found a positive correlation between values of TGF-beta1 and IGF-1 and the initial clinical scale evaluations.
Keywords: Knee OA; Platelet-rich plasma; TGF-beta1; IGF-1
Introduction
Osteoarthrosis (OA) is a disease characterized by changes in the articular cartilage, the subchondral bone, the intra-articular space, ligaments and the articular capsule. Clinically, patients present with pain, limited mobility, and a reduction in quality of life; in fact, OA is considered to be the most common cause of disability and pain worldwide [1]. The pathophysiology of OA consists of an imbalance between the anabolic and catabolic reactions of articular cartilage homeostasis [2]. Classified as a chronic degenerative disease, OA provides a large window of time in which to modify the natural course of the disease. In the early stages of this disease, non-surgical treatment is based on reducing symptoms to help preserve the patient’s basic life activities. These treatment options include acetaminophen, Nonsteroidal Anti-Inflammatory Drugs (NSAIDs), hyaluronates, glycosaminoglycans, and topical and/or intra-articular steroids. These options have presented good short-term results but do not change the natural course of the disease [3]. Acetaminophen is the drug of choice for pain management due to its safety at recommended doses [4]. It has been used for pain relief in OA for about a century; however its efficacy has been recently challenged in a systematic review [5].
Newer therapies are based on improving symptomology in an attempt to slow articular degeneration. Clinical studies have demonstrated the benefits to the use of Platelet-Rich Plasma (PRP) in muscle, tendon and osteochondral lesion repair, bone formation and anti-inflammatory activity [6-10]. PRP treatment is a nonsurgical alternative used for the treatment of OA, which consists of an autologous volume of plasma with higher platelet levels than the patient’s basal level [11]. It functions due to the activation and release of growth factors contained in the alpha granules of the platelets [12]. Studies have shown that PRP can be used for cartilage regeneration as it contain therapeutic concentrations of several growth factors that have been used for cartilage induction of mesenchymal cells; the growth factors associated with articular cartilage growth and repair, are Insulin-like Growth Factor 1 (IGF-1), Transforming Growth Factor beta 1 (TFG-β1) and Fibroblast Growth Factor (b-FGF) [13]. The aim of this study is to treat patients diagnosed with mild OA of the knee with an injection of PRP to provide a correlation between clinical knee scales (the Western Ontario and McMaster Universities Arthritis Index [WOMAC] and the Knee Society Score [KSS]) and the Visual Analog Scale as well as IGF-1 and TFG-β1 plasma values.
Materials and Methods
Patients and study design
The study was approved by the ethics committee of our institution, number of approval OR11-006. All patients read and signed the informed consent. This prospective study included 29 patients with a diagnosis of knee OA (grade I and grade II) acording to Kellegren and Lawrence (14), who received a single dose of intra-articular PRP and completed follow-up at 6 months. The inclusion criteria were the following: diagnosis of mild knee OA, any gender, age greater than 40 years, and not having had any treatment for OA in the last 30 days. The exclusion criteria were the following: pregnancy, obesity grade II, III, IV or morbidity, angular deformity >15º in the varus/valgus, instability, previous history of septic arthritis, autoimmune disease, vascular disease, blood dyscrasia and history of intra-articular infiltration in the last 3 months in the knee that was being treated (Table 1).
Patients
29
Age
53.83± 5.63
Gender
Male: 5 Female: 24
BMI
32.05± 4.16
Kellgren-Lawrence
Grade 1
6
Grade 2
23
BMI: Body Mass Index; M: Male; F: Female
Table 1: Demographic table.
Preparation and application of PRP
A total of 40 ml of venous blood was obtained from the forearm (cubital or basilic) in 8 Vacutainer tubes with 3.8% sodium citrate as an anticoagulant (BD Vacutainer; Bectron, Dickinson and Company, NJ). These samples were gently shaken to assure that the blood and the anti-coagulant were mixed. The samples were centrifuged (Heraeus Megafuge 1.0R, Thermo Electron Corporation) for 15 minutes at 2100 G-force, which separated the sample into three 3 layers (erythrocytes, white and yellow). The white layer (rich in platelets) was then extracted in a sterile environment under a laminar flow hood (SterilGuard III, The Baker Company) and with an automatic pipette (Corning, NY) and was deposited into 15-ml Falcon tubes. A 6-ml final sample was obtained for each patient. From this sample 5 ml was injected in the symptomatic knee and the remaining 1 ml was used for growth factors (IGF-1, TFG- β1) quantification using the Western blot technique. These steps were all performed following the Anitua et al. laboratory method [12].
With the patient in the supine position and the knee flexed at 25º, aseptic procedures were performed (3M™ AvagardTM), and 1 ml of local anesthetic was applied to the skin with 2% lidocaine hydrochloride (2% 200 mg/10 ml Piscaine). We used calcium chloride as the PRP activator at doses of 0.05 μl for each ml of PRP injected. PRP injected was performed on the superolateral face of the knee using a 22 G syringe. When the application was completed, passive flexion and knee extension movements were performed for 10 seconds.
Evaluation of knee scales and knee function
The clinical scores used for the pain was the Visual Analogue Scale (VAS) and was evaluated using values of 0-10 (with 10 being the worst pain felt by the patient) [15]. The clinical knee scores used were the WOMAC, which evaluated pain, stiffness and functional state, giving points from 0-96 (with 96 points being the worst score), and the KSS with its two rubrics: knee/anatomical, which evaluates pain, flexion contractures, lack of extension, ranges of mobility, alignment and stability; and functional state, which evaluates abilities such as walking, climbing and going down stairs, and moving around with and without assistance. Points on this scale were assigned from 0 (poor) to 100 (excellent) [16].
Follow-up and patient management
After the procedure and the initial measurement of the evaluation scales, each patient received 500 mg acetaminophen orally every 8 hours for 1 month. On days 7, 14, and 21, patients received a telephone call from an independent study evaluator for the weekly VAS evaluation. After 1 month of PRP infiltration, the VAS, WOMAC and KSS scales were newly applied. The final evaluation was applied after 6 months and consisted of an exit survey of 8 questions (Table 2).
1
When was the knee inyected?
2
How many weeks did you last without pain? (pain 0)
3
What are you actual complaints or symptoms?
4
The knee pain is; lesser, greater or the same as before the treatment?
5
When did you started to take pain pills for the knee pain?
6
What pain pills? And the doses?
7
Did you follow our reccomendations of losing weight and excercising?
8
Would you like to receive the treatment again?
Table 2: Exit survey.
Analysis of growth factors
The growth factors IGF-1 and TFG- β1 were detected by Western blot using 30 μL of inactivated PRP. Proteins were separated using electrophoresis in a polyacrylamide gel. The transfer was verified with a red Ponceau-S stain. Membrane blocking was performed for 1 hour at room temperature in 5% non-fat milk in Tris-Buffered Saline with Tween (TBST). The primary dilution of antibodies was 1:3000 in TBST, and antibody solutions were incubated for 1 hour at room temperature (Anti-IGF1 ab39398, Anti-TGF beta 1 ab9758, ABCAM, Cambridge, MA, USA). The secondary dilution of antibodies was 1:5000 in TBST (ab191866, ABCAM, Cambridge, MA, USA). The membrane was photographed by chemo luminescence using a ChemiDocXRS+ (BIO-RAD Laboratories Inc. USA), and Western blots were read using a Luminol Reagent kit (sc-2048, Santa Cruz Biotechnology Inc. USA). The normalization and quantification of the bands were performed using the Phoretix 1D 10.0 program (Cleaver Scientific Ltd, UK) (Figure 1).
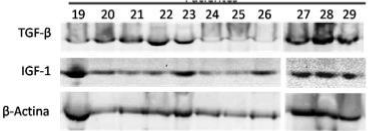
Figure 1: Western blot for TG23e76F-β, IGF-1 and β-actine in platelet rich
plasma.
Statistical analysis
All data were analyzed with the STATA-13 program (License 1910531247) by a statistics expert. The results were expressed in means and standard deviations. The equality and distribution of normal variables were verified using the Kolmogorov-Smirnov test. Parametric tests were performed using Student’s t test. A P-value of P=<0.05 was considered statistically significant.
Results
Knee pain was measured using the VAS, whose initial value was 3.41 (± 1.053); at 30 days, the value was 1.17 (± 0.92). This difference translated into a 65% (3.41- 1.17) improvement with regard to pain with a value of P=<0.010. The VAS was measured weekly, demonstrating a progressive clinical and statistically significant improvement (Table 3), which can be interpreted as a 30% improvement in the first seven days (the greatest time of improvement), a 45% improvement at day fourteen and a 56% improvement at day twenty-one post-procedure.
On the functional knee scales, the WOMAC was 34.83 points (± 19.02) initially and then 17.50 points (±12.96) at 30 days, demonstrating a 17.33 points improvement. This difference can be translated into a 50% clinical improvement in pain, stiffness and functionality (P=<0.00). The KSS was divided into its 2 Knee/ anatomical (K) and Functional (F) scales, with the initial results being 57.45 points (± 14.92) (K) and 70.17 points (± 19.93) (F). The final results were 60.86 points (± 17.68) (K) and 72.24 points (± 19.71) (F). These results did not show statistically significant differences (Table 3).
Initial
Day 0
Day 7
Day 14
Day 21
Final
Day 30
P Value
VAS
3.41± 1.05
2.41±1.05
1.90± 1.11
1.52± 1.18
1.17± 0.92
D. 7< 0.023
D. 14<0.003
D. 21<0.008
D. 30<0.010
WOMAC
34.83 ± 19.02
NA
NA
NA
17.50 ±12.96
0.00
KSS
K 57.45 ± 14.92
F 70.17 ± 19.93
NA
NA
NA
K 60.86 ± 17.68
F 72.24 ± 19.71
0.094
0.071
VAS: Visual Analog Scale; WOMAC: Western Ontario and McMaster Universities Arthritis Index; KSS: Knee Society Score; K: Knee; F: Functional; D: Day; NA: Not Applied
Table 3: Results of clinical and knee socres 3.
The objective of the exit survey was to evaluate pain at 6 months after the procedure. During follow-up, 29 patients (100%) were without pain for more than 3 months. No administration of complementary medication was necessary (apart from 500 mg acetaminophen during the first month) for pain management during the 15.89 weeks. Patients were asked whether they would like to receive treatment again, and 29 patients responded affirmatively.
In the growth factor analysis, when performing the correlation between basal plasma values (TGF-β1 0.97 ± 0.46 ng/mL and 1.05 ± 0.35 ng/mL of IGF-1) and the clinical scales utilized, positive correlations were detected between IGF-1 values and the VAS at 14, 21 and 30 days (P=<0.027, 0.037 and 0.034, respectively), in addition to TGF-β1 and the VAS at 7 days (P=<0.023). Another statistically significant positive correlation was detected between TGF- β1 /IGF-1 and the initial KSS (Table 4).
Initial
Day 0
P Value
Day 7
P Value
Day 14
P Value
Day 21
P Value
Final
Day 30
P Value
VAS/ TGF- β1
0.178
.023
0.262
0.266
0.138
VAS/ IGF-1
0.236
0.204
0.027
0.037
0.034
WOMAC/ TGF- β1
0.200
NA
NA
NA
0.155
WOMAC/ IGF-1
0.251
NA
NA
NA
0.266
KSS/ TGF- β1
K .013
F -.067
NA
NA
NA
K .221
F 0.139
KSS/ IGF-1
K -.161
F .048
NA
NA
NA
K 0.157
F 0.282
VAS: Visual Analog Scale; WOMAC: Western Ontario and McMaster Universities Arthritis Index; KSS: Knee Society Score; K: Knee; F: Functional; NA: Not Applied (p<0.05).
Table 4: Results of P value between clinical scales and growth factor analysis.
No severe complications were presented during the study. Only mild inflammation at the site of infiltration was reported in three patients, without intra-articular inflammation data, which were resolved in less than 48 hours without any additional treatment.
Discussion
The treatment with PRP has become a non-surgical option for the treatment of knee OA, with good results [17]. This technique offers several advantages, including a simple preparation, low cost and autologous therapy. Both non-commercial PRP preparation methods, known as “in office”, such as that of [12] and Spakova et al. [18] along with commercial kits (GPS, HARVEST, SYMPHONY, Vivostat PRF Preparation Kit®, PCCS Platelet Concentrate Collection System®, Harvest® SmartPReP 2APC 60 Process, and the Fibrinet® Autologous Fibrin & Platelet System) are currently available [19]. Any of these methods can be activated with different activating substances, such as calcium chloride, thrombin and calcium gluconate. In a clinical study by Filardo et al. [20], in which 144 patients with a diagnosis of OA were evaluated, the “in office” method was compared in two groups of 72 patients. Utilizing a simple versus a double centrifugation, no difference in pain was detected. However, the double centrifugation patients presented with more knee inflammation, which could be due to the high concentration of leukocytes present in the double centrifugation preparation [21]. In our study, we used simple centrifugation, activating the platelets with calcium chloride. We decided to use calcium chloride because it offers advantages such as autoimmunity (compared to the effects of thrombin), prolonged release of growth factors for up to 7 days and the promotion of the differentiation of growth factors such as IGF-1 [22,23].
One of the benefits of PRP treatment in regard to OA is the clinical and functional improvement of the patient, with good shortterm results [6,17]. Our study showed good short-term results, with pain reduced by more than 60%, and with a functional improvement of 50% on the WOMAC scale (P=<0.00). These results are similar to those obtained by Cerza et al. which compared the use of PRP versus hyaluronic acid in 120 patients with a diagnosis of OA. They obtained an initial WOMAC of 79 points, decreasing to 49.6 the following month, which translated into a clinical improvement of >50% [24]. We selected only patients with mild OA (Grades I and II), as this population could most benefit from PRP [25]. The highest percentage of improvement with regard to pain was in the first week, with 30%, which could be due to the average lifespan of platelets of 5-9 days [26].
The PRP contains large quantities of growth factors and plays important roles in chemotaxis, differentiation, proliferation, and cartilage cell synthesis, thus regulating the cartilage remodeling process [2,27,28]. For this reason, PRP has become a treatment option for OA-related knee pain. We were able to detect IGF-1 and TGF-β1 plasma levels that induce cellular proliferation and intraand extracellular matrix production, in addition to catabolic activity against proinflammatory interleukins [29]. One report demonstrated in vitro chondrogenic activity with TGF-β1 levels of 0.3±20.0 ng/ ml [30]. In our study, the levels obtained were 0.97± 0.46 ng/ml of TGF-β1 and 1.05± 0.35 ng/ml of IGF-1.Kenneth et al. evaluated condrogenic activity using TGF-β1 and IGF-1 in vitro. Two different study groups were evaluated; first group 28 days (transient) of continuos exposure of growth factors and second group to 42 days (prolonged), concluding that at day 14 a “switch off” is achieved and no chondrogenic increases after [31]. This leads us to the hypothesis that our patients are exposed to growth factors to 9 days, due to the lifespan of platelets, which is a good time lapse for chondrogenic activity.
Schal et al. [32] evaluated the perception of knee pain in patients with cartilaginous lesions and demonstrated a statistically significant correlation between intra- articular IGF-1 levels and pain perception. We found that pain perception was reduced in our patients, with statistically significant improvements (P=<0.027, 0.037 and 0.034) between the VAS and IGF-1 levels. However, we do not know the true significance of this result. In a study to analyze the effect of PRP rich in leukocyte in the local or systemic presence of cytokines pro and anti-inflammatory in patients with knee OA, were studied 36 patients, was collected 1 mL of synovial fluid prior to infiltration, also took samples of peripheral blood and plasma at the beginning, two, six and 12 months to analyze the presence of IL-1beta, IL-6, IL-8, Il-17, IL-4, IL-10 and IL-13 and growth factors as FGF-b, HGF and PDGF-AB/BB. They found no differences between these cytokines in the baselines and post-treatment analysis, besides they only found an increase in the presence of PDGF-AB/BB in the PRP sample [33].
In a review to compare the clinical evolution and rates of adverse reactions between the use of rich and poor-leukocyte PRP, they found that the use of poor-leukocyte PRP improves the functional scales compared with hyaluronic acid and placebo in knee OA, also they did not find that both PRP had an increase in adverse reactions, and they mentioned that these reactions are not directly related to the concentration of leukocytes [34]. We only found adverse mild reactions in three patients, with no intervention into the symptoms.
Conclusion
The treatment with PRP is a non-surgical treatment option for OA with good short-term results in clinical and functional knee scales. The “in office” preparation methods provide good results, are easy to prepare and decrease the cost of a commercial kit. The impact of growth factors is a controversial topic and continues to be such in this study. The true significance of our results is uncertain. However, we believe that a relationship between IGF-1 and OA-related knee pain does exist.
Conflict of Interest
Carlos Acosta-Olivo declares that he has no conflict of interest.
Gregorio Villarreal-Villarreal declares that he has no conflict of interest. Felix Vilchez-Cavazos declares that he has no conflict of interest; Jorge Lara-Arias declares that he has no conflict of interest; Victor Pea-Martinez declares that he has no conflict of interest; Eloy Cardenas-Estrada declares that he has no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
References
- Woolf AD, Pfleger B. Burden of major musculoskeletal conditions. Bull World Health Organ. 2013; 81: 646-656.
- Spakova T, Rosocha J, Lacko M, Harvanova D, Gharaibeh A. Treatment of Knee Joint Osteoarthritis with Autologous Platelet-Rich Plasma in Comparison with Hyaluronic Acid. Am J Phys Med Rehabil. 2012; 91: 411-417.
- Nelson AE, Allen KD, Golightly YM, Goode AP, Jordan JM. A systematic review of recommendations and guidelines for the management of osteoarthritis: The Chronic Osteoarthritis Management Initiative of the U.S. Bone and Joint Initiative. Semin Arthritis Rheum. 2014; 43: 701-712.
- Jawad AS. Analgesics and osteoarthritis: are treatment guidelines reflected in clinical practice?. Am J Ther. 2005; 12: 98-103.
- Ennis ZV, Dideriksen D, Vaegter HB, Handberg G, Pottegard A. Acetaminophen for Chronic Pain: A Systematic Review on Efficacy. Basic Clin Pharmacol Toxicol. 2016; 118: 184-189.
- Griffin XL, Smith CM, Costa ML. The clinical use of platelet-rich plasma in the promotion of bone healing: A systematic review. Injury-International Journal of the Care of the Injured. 2009; 40: 158-162.
- Anitua E, Andia I, Sanchez M, Azofra J, del Mar Zalduendo M, de la Fuente M, et al. Autologous preparations rich in growth factors promote proliferation and induce VEGF and HGF production by human tendon cells in culture. J Orthop Res. 2005; 23: 281-286.
- McCarrel T, Fortier L. Temporal Growth Factor Release from Platelet-Rich Plasma, Trehalose Lyophilized Platelets, and Bone Marrow Aspirate and Their Effect on Tendon and Ligament Gene Expression. J Orthop Res. 2009; 27: 1033-1042.
- Menetrey J, Kasemkijwattana C, Day CS, Bosch P, Vogt M, Fu FH, et al. Growth factors improve muscle healing in vivo. J Bone Joint Surg Br. 2000; 82: 131-137.
- Bendinelli P, Matteucci E, Dogliotti G, Corsi MM, Banfi G, Maroni P, et al. Molecular basis of anti-inflammatory action of platelet-rich plasma on human chondrocytes: mechanisms of NF-?B inhibition via HGF. J Cell Physiol. 2010; 225: 757-766.
- Raeissadat SA, Rayegani SM, Babaee M, Ghorbani E. The effect of platelet-rich plasma on pain, function, and quality of life of patients with knee osteoarthritis. Pain Res Treat. 2013: 165967.
- Anitua E. Plasma rich in growth factors: preliminary results of use in the preparation of future sites for implant. Int J Oral Maxillofac Implants. 1999; 14: 529-535.
- Dragoo JL, Korotkova T, Wasterlain AS, Pouliot MA, Kim HJ, Golish SR. Age-Related Changes of Chondrogenic Growth Factors in Platelet-Rich Plasma. Oper Tech Orthop. 2012; 22: 49-55.
- Kijowski R, Blankenbaker D, Stanton P, Fine J, De Smet A. Arthroscopic validation of radiographic grading scales of osteoarthritis of the tibiofemoral joint. AJR Am J Roentgenol. 2006; 187: 794-799.
- Wu W, Zhang J, Dong Q, Liu Y, Mao T, Chen F. Platelet-rich plasma - A promising cell carrier for micro-invasive articular cartilage repair. Med Hypotheses. 2009; 72: 455-457.
- Bellamy N, Buchanan WW, Goldsmith CH, Campbell J, Stitt LW. Validation study of WOMAC: A health status instrument for measuring clinically important patient relevant outcomes to antirheumatic drug therapy in patients with OA of the hip and knee. J Rheumatol. 1988; 15: 1833-1840.
- Meheux CJ, McCulloch PC, Lintner DM, Varner KE, Harris JD. Efficacy of Intra-articular Platelet-Rich Plasma Injections in Knee Osteoarthritis: A Systematic Review. Arthroscopy. 2016; 32: 495-505.
- Spaková T, Rosocha J, Lacko M, Harvanová D, Gharaibeh A. Treatment of knee joint osteoarthritis with autologous platelet-rich plasma in comparison with hyaluronic acid. Am J Phys Med Rehabil. 2012; 91: 411-417.
- Leitner GC, Gruber R, Neumüller J, Wagner A, Kloimstein P, Höcker P, et al. Platelet content and growth factor release in platelet-rich plasma: a comparison of four different systems. Vox Sang. 2016; 91:135-139.
- Filardo G, Kon E, Pereira Ruiz MT, Vaccaro F, Guitaldi R, Di Martino A, et al. Platelet-rich plasma intra-articular injections for cartilage degeneration and osteoarthritis: single- versus double-spinning approach. Knee Surg Sports Traumatol Arthrosc. 2012; 20: 2078-2087.
- Mazzocca AD, McCarthy MB, Chowaniec DM, Cote MP, Romeo AA, Bradley JP, et al. Platelet-rich plasma differs according to preparation method and human variability. J Bone Jone Srug Am. 2012; 94: 308-316.
- DeLong JM, Russell RP, Mazzocca AD. Platelet-rich plasma: the PAW classification system. Arthroscopy. 2012; 28: 998-1009.
- Hamilton B, Tol JL, Knez W, Chalabi H. Exercise and the platelet activator calcium chloride both influence the growth factor content of platelet-rich plasma (PRP): overlooked biochemical factors that could influence PRP treatment. Br J Sport Med. 2015; 49: 957-960.
- Cerza F, Carnì S, Carcangiu A, Di Vavo I, Schiavilla V, Pecora A, et al. Comparison between hyaluronic acid and platelet-rich plasma, intra-articular infiltration in the treatment of gonarthrosis. Am J Sports Med. 2012; 40: 2822-2827.
- Khoshbin A, Leroux T, Wasserstein D, Marks P, Theodoropoulos J, Ogilvie-Harris D, et al. The efficacy of platelet-rich plasma in the treatment of symptomatic knee osteoarthritis: a systematic review with quantitative synthesis. Arthroscopy. 2013; 29: 2037-2048.
- Mehta S. Platelet Rich Concentrate: Basic Science and Current Clinical Applications. J Orthop Trauma. 2008; 22: 432-438.
- Kilian O, Flesch I, Wenisch S, Taborski B, Jork A, Schnettler R, et al. Effects of platelet growth factors on human mesenchymal stem cells and human endothelial cells in vitro. Eur J Med Res. 2004; 9: 337-344.
- Anitua E, Andia, I, Ardanza B, Nurden P, Nurden AT. Autologous platelets as a source of proteins for healing and tissue regeneration. Thromb Haemost. 2004; 91: 4-15.
- Civinini R, Nistri L, Martini C, Redl B, Ristori G, Innocenti M. Growth factors in the treatment of early osteoarthritis. Clin Cases Miner Bone Metab. 2013; 10: 26-29.
- Iwasaki M, Nakata K, Nakahara H, Nakase T, Kimura T, Kimata K, et al. Transforming growth factor-beta 1 stimulates chondrogenesis and inhibits osteogenesis in high density culture of periosteum-derived cells. Endocrinology. 1993; 132: 1603-1608.
- Ng KW, O’Conor CJ, Kugler LE, Cook JL, Ateshian GA, Hung CT. Transient supplementation of anabolic growth factors rapidly stimulates matrix synthesis in engineered cartilage. Ann Biomed Eng. 2011; 39: 2491-2500.
- Schmal H, Niemeyer P, Südkamp NP, Gerlach U, Dovi-Akue D, Mehlhorn AT. Pain perception in knees with circumscribed cartilage lesions is associated with intra-articular IGF-1 expression. Am J Sports Med. 2011; 39: 1989-1996.
- Mariani E, Canella V, Cattini L, Kon E, Marcacci M, Di Matteo B, et al. Leukocyte-rich platelet-rich plasma injections do not up-modulate intra-articular pro-inflammatory cytokines in the osteoarthritic knee. PLos One. 2016; 11: 0156137.
- Riboh JC, Saltzman BM, Yanke AB, Fortier L, Cole BJ. Effect of leukocyte concentration on the efficacy of platelet-rich plasma in the treatment of knee osteoarthritis. Am J Sports Med. 2016; 44: 792-800.
Citation: Villarreal-Villarreal GA, Vilchez-Cavazos JF, Lara-Arias J, Pea-Martinez VM, Cardenas-Estrada E and Acosta-Olivo CA. Correlation between TGF-Beta1 and IGF-1 Plasma Values and Functional Clinical Scales in Knee Osteoarthritis after an Infiltration with Platelet-Rich Plasma. Austin J Orthopade & Rheumatol. 2016; 3(4): 1041. ISSN: 2472-369X