
Case Report
Austin J Orthopade & Rheumatol. 2016; 3(4):1045.
Are Ankylosing Spondylitis Patients at Risk for Poor Total Hip Replacement Outcomes?
Costa C¹*, Alegre C², Carvalho M², Rodrigues M¹, Carvalho P¹ and Judas F³
¹Department of Rheumatology, Centro Hospitalar e Universitário de Coimbra, Portugal
²Department of Orthopedics, Centro Hospitalar e Universitário de Coimbra, Portugal
³Faculty of Medicine, University of Coimbra; Department of Orthopedics, Centro Hospitalar e Universitário de Coimbra, Portugal
*Corresponding author: Carlos Costa, Department of Rheumatology, Centro Hospitalar e Universitário de Coimbra, Portugal
Received: November 14, 2016; Accepted: December 19, 2016; Published: December 22, 2016
Abstract
Hip involvement in Ankylosing Spondylitis is common and leads to physical and function restriction. Hip replacement surgery is a successful and effective treatment for end-stage hip involvement; however in Ankylosing Spondylitis patient’s prosthesis long-term survival is lesser than other causes of hip osteoarthritis. We report a case of 61-year old Ankylosing Spondylitis male patient with bilateral cementless hip replacement with 26-year and 25-year follow-up.
Keywords: Ankylosing spondylitis; Arthroplasty; Hip
Introduction
Ankylosing Spondylitis (AS) is the prototype of Axial Spondyloarthritis (SpA) and is a chronic inflammatory disease of unknown etiology that affects mainly active young men [1]. AS is characterized by inflammation of the sacroiliac joints, axial spine and peripheral joints. Peripheral involvement has been reported between 73% of the cases with hip being the most commonly affected joint (25- 50%) [2,3]. Hip joint and spine involvement affect patient’s ability to walk and leads to deterioration of their function and physical activity, increases the burden of the disease and its prognosis [4].
A specific treatment option in end-stage hip involvement in AS is the Total Hip Replacement Surgery (THR). The aims of THR are pain relief, increased range of motion, improved mobility and correction of posture. THR is a successful surgical procedure in advance hip osteoarthritis with long-term outcome studies demonstrating a 90% outcome survival at 15 to 20 years of follow-up [5]. However, THR survival in AS patients is lesser, being reported as 60-65% over 15 years in best series [6-8].
The authors report a case of an AS 61-year-old patient with a severe disease with several joint replacements (shoulders, hips and right knee) with a bilateral THR with 26 and 25-year follow-up.
Case Presentation
A history of low back and cervical inflammatory pain began 40 years ago with prolonged morning stiffness leading to AS diagnosis 10 years later. He was under treatment with various NSAIDs. There was a history of dactilitis, entesitis and peripheral arthritis, but there was not uveitis, psoriasis or bowel inflammatory disease and he was HLA-B27 negative. There was syndesmophites in lumbar X-ray and radiological grade III bilateral sacroiliitis. Other co-morbidities were obesity (body mass index of 38 Kg/m2), arterial hypertension and dyslipidemia.
Despite NSAID treatment the patient presented hip inflammatory pain with progressive limitation of hip range of motion and inflammatory shoulder pain. Due to the bilateral hip osteoarthritis, continuous hip pain and daily life limitations, a right and left cementless THR were performed 26 and 25 years ago respectively.
The bilateral THR were implanted using a standard posterior hip approach with the patient in lateral decubitus. THR was composed by an acetabular cup (RM®classiccup) and by a cementless femoral stem with a proximal porous coating, which allowed bone ingrowth into the stem.
Secondary shoulder osteoarthritis led to bilateral shoulder total replacement 7 and 5 years ago. Two years ago a right cemented Total Knee Replacement (TKR) was performed due a knee secondary osteoarthritis.
Currently, he presented mechanical right knee pain and unglued knee prosthesis at X-ray and need a revision surgery, however the others prostheses are well concreted.
In the last clinical and radiological controls, at 25 and 26 years after the bilateral hip artroplasty, the patient was asymptomatic, the hip mobily were normal and the patient was very pleased with the functional results. Hip radiographic study showed a stable seating of the acetabular components, no signs of stress shielding of the proximal femur, no heterotopic ossification and no signs of osteolysis (Figure 1). However, there were faint signs of wear of the left polyethylene cup, evidenced by a superior displacement of the metallic femoral head from the center of the acetabular cup.
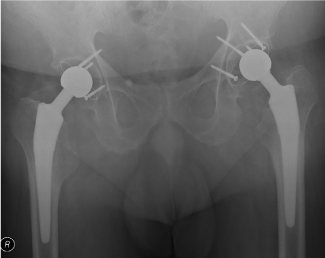
Figure 1: Hip radiograph made 26 years and 25 years after a cementless
bilateral hip arthroplasty in an ankylosing spondylitis patient. The components
of the hip prosthesis presented a solid fixation with no signs of osteolysis and
no pain. Signs of wear of the left polyethylene cup.
Discussion & Conclusion
THR is considered one of the most successful interventions in orthopedics replacement surgery, nevertheless is not a permanent implant and later or earlier will failure, regardless of the hip osteoarthritis etiology [5]. It is known that THR in inflammatory rheumatism have a lower durability due to poor bone quality and these patients had worse preoperative status and more comorbidities [9]. However, in our case the result of THR was excellent because they survived over 20 years. Despite AS inflammatory features, there was not any intolerance to foreign body in our AS patient. As known, the attrition of biomaterial prostheses particles is the source of internal biological reactions that lead to an osteolysis of acetabular and femoral bone [10]. Nevertheless, the left hip radiography shows a wear of the left polyethylene cup, there are no signs of osteolysis. Heterotopic bone formation is a well-recognized complication of THR and AS could be a risk factor for that, with an estimated incidence in some studies around 40% [11,12]. In our patient, there was not any sign of heterotopic bone formation.
The RM® classic cup (isoeslastic cup of Robert Mathys, Switzerland) is anuncemented monoblock cup system with pure titanium particle coating. The coated implant is made of UHMWPE (Ultra High Molecular Weight Polyethylene) and had been implanted all over the world since 1983. Additional fixation of the acetabular cup can be achieved, if required, with 4 mm special screws made of steel or titanium.
Cemented and cementless THR have been used for the management of hip involvement in AS patients with good results [8]. Good long-term survivorship has been reported with cemented THR, however studies of cementless THR have shorter duration of followup and therefore a conclusion of their superiority cannot be made [10]. The patient is currently asymptomatic and extremely pleased because had no complications in these 26 years and it is assumed that prostheses will continue to perform their function for many more years, although there are some signs of the left acetabular dome polyethylene wear, but without indication for surgical revision.
In conclusion, despite the less probability of THR durability in inflammatory rheumatism as AS, this is not happened in our case and we believe that will continue to play its role for many years.
References
- Zochiling J, Van der Heijde D, Burgos-Vargas R, Collantes E, Davis JC Jr, Dijkmans B, et al. ASAS/EULAR recommendations for the management in ankylosing spondylitis. Ann Rheum Dis. 2006; 65: 442-452.
- Brophy S, Taylor G, Blake D, Calin A. The interrelationship between sex, susceptibility factors and outcome in ankylosing spondylitis and its associated disorders including inflammatory bowel disease, psoriasis and iritis. J Rheumatol. 2003; 30: 2054-2058.
- Doran MF, Brophy S, MacKay K, Taylor G, Calin A. Predictors of longterm outcome in ankylosing spondylitis. J Rheumatol. 2003; 30: 316-320.
- Kubiak EN, Moskovich R, Errico TJ, Di Cesare PE. Orthopaedic management of ankylosing spondylitis. J Am Acad Orthop Surg. 2005; 13: 267-278.
- R. Stephen, J. Burnett. Total hip arthroplasty: techniques and results. BCMJ. 2010; 9: 455-464.
- Sweeney S, Gupta R, Taylor G, Calin A. Total hip arthroplasty in ankylosing spondylitis: outcome in 340 patients. J Rheumatol. 2001; 28: 1862-1866.
- Vander Cruyssen B, Munoz-Gomariz E, Font P, Mulero J, De Vlam K, Boonen A, et al. Hip involvement in ankylosing spondylitis: epidemiology and risk factors associated with hip replacement surgery. Rheumatology. 2010; 49: 73-81.
- Joshi A, Markovic L, Hardinge K, Murphy J. Total hip arthroplasty in AS: as analysis of 181 hips. J Arthroplasty. 2002; 17: 427-433.
- Goodman SM, Zhu R, Figgie MP, Huang WT, Mandl LA. Short-term total hip replacement outcomes in AS. J Clin Rheumatol. 2014; 20: 363-368.
- Malhotra R, Sharma G. Hip replacement in patients with ankylosing spondylitis. Orthophedic and muscular System. 2014; 3: 149.
- Sundaram NA, Murphy JC. Heterotopic bone formation following total hip arthroplasty in ankylosing spondylitis. Clin Orthop Relat Res. 1986; 207: 223- 226.
- Nagi ON, Dhilon MS, Batth HS. Heterotopic ossification after total hip arthroplasty: a review of etiopathogenesis, risk factors and treatment modalities. IJO. 2002; 36: 225-233.